Tomás Gallego Izquierdo, PT, PhD1, Daniel Pecos-Martin, PT, PhD1, Enrique Lluch Girbés, PT2,3,4,5, Gustavo Plaza-Manzano, PT, PhD6, Ricardo Rodríguez Caldentey, PT1, Rodrigo Mayor Melús, PT1, Diego Blanco Mariscal, PT1 and Deborah Falla, PT, PhD7,8
From the 1Department of Physical Therapy, University of Alcalá, Alcalá de Henares, Madrid, 2Department of Physical Therapy, Faculty of Physiotherapy, University of Valencia, Spain, 3Departments of Human Physiology and Physiotherapy, Faculty of Physical Education & Physiotherapy, Vrije Universiteit Brussel, 4Department of Physical Medicine and Physiotherapy, University Hospital Brussels, Belgium, 5Pain in Motion Research Group, www.paininmotion.be, 6Department of Medicine, University Complutense of Madrid, Madrid, Spain, and 7Pain Clinic, Center for Anesthesiology, Emergency and Intensive Care Medicine, University Hospital Göttingen, Göttingen, and 8Institute for Neurorehabilitation Systems, Bernstein Center for Computational Neuroscience, University Medical Center Göttingen, Georg-August University, Göttingen, Germany
OBJECTIVE: To compare the effects of cranio-cervical flexion vs cervical proprioception training on neuromuscular control, pressure pain sensitivity and perceived pain and disability in patients with chronic neck pain.
METHODS: Twenty-eight volunteers with chronic non-specific neck pain were randomly assigned to 1 of 2 interventions and undertook 6 physiotherapist-supervised sessions over a period of 2 months. Both groups performed daily home exercise. Performance on the cranio-cervical flexion test, pressure pain thresholds and reported levels of pain and disability were measured before and immediately after the first treatment session, 1 month after starting treatment and 2 months after starting treatment (at completion of the intervention).
RESULTS: At 2 months, both groups improved their performance on the cranio-cervical flexion test (p < 0.05), but this did not differ between groups (p > 0.05). Both groups showed a reduction in their pain at rest and disability at 2 months, but this was also not different between groups (p > 0.05). Pressure pain sensitivity did not change for either group.
CONCLUSION: Both specific cranio-cervical flexion training and proprioception training had a comparable effect on performance on the cranio-cervical flexion test, a test of the neuromuscular control of the deep cervical flexors. These results indicate that proprioception training may have positive effects on the function of the deep cervical flexors.
Key words: neck pain; proprioception; exercise; intervention.
J Rehab Med 2016; 00: 00–00
Correspondence address: Deborah Falla, Pain Clinic, Center for Anesthesiology, Emergency and Intensive Care Medicine University Hospital Göttingen, Robert-Koch-Str. 40, DE-37075 Göttingen, Germany. E-mail: deborah.falla@bccn.uni-goettingen.de
Accepted Aug 27, 2015; Epub ahead of print Nov 26, 2015
INTRODUCTION
A myriad of sensorimotor disturbances have been identified in people with chronic neck pain (1, 2). Consequently, a pragmatic multimodal intervention approach has been recommended to address changes in sensorimotor control (2, 3), since no approach in isolation has been shown to address all aspects of sensorimotor function. As an example, impaired proprioception and postural control is a feature of some patients with neck pain, and several treatment approaches have been proposed to directly address these impairments, such as head-neck awareness exercises (i.e. training of joint position sense with head relocation), oculomotor exercises (i.e. gaze stability, eye-neck coordination) or balance training (4). These programmes lead to enhanced sensorimotor control and reduced neck pain and disability (5–7). However, it is not known if this training approach also has an effect on other aspects of neuromuscular function in people with neck pain. For instance, there is evidence for a high prevalence of increased activation of the sternocleidomastoid muscle in people with neck pain (8, 9) and reduced activation of deeper cervical flexor muscles has commonly been associated with this augmented activity (8, 10). Altered coordination between the deep and superficial flexor muscles is reflected as poor performance on the cranio-cervical flexion test (CCFT), a clinical test used to evaluate neuromuscular control of the deep cervical flexors (11).
Typically specific proprioceptive training regimes are designed to target the deep muscles, especially the suboccipital muscles (7), since they have the highest density of receptors (12) and are known to have a specific role in reflex and central connections to the vestibular, visual and postural control systems (13). It is not known whether this training approach has a beneficial effect on the control of other muscles, such as the coordination between the deep and superficial cervical flexors. Especially considering that the deep cervical flexor muscles (e.g. longus colli) also have a relatively high density of muscle spindles (12).
