Cindy Gauthier, MScPT (candidate)1,2, Dany Gagnon, PT, PhD1–3, Murielle Grangeon, PhD1,2, Géraldine Jacquemin, MD1, Sylvie Nadeau, PT, PhD1,2, Kei Masani, PhD3,4 and Milos R. Popovic, Eng, PhD3,4
From the 1Pathokinesiology Laboratory, Center for Interdisciplinary Research in Rehabilitation of Greater Montreal, Institut de réadaptation Gingras-Lindsay-de-Montréal, 2School of Rehabilitation, University de Montréal, Montreal, 3Rehabilitation Engineering Laboratory, Toronto Rehabilitation Institute -UHN, 4Institute of Biomaterials and Biomedical Engineering, University of Toronto, ON, Canada
OBJECTIVES: To compare multidirectional seated postural stability between individuals with spinal cord injury and able-bodied individuals and to evaluate the impact of abdominal and low back muscle paralysis on multidirectional seated stability.
DESIGN: Case-control study.
PARTICIPANTS: Fifteen individuals with complete or incomplete spinal cord injury affecting various vertebral levels participated in this study and were gender-matched with 15 able-bodied individuals.
METHODS: Participants were instructed to lean as far as possible in 8 directions, set apart by 45° intervals, while seated on an instrumented chair with their feet placed on force plates. Eight direction-specific stability indices and a global stability index were calculated.
RESULTS: The global stability index and all direction-specific indices, except in the anterior and posterior directions, were lower in individuals with spinal cord injury than in able-bodied individuals. However, the individuals with spinal cord injury who had partial or full control of their abdominal and lower trunk muscles obtained a similar global stability index and similar direction-specific indices compared to the able-bodied individuals.
CONCLUSION: Multidirectional seated postural stability is reduced in individuals with SCI who have paralysis of the abdominal and lower back muscles in comparison to able-bodied individuals.
Key words: movement; outcome assessment; postural balance; rehabilitation; spinal cord injuries.
J Rehabil Med 2013; 45: 00–00
Correspondence address: Dany Gagnon, School of Rehabilitation, University de Montréal, Pavillon 7077 Avenue du Parc, P.O. Box 6128, Station Centre-Ville, Montreal, Quebec, H3C 3J7 Canada. E-mail: dany.gagnon.2@umontreal.ca
Submitted November 30, 2011; accepted August 10, 2012
INTRODUCTION
Individuals with a spinal cord injury (SCI) often experience sensory and motor impairments that can affect, to varying degrees, the muscles in the trunk, lower extremities (L/Es) or upper extremities (U/Es). The severity of these impairments is primarily related to the vertebral level and the degree of completeness of the lesion sustained to the spinal cord. Seated postural stability is affected in the majority of individuals with SCI since the strength generating ability and muscle synergies of the trunk, hip and L/E muscles governing seated postural stability are impaired (1). As a consequence, individuals with SCI are exposed to an increased risk of instability, and even falls (2), when maintaining a sitting posture or performing functional activities in a sitting position. This may have deleterious consequences on their ability to carry out numerous functional activities or their confidence in their balance, which may, in turn, hamper their societal participation. Unfortunately, while the relevance of studying multidirectional seated postural stability or postural control of the trunk is frequently acknowledged in the literature, particularly in individuals with SCI who rely on a wheelchair for mobility (3, 4), the quantitative assessment of seated postural stability has only sparsely been investigated to date among individuals with SCI (5–13).
Aside from the clinical measurement tools that have been proposed to investigate seated postural stability in individuals with SCI (10–12), only a few studies have quantified it using a biomechanical approach in this population (5, 6, 8). Among these few studies, even fewer have investigated dynamic seated postural stability (5, 6) and no consensus has yet been reached regarding the preferred methodological approach in this population. To date, most of these studies have investigated the forward (anterior direction) reaching test with unilateral or bilateral U/E use while individuals with SCI sit on a force plate with their feet resting or not resting on the floor (3, 5, 9). The main outcome measures of these studies were generally determined by measuring linear reaching distance of the hand(s) or trunk displacement (5) or by computing center of pressure (COP) measures from stabilograms (3, 5, 8). These outcome measures, especially COP-related outcome measures, provide vital information about the coordinated neuromuscular responses of recruited postural and non-postural muscles and on the contribution of passive stiffness to regulate the complex interactions between the center of mass (COM) and the COP (14–18). The generalizability of the results found in most of these studies is potentially restricted for the following reasons: reaching tests have not generally been conducted in numerous directions, reaction forces underneath the feet have not always been recorded on the floor, the feet have often been unsupported and the area of the base of support has been unknown. Furthermore, since these studies often required the use of the U/Es to reach out toward targets, the ability to assess individuals with tetraplegia or severe U/E impairments was limited.
