Manuela Karloh, MSc1,2, Marlus Karsten, PhD5, Fernanda V. Pissaia, PT1, Cintia L. P. de Araujo, PT1,3 and Anamaria F. Mayer, PhD1,3,4
From the 1Center of Assistance, Education and Research in Pulmonary Rehabilitation, 2Postgraduate Program in Human Movement Sciences, 3Postgraduate Program in Physiotherapy, 4Physical Therapy Department, Santa Catarina State University (UDESC), Florianópolis and 5Postgraduate Program in Rehabilitation Sciences, Federal University of Health Sciences of Porto Alegre (UFCSPA), Porto Alegre, Brazil
OBJECTIVE: The aim of this study was to investigate the physiological responses induced by the Glittre-ADL test (TGlittre) test in patients with chronic obstructive pulmonary disease (COPD) and compare them with those induced by the 6-minute walk test (6MWT).
DESIGN: Cross-sectional observational study.
SUBJECTS: Eighteen patients with COPD 66 years (standard deviation (SD) 8) and forced expiratory volume in 1 s of 40.4% (SD 16.8) predicted) who performed in randomized order the 6MWT and TGlittre on 2 separate days.
RESULTS: Baseline cardiopulmonary variables were similar between the 6MWT and TGlittre (p > 0.05). TGlittre induced slightly higher final VO2 than 6MWT 83.6 ml/min (SD 163.9); p < 0.05) and oxygen consumption (VO2) reached a plateau after the third lap during TGlittre. The other physiological variables, except respiratory exchange rate, were similar at the end of both tests (p > 0.05). All measured variables were significantly correlated between the 2 tests (p < 0.05).
CONCLUSION: TGlittre can induce slightly higher oxygen uptake than the 6MWT with similar cardiovascular and ventilatory demand and ventilatory efficiency.
Key words: pulmonary disease; chronic obstructive; outcome assessment; activities of daily living; oxygen consumption.
J Rehabil Med 2013; 45: 00–00
Guarantor’s address: Anamaria F. Mayer, Departamento de Fisioterapia, Centro de Ciências da Saúde e do Esporte (CEFID), Universidade do Estado de Santa Catarina (UDESC). Rua Paschoal Simone, 358. CEP 88080-350. Florianópolis, SC, Brazil. E-mail: anamaria.mayer@udesc.br
Accepted May 20, 2013; Epub ahead of print Oct 8, 2013
Introduction
Deterioration of functional capacity is a common manifestation in patients with chronic obstructive pulmonary disease (COPD) (1–3) and it plays an important role in their morbidity and mortality (3). The ability to perform activities of daily living (ADL) in these patients is better predicted by an integrative test than by tests focused on a single component of functional activities (4). In this regard, the 6-minute walk test (6MWT) has been widely used in assessing functional capacity (5–8). Although it reflects limitations in ADL performance (4), the 6MWT does not evaluate the influence on ADL limitation of upper limb work or activities other than walking (9). Unsupported upper limb activities are known to increase oxygen demand and lead to the consumption of much of the ventilatory reserve, which plays a role in ADL limitation among these patients (10).
Thus, to improve the assessment of functional capacity of patients with COPD, Skumlien et al. (9) developed the Glittre ADL-test (TGlittre), which is reproducible and responsive to a pulmonary rehabilitation programme. This test is characterized by activities such as sitting and rising from a chair, walking, climbing up and down stairs and performing activities with unsupported arms. Therefore, TGlittre can provide additional information about the ability to perform ADLs, especially in patients with more severe COPD (9). It can also differentiate the functional capacity of these patients from that of healthy subjects (11). TGlittre has shown a strong negative correlation with the 6MWT (9, 11), especially for patients who walk longer distances in the 6MWT (9). Furthermore, it has been observed that the time spent to complete the TGlittre correlated better than the 6MWT with some of the most impacting factors related to the disease prognosis, such as the severity of the disease, hospitalization rate and body mass index (9).
However, the magnitude of the physiological demands induced by the TGlittre on patients with COPD is still unknown in terms of metabolic, ventilatory and cardiovascular responses. Although both tests are self-paced and can assess the functional limitations of patients with COPD, it is hypothesized that the physiological response induced by the TGlittre might be different from that induced by the 6MWT. This could be mainly due to the differences in ergonomics and standard tasks performed. Since the TGlittre seems to be more specific for assessing ADL limitations, the physiological adjustments that occur during this test may more accurately reflect those that occur in the daily activities of patients. Therefore, the present study aimed to investigate the physiological responses induced by the Glittre-ADL test in patients with COPD and compare them with those induced by the 6MWT.