One form of exercise that has been advocated for addressing impaired neuromuscular control of the cervical flexor muscles is cranio-cervical flexion (CCF) training, which aims to enhance activation of the deep cervical flexor muscles and restore coordination between the deep and superficial cervical flexors (14). Clinical trials examining the effectiveness of this exercise regime have demonstrated positive outcomes in terms of reduction in neck pain and disability, improvement in sitting posture and enhanced neuromuscular control of the cervical flexor muscles (7, 14–21). Interestingly, CCF training also improved proprioceptive acuity of the neck (7), indicating that proprioception can be enhanced with specific exercise.
The primary aim of this study was to compare the effects of conventional cervical proprioception training vs CCF training on cervical flexor muscle function, measured through performance on the CCFT, in patients with chronic non-specific neck pain, in order to evaluate whether proprioception training can achieve a beneficial effect on neuromuscular control of the cervical flexor muscles. Besides effects on neck muscle function, the impact of the 2 exercise programmes on patient self-reports of pain and disability and neck muscle hyperalgesia was explored. In addition to evaluating the effects after 2 months of training, we were interested in understanding how rapidly improvements can be seen. Thus, we included measures immediately after the first session of exercise, after the first month of exercise and after 2 months when the exercise programme was completed. This was based on earlier work showing immediate positive effects of specific neck training on performance on the CCFT (22).
METHODS
Participants
Twenty-eight subjects (18 women) with a history of chronic non-specific neck pain, greater than 3 months’ duration, participated in the study. The sample size was calculated using G*Power 3.0.18 Software (23) based on the CCFT score as the primary outcome measure. The effect size for the CCFT was determined as 0.25 and the correlation between repeated measurements assumed at 0.5. Assuming 4 measurements (pre-session, post-session 1, 1 month after starting treatment, and 2 months after starting treatment (i.e. after completion of treatment)) in the 2 groups, the correction of sphericity was determined as 0.5. With a statistical power of 0.80 and an alpha level of 0.05, a total sample size of 24 patients was estimated. An allowance was made for a 15% drop-out rate, increasing the sample size to 28 patients (14 per group).
Participants were recruited via advertisements during the period January to June 2014. Inclusion criteria were: age between 18 and 55 years, score ≤ 15/50 on the Neck Disability Index (NDI) (24), showing signs of cervical movement control dysfunction (25), and manual physical examination revealing muscle tenderness. A cervical movement control dysfunction was defined as the presence of aberrant or uncontrolled movements of the cervical spine observed during prescribed active movements of the neck and/or upper limb (25).
Subjects were excluded if they had vascular, neoplastic or vestibular disease, a diagnosis of fibromyalgia or rheumatoid arthritis, or any medical condition that prevented exercise.
The study was approved by the ethics committee of the University of Alcalá, Spain and procedures were conducted according to the Declaration of Helsinki. The study was registered in Clinical Trials database (NCT 022258730). Patients were informed orally and in writing about the procedures. Written informed consent was provided before participation.
Interventions
This study was a randomized controlled clinical trial, with parallel groups and a blinded assessor. It was guided according to the CONSORT Statement. Patients were randomized into 2 exercise groups: CCF training and proprioception training (Fig. 1). Randomization was performed using computer-generated random numbers (Epidat® version 3.1). Concealment of allocation was ensured using sequentially numbered opaque, sealed envelopes. Patients in each group received 6 physiotherapist-supervised sessions distributed within a 2 month-period by the same physical therapist with 5 years of experience. The first session was delivered immediately after the baseline assessment, the second and third sessions were 1 and 2 weeks after the baseline assessment, respectively, and the following 3 sessions were given once every 2 weeks for the remainder of the training duration (i.e. 4th, 6th and 8th week).
Exercise sessions lasted a maximum of 45 min. All the subjects received an exercise diary and were requested to practice twice per day for the 2 month-period of the study. Participants were instructed to perform their exercise in the same way that they were instructed during their supervised sessions. The exercise session at home took no longer than 20 min per day and no provocation of pain was permitted. Participants were advised not to receive any other specific treatments for neck pain, although their usual medication was not withdrawn.
Performance on the CCFT, pressure pain threshold (PPT) over cervical muscle sites and levels of pain and disability, were measured before and immediately after the first treatment session, 1 month after starting treatment and 2 months after starting treatment, when the intervention was completed.

Fig. 1. Participant flow and retention. CCF: cranio-cervical flexion.