To overcome these limits, the recently proposed approach by Preuss & Popovic (19) to quantitatively define the limits of stability within a well-defined base of support (BOS) while sitting in able-bodied individuals appears promising. This approach specifically incorporates 8 target-directed trunk inclinations, from which COP excursion is quantified in order to determine the limits of stability. These inclinations, along with their resulting inertial forces, need to be counterbalanced by coordinated responses guided by the central nervous system to regulate the complex interactions between the COM and the COP (14, 20–23). This approach was also validated when the limits of stability were changed, when the target distances were modified or when the speed of trunk movements was altered (19). Even if the limits of stability do not explain all of the compensatory strategies and postural balance control, they provide quantitative and validated measures of postural stability. Such measures are becoming essential in rehabilitation and could rapidly translate into changes in clinical practice and research protocols.
Therefore, the first objective of this study was to compare multidirectional seated postural stability between individuals with a SCI and able-bodied individuals by using 8 direction-specific stability indices and an overall stability index. The second objective was to evaluate the effects of back and abdominal muscles on multidirectional seated postural stability by comparing individuals who have partial (paresis) or complete innervations of their low back and abdominal muscles to individuals who have complete paralysis of their low back and abdominal muscles. The third objective was to verify if the individuals with SCI who have partial or complete innervations of their low back and abdominal muscles had multidirectional seated postural stability ability similar to that measured in able-bodied individuals. It was hypothesized that the able-bodied individuals would exhibit higher direction-specific stability indices and a higher overall stability index than individuals with SCI. Moreover, differences in multidirectional seated postural stability were expected between individuals with SCI who have the preservation of their low back and abdominal muscles, individuals with no low back or abdominal muscles innervations, and able-bodied individuals.
METHODS
Participants
A convenience sample of 15 individuals with SCI and 15 able-bodied individuals volunteered to participate in this study after having met the inclusion criteria. Individuals with SCI were eligible to participate in this study if they had sustained a complete or incomplete SCI (American Spinal Injury Association Impairment Scale (AIS A–D) affecting various vertebral levels at least 3 months prior to the study (Table I). Moreover, individuals with SCI had the ability to independently maintain an unsupported short-sitting position with their feet resting on the floor for one minute, and had an activity tolerance of at least 60 min when rest periods were allowed. Individuals with SCI were also stratified into two subgroups: 1) individuals with SCI who had partial or total use of their low back and abdominal muscles (SCIAbdo; n = 9), and 2) individuals with SCI who had complete paralysis of their low back and abdominal muscles (SCINo Abdo; n = 6). For individuals who had a complete motor SCI (AIS A or B), allocation to either subgroup was solely determined by the neurological level of the SCI. More precisely, individuals who had a neurological level below the seventh thoracic neurological level (T7) were assigned to the SCIAbdo subgroup, whereas those with a level above T7 were assigned to the SCINo Abdo subgroup. As for individuals who had an incomplete SCI (AIS C or D), subgroup assignment was determined by their ability to voluntary contract their abdominal muscles to generate trunk flexion with at least partial range of motion while supine with U/Es at their sides (24) (preservation of motor function = SCIAbdo subgroup).
