Sandrine Benoit and Matthias Goebeler
Department of Dermatology, Venereology and Allergology, University Hospital Würzburg, Würzburg, Germany
Treatment of recalcitrant cutaneous lupus erythematosus (CLE) is challenging. In situations where conventional treatment approaches fail mepacrine – an antimalarial/antiinflammatory drug that has fallen into oblivion in the last decades – might still be a promising option. We retrospectively analysed medical records of 10 patients with refractory CLE that were treated with mepacrine (100–200 mg/day) as mono- or combination therapy for various time intervals between 2001 and 2013 at the University Hospital Würzburg. Mepacrine was generally well tolerated. Side effects were mild and usually resolved after reduction or cessation. Over 50% of the patients experienced amelioration of their symptoms despite a previously recalcitrant clinical course. Altogether, our data demonstrate that mepacrine still remains a useful and effective therapeutic option for otherwise treatment-resistant CLE. Key words: cutaneous lupus erythematosus; mepacrine; quinacrine.
Accepted Dec 3, 2014; Epub ahead of print Dec 4, 2014
Acta Derm Venereol
Sandrine Benoit, MD, Department of Dermatology, Venereology and Allergology, University Hospital Würzburg, Josef-Schneider-Str. 2, DE-97080 Würzburg, Germany. E-mail: benoit_s@ukw.de
Chloroquine (CQ) and its derivative hydroxychloroquine (HCQ) are still considered as treatment of choice in cutaneous lupus erythematosus (CLE). They have been widely used in dermatology and rheumatology for about 80 years. Although the clinical response is excellent in most cases (1), recalcitrant courses can be a challenge. In those patients the acridine derivative mepacrine (MPC; also known as quinacrine), either in combination with CQ/HCQ or as monotherapy, could result in a breakthrough (2). Initially introduced as an antimalarial drug, MPC was described by Page in 1951 (3) to improve lupus erythematosus. In the subsequent years several case series were published confirming Page’s observations. However, since its withdrawal from sale in most countries, MPC has widely fallen into oblivion.
The purpose of this retrospective study was to re-evaluate the use of MPC as therapeutic option for CLE in recalcitrant cases.
Material and Methods
We analysed patients that were treated with MPC between August 2001 and August 2013 at the Department of Dermatology, Venereology and Allergology, University Hospital Würzburg. MPC (BCM, Nottingham, United Kingdom) was obtained from international pharmacies since it is not approved in Germany.
Patients’ clinical records were reviewed and information on subtype of CLE, sex, age at diagnosis and at start of treatment with MPC, smoking history, previous and concomitant treatments, initial and maximum dose of MPC, duration of treatment, response, side effects and duration of follow-up collected. Clinical subtype of CLE was diagnosed under consideration of clinical picture, histopathology and immunological results. Clinical response was analysed in patients in whom MPC was applied for at least 12 weeks. Complete remission was defined as absence of evident skin disease activity. A subset of patients achieved complete remission followed by flare-ups. These patients were classified separately. Partial responders were subdivided in those who experienced long-term partial resolution of the skin disease activity and a second group that only improved for a short time. Non-responders experienced no improvement. Moreover, the activity of the disease was measured by the Revised Cutaneous Lupus erythematosus disease Area and Severity Index (RCLASI) (4), which considers the activity of skin lesions in 14 anatomical regions as well as the involvement of mucous membranes and alopecia. Compared to the Cutaneous Lupus erythematosus disease Area and Severity Index (CLASI) the RCLASI is considering 2 additional parameters to better cover disease activity of the skin (i. e. oedema/infiltration and subcutaneous nodules/plaques); furthermore, evaluation of mucous membranes had been improved.
According to the German national guidelines, dosage of MPC was reduced in patients who experienced complete or partial remission to find the individual maintenance dose (2). Worsening occurring in the context of this dose reduction was not considered. MPC was stopped either in context of side effects or after achieving stable disease.
