Julie Cendras1, Luc Durand2 and Olivier Dereure1*
1Department of Dermatology, University of Montpellier I, Hôpital Saint-Eloi, 2Laboratory of Pathology, University of Montpellier I, Hôpital Gui de Chauliac, FR-34000 Montpellier, France. *E-mail: o-dereure@chu-montpellier.fr
Accepted March 20, 2007.
Sir,
Idiopathic localized involutional lipoatrophy (ILIL) is a rare and nosologically imprecise condition characterized by a focal loss of subcutaneous tissue on one or several sites, occurring without any significant triggering factor or auto-immune background, and regressing spontaneously within a few months (1, 2). We report here on a new observation of ILIL that emphasizes its deceitful clinical resemblance to lupus profundus and the necessity for clinicians to be aware of this unusual differential diagnosis of better prognosis.
CASE REPORT
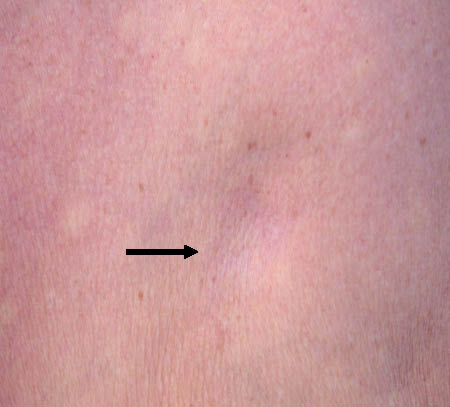
A 67-year-old woman without significant medical history was referred for evaluation of 5 similar atrophic skin lesions of 6 weeks’ duration. These elements were asymptomatic, sharply demarcated, oval-shaped and depressed areas ranging from 2 to 5 cm in diameter, located on the chest and the outer aspect of both upper limbs (Fig. 1). The patient reported that they appeared spontaneously and rapidly, without previous trauma or injection at these sites, but were preceded by a transient inflammatory phase of short duration. Standard blood tests were normal, as were pancreatic enzymes and alpha-1-antitrypsin rates; serum titres of anti-nuclear antibodies and rheumatoid factor were non-significant.
Fig. 1. Spontaneously regressive and well-defined cupule-shaped depressed area on the chest.
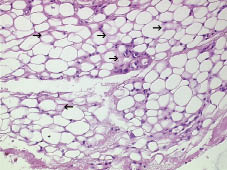
Two biopsy specimens showed similar features, with normal epidermis, dermis and skin appendages, contrasting with a sharp decrease in size of subcutaneous fat lobules, along with atrophy of adipocytes sometimes replaced by acidophilic bodies and separated by hyaline material (Fig. 2). No significant inflammatory infiltrate was present in the dermis or subcutaneous tissue, but immunostaining revealed the presence of a limited number of CD68+ histiocytes within the atrophic lobules. Direct cutaneous immunofluorescence was negative.
Fig. 2. Reduced size adipocytes with vascular dilatations and hyalin substance surrounding fat lobules (arrows): involutional pattern. (H&E ×200).
The clinical outcome was remarkable for complete spontaneous regression of the first lesions within 2 months, which, together with biological and microscopic data, led us to consider ILIL as the most suitable diagnosis, although lupus erythematous profundus had been rated the most probable hypothesis according to the initial clinical presentation. After a few weeks, 2 new and similar lesions appeared on the presternal area and a treatment with hydroxychloroquine (Plaquenil®, Sanofi-Aventis, Paris, France) was implemented in an attempt to prevent the occurrence of subsequent lesions.