|
Table I. Description of individuals with spinal cord injury (n = 15) |
||||||||||
|
Subjects |
Age, years |
Height, m |
Weight, kg |
Time since injury, years |
AIS Neurological level |
AIS Severity |
ASIA-Motor |
ASIA-Sensory |
ASIA-Sensory |
BOS area, m2 |
|
1 |
57.2 |
1.68 |
98.3 |
2.93 |
T4 |
A |
50 |
96 |
No Abdo |
0.35 |
|
2 |
23.2 |
1.68 |
86.3 |
0.88 |
C3 |
D |
93 |
187 |
Abdo |
0.33 |
|
3 |
52.3 |
1.63 |
88.4 |
1.76 |
C6 |
B |
28 |
72 |
No Abdo |
0.31 |
|
4 |
46.6 |
1.83 |
109.1 |
5.02 |
L1 |
C |
70 |
176 |
Abdo |
0.39 |
|
5 |
49.1 |
1.73 |
84.5 |
1.73 |
C5 |
D |
78 |
153 |
Abdo |
0.37 |
|
6 |
53 |
1.78 |
129.6 |
5.14 |
T10 |
A |
50 |
144 |
Abdo |
0.36 |
|
7 |
44.4 |
1.70 |
73.8 |
2.67 |
T10 |
A |
50 |
140 |
Abdo |
0.27 |
|
8 |
57.9 |
1.88 |
98.2 |
2.99 |
T10 |
B |
50 |
140 |
Abdo |
0.33 |
|
9 |
26.1 |
1.63 |
46.8 |
2.78 |
T11 |
A |
50 |
148 |
Abdo |
0.25 |
|
10 |
32.6 |
1.75 |
65.1 |
3.09 |
C7 |
B |
48 |
156 |
No Abdo |
0.25 |
|
11 |
25.3 |
1.80 |
52.9 |
2.77 |
T4 |
A |
51 |
96 |
No Abdo |
0.25 |
|
12 |
30.2 |
1.88 |
98.1 |
3.33 |
T10 |
A |
50 |
140 |
Abdo |
0.34 |
|
13 |
49.9 |
1.80 |
78.1 |
25.9 |
T7 |
B |
51 |
194 |
No Abdo |
0.31 |
|
14 |
25.2 |
1.83 |
67.9 |
2.08 |
C5 |
B |
14 |
58 |
No Abdo |
0.32 |
|
15 |
40.0 |
1.70 |
59.3 |
0.15 |
C8 |
C |
69 |
110 |
Abdo |
0.24 |
|
Mean (SD) |
40.9 (12.6) |
1.75 (0.08) |
82.43 (22.4) |
4.21 (6.1) |
53.5 (18.9) |
134.0 (40.1) |
n = 6 |
0.31 (0.05) |
||
|
AIS: American Spinal Injury Association (ASIA) Impairment Scale; BOS: base of support; Abdo/No Abdo: ability to use their low back and adbominal muscles or not; SD: standard deviation. |
||||||||||
A gender-matched control group of 15 able-bodied individuals were recruited (Table II). None of the participants reported having musculoskeletal impairments that affected their trunk, L/Es or U/Es or any other condition that might have altered their ability to maintain a short-sitting position. The study was conducted at the Pathokinesiology Laboratory of the Center for Interdisciplinary Research in Rehabilitation of Greater Montreal (CRIR) located at the Institut de réadaptation Gingras-Lindsay-de-Montréal. Ethical approval was obtained from the Research Ethics Committee of the CRIR (CRIR456-0809). All participants reviewed and signed the informed consent form before entering the study.
|
Table II. Comparison between individuals with spinal cord injury (SCI) (n=15) and able-bodied individuals (n = 15) |
|||||
|
Gender Male/female, n |
Age, years Mean (SD) |
Height , m Mean (SD) |
Weight, kg Mean (SD) |
BOS area, m2 Mean (SD) |
|
|
Individuals with SCI |
14/1 |
40.9 (12.6) |
1.75 (0.08) |
82.4 (22.4) |
0.31 (0.05) |
|
Able-bodied Individuals |
14/1 |
39.3 (12.6) |
1.74 (0.07) |
77.4 (11.7) |
0.32 (0.04) |
|
p-value |
N/A |
0.731 |
0.521 |
0.443 |
0.775 |
|
p ≤ 0.05. BOS: base of support; SD: standard deviation. |
|||||
Laboratory assessment
Center of pressure assessment. Participants were seated on a height-adjustable instrumented seat built with two force-sensing surfaces (i.e., underneath the right and left buttock), with their right and left feet supported on two separate force plates embedded into the floor (25, 26). The ground reaction force was recorded with a sampling frequency of 600 Hz during the experimental tasks. Participants were positioned with approximately 75% of the length of their thighs in contact with the instrumented seat and their knees flexed at approximately 85°. Participants sat upright with both hands placed on their thighs (starting position) to support part of their body weight (head, U/E and trunk segments) and to facilitate sitting balance control prior to initiating the tests.