Cranio-cervical flexion training. Low load training of the cranio-cervical flexor muscles followed the protocol described by Jull et al. (3). This exercise specifically targets the deep flexor muscles (longus capitis and longus colli), whilst aiming to minimize the activation of the superficial flexor muscles (sternocleidomastoid and anterior scalene). Initially, patients were taught to perform the CCF movement slowly and in a controlled manner in a supine position, with the head and neck in a neutral position. Once the correct CCF motion was achieved, subjects began to hold progressively increasing ranges of CCF using feedback from an air-filled pressure sensor (Stabilizer™, Chattanooga Group Inc., Tennessee, USA) placed behind the neck. The patient initially performed CCF to sequentially reach 5 pressure targets in 2 mmHg increments from a baseline of 20 mmHg to the final level of 30 mmHg. The physiotherapist identified the target level that the patient could hold steadily for 5 s without resorting to retraction, without dominant use of the superficial neck flexor muscles, and without a quick, jerky cranio-cervical flexion movement. Training commenced at this target level. For each target level, the contraction duration was increased to 10 s, and the subject trained to perform 10 repetitions with brief rest periods between each contraction (~3–5 s). Once one set of 10 repetitions of 10 s was achieved at one target level, the exercise was progressed to train at the next target level up to the final target of 10 repetitions of 10 s at 30 mmHg.
The exercise load prescribed to each patient was based on their assessment performance. Patients were not given a pressure biofeedback unit for home training, but they were taught in the clinic to replicate their training pressure level by performing several repetitions to reach the target without visual feedback from the dial. The training load of each patient was adjusted at each session.
Proprioceptive training. Patients trained cervical proprioception following the protocol described by Revel et al. (5, 26). This regime consisted of exercises of head relocation, eye-follow, gaze stability and eye-head coordination. For head relocation exercises, subjects started in a sitting position, with a laser attached to a helmet at the apex of their head, and a target located at eye level on a wall 90 cm away. This was established as the natural head posture. Subjects then practiced relocating their head to the natural head posture after active neck movements, first with eyes open using feedback from the laser attached to their head, then with pupillary glasses preventing pupillary excursion, and finally with their eyes closed. All active movements of the cervical spine (flexion, extension, rotation, lateral flexion) were performed.
Oculomotor exercises were progressed through several stages. First, eye movement following a target located at a comfortable distance was practiced with the head stationary, progressing to movements of the head with visual fixation on a target (i.e. gaze stability). Pupillary glasses were used in the clinic to ensure a steady gaze during this exercise. Eye-head coordination exercises started with rotation of the eyes and head to the same side, both left and right. After that, patients practiced following a target with the eyes first, followed by the head, ensuring that they maintained focus on the target. As a further progression, the eyes moved first, and then the head, to look between 2 targets positioned horizontally or vertically, and finally, the eyes and head rotated in opposite directions, both left and right. All these exercises were progressed by increasing the speed and range of motion of the target and with patients in a standing position.
Outcome measures
The main outcome measure for this study was performance on the CCFT. The secondary outcome measures were patient-reported levels of pain and disability and PPT. The assessor, who was blinded to subject group for the outcome assessments, was a physical therapist with 3 years of clinical experience in outpatient orthopaedic practice with a Master’s degree in physical therapy.
Performance on the cranio-cervical flexion test. The assessor identified the target level (22–30 mmHg) that the subject could hold steadily for 5 s using the correct CCF action. Secondly, the assessor evaluated the number of repetitions of a 10 s hold that the patient could perform at their target level. Performance on the CCFT was scored as the pressure level that the patient was able to achieve (activation score) multiplied by the number of repetitions they could perform. For example, if a patient could achieve the second level of the test (24 mmHg) and perform 6 10-s holds with the correct action of CCF, then the performance index was 4 × 6 = 24. The performance index ranged from 0 to 100.
Pressure pain thresholds. PPT were recorded bilaterally over the levator scapulae, upper trapezius, splenius capitis, sternocleidomastoid and anterior scalene muscles at the points of greatest hyperalgesia. The hyperalgesic points were considered for assessment if a nodule within a taut band of skeletal muscle was palpated, pressure over the muscle fully or partially reproduced the usual pain experienced by the subject and full muscle stretching was restricted (27).
To ensure repeatability of location for the subsequent assessment sessions, the distance to the hyperalgesic points from the spinous process of C7 (for the upper trapezius), the mastoid process (for the sternocleidomastoid, splenius capitis and levator scapulae) and the middle third of the clavicle (for the anterior scalene), was measured. Testing sites were also marked and photographed as this has been shown to improve the reliability of PPT measurements (28).