Methods
Participants
The study included Global Initiative for Chronic Obstructive Lung Disease (GOLD) stages 2, 3, and 4 (1) COPD patients with a history of smoking ≥ 20 pack-years, clinical stability in the 4 weeks prior to the study protocol, and age ≥ 40 years. Exclusion criteria were long-term oxygen therapy, current smoking, any pulmonary disease other than COPD, and comorbidities that would compromise their ability to perform any of the evaluations in the study. A total of 33 clinically stable COPD patients from the pulmonology outpatient services of public hospitals and private clinics were invited to participate in the study. Twelve out of 33 invited participants declined to take part in the study and 21 agreed to participate. Eighteen patients completed the study (14 men) and 3 were excluded: 2 due to inability to perform the proposed tests, and one for returning to smoking during the protocol.
The study was approved by the regional ethics committee for human research and all participants signed a written informed consent form.
Study design and protocol
Anthropometric and lung function assessments were carried out for all subjects (see supplemental digital content in Appendix SI (available from http://www.medicaljournals.se/jrm/content/?doi=10.2340/16501977-1217)). On the same day, patients underwent a familiarization trial for both the 6MWT and TGlittre. On 2 separate days, 1 week apart, 1 randomly selected test was performed: 6MWT or TGlittre. A symptom questionnaire was applied to determine clinical stability between the evaluations (12).
Physical activity in daily life
The quantification of physical activity in daily life was performed with an accelerometer-based activity monitor (DynaPort MiniMod; McRoberts BV, The Hague, The Netherlands). Patients were monitored as described previously (4) see Appendix SI.
Six-minute walk test
The 6MWT was performed according to the guidelines of American Thoracic Society (5). Peripheral oxygen saturation (SpO2; Oxi-Go, Oximeter Plus, New York, USA) and dyspnoea (Borg CR10 scale) (13) were measured at the beginning and end of the test. Predicted values for walking distance were calculated according to Iwama et al. (14).
Glittre ADL test
The TGlittre consists of completing a circuit while carrying a weighted backpack (2.5 kg for women, 5.0 kg for men). The circuit is as follows: from a sitting position, the patient stands up and walks along a flat 10-m long course; in the middle of which is a 2-step staircase (each step 17 cm high × 27 cm deep) to be traversed; after completing the second 5 m, the subject faces a shelf containing 3 objects, each weighing 1 kg, positioned on the top shelf (shoulder height) and moves them 1 by 1 to the bottom shelf (waist height) and then to the floor; the objects are then returned to the bottom shelf and finally to the top shelf again; the patients then walk back along the circuit, climbing and descending the stairs, until reaching the starting point (chair); sitting down and immediately beginning the next lap. Patients were instructed to complete 5 laps on this circuit as quickly as possible (9). SpO2 and dyspnoea (13) were measured at the beginning of the test, at the end of each lap and at the end of the test.
Physiological responses
During both functional capacity assessment protocols, patients were connected to a telemetric portable gas analyser (K4b2; Cosmed, Rome, Italy) to evaluate physiological responses. The device was calibrated according to the manufacturer’s recommendations. The following parameters were measured during the tests: breath-by-breath oxygen uptake (VO2), carbon dioxide output (VCO2), minute volume (VE) and respiratory exchange rate (RER), heart rate (HR), oxygen pulse (VO2/HR), ventilatory demand (VE/MVV), and ventilatory equivalent for oxygen uptake and carbon dioxide output (VE/VO2 and VE/VCO2, respectively) (8). Maximum voluntary ventilation (MVV) was calculated based on the equation forced expiratory volume in 1 s (FEV1) × 37.5 (15). Ventilatory efficiency was assessed by analysing the VE/VCO2 slope during both tests and was calculated from the beginning until the end of the tests. Predicted VE/VCO2 slope values were obtained using previously described equations (16). Other information regarding physiological response is available in Appendix SI.
Statistical analysis
The data were reported as means with standard deviations (SD). The Shapiro-Wilk test was used to analyse data normality. A paired t-test or the Wilcoxon test was used to compare both testing conditions (TGlittre and 6MWT). One-way repeated measures analysis of variance (ANOVA) was used to analyse variable response profiles during the tests. Pearson’s or Spearman’s correlation tests were performed to verify the association between physiological variables. Statistical significance was set at p < 0.05. Data analysis was performed with SPSS 20.0.