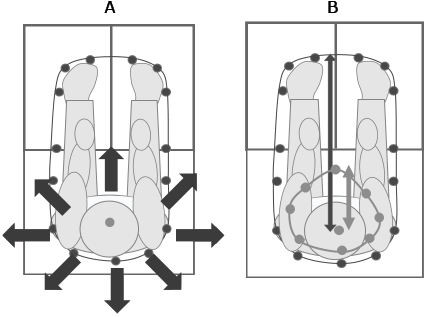
Base of support assessment. To measure the BOS, kinematic parameters were recorded during each experimental trial at a sampling frequency of 60 Hz using 6 synchronized motion analysis camera bars (4x Optotrak model 3020 and 2x Optotrak model Certus; NDI Technology Inc., Waterloo, Ontario, Canada). This motion capture system recorded the 3-dimensional (3D) coordinates of 10 infrared light emitting diodes (LEDs) fixed on the instrumented seat to locate it within the global referential (laboratory referential). Additionally, the 3D coordinates of 18 skin-fixed LEDs used to define the head, trunk, pelvis, U/E and L/E segments (including the feet) were recorded when participants leaned in the various directions. A total of 24 specific bony landmarks were also digitized using a 6-marker probe while participants maintained a static seated position to further define principal axes of segments as well as the contour of the feet and buttocks used to calculate the area of the BOS. The area of the BOS reflects the convex area enclosing the contour of the feet and buttock segments (peripheral points) projected into the horizontal plane of the COP (Fig. 1).
Fig. 1. Schematic representation of the 8 specific directions assessed (thick arrows) (A) and of the anterior direction-specific stability index and the overall stability index (B). The tall arrow represents the maximal the oretical position the center of pressure (COP) could have moved to reach the boundary of the base of support in the anterior direction, whereas the short arrow represents the real distance travelled by the COP.
Experimental tasks. Following a familiarization period, participants were asked to lean their head and trunk segments (axial skeleton) from the starting position as far as possible at a self-selected speed in 8 specific directions, each separated by 45°, and to return to their initial position within a 15-s period. Participants were instructed to place and maintain their hands on their thighs and to refrain from anchoring themselves or grabbing their clothes or body segments (i.e., thighs). A flat screen placed 2 m in front of them revealed the tested direction and indicated specific boundaries in which they had to move their COP while providing the real-time position of the COP (visual feedback). Each of the 8 movement directions was tested twice for a total of 16 movements, performed in random order determined by computer and locked into the program prior to the start of the test. One research associate remained next to the participants to ensure optimal safety and to prevent loss of balance or a fall during these movements. If loss of balance occurred during one or more trial(s) during the testing procedure, the trial(s) were not repeated due to the constraint of the computer program, which randomly assigned two trials in each direction in a precise sequence prior to the start. Consequently, the(se) trial(s) could not be repeated and were not included in the analysis. Another research associate coordinated the computerized data acquisition and storage at all times.
While these movements were performed, the tri-axial components of the ground reaction forces underneath the left and right buttock as well as underneath the left and right foot were continuously recorded to compute the COP time series with respect to the starting point on the force plate coordinate system. All data were filtered with a fourth-order Butterworth zero-lag filter, with a cut-off frequency of 5 Hz and then down-sampled at 300 Hz prior to computing the outcome measures.
Outcome measures
Direction-specific index of stability. For each of the 8 tested directions, the coordinates of the initial position of the COP (COPStart), the farthest position reached by the COP in the indicated trajectory (COPFinal) and the maximal theoretical potential position the COP could have reached to attain the boundary of the BOS in the indicated trajectory (COPMaximal) were calculated. Then, the direction-specific stability index (DSI), expressed as a percentage (%), was calculated for each of the 8 directions using this equation:
|
DSI (%) = |
[ |
COPFinal – COPStart |
] |
×100 |
|
COPMaximal – COPStart |
Overall stability index. An overall stability index (OSI) representing the area defined by an ellipse fitting the mean peak COP excursion (COPArea) reached in each of the 8 tested directions (limits of stability), normalized against the area of the BOS (BOSArea),was calculated and expressed as a percentage (%):
|
OSI (%) = |
[ |
COPArea |
] |
×100 |
|
BOSArea |
Statistical analyses
Descriptive statistics (mean and standard deviation (SD)) were calculated for different participants’ characteristics and all seated postural stability outcome measures. Prior to conducting the parametric statistical analyses, a Kolmogorov-Smirnov test was completed to confirm the normality of the distribution of the seated postural stability outcome measures. For the direction-specific indices, a two-way repeated measure analysis of variance with one between factor (individuals with SCI and able-bodied individuals) and one within factor (8 tested directions) was conducted to verify if significant differences existed. Given that a significant interaction effect was found (p = 0.015), Student t-tests for independent samples were performed to pinpoint significant differences between groups in each direction (p-value = 0.05), whereas a one-way analysis of variance with a Bonferroni post-hoc test with an adjusted p-value (p = 0.05/28) was performed to compare DSIs within each group. For the overall stability index, Student t-tests for independent samples were performed to determine the presence of a significant difference between the groups. A similar approach was also used to explore differences between the subgroups of individuals with SCINo Abdo and SCIAbdo. A level of significance of 0.05 or less was selected to confirm differences between groups for all tests. All data were analyzed using the SPSS® statistical analysis software.