The PPT was measured using an analogue algometer (Force Dial model FDK 20, Wagner Instruments, Connecticut, USA), with a surface area at the round tip of 1cm2. The algometer probe tip was applied perpendicularly to the skin at a rate of 1kg/cm2/s. PPT was measured at each site with a 30 s rest period between each measurement. A familiarization phase preceded the formal measurements where participants were instructed on the procedure and the examiner practiced with them at a remote site (forearm). Subjects were instructed to indicate the moment when pressure changed to pain, which correspond to the definition of the PPT. The same researcher performed the PPT measurements in all subjects and was blinded to purpose of the study.
Four consecutive PPT measures were performed at each location with 30 s of rest between measurements. The first PPT measure was discarded and the mean of the subsequent 3 PPT measures was used for further analysis.
Pressure algometry is a valid and reliable method to measure PPT (29), with studies showing good repeatability of measurements on the neck muscles (intracorrelation coefficient 0.78–0.93) (30).
Measures of pain and disability. Neck pain intensity was measured on a 10-cm visual analogue scale (VAS), anchored with “no pain” and “the worst pain imaginable”. Patients were requested on each assessment to complete a triple VAS: their worst or maximal pain experienced during the last 2 weeks (maximum VAS), their least or minimum pain experienced during the last 2 weeks (minimum VAS), and current pain at rest (current VAS). The Spanish version of the Neck Disability Index (NDI) questionnaire was used to assess perceived pain and disability related to neck pain (31, 32).
Data analysis
Data were analysed using the statistical package SPSS 21.00 for Windows. Statistical significance was set at p < 0.05. In order to analyse the effectiveness of the 2 interventions, an intention-to-treat analysis was performed. The existence of differences between groups in the dependent variables was determined. Four measurements were performed: baseline (pre), immediately after the first treatment session (post session 1), 1 month after commencement of treatment (post month 1), and 2 months after commencement of treatment when the intervention was completed (post month 2). For comparison between groups, a variable defined as “difference” was calculated for each dependent variable, by subtracting pre-test and post-test.
Prior to statistical comparisons, all data were tested for normal distribution by the Shapiro-Wilk test. Then, a descriptive analysis of the data was obtained for the dependent variables in the pre, post session 1, post month 1 and post month 2 measurements, and for the variable “difference”. In those analyses, mean and standard deviation (SD) were shown for dependent variables normally distributed. For those variables that did not conform to normal, the data were expressed as median and first and third quartiles.
Subsequently, homogeneity of the 2 intervention groups was studied using the Student’s t-test for independent samples. For values that did not conform to normal, the Mann-Whitney U test was applied. For the variable sex, homogeneity was studied through Pearson’s χ2 test or the Fisher’s exact test, in case the former could not be used.
To determine whether there were differences in each group, considering each group in isolation, between the 4 assessments (pre, post session 1, post month 1 and post month 2) in each of the variables, repeated measures analysis of variance (ANOVA) was used. ANOVA was complemented with Simple and Helmert contrasts in those variables where the 4 assessments presented a data distribution similar to normal. Friedman ANOVA together with multiple comparisons tests were used when variables were not normally distributed.
To determine whether there were differences in the dependent variables between the 2 intervention groups, the Student’s t-test for independent samples was used. In those following normal, the effect size was calculated according to the formula d = 2t/√g. For the variables that did not conform to normal, this analysis was performed using the Mann-Whitney U test and the estimated effect size according to Grissom’s procedures.
RESULTS
The study flow diagram is shown in Fig. 1. A total of 34 patients were screened for eligibility. Six participants were excluded as they failed to fulfil the necessary criteria for inclusion. A final total of 28 (18 women, 10 men) participants were included. Participants were randomized into 2 groups: CCF training (n = 14) and proprioception training (n = 14). There were no drop-outs during the study period. All participants completed the 6 physiotherapist-supervised sessions and verbally confirmed that they complied with the home-exercise programme.
Baseline characteristics of the CCF and proprioception training groups are presented in Table I. There were no significant differences in baseline variables between groups (all p > 0.05).