Sample size calculation
To calculate the sample size for the present study, we used the differences in VO2 between 6MWT and shuttle walk test (TShuttle) found by Casas et al. (8), an α = 0.05 and a power of 80%. Based on these parameters, the estimated number of patients who should complete the present study was of 18. Among the tests applied by Casas et al. (8), the TShuttle was considered for sample size calculation because it was the test that more closely resembles TGlittre regarding the length of the circuit.
Results
The patients had a mean age of 66 years (SD 8) and a FEV1 of 40.4% (SD 16.8) of the predicted value. The measured anthropometric and spirometric data are shown in Table I. Group characteristics divided by GOLD stages are set out in Appendix SI.
|
Table I. Characteristics of the study group |
|||
|
Mean (SD) |
Median |
95% CI |
|
|
Age, years |
66.00 (8) |
65.00 |
62.00–70.00 |
|
Smoking history, pack-years |
55.20 (33.4) |
47.50 |
38.60–71.80 |
|
GOLD 2, n |
5 |
||
|
GOLD 3, n |
6 |
||
|
GOLD 4, n |
7 |
||
|
Weight, kg |
74.70 (14.05) |
76.60 |
67.70–81.70 |
|
Height, m |
1.66 (0.73) |
1.67 |
1.63–1.70 |
|
BMI, kg/m2 |
27.04 (5.23) |
28.70 |
24.40–29.60 |
|
Body circumferences, cm |
|||
|
Thigh |
48.50 (5.38) |
47.90 |
45.80–51.10 |
|
Arm |
30.80 (3.44) |
31.10 |
29.10–29.10 |
|
FEV1/FCV, % |
0.47 (0.11) |
0.47 |
0.41–0.52 |
|
FEV1, l |
1.21 (0.53) |
1.16 |
0.95–1.48 |
|
FEV1, %pred |
40.40 (16.8) |
42.00 |
32.00–48.80 |
|
FCV, l |
2.49 (0.76) |
2.48 |
2.11–2.87 |
|
FCV, %pred |
65.20 (16.2) |
67.00 |
57.20–73.30 |
|
MVV, l/min |
46.50 (19.7) |
46.40 |
36.70–56.30 |
|
SD: standard deviation; 95% CI: 95% confidence interval; GOLD: Global Initiative for Chronic Obstructive Lung Disease; LL: lower limit; UL: upper limit; BMI: body mass index; FEV1: forced expiratory volume in 1 s; FVC: forced vital capacity; MVV: maximal voluntary ventilation; %pred: %predicted. |
|||
Characteristics of functional assessment
The mean time required to complete the TGlittre was 4.77 min (SD 1.46) (range 3.17–9.50 min) and the mean distance walked in the 6MWT was 469 m (SD 67) 81.1% (SD 22.3) [range 66.0–105.5%] of the predicted distance). Time spent in TGlittre was negatively correlated with distance walked in the 6MWT (r = –0.87, p < 0.01). Regarding physical activity in daily life, the patients spent a mean of 54.7% (SD 14.6) of the monitored time in a seated position, 20.0% (SD 5.5) standing, 13.1% (SD 6.0) walking and 12.4% (SD 12.3) lying down. The participants overall performed predominantly short walking periods lasting less than 1 min.
Physiological responses during Glittre ADL test
All variables showed significant changes compared with baseline values at the end of TGlittre (p < 0.05), except RER. All the physiological variables measured at TGlittre are shown in Table II. Baseline VO2 ranged from 192.5 to 453.9 ml/min, and final VO2 from 868.6 to 1,932.8 ml/min. Patients reached a mean of 86.9% (SD 33.2) of MVV. VE/VCO2 slope during TGlittre was 28.6 (SD 5.01), which was slightly higher 3.4% (SD 17.4) than predicted value. VO2 reached a plateau after the third lap and no significant changes were observed after that (1,265.3 (SD 255.7), 1,292.5 (SD 293.5), 1,329.2 (SD 314.4) ml/min at third, fourth and fifth laps, respectively, p > 0.05). During the last 2 laps, VO2 changed less than 7% (6.34% (SD 18.6%)). It is worth noting that VCO2 reached a plateau only in the last lap. Individual and mean group VO2 data are shown in Figs 1B and 1D, respectively. VCO2, VE, HR and SpO2 profiles are shown in Fig. 2. Final VO2 was not related to the GOLD stage (p > 0.05).
