Loris Pignolo, Eng, Stefania Rogano, MD, Maria Quintieri, MD, Elio Leto, MD and Giuliano Dolce, MD
From the S. Anna Institute and RAN – Research in Advanced Neurorehabilitation, Crotone, Italy
Loris Pignolo, Eng, Stefania Rogano, MD, Maria Quintieri, MD, Elio Leto, MD and Giuliano Dolce, MD
From the S. Anna Institute and RAN – Research in Advanced Neurorehabilitation, Crotone, Italy
OBJECTIVE: To update knowledge of the incidence of paroxysmal sympathetic hyperactivity (PSH, also referred to as dysautonomia), an emergency condition tentatively attributed to sympathetic paroxysms or diencephalic-hypothalamic disarrangement associated with severe diffuse brain axonal damage or hypoxia. This condition is reportedly common in the vegetative state, threatens survival and affects outcome.
METHODS: The results of a retrospective study on 333 subjects in a vegetative state admitted to a dedicated unit in 1998–2005 are compared with a survey on patients admitted to the same unit in 2006–2010.
Results and comment: In the 1998–2005 period, the incidence of PSH was 32% and 16% in post-traumatic and non-traumatic patients, respectively. It decreased to 18% and 7% in the 2006–2010 period. The PSH duration and the time spent in emergency units before admission and in the dedicated unit for the vegetative state after admission also decreased significantly. Incidence was greater among post-traumatic patients; its effect on outcome does not appear to have changed.
Key words: paroxysmal sympathetic hyperactivity; dysautonomia; incidence; vegetative state; outcome.
J Rehabil Med 2012; 44: 502–504
Correspondence address: Loris Pignolo, S. Anna Institute and RAN – Research in Advanced Neurorehabilitation, Crotone, Italy. Email: l.pignolo@istitutosantanna.it
Submitted September 27, 2011; accepted March 23, 2012
INTRODUCTION
The critical association of signs such as tachycardia (> 120 beats/min), tachypnea (> 30/min), systolic hypertension (> 160 mmHg), hyper/hypothermia, excessive sweating, decerebration/decortication, increased muscle tone, horripilation and/or flushing is collectively referred to as “dysautonomia” or “paroxysmal sympathetic hyperactivity” syndrome (PSH) (1, 2). PSH is reportedly a common event in the vegetative state (VS, also referred to as “unresponsive wakefulness syndrome” or UWS) (3) and threatens these subjects’ survival and recovery. It is tentatively attributed to sympathetic paroxysms or diencephalic-hypothalamic disarrangement associated with severe diffuse brain axonal damage or hypoxia, and, by all criteria, is classed as an emergency condition (1–9).
A total of 333 subjects with severe disorder of consciousness following massive traumatic (n = 213; 64%) or non-traumatic (vascular, anoxic-hypoxic, infective or others) acute brain damage were retrospectively surveyed in a previous study (8). All patients had been referred to the S. Anna Institute – RAN in the years 1998–2005 for being in a VS/UWS condition (8). PSH occurred in 26.1% of them, with greater incidence after traumatic than non-traumatic brain injury (31.9% vs 15.8%). Outcome was worse following non-traumatic brain damage irrespective of PSH and worst among non-traumatic subjects with PSH. Occurrence of PSH and outcome were accounted for by the variance explained by variables (such as aetiology, age and sex) that are already known to be predictors of outcome for patients with severe disorder of consciousness, such as the VS/UWS (10–14). However, the mathematical model correlating the occurrence of PSH with the subjects’ clinical characteristics accounted for only 40% of the overall data variance (8). In this respect, the study was inconclusive and the natural history of the PSH remains poorly understood. Incidence is also unclear due to the lack of studies on large samples and over time (1, 4, 5). The purpose of this paper was to compare the incidence of PSH in 1998–2005 with a new group of subjects in VS/UWS admitted to and cared for in the same institute in the period 2006–2010.
PATIENTS AND METHODS
A new database of 169 patients admitted to the dedicated semi-intensive care unit of the S. Anna – RAN institute over a 4-year period (January 2006 to May 2010) was compared with the subjects’ group of the first survey (8). Eighty-eight subjects (52%) were in a VS/UWS due to traumatic brain injury; non-traumatic aetiologies (major vascular insults, anoxia-hypoxia, etc.) were documented for 81 subjects (48%). Subjects were diagnosed at admission as being in a VS/UWS according to the current clinical criteria (11, 16–19) and established evaluation scales. The scores of subjects in VS/USW were lower than 25 on the Loewenstein Scale (20), lower than 2 on the Level of Cognitive Function scale (21), and higher than 21 on the Disability Rating Scale (22). The revised Coma Recovery Scale (CRS-r) (23) global score was assessed retrospectively and found to be lower than 8 in all subjects. In all cases, subjects with infection, metabolic disorder, lung diseases affecting the cardio-respiratory function, or drug side-effects were excluded from the study. Outcome was defined in full accordance with the Glasgow Outcome Scale (GOS) (23, 24). The ranking classes were: 1 = death; 2 = VS/UWS exceeding 1 year in duration; 3 = recovery, with severe disabilities; 4 = recovery, with mild disabilities; and 5 = full recovery or recovery with minimal disabilities not interfering with everyday life (24–27).