Results
We identified 10 patients that were treated with MPC (8 women, 2 men; Table SI1). Five of these suffered from discoid lupus erythematosus (DLE), 4 from subacute cutaneous lupus erythematosus (SCLE) and 1 from lupus erythematosus tumidus (LET). The age at start of MPC ranged from 22 to 73 years (mean age ± standard deviation (SD): 41.5 ± 15.7 years). MPC therapy was started 1 to 13 years after initial diagnosis of CLE (mean ± SD duration of illness: 6.3 ± 4.3 years). All patients were smokers (n = 8) or had a history of smoking (n = 2). All patients had previously been treated with HQC, 3 patients additionally with CQ. In addition, some patients had received systemic corticosteroids (n = 3), thalidomide (n = 1), azathioprine (n = 1) or acitretin (n = 1) before. MPC was given as adjunctive therapy; only one patient received it as monotherapy (Table SI1).
Three patients received MPC over several months at 2 different time points; thus, a total of 13 treatment courses in 10 patients was analysed. MPC was started at a daily dosage of 100 mg in 11 treatment courses and increased to up to 200 mg daily in 2 courses. In another 2 courses MPC was directly started in a dosage of 200 mg daily. The follow-up ranged from 8 months to 12 years.
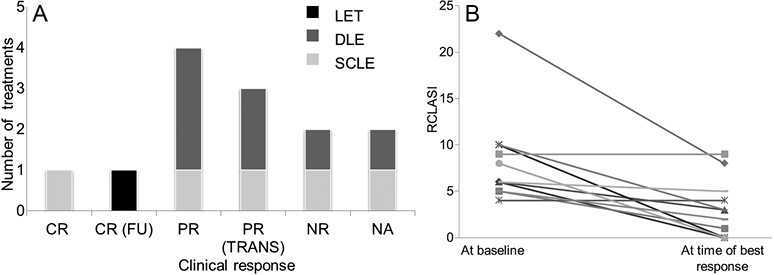
Two treatment courses were stopped 4 weeks after initiation due to side effects; therefore, clinical outcome was not analysed in these cases. In 6 out of 11 treatments either complete response (n = 1), complete response with flare-ups (n = 1) or partial response (n = 4) was achieved (Figs 1 and 2A). Another 3 treatments resulted in temporary improvement while 2 were not effective at all.
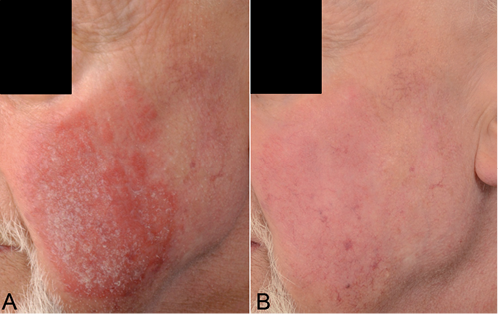
Fig. 1. Clinical status of patient No. 1 at initiation of mepacrine (A) and at 20 weeks showing complete remission (B).
In the 3 patients who received more than one course of MPC therapy, the first MPC treatment was stopped either due to side effects (n = 1), stable disease (n = 1) or lack of longstanding improvement (n = 1). One of those patients who were treated twice experienced partial remission in either case. Another patient achieved a partial response first, but no longstanding improvement during the second treatment phase. The third patient did not respond to first MPC use and the second therapy had to be stopped within 4 weeks due to side effects.
RCLASI was assessed for 11 therapy courses. In 2 cases RCLASI could not be calculated because of incomplete documentation. RCLASI scores at initiation of MPC treatment and at the time point when best response was first achieved are shown in Fig. 2B. In patient #6, complete remission was achieved temporarily, but was not longstanding although the dosage of MPC was not reduced to less than 100 mg/day. Therefore, this patient was classified as partial responder.
Adverse effects were noted during 6 treatment courses; none of them was serious. During 3 treatment courses patients experienced yellow discoloration of the skin. Augmented sensitivity to UV exposure was observed once and treatment was ceased therefore. In 3 other cases MPC was stopped due to fatigue and weight loss (n = 1), pruritus 4 weeks after initiation of treatment (n = 1) or elevation of liver enzymes followed by a rash 4 months after MPC had been started (n = 1). In all cases, symptoms relieved after cessation.