RESULTS
Direction-specific stability index
All participants successfully completed two trials in each of the 8 tested directions, except for two individuals with SCI who each missed one trial in the posterior and right anterolateral directions, respectively. Mean and SD (± 1 SD) for all DSIs computed for individuals with a SCI and able-bodied individuals are summarized in polar coordinate diagrams (Fig. 2A and 2B). The anterior DSI was the lowest in both groups (individuals with SCI = 22.77%; able-bodied individuals = 28.72%) compared to the other DSI. The posterior DSI was the highest in individuals with SCI (41.23%), whereas for the able-bodied individuals, the right DSI (53.20%) was the highest. For six of the 8 directions assessed, a statistically significant difference was found between individuals with SCI and able-bodied individuals (p = 0.000–0.041; mean absolute Δ = 9.9–18.52%). However, for the anterior direction (p = 0.052; mean absolute Δ = 5.96%), no statistically significant difference was revealed between individuals with SCI and able-bodied individuals.
When comparing the DSI obtained between the two subgroups of individuals with SCI (Fig. 2C and 2D), the lowest DSI was once again found in the anterior direction for both subgroups (SCIAbdo = 15.69%; SCINo Abdo = 27.48%). The highest DSI for the SCIAbdo subgroup (49.63%) was found when moving posteriorly (Fig. 2C), whereas it was in the left direction (32.19%) for the SCINo Abdo subgroup. Statistically significant differences between the subgroups of individuals with SCIAbdo and with SCINo Abdo (p = 0.002–0.020; Δ = 11.79–21.02%) were also found for most of the directions, except for the left (p = 0.087; Δ = 10.19%) and left anterolateral (p = 0.072; Δ = 11.70%) directions.
Fig. 2. Group mean (bold dark colored line) ± 1 standard deviation (light colored area) for all direction-specific indices of stability (%) in the 8 directions assessed for able-bodied individuals (A) and individuals with spinal cord injury (SCI) (B), as well as for the individuals with SCI who are able to use their low back and adbominal muscles (SCIAbdo) (C) and individuals with SCI who are not able to use their low back and adbominal muscles (SCINo Abdo) (D).
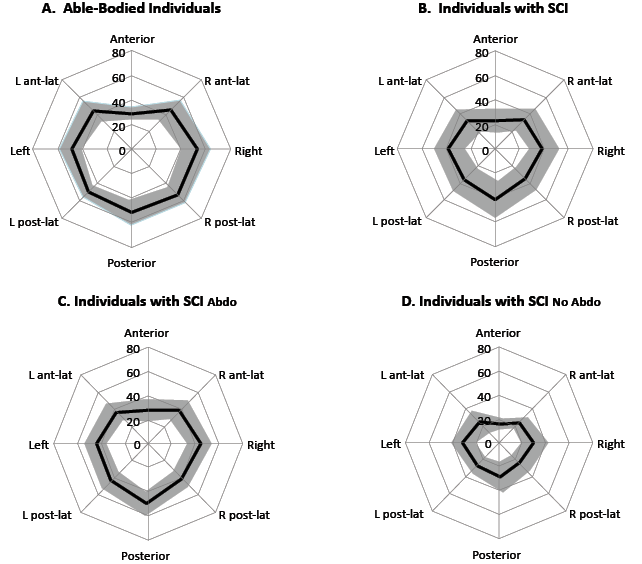
Interestingly, individuals from the SCIAbdo subgroup achieved similar values as those obtained among able-bodied individuals for 7 of the 8 DSIs investigated (p = 0.051–0.692; Δ = 3.11–4.91%). A statistically significant difference between these two groups was only found when the participants were moving in the right posterolateral direction (p = 0.011; Δ = 3.93%). In contrast, statistically significant differences (p ≤ 0.005; mean absolute Δ = 13.03–29.84%) were found between the SCINo Abdo subgroup and able-bodied individuals in all directions tested.