|
Table I. Baseline characteristics of the variables for the cranio-cervical flexion and proprioceptive training groups |
|||
|
CCF training (n = 14) |
Proprioception training (n = 14) |
p-value |
|
|
Age, years, mean (SD) |
28.43 (6.16) |
29.93 (7.34) |
0.56 |
|
Weight, kg, mean (SD) |
65.87 (12.80) |
62.50 (9.51) |
0.43 |
|
Height, cm, mean (SD) |
167 (0.08) |
168 (0.60) |
0.73 |
|
BMI, kg/m2, mean (SD) |
23.68 (3.97) |
22.04 (0.76) |
0.22 |
|
CCFT, median (IQR) |
10 (2.0, 25.0) |
11 (2.0, 20.8) |
0.35 |
|
NDI (0–50) mean (SD) |
7.71 (2.78) |
7.42 (2.87) |
0.79 |
|
VAS at rest (0–10 cm), median (IQR) |
3.45 (2.95, 4.35) |
4.00 (2.66, 4.62) |
0.48 |
|
VAS maximum (0–10 cm), median (IQR) |
5.90 (4.40, 7.00) |
5.00 (3.26, 6.40) |
0.22 |
|
VAS minimum (0–10 cm), median (IQR) |
0.22 (0.00, 0.77) |
1.00 (0.00, 2.10) |
0.12 |
|
IQR: interquartile range; SD: standard deviation; CCF: cranio-cervical flexion; BMI: body mass index; CCFT: cranio-cervical flexion test; NDI: Neck Disability Index; VAS: visual analogue scale. |
|||
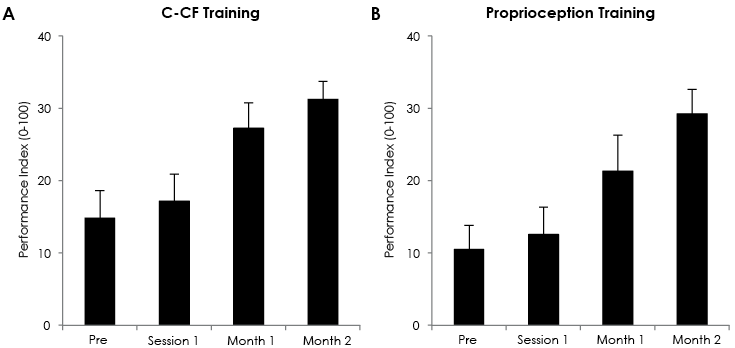
Cranio-cervical flexion test performance
Fig. 2 shows the performance index on the CCFT for each group at each time-point. For the CCF training group, significant differences were observed between post month 2 and baseline (p < 0.01). The proprioception training group showed significant differences in the performance index on the CCFT at both post month 1 and post month 2 compared with baseline (p < 0.01).
Pressure pain thresholds
Fig. 3 presents the PPT for each group at each time-point. Both groups showed a significant increase in the PPT over the right anterior scalene muscle from baseline to post month 2. In addition, the proprioceptive training group showed an increase in the PPT over the right upper trapezius (p < 0.05), right splenius (p < 0.05) and right elevator scapulae (p < 0.05) at post month 2 compared with baseline. No within-group differences were found for the rest of the variables.
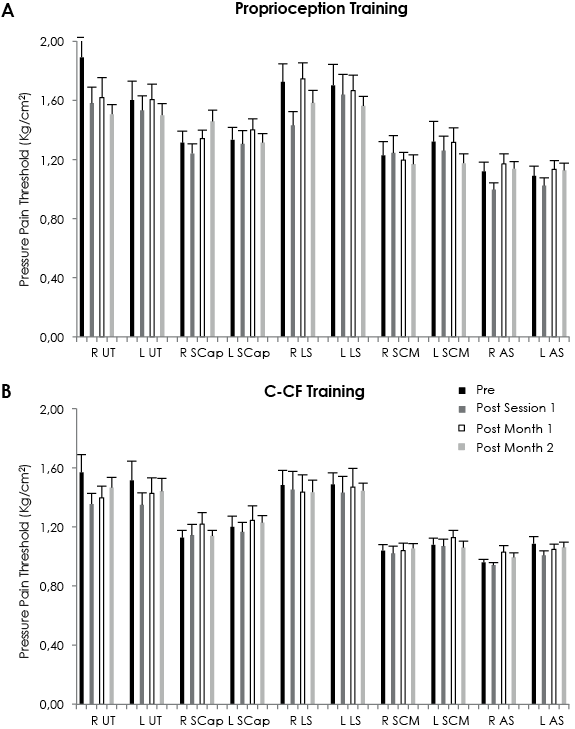
Fig. 3. Pressure pain thresholds for cranio-cervical flexion (CCF) and proprioception training groups at each measurement time-point. R: right; L: left; AS: anterior scalene; LS: elevator scapulae; SCap: splenius capitis; SCM: sternocleidomastoid; UT: upper trapezius.