Discussion
As stated in a Cochrane review in 2009, randomised controlled studies investigating therapies for CLE are widely lacking (1). Although CQ/HCQ is generally used as first-line treatment in CLE, only one comparative trial was identified. In this study 50% of the patients treated with HCQ achieved improvement after 8 weeks (5). Taking into account that the onset of clinical improvement may start with a delay of months it may be assumed that true response rates are higher. According to a recent survey of the European Society of Cutaneous Lupus Erythematosus, amelioration of CLE was achieved in 70.6–92.8% of 706 CLE patients analysed (6). While unresponsiveness to HCQ may be due to low blood concentrations because of poor adherence to treatment (7), there obviously remains a subset of CLE patients experiencing no or only limited amelioration with HCQ. In these patients, numerous systemic treatments have been proposed including mycophenolate mofetil, methotrexate, dapsone, thalidomide, retinoids, intravenous immunoglobulin and biologicals as well as MPC either as monotherapy or in combination (8–10). These recommendations are mostly based upon expert opinions, case reports and uncontrolled trials. Altogether, evidence levels of recommendations for treatment of recalcitrant CLE are low. Conclusive studies are needed but – as in our study – may be hampered by a variety of problems: since MPC had been administered in systemic lupus erythematosus (SLE) or different types of CLE, either as first or second line therapy, as monotherapy or in combination with HQC, CQ and different immunosuppressants, comparison of the results remained difficult (11–13). Skin lesions occur in up to 85% of patients suffering from SLE (14). The criteria established by the American College of Rheumatology for the classification of SLE are suitable to only a limited extent to distinguish CLE (15). Revised criteria were suggested, but still need to be incorporated into studies and clinical practice (16). Besides the physician assessment, disease activity of CLE could be measured by CLASI (17, 18). It was revised and improved in 2010 to take the different subtypes of CLE – especially lupus erythemathosus profundus and LET – into account (4). Nevertheless, it is still challenging to judge and compare the response of CLE in patients that experience flare-ups. These patients might benefit from therapy in terms of reduced quantity or length of disease episodes, which, however, is difficult to assess. Therefore, we judged clinical improvement by physician assessment and divided patients in different groups including complete remission followed by flare-ups and transitory partial response.
Response rates achieved by MPC are varying. In our series, complete or partial response was achieved in 6 out of 11 treatments (55%) that should be regarded as satisfactory taking into account, that we investigated a preselected group of patients mostly having a long history of CLE and various pre-treatments. Toubi et al. (13) reported complete remission – defined as Systemic Lupus Erythematosus Disease Activity Index (SLEDAI) 0–2 points – in 5 of 6 SLE patients treated. Cavazzana et al. (11) investigated the amelioration of skin involvement in lupus erythematosus in 34 patients treated with HCQ/MPC. All patients suffering from acute lupus rash improved as well as 60% of patients suffering from SCLE and 50% affected by chilblain lupus. Lupus profundus, however, did not improve. In 2011, Chang et al. (19) reported improvement in 67% of their patients treated with a combination of HCQ/MPC (n = 15) and in 33% of their cases treated with a combination of CQ/MPC (n = 6).
Environmental factors such as sun exposure or smoking not only influenced the clinical course of CLE itself but also the response to therapy, e.g. with HCQ/CQ (6, 20, 21). In our study all patients were smokers or had a history of smoking, which may explain the recalcitrant course of disease. While all patients participating in our study were encouraged to stop smoking, to use sunscreens and to avoid sun exposure, standardisation of these treats remained challenging and need to be considered for the interpretation of therapy outcome.
MPC has been used by roughly 3 million soldiers during the Second World War; thus, there is substantial experience regarding its side effects. As in our patients, yellow discoloration of the skin and/or conjunctiva, which is a harmless side effect regularly dissolving after cessation, was observed in up to one third of the cases (22, 23). Additionally, gastrointestinal symptoms, neurological or psychic alterations and hepatitis have been described (23). These symptoms are generally mild and mostly reversible after reduction or drug withdrawal. In the literature, MPC dosages varied from 300 mg/day to 50 mg/day (11–13, 22); 100 mg/day of MPC is considered as optimal dose balancing efficacy and potential side effects (11, 22).
Although the value of our study may be limited due to small sample size, retrospective study design, different subtypes of CLE, concomitant therapy and confounding environmental factors we are convinced that nowadays MPC treatment still remains a useful and reasonable therapeutic strategy with an overall good safety profile in patients suffering from recalcitrant CLE.
Acknowledgement
This publication was funded by the German Research Foundation (DFG) and the University of Würzburg in the funding programme Open Access Publishing.
The authors declare no conflict of interest.

1http://www.medicaljournals.se/acta/content/?doi=10.2340/00015555-2031
References
