OBJECTIVE: To illustrate that a patient with distal spinal muscular atrophy can recover gait with a combination of orthoses and orthopaedic shoes.
Subject: A 28-year-old man with distal spinal muscular atrophy affecting only the distal muscles of the lower limbs. Clinical examination showed a bilateral pes cavus with a varus and a 90° equinus of the ankle joint.
METHODS: The patient was fitted with orthopaedic shoes and a patellar tendon-bearing orthosis. In order to assess the clinical effects of this fitting, a complete physical examination was performed and