|
Table II. Comparison between functional capacity tests |
|||||||||
|
Rest |
Finala |
∆ |
|||||||
|
6MWT |
TGlittre |
p-value |
6MWT (6th min) |
TGlittre (5th lap) |
p-value |
6MWT |
TGlittre |
p-value |
|
|
Mean (SD) |
Mean (SD) |
Mean (SD) |
Mean (SD) |
||||||
|
SpO2, % |
96.7 (1.49) |
96.6 (1.67) |
0.73 |
90.2 (6.3) |
91.6 (4.54) |
0.08 |
–4.76 (3.65) |
–6.50 (5.43) |
0.06 |
|
RR, bpm |
19.1 (4.58) |
20.1 (4.17) |
0.24 |
28.5 (4.60) |
29.3 (5.14) |
0.29 |
9.45 (2.88) |
9.22 (2.98) |
0.82 |
|
VT, L |
0.68 (0.18) |
0.66 (0.19) |
0.69 |
1.23 (0.34) |
1.22 (0.28) |
0.80 |
0.56 (0.27) |
0.57 (0.18) |
0.88 |
|
VE, L/min–1 |
12.1 (2.41) |
12.5 (2.66) |
0.52 |
34.3 (7.26) |
35.0 (6.32) |
0.53 |
22.2 (7.12) |
22.4 (5.26) |
0.86 |
|
VO2, ml/min |
308.5 (65.7) |
321.5 (108.3) |
0.95 |
1,245.7 (3,24.1) |
1,329.2 (3,14.4) |
0.04 |
937.2 (310.1) |
1,007.7 (315.1) |
0.16 |
|
VO2/kg, ml/min/kg |
4.27 (1.01) |
4.39 (1.32) |
0.98 |
17.00 (3.86) |
18.1 (3.30) |
0.04 |
12.7 (3.57) |
13.7 (3.65) |
0.15 |
|
VCO2, ml/min |
250.4 (53.2) |
260.3 (75.9) |
0.64 |
1,019.8 (292.1) |
1,029.1 (224.2) |
0.82 |
769.4 (284.8) |
768.8 (210.0) |
0.99 |
|
VE/VO2 |
36.9 (5.58) |
37.8 (8.25) |
0.50 |
26.7 (4.39) |
25.9 (4.75) |
0.13 |
–10.0 (5.39) |
–11.9 (7.54) |
0.27 |
|
VE/VCO2 |
45.9 (8.57) |
46.3 (9.37) |
0.71 |
32.9 (4.51) |
33.1 (4.73) |
0.87 |
–12.9 (7.17) |
–13.2 (7.54) |
0.88 |
|
RER |
0.81 (0.07) |
0.82 (0.08) |
0.84 |
0.82 (0.07) |
0.78 (0.07) |
0.01 |
0.00 (0.09) |
–0.04 (0.10) |
0.14 |
|
HR, bpm |
79.2 (14.8) |
82.6 (12.9) |
0.29 |
113.8 (15.8) |
116.2 (13.2) |
0.91 |
34.6 (10.8) |
34.0 (12.2) |
0.95 |
|
O2 pulse, VO2/HR |
4.03 (1.19) |
3.91 (1.13) |
0.89 |
11.0 (2.35) |
11.6 (2.60) |
0.20 |
6.92 (2.03) |
7.67 (2.71) |
0.16 |
|
VE/MVV |
0.32 (0.17) |
0.32 (0.15) |
0.98 |
0.85 (0.36) |
0.87 (0.33) |
0.32 |
0.53 (0.23) |
0.55 (0.20) |
0.55 |
|
aFinal values refer to the average of the last 15 s of both the last minute of 6MWT (6th minute) and the last lap of TGlittre (5th lap). 6MWT: 6-minute walk test; TGlittre: Glittre activities of daily living-test; ∆: change (final – rest values); SpO2: oxygen saturation pulse oximetry; RR: respiratory rate; VT: tidal volume; VE: minute ventilation; VO2: oxygen uptake; VCO2: carbon dioxide output; VE/VO2: ventilatory equivalent for oxygen; VE/VCO2: ventilatory equivalent for carbon dioxide; RER: respiratory exchange ratio; HR: heart rate in beats per minute; MVV: maximal voluntary ventilation. p: significance level between tests (6MWT and TGlittre) |
|||||||||
Comparison between the Glittre ADL test and the 6-minute walk test
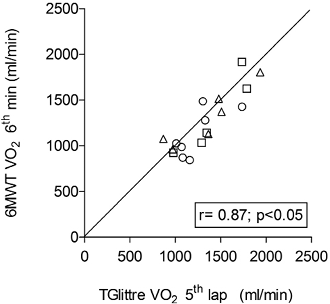
Baseline cardiopulmonary variables were similar between the 6MWT and TGlittre (p > 0.05). Both VO2 and RER were significantly higher during TGlittre (p < 0.05). VO2 values for the 6MWT are shown in Figs 1A and 1C. Fig. 3 shows the correlation plot for final VO2 between tests. All measured variables were significantly correlated between the tests (p < 0.05; see Appendix SI).