Overall stability index
The OSI (Fig. 3), which varied between 2.00% and 24.24% for individuals with SCI (mean = 10.23%) and 9.55% and 35.20% for able-bodied individuals (mean = 16.75%), was statistically different between the groups (p = 0.011; mean absolute Δ = 6.52%). As for the comparison within individuals with SCI, the OSI showed a statistically significant difference (p = 0.010; mean absolute Δ = 8.35%) between the SCIAbdo subgroup (mean = 13.57%; range = 5.9%–24.2%) and the SCINo Abdo subgroup (mean = 5.22%; range = 2.0%–11.7%). Interestingly, no statistically significant difference (p = 0.253; mean absolute Δ = 2.71%) between the SCIAbdo subgroup and able-bodied individuals was found, whereas a statistically significant difference (p ≤ 0.001; mean absolute Δ = 10.53%) was found between the SCINo Abdo subgroup and able-bodied individuals.
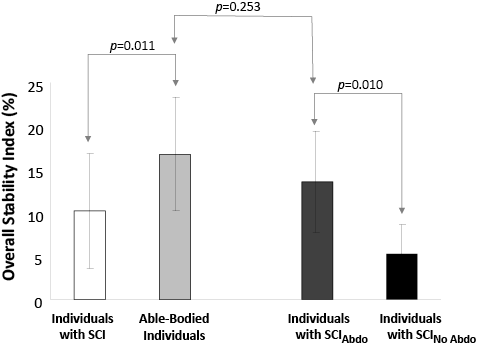
Fig. 3. Group mean (± 1 standard deviation) for the overall stability index. SCIAbdo/ SCINo Abdo: individuals with spinal cord injury who are able or not able to use their low back and adbominal muscles.
DISCUSSION
Individuals with SCI versus able-bodied individuals
The results of the current study support the hypothesis that able-bodied individuals have better multidirectional seated postural stability than individuals with SCI. Indeed, the mean DSIs and the OSI were reduced in individuals with SCI compared to able-bodied individuals, except for the anterior direction for which no difference was revealed. Since the participants had their hands resting on their thighs and could use their U/Es to some extent to control trunk displacement, a large proportion of the trunk weight might have been supported by the U/Es especially in the anterior direction. Thus, the best margin of stability occurred in this direction (expressed by the lowest DSI) and this might explain the absence of difference. When leaning forward in a seated position, the use of the U/Es represents an efficient compensatory strategy to better control the trunk, especially when paresis or paralysis of the abdominal and back muscles is present. In theory, the risk of falling when leaning forward in the present study is less than in other directions since the anterior boundary of the BOS, determined by the position of the feet resting on the floor, is enlarged as opposed to if we had elected not to allow any L/E weight support (i.e., unsupported short-sitting position (27)). As for the fear of falling forward when leaning in this direction, since individuals with SCI rely on additional sensory feedback (i.e., visual information) and the fact that they would most likely land on their thighs if they did fall from loss of balance in this direction, this may explain the reduced fear of falling, which was qualitatively reported by many participants during the laboratory assessment. Better postural control using an efficient compensatory strategy and less fear of falling might provide confidence to lean further in the anterior direction. Conversely, the lowest COP excursion range available when leaning in the posterior direction, combined with the increased fear of falling, qualitatively expressed by many participants due to the limited visual information available, the unfamiliar leaning direction and physical environment possibly restricting postural adjustments, may explain why the lowest margin of stability (expressed by the greatest DSI) was found in the posterior direction among individuals with SCI.
During lateral or diagonal trunk displacements, the weight of the axial skeleton (i.e., trunk and head segments) might become unevenly distributed across both U/Es. Furthermore, the U/Es are less effective in controlling the moving trunk due to the asymmetry between displacement and arm support, which might explain the increased instability observed for these directions in individuals with SCI compared to able-bodied individuals. Indeed, Shirado et al. (28) showed that individuals with SCI predominantly had a mediolateral displacement of the COP when U/E support was permitted in long-sitting positions, whereas able-bodied individuals exhibited a central COP pattern. The authors suggested that the U/E support primarily counteracted the forward trunk rotation or instability in the sagittal plane in individuals with SCI.
The greatest differences between the individuals with a SCI and the able-bodied individuals were found with the backward and diagonal backward directions. The compensatory role of the U/Es was indeed not as efficient in these positions compared to the other positions since participants were not allowed to grab their thighs or anchor themselves with their U/Es. The backward and diagonal backward directions, which strongly recruit the hip flexors and abdominal muscles, may also highlight the severity of the motor impairments of these muscles. Moreover, a frequent compensatory strategy observed by Minkel (29) among individuals with impairments of the trunk musculature is a change in trunk and pelvis alignment. In fact, a long C-shaped kyphotic thoracolumbar spine, a flattened lumbar spine, and a posteriorly tilted pelvis are generally observed in individuals with SCI. In this position, the posterior pelvic tilt creates a 3-point support base under the buttocks formed by the bilateral ischial tuberosities and the sacrum, with the later enlarging the BOS posteriorly. As a result, the projection of the center of gravity of the trunk, head and U/Es and the COP can shift further back which may help to optimize seated postural stability in individuals with SCI.
Thus, the present results suggest that DSIs and the OSI may effectively discriminate individuals with SCI who generally experience sensory and motor trunk impairments affecting their multidirectional seated postural stability from able-bodied individuals.
Individuals with SCIAbdo versus individuals with SCINo Abdo
As hypothesized, there was a difference in seated postural stability between individuals with no paralysis or with paresis of their low back and abdominal muscles, and individuals with paralysis of their low back and abdominal muscles, suggesting different postural strategies between these groups. In a previous study, Seelen et al. (30) found that individuals with low SCI (neurological level T9–T12) used less compensation strategies than individuals with high SCI to control sitting balance during bi-manual reaching tasks. In fact, they reported that individuals with low thoracic SCI use their trapezius pars ascendens, latissimus dorsi, pectoralis major, serratus anterior and the upper portion of their erector spinae less than individuals with high SCI while sitting. Different trunk movement strategies have also been observed during other functional tasks such as posterior transfers (31). During this transfer, a forward flexion strategy was used by individuals with limited lifting ability to create an angular momentum that facilitated the transfer. Individuals with better neuromuscular capacities used a lift strategy that used less angular momentum and greater strength. These results are compatible with the results of the present study. The higher DSI and OSI calculated in the SCIAbdo subgroup compared to the SCINo Abdo subgroup suggest that those individuals may not only have greater motor control of their trunk musculature, but also require less contribution of their none postural thoracohumeral muscle (i.e., less compensation strategies) when maintaining sitting balance or moving their trunk in various directions. In the present study, different trunk and U/Es movement strategies have been observed across directions for each participant and between individuals with and without low back and abdominal muscles during the laboratory assessment. However, these strategies were not specifically assessed in the current study.
Furthermore, individuals with no paralysis or with paresis of their low back and abdominal muscles had higher mean DSIs for the right and the right forward directions than the left and left anterolateral directions. The opposite was true for the group of individuals with paralysis of their low back and abdominal muscles. Thus, we might speculate that individuals with no paralysis of their low back and abdominal muscles might use abdominal and erector spinae muscles to control trunk movement while leaning (32). Since individuals with the most severe sensorimotor trunk impairments could not voluntary contract or only very weakly contract their low back and abdominal muscles (postural muscles), they may have stabilized their trunk with non-postural muscles on the opposite side as the hand is used to reach (i.e., the trapezius pars ascendens, latissimus dorsi, pectoralis major, serratus anterior and the upper portion of their erector spinae (30)). Based on this theory and the fact that most of the participants were right-handed, the performance in right directions observed in individuals with abdominal musculature might be explained by an enhanced development of the right side compared to the left. Conversely, individuals without the use of their low back and abdominal muscles may develop the most efficient muscle synergies to stabilize the trunk on the non-dominant side (left) to allow reaching with the dominant U/E (right) in the right direction. A comparison study between right- and left-side dominance in individuals with SCI could be conducted in the future to confirm this hypothesis. Moreover, the fact that both hands positioned on the thighs allowed the U/Es to work in a closed kinetic chain, may be an effective way to optimize postural stability, particularly among individuals with tetraplegia. However, in this latest population, careful U/E sensorimotor assessment would also be required to highlight, for example, U/E strength deficit or asymmetry.
Subgroups of individuals with SCI versus able-bodied individuals
Contrary to what was expected, similar DSIs and OSI were found between individuals with SCIAbdo and able-bodied individuals, except for the DSI measured in the posterior direction. The reduced performance in the posterior direction observed between these groups may be due to the difficulty experienced in stabilizing the trunk without the compensatory strategy of the U/Es. In fact, the proximity of the posterior boundary of the BOS with respect to the COP, which has been previously reported in the literature as a possible compensatory strategy to optimize postural stability among individuals with SCI (29), drastically restricts the range of movement in this direction, therefore reducing the COP range available for individuals to make postural adjustments. The fact that visual information (sensory afferent information) is limited in this direction may also make it difficult to anticipate the postural adjustments in most individuals with SCI. The results of Seelen et al. (30), who found no significant difference between individuals with SCI who have no paralysis or paresis of their low back and abdominal muscles and able-bodied individuals, strengthened our findings observed in the other directions. As their impairments were less than those experienced by individuals with a complete paralysis of their low back and abdominal muscles, the use of the U/Es as a compensatory strategy might be more effective. Therefore, the proposed tasks in the present study may not be difficult enough to differentiate between individuals with no paralysis or with paresis of their low back and abdominal muscles from able-bodied individuals. The same tasks performed either with unilateral U/E support or without U/E support with the U/Es crossed over chest, or performed at an increased speed (19) in a future study could reveal significant dynamic postural stability differences in other directions than a backward direction.