Pain and disability
Table II presents the pain and disability scores across sessions and Table III presents the within-group differences obtained with each variable at each measurement time. Both groups showed a significant reduction in NDI score and current VAS immediately after the first treatment session (post session 1) (all p < 0.05).
|
Table II. Pain and disability scores obtained at each measurement session (n = 14) |
||||
|
Group |
Pre |
Post session 1 |
Post month 1 |
Post month 2 |
|
NDI, mean (SD) |
||||
|
CCF |
7.71 (2.78) |
6.64 (2.61) |
7.60 (3.19) |
4.46 (2.02) |
|
Proprioception |
7.42 (2.87) |
6.21 (2.35) |
4.78 (2.60) |
4.14 (2.62) |
|
VAS maximum, median (IQR) |
||||
|
CCF |
5.90 (4.40, 7.00) |
2.75 (1.00, 4.00) |
2.25 (1.40, 3.17) |
0.20 (0.00, 1.01) |
|
Proprioception |
5.00 (3.26, 6.40) |
3.45 (2.30, 4.30) |
1.70 (0.95, 2.30) |
1.25 (0.00, 2.02) |
|
VAS minimum, median (IQR) |
||||
|
CCF |
0.22 (0.00, 0.77) |
6.10(4.43,7.00) |
4.60 (3.43, 6.35) |
2.17 (1.00, 340) |
|
Proprioception |
1.00 (0.00, 2.10) |
4.20 (3.97, 5.77) |
3.45 (1.97, 4.67) |
2.05 (0.65, 3.10) |
|
VAS rest, median (IQR) |
||||
|
CCF |
3.45 (2.95, 4.35) |
0.30 (0.00, 0.70) |
0.35 (0.00, 0.50) |
0.00 (0.00, 0.26) |
|
Proprioception |
4.00 (2.66, 4.62) |
1.10 (0.00, 2.92) |
0.55 (0.00; 0.92) |
0.00 (0.00, 0.70) |
|
IQR: interquartile range; SD: standard deviation; CCF: cranio-cervical flexion; NDI: Neck Disability Index; VAS: visual analogue scale. |
||||
|
Table III. Results of data analysis and within-group differences obtained with each variable at each measurement time |
||||||||
|
Group |
p-value |
Pre – post session 1 |
Pre – post month 1 |
Pre – post month 2 |
Post session 1-post month 1 |
Post session 1-post month 2 |
Post month 1-post month 2 |
|
|
CCFT |
||||||||
|
CCF |
0.002a |
0.986 |
0.112 |
0.002 |
> 0.999 |
0.169 |
> 0.999 |
|
|
Proprioception |
< 0.001a |
> 0.999 |
0.005 |
< 0.001 |
0.094 |
0.08 |
> 0.999 |
|
|
VAS minimum |
||||||||
|
CCF |
0.359a |
– |
– |
– |
– |
– |
– |
|
|
Proprioception |
< 0.001a |
> 0.999 |
0.746 |
< 0.05 |
0.342 |
0.016 |
> 0.999 |
|
|
VAS rest |
||||||||
|
CCF |
< 0.001a |
0.746 |
0.50 |
< 0.001 |
> 0.999 |
0.02 |
0.62 |
|
|
Proprioception |
< 0.001a |
> 0.999 |
< 0.001 |
< 0.001 |
0.41 |
< 0.001 |
> 0.999 |
|
|
VAS maximum |
||||||||
|
CCF |
< 0.001a |
> 0.999 |
> 0.999 |
< 0.001 |
> 0.999 |
< 0.001 |
0.013 |
|
|
Proprioception |
< 0.001a |
> 0.999 |
0.94 |
< 0.001 |
0.32 |
< 0.001 |
0.554 |
|
|
NDI |
||||||||
|
CCF |
0.020b |
0.006 |
0.747 |
< 0.001 |
0.418 |
0.003 |
< 0.001 |
|
|
Proprioception |
< 0.001b |
0.022 |
0.01 |
< 0.001 |
0.002 |
< 0.001 |
0.082 |
|
|
aFriedman test; banalysis of variance. –: In those measurements for which the Friedman analysis of variance (ANOVA) test showed no significant differences, tests for multiple comparisons were not performed; IQR: interquartile range; SD: standard deviation; CCF: cranio-cervical flexion; CCFT: cranio-cervical flexion test; NDI: Neck Disability Index; VAS: visual analogue scale. |
||||||||
One month after starting treatment, both groups showed a significant reduction in current VAS compared with baseline (both p < 0.001). In addition, the proprioception training group showed a significant reduction in NDI score (p < 0.01) and in maximum VAS (p < 0.05) between these time-points. When evaluating the change from post session 1 to post month 1, only the proprioception training group showed a significant change in NDI score (p < 0.05), current VAS (p < 0.001) and maximum VAS (p < 0.05).
Between post session 1 and post month 2 both groups showed a significant reduction in NDI score (both p < 0.01), current VAS (both p < 0.001) and maximum VAS (both p < 0.001). Moreover, the proprioception training group showed a significant change in minimum VAS (p < 0.05) between these time-points. Between post month 1 and post month 2, only the CCF training group showed a significant change in NDI score (p < 0.001) and in current VAS (p < 0.001). Both groups showed a significant reduction in maximum VAS score (both p < 0.001) between these time-points.