DISCUSSION
ILIL was first reported in 1986 by Peters & Winkelmann (1, 2) and our observation fits perfectly the original description of this unusual entity. This condition has rarely been reported since then, but its true incidence is probably underestimated due to the lack of awareness of physicians of this condition, which can easily be mistaken for lupus profundus. It mostly affects women and is clinically characterized by the occurrence of areas of non-inflammatory focal loss of subcutaneous tissue, resulting in sharply-demarcated cupule-shaped depressions of the skin, without any significant epidermal alteration. These elements are located mainly on the breasts and proximal limbs. They appear without any triggering factor such as injection or injury at the involved sites (hence their “idiopathic” nature) and regress spontaneously after a few weeks. They are not associated with any non-cutaneous symptoms and general status remains good. Standard tests and immunological investigations are normal. Cutaneous biopsies display a unique pattern of fat involution, featuring various-sized lobules, with individual adipocytes often smaller and rounder with more prominent nuclei than normal fat cells, surrounded by a background of hyaline material. At high magnification, the lobules may contain eosinophilic bodies. No or few inflammatory cells are present, as in our patient. Capillaries are abnormally numerous and prominent. Overall, this pattern is reminiscent of foetal fat (2). The underlying muscle tissue is normal. Direct cutaneous immunofluorescence is negative.
Other, more common, conditions must be considered when evaluating localized lipoatrophy affecting one or multiples sites: intramuscular or intra-articular corticosteroids, antibiotics or insulin injections, post-injury atrophy (such as semi-circular lipoatrophy of the limbs), or late-stage inflammatory panniculitis, including Weber-Christian disease, alpha-1 anti-trypsin deficit, pancreatic panniculitis or panniculitis associated with connective tissue disorders, mainly subcutaneous lupus erythematosus (lupus profundus of Kaposi-Irgang), which is probably the closest and most deceitful differential diagnosis with a very similar clinical pattern. However, ILIL differs sharply from all these latter entities by its clinical characteristics (self-regressive lesions appearing without any triggering factor and with very limited, if any, inflammation) and by its almost unique involutional histological features. Indeed, localized lipoatrophic lesions of other origin usually display an inflammatory infiltrate predominantly involving either macrophages (post-injection and post-injury lipoatrophy) or lymphocytes (lupus panniculitis) (2–4). In other cases, especially in the late stages of the above-mentioned conditions, only lipoatrophy is present, theoretically lacking the unusual “involutional”, foetal-like features characteristic of ILIL. Gowers localized panatrophy is a rare entity with atrophic elements occurring on the trunk or limbs; its cutaneous presentation may be consistent with ILIL, but the lesions are non-regressive and extend deeper into the muscle tissues.
The pathomechanisms and nosological situation of this peculiar clinical and histological entity are still uncertain. A transient initial inflammation is likely, as illustrated by our patient who experienced a mild inflammatory phase at some sites before the occurrence of skin atrophy. This hypothesis is supported by the persistence of CD68+ inflammatory cells in some lesions, but the mechanisms underlying the self-regressive outcome and the occurrence of this unique involutional pattern are currently unknown.
No specific therapeutic strategy has been reported in literature. Our patient received hydroxychloroquine (Plaquenil®) by analogy with lupus panniculitis, essentially to prevent the occurrence of new lesions, but a minimum period of treatment is necessary to properly evaluate its results.
This rare condition should certainly be carefully identified as a separate entity by dermatologists, especially because of its striking clinical resemblance to lupus erythematosus profundus, the cutaneous and general prognosis of which is very different.
REFERENCES
1 Peters MS, Winkelmann RK. Localized lipoatrophy (atrophic connective tissue disease panniculitis). Arch Dermatol 1980; 116: 1363–1368.
2 Peters MS, Winkelmann RK. The histopathology of localized lipoatrophy. Br J Dermatol 1986; 114: 27–36.
3 Zalla MJ, Winkelmann RK, Gluck OS. Involutional lipoatrophy: macrophage-related involution of fat lobules. Dermatology 1995; 191: 149–153.
4 Dahl PR, Zalla MJ, Winkelmann RK. Localized involutional lipoatrophy: a clinicopathologic study of 16 patients. J Am Acad Dermatol 1996; 35: 523–528.