Study limitations
The results of this study should be interpreted cautiously given its limitations. Firstly, the fact that the participants’ hands were positioned on their thighs allowed them to use their U/Es to assist with the control of their trunk, especially when leaning forward. Thus, the present study does not totally isolate dynamic trunk stability within the context of seated postural stability. However, most of the participants with SCI could not have leaned in the proposed directions in a sitting position without the assistance of their U/Es (unsupported reaching). In fact, many individuals with SCI elect to anchor one U/E on a fixed object (i.e., wheelchair handle or backrest) to stabilize their trunk and prevent loss of balance or fall when leaning or reaching with the other U/E in daily life. A future study will evaluate multidirectional seated postural stability with only one hand positioned on the thighs and the other hand reaching in the proposed direction with the shoulder flexed to at least 90° to better reflect everyday activities and highlight the potential effect of hand dominance on multidirectional postural stability. This new experimental task will also challenge individuals with SCI as they will have to conciliate two key imperatives: generating enough strength to simultaneously stabilize their trunk while reaching with one U/E. Although the ideal task would be to perform isolated trunk postural control movements (e.g., spiral tracking task) as done in other populations (33), only a minority of individuals with SCI could successfully perform these tasks. Such an important limit justifies the exploration of alternative approaches to quantify the capability to stabilize the trunk in this population. Secondly, the fact that a real-time COP visual feedback was provided to indicate the desired COP trajectory during the tasks may have modified their performance as all participants were looking at the screen positioned in front of them. Thirdly, the statistical power of the study was limited by the small groups, the uneven distribution of individuals with SCI in both subgroups and the non-homogeneity of the subgroups, especially of the SCIAbdo subgroup. A future study should include a larger cohort and better balanced subgroups of individuals with tetraplegia, high paraplegia (no low back and abdominal muscles contraction) and low paraplegia (partial or complete low back and abdominal muscles contraction). Lastly, the fact that the multidirectional postural stability measures were not normalized based on participants’ characteristics (e.g., weight, trunk height, arm length, arm/trunk length ratio) also warrants consideration. Nevertheless, the fact that no significant difference was found between individuals with SCI and able-bodied individuals with respect to age, weight, total height known to potentially affect COP excursion and the area of the BOS supports the present results.
Conclusion
Multidirectional seated postural stability is reduced in individuals with SCI, particularly among those who have complete paralysis of their low back and abdominal muscles, in comparison to able-bodied individuals. Among individuals with SCI, the complete or incomplete preservation of their low back and abdominal muscles increased multidirectional seated postural stability to a level comparable to that reached by able-bodied individuals. The DSIs and the OSI may become useful outcome measures of multidirectional seated postural stability for rehabilitation professionals to characterize change over time or the impact of various treatments on multidirectional seated postural stability in clinical practice or in the context of research projects. Further research should define the test-retest reliability of the DSIs and of the OSI, as well as their construct validity using trunk muscle strength or kinematic measures, within a large cohort of individuals with SCI.
ACKNOWLEDGEMENTS
Special thanks are expressed to Professor Cyril Duclos, PhD, Michel Goyette, BSc, Eng, Pierre Desjardins, MScA, Eng and Daniel Marineau, DEC, for their intellectual, engineering and technical contributions that have enriched this project. Dany Gagnon holds a Junior 1 Research Career Award and Sylvie Nadeau a Senior Research Career Award from the Fonds de la recherche en santé du Québec (FRSQ). Cindy Gauthier received a Summer Research Award from the Quebec Rehabilitation Research Network (REPAR). Dany Gagnon, Sylvie Nadeau, Géraldine Jacquemin, Kei Masani and Milos Popovic are members of the Quebec-Ontario Spinal Cord Injury Mobility (SCI-MOB) Research Group financed by the Quebec Rehabilitation Research Network (www.repar.ca) and the Ontario NeuroTrauma Foundation (www.onf.org). The Pathokinesiology Laboratory was financed in part by the Canada Foundation for Innovation (CFI). The project was supported by the REPAR.
REFERENCES