Two months after initiating the intervention, when treatment was completed, both groups showed a significant reduction in NDI score (both p < 0.001), current VAS (both p < 0.001) and maximum VAS (both p < 0.001) compared with baseline. Moreover, the proprioception training group showed a significant change in minimum VAS (p < 0.05) between these time-points.
Between-group differences
Differences between the 2 interventions at the end of treatment were studied using the Student’s t-test and Mann-Whitney U test, in addition to the effect size (Table IV). The comparison between the CCF and the proprioceptive training groups at the end of treatment (post month 2) did not show significant differences for the score on the CCFT (Fig. 2). The effect size for the CCFT was small (d = 0.05) at the end of both interventions. There was no significant difference between groups for any of the outcome measures except for the change in the minimum VAS, which was significantly different favouring the CCF training group (p < 0.05) with a moderate effect size (d = 0.44). Moderate effect sizes were observed for the right sternocleidomastoid (d = 0.37), right splenius capitis (d = 0.38) and right upper trapezius (d = 0.38) PPTs, but no between-group differences were observed.
|
Table IV. Between-group variable differences between baseline (pre) and assessment at 2 months after starting treatment. Results are expressed as mean and standard deviation (SD) for normally distributed variables and median and first and third quartiles for non-normal variables |
||||
|
Variables |
Student t-test |
Effect size Cohen’s d |
CCF training Mean (SD) |
Proprioception training Mean (SD) |
|
PPT right SCM |
0.347 |
0.37 |
–0.013 (0.161) |
0.060 (0.237) |
|
PPT right AS |
0.781 |
0.11 |
–0.033 (0.134) |
–0.016 (0.172) |
|
PPT left LE |
0.538 |
0.23 |
0.044 (0.290) |
0.140 (0.494) |
|
PPT left SC |
0.715 |
0.13 |
–0.028 (0.299) |
0.018 (0.353) |
|
PPT right SC |
0.313 |
0.38 |
–0.012 (0.239) |
–0.145 (0.420) |
|
NDI |
0.964 |
0.01 |
3.250 (2.026) |
3.285 (2.163) |
|
Mann-Whitney U test |
Grissom |
Median (IQR) |
Median (IQR) |
|
|
CCFT |
0.804 |
0.05 |
–20 (–28, –3.75) |
–21.25 (–29, –5) |
|
PPT right UT |
0.085 |
0.38 |
0.120 (–0.247, 0.312) |
0.405 (–0.015, 0.792) |
|
PPT left SCM |
0.635 |
0.10 |
0.000 (–0.155, 0.107) |
0.000 (–0.125, 0.185) |
|
PPT left AS |
0.603 |
0.12 |
–0.040 (–0.147, 0.240) |
–0.035 (–0.221, 0.007) |
|
PPT right LE |
0.701 |
0.24 |
0.130 (–0.272, 0.390) |
0.000 (–0.186, 0.257) |
|
PPT left UT |
0.306 |
0.23 |
0.100 (0.000, 0.270) |
0.015 (–0.177, 0.275) |
|
VAS minimum |
0.044 |
0.44 |
0.000 (–0.025, 0.500) |
0.550 (0.000, 1,075) |
|
VAS rest |
0.769 |
0.08 |
2.92 (2.37, 3.62) |
2.87 (1.57, 4.12) |
|
VAS maximum |
0.810 |
0.04 |
3.40 (2.22, 4.05) |
3.05 (1.35, 4.52) |
|
IQR: interquartile range; PPT: pressure pain threshold; AS: anterior scalene; LE: elevator scapulae; SC: splenius capitis; SCM: sternocleidomastoid; UT: upper trapezius; SD: standard deviation; CCF: cranio-cervical flexion; CCFT: cranio-cervical flexion test; NDI: Neck Disability Index; VAS: visual analogue scale. |
||||
DISCUSSION
This study is the first to evaluate whether proprioception training is capable of inducing improvements in neck muscle function, in the same manner that CCF exercise has demonstrated a significant benefit on impaired proprioception (7). Our results showed that cervical proprioception training not only improves patient perceived pain and disability, but also has an effect on other aspects of neuromuscular function, specifically the coordination between the deep and superficial cervical flexors measured through performance on the CCFT. Perhaps this is not surprising, considering that the proprioception exercises required fine control of neck movement. In addition, a significant improvement in neck flexor function, as measured via the CCFT, was noted with proprioception training prior to CCF training (1 month vs 2 months after starting treatment). At 2 months, when treatment was completed, the improvements in neck flexor function were comparable between groups.