Fig. 1. Oxygen consumption (VO2) during the 6-minute walk test (6MWT, left) and Glittre activities of daily living-test (TGlittre, right). (A and B) Individual data; (C and D) mean group data (standard deviation). NS: not significant.
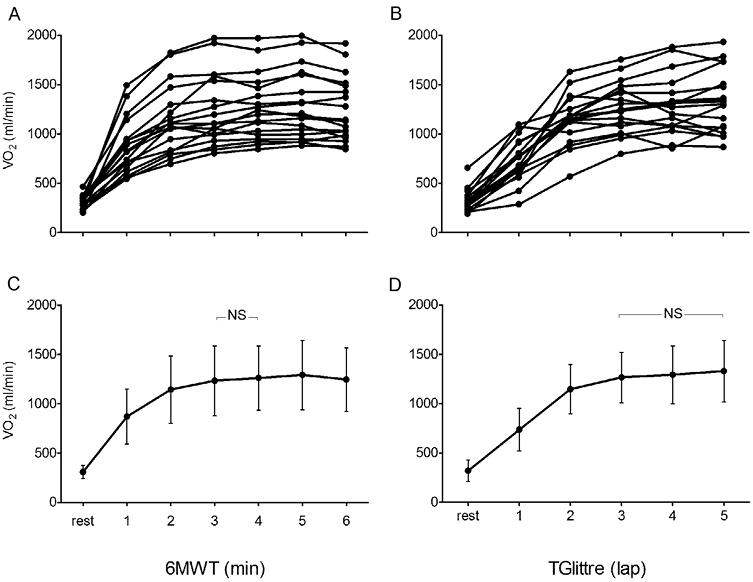
Fig. 2. Cardiopulmonary responses during the 6-minute walk test (6MWT, left) and Glittre activities of daily living-test (TGlittre, right). (A) mean group data (standard deviation; SD) for carbon dioxide production (VCO2); (B) mean group data (SD) for minute ventilation (VE); (C) mean group data (SD) for heart rate (HR); (D) mean group data (SD) for oxygen saturation (SpO2); NS: not significant.
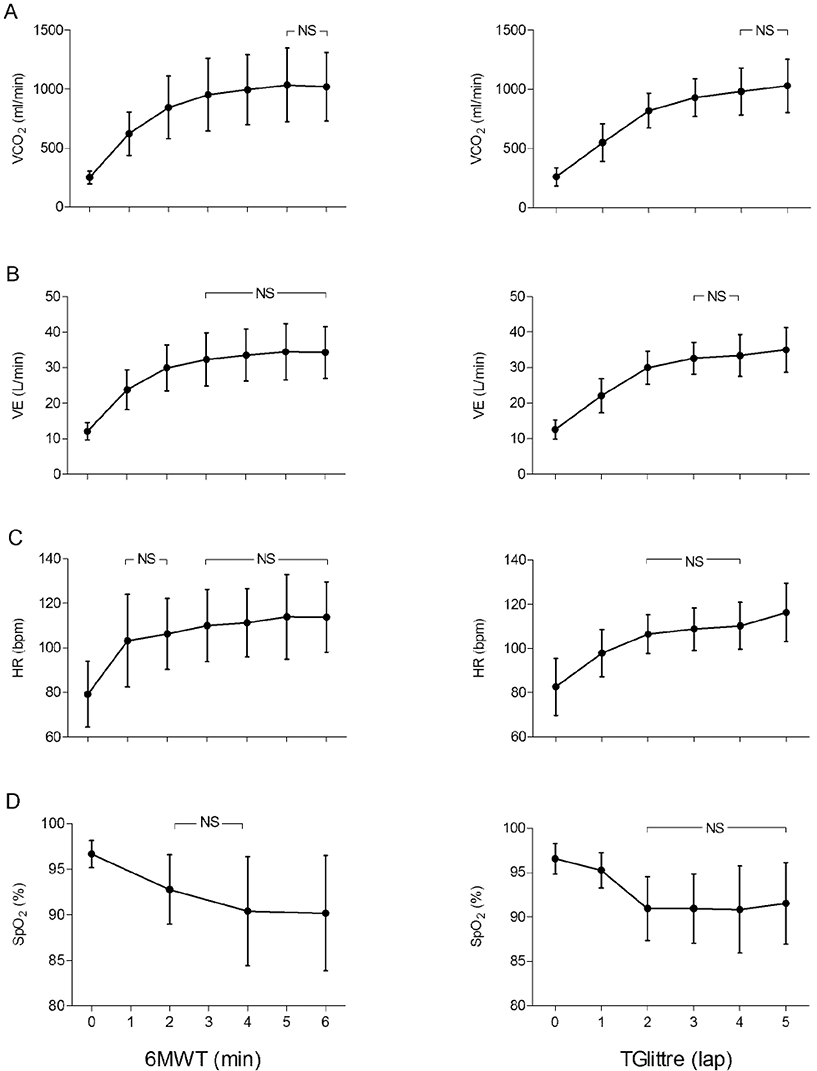
Fig. 3. Correlation plot of final VO2 between the 6-minute walk test (6MWT) and Glittre activities of daily living-test (TGlittre). r = 0.87; p < 0.05. □ Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2; ∆ GOLD 3; ○ GOLD 4.
Discussion
The main finding of this study is that in a group of moderate to very severe COPD patients with a sedentary lifestyle but, on average, no evidence of severe functional impairment, TGlittre led to a slightly higher oxygen uptake, but similar ventilatory and cardiovascular responses to the 6MWT.
The metabolic, ventilatory and cardiovascular responses to exercise have been studied in COPD patients undergoing different walking test protocols, such as the 6MWT (6–7, 17), the shuttle walk test (7–8, 17) and ADL-test (18). Previous studies have reported that the 6MWT leads to similar VO2 to that induced by incremental exercise protocols, but with lower VE, VCO2, RER and blood lactate concentration. Thus, the 6MWT is capable of generating a high, but submaximal, physiological requirement (6, 8, 17, 19). A plateau in VO2 after the third minute of the 6MWT (6, 17, 19) and after the first 2 or 3 min of an ADL-based test (18) was shown previously. This suggests that patients choose a nearly constant activity speed in order to reach a sustainable workload during self-paced tests. Casas et al. (8) confirmed that COPD