With the exception of the revised Coma Recovery Scale (which was not in use in this country before 2007), the criteria by which patients have been diagnosed as being in a VS/UWS and by which PSH was identified were the same in the two studies, as were the monitoring, healthcare, pharmacological treatment (27) and rehabilitative procedures and protocols in the S. Anna – RAN unit; in addition, the attending physicians were the same. The data from the 1998–2005 and the 2006–2010 periods were compared using the exact Fisher’s test.
The study is retrospective and was approved by the local public healthcare ethics committee. Regulations about subjects’ privacy and the ethical principles of the Declaration of Helsinki (1964) of the World Medical Association concerning human experimentation were followed.
RESULTS
The incidence of PSH was found to have decreased from the 1998–2005 period to the 2006–2010 period, with a reduction from 32% to 18% and from 16% to 7% among subjects with post-traumatic and non-traumatic brain damage, respectively.
Both the time spent in the emergency or intensive care units before admission to the S. Anna – RAN dedicated unit for the VS/UWS and the permanence in this unit have decreased irrespective of aetiology; the PSH duration decreased among non-traumatic subjects (Table I). Outcome did not change significantly (χ2, Pearson’s = 0.332, p = 0.56423), although the percentage of subjects with outcome in the GOS rank 1 (death) appears to have increased (Fisher’s exact test: p = 0.8053633) (Fig. 1).
Table I. Incidence of paroxysmal sympathetic hyperactivity (PSH) syndrome in vegetative state (VS)/unresponsive wakefulness syndrome (UWS) following traumatic and non-traumatic brain injury. Comparison between the subjects admitted in the 2006–2010 period with those of the previous survey (1998–2005)
|
Traumatic brain injury |
Non-traumatic brain injury |
|||
|
1998–2005 |
2006–2010 |
1998–2005 |
2006–2010 |
|
|
Subjects with PSH, % |
32 |
18 |
16 |
7 |
|
Age, years, mean (SD) |
25.0 (9) |
25.5 (9) |
31.0 (15) |
50 (15) |
|
Time in emergency/intensive care units before admission to the dedicated unit for VS, days, mean (SD) |
77.0 (71) |
44.3 (26)* |
74.0 (65) |
58.6 (15)*** |
|
Time in the dedicated unit for VS, days, mean (SD) |
186 (69) |
164 (104.5)** |
224.0 (88) |
201 (125)** |
|
Duration of PSH, days, mean (SD) |
162 (90) |
70 (34) |
190.0 (50) |
116 (146)*** |
|
Fisher’s exact test vs 1998–2005. *p < 0.05, **p < 0.01, ***p < 0.001. SD: standard deviation. |
||||
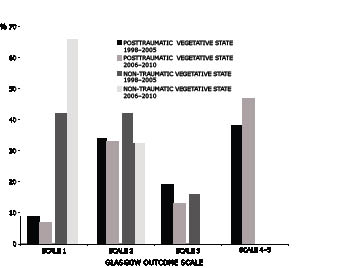
Fig. 1. Outcome of subjects in a vegetative state with paroxysmal sympathetic hyperactivity syndrome. Comparison between the 1998–2005 and 2006–2010 subject groups.
DISCUSSION
Epileptogenic mechanisms cannot be excluded a priori in all cases (29), but the pathophysiological processes starting and sustaining PSH remain a matter of speculation. Two main underlying mechanism have been suggested, notably a functional disconnection or unbalanced activation of structures usually under the control of higher brain centres (30), and an excitatory/inhibitory ratio model of paroxysms resulting from the abnormal processing of and over-responsiveness to the afferent stimuli from the medulla (31). A residual neuroendocrine reactivity is suggested by the lower incidence among anoxic-hypoxic patients with diffuse brain damage (9); its remission following treatment with serotonin or GABA modulators (32, 33) suggests hypothalamic dysregulation (34, 35). A multifactorial origin appears conceivable and would be consistent with the variability of the PSH clinical picture as to number, relevance, variability or development over time, and spontaneous or drug-mediated remission of clinical signs.
Undetected (interactions among) factors possibly modifying the clinical picture or affecting its incidence may have accounted for the differences observed in the two subject groups and are not necessarily compensated for by the group sizes. This caveat notwithstanding, the comparison between two large patient groups monitored in the same unit for a short time interval suggests that the incidence of PSH may be decreasing, and that the condition has somehow become less severe and/or is better managed, at least in subjects with VS/UWS of non-traumatic aetiology. A more effective (although not necessarily intentional) prevention and better focused treatment in intensive care units appears possible; improved procedures to reduce brain oedema and control intracranial hypertension and early sedation in intensive care units are possible factors that may help reduce the incidence of dysautonomia (36).
Outcome does not seem to have improved in recent years, however. The differences between the two subject groups in a VS/UWS of non-traumatic aetiology suggests a higher percentage of subjects who died during the observation after PSH (i.e. with outcome to be rated as GOS 1), but in all cases death resulted from clinical events unrelated to the pathophysiology of the VS/UWS or PSH. The relevance of PSH as a negative prognostic indicator remains confirmed; patients should be monitored for its occurrence and ad hoc therapeutic procedures should be devised.
ACKNOWLEDGEMENTS
The study has been carried on at the S. Anna – RAN Institute with support from the institute; authors are all employees of the institute.
The authors report no conflicts of interest.
REFERENCES