Patients with neck pain can present with a myriad of sensorimotor impairments and 1 mode of exercise may not address all potential motor impairments adequately (21). Moreover, a single exercise is unlikely to affect both the functional as well as structural changes that may be present in the neck muscles in people with neck pain (1). Exercise-induced changes in motor performance are usually specific to the mode of the exercise protocol applied (21). Yet, studies investigating exercise-induced changes in motor performance show somewhat conflicting results. For instance, training of the deep neck flexors using CCF exercises has been shown to produce significant improvements in neuromuscular coordination between the deep and superficial neck flexors, but negligible effects on flexor muscle strength (16, 21) or neck flexor muscle activation during a functional upper limb activity (18). Furthermore, endurance training of the deep cervical flexors showed significant gains in endurance performance and some carryover effects in strength, but no gains in coordination performance (21). However, other studies have demonstrated a potential carryover effect of neck exercises to domains of motor function different from the specific mode of the exercise intervention (7, 14, 17, 19). In accordance, the current study demonstrates that improvements in domains of motor performance (i.e. neuromuscular coordination) other than those aligned with the primary behavioural demand of the exercise protocol (i.e. proprioception training), may be acquired.
An improvement in the activation of the deep cervical flexors, as assessed via the CCFT, was obtained with the 2 interventions applied in this study. Enhanced deep cervical flexor muscle performance with CCF exercise was expected and is in agreement with previous observations (7, 14–21). However, improvement in performance on the CCFT following proprioception training is a novel finding. The high density of muscle spindles in the deep cervical flexor muscles (12) could justify the effect of proprioception training on the activation and control of these muscles and not just the sub-occipital muscles and cervical multifidus as classically proposed (5). Improved performance on the CCFT following a period of cervical proprioception exercise may be also related to other peripheral and central mechanisms, although the mechanisms underlying the positive effect of the studied interventions on motor performance were not addressed directly in this study. Other studies have also reported positive effects on performance of the CCFT with interventions not directly addressing the activation of the deep cervical flexors, such as passive mobilizations (33, 34), although several others have shown no effect (e.g. 15, 22).
Both interventions resulted in a reduction in pain and disability, which confirms the pain-modulation properties of active neck exercises (35) and highlights the importance of exercise as a component of treatment for the management of patients with chronic neck pain. However, the change in the subjective report of pain and disability was not accompanied by a consistent objective improvement on PPTs evaluated with algometry. This observation is in line with a finding that 6 weeks of CCF training did not change pressure pain sensitivity over myofascial trigger points located in superficial cervical muscles (20). In the current study, we measured PPT not only in the upper trapezius, elevator scapulae and splenius capitis as in Lluch et al. (20), but also extended PPT measurements to include the sternocleidomastoid and anterior scalene, which are often excessively activated in people with chronic neck pain (1). However, changes in pressure pain sensitivity were not observed for these muscles. A too low training intensity and/or insufficient intervention duration may have accounted for the lack of significant changes in muscle tissue sensitivity (36). In addition, a longer follow-up period may inform whether there are eventual changes in pressure pain sensitivity.
Study limitations
Some limitations of this study should be considered. We only included people with neck pain with a NDI score less than 15/50, in order to avoid potential aggravation of neck symptoms due to exercise. Thus, generalization of the results to patients with higher levels of pain and disability is not feasible, and future studies should assess the effectiveness of the 2 protocols on individuals with varying clinical severity. Moreover, we did not include a control group that did not receive a form of specific training, thus it is difficult to appreciate the small, yet significant, reduction in pain and disability.
Unlike previous clinical trials (19, 21), patients in the CCF exercise group were not given a pressure biofeedback unit for home training. Although they practiced several repetitions of the CCF exercise before training at home, we cannot be sure that the level or movement they practiced at home was the same as under physiotherapist supervision. This fact may have influenced the results obtained with the protocol of CCF training. Similarly, pupillary glasses were only used in the clinic for cervical proprioception training. Both oculomotor control and cervical joint position sense are often altered in people with neck pain (4), although they were not formally evaluated prior to the study commencement in the way some authors have recently suggested (37).
Conclusion
Training protocols of CCF and proprioception training produced an improvement in activation and endurance of the deep cervical flexors, as assessed via the CCFT, on pain measured by triple VAS and on the level of disability evaluated with NDI, with similar results in both groups. However, pressure pain sensitivity was not affected in either group. Proprioception training may provide an additional benefit of facilitating the deep cervical flexor muscles. Care should be taken in extrapolating these results to patients with higher levels of pain and disability.
REFERENCES