patients assume a constant speed in 6MWT that is equivalent to the maximum sustainable load and critical walking speed. Both VO2 plateau and self-selection of maximum sustainable speed reflect the integrated response of the involved systems in oxygen transport and utilization and may explain the high prognostic value of submaximal tests (8, 20).
The current study showed that 13 of the 18 patients experienced higher VO2 during TGlittre than during the 6MWT, and that this occurred independently of GOLD stage (Fig. 3). Metabolic demand and energy expenditure during ADLs had been studied only in an isolated way (10, 21, 22), not integrated, as in TGlittre. In a study comparing 5 isolated activities, based on the TGlittre protocol, performed for 1 min each, it was shown that climbing up and down stairs generates higher energy expenditure than walking and causes a greater dyspnoea and fatigue (21). Otherwise, moving objects onto and off a shelf, using unsupported arms, was the activity in which patients with COPD had the lowest energy expenditure (21). However, we observed in a pilot study analysing video-recordings (unpublished data) that, during TGlittre, patients spent 50–65% of one lap only in the activity of moving these objects on and off the shelf with unsupported arms, which could have lead to an increase in metabolic demand. Velloso et al. showed that moving weighted pots, which is an activity similar to that performed in TGlittre, was the ADL that induced higher VO2 in COPD patients (10). Thus, the slightly higher VO2 observed in TGlittre in the present study may be associated with the involvement of a greater number of muscle groups, since it adds other ADL-based activities besides walking. Also, during the TGlittre tasks that require unsupported upper limb movements, the accessory muscles of inspiration are recruited to participate in primary motor action (23). Evidence suggests that higher respiratory muscle work and fatigue compromise blood flow to postural and gait muscles, probably contributing to a further increase in metabolic demand.
Oxygen uptake reached a plateau after the third lap of TGlittre, which occurred close to the third minute of the test. This profile throughout TGlittre was similar to the steady-state response reached after the third minute of the 6MWT (6, 17, 19) and the second to third minute of and ADL sit-walk test (18). Despite this, individual VO2 profiles were irregular throughout the TGlittre (Fig. 2). This pattern may be explained by the activity variation during this test, including moments without horizontal displacement or without any work (e.g. sitting), even if for a short period of time. ADLs are mostly irregular in nature, intensity and duration, and are therefore (17) rarely associated with steady-state conditions (24), reinforcing the specificity of TGlittre for evaluating activities of daily living.
The ventilatory demand during exercise was similar in both tests. It was observed that patients reached high values during both tests. This may have prevented better performance and consequently additional VO2 increments. Previous findings (10, 18) also demonstrated that COPD patients use a large part of the ventilatory reserve during ADLs, reflecting the role of ventilatory limitation in their functional and exercise capacity. Palange et al. (25) demonstrated that patients with COPD have less ventilatory efficiency and gas exchange during a shuttle walk test than a maximal incremental test on a bicycle. While walking and during upper limb activities, the involved muscles are activated and send reflex impulses to the respiratory centre, causing thoraco-abdominal dyssynchrony (23). On the other hand, fixed and supported arm activities (e.g. cycling) seem to reduce the upper limb contribution to respiratory stimulation by neurogenic reflex, as a result, being less detrimental to ventilatory efficiency (25). Although it could have been assumed that ventilatory efficiency would be lower during TGlittre, since it involves unsupported upper limb activities, no difference was observed in VE/VCO2 slope between tests.
To our knowledge, this is the first study demonstrating the physiological responses of COPD patients to TGlittre. This adds value and usefulness to the TGlittre, which yields information complementary to the 6MWD in functional assessment of patients with COPD due to the fact that it involves activities other than walking, which makes it useful in the clinical setting for both the prescription and outcome evaluation of pulmonary rehabilitation programmes.
Some limitations of this study should be made clear. Although the sample size was sufficient, a relatively small number of patients was included in the study. The results, however, were consistent within these patients and thereby seem to be representative for this group. We preferred to study a wide range of airflow obstruction (GOLD 2–4), even if it represents a small number of patients for each GOLD stage, because FEV1 itself is not considered the best predictor for functional capacity in these patients (4). Another possible limitation of the present study is related to the fact that a maximal incremental exercise test was not performed. This would have determined the maximum or peak values of metabolic, ventilatory and cardiovascular variables, which could have been used as a parameter for comparing the 6MWT and TGlittre, and obviated the use of prediction equations, which can often under- or over-estimate measured values. However, the 6MWT was chosen because it is considered the most widely used functional capacity and exercise test in clinical and scientific protocols (5) and, so far, is the only test for which a correlation with TGlittre has been demonstrated (9). In addition, the 6MWT and TGlittre seem to impose a similar workload. Another potential limitation was the exclusion of patients receiving long-term oxygen therapy, since the coupling of an external oxygen source would have changed the cardiorespiratory response results. For that reason, the physiological responses to TGlittre in patients with severe gas exchange impairment remain unclear. Also, as the study protocol excluded COPD current smokers the results should not be generalized for this group of patients.
In conclusion, TGlittre can induce a slightly higher oxygen uptake than the 6MWT, which is probably related to the characteristics of the activities performed during the test and to the greater muscle demand. However, the higher oxygen uptake was achieved with similar cardiovascular and ventilatory demand and no difference in ventilatory efficiency.
AcknowledgEments
The authors would like to thank those who supported the data acquisition, all the pulmonologists who referred patients to the study protocol, and the Foundation for Support of Scientific and Technological Research in the State of Santa Catarina/National Council of Technological and Scientific Development FAPESC/CNPq for funding this study.
Disclosures
This research was funded by Foundation for Support of Scientific and Technological Research in the State of Santa Catarina/National Council of Technological and Scientific Development FAPESC/CNPq [3509/2010-2], Brazil.
The authors declare that they have no potential conflicts of interest to disclose.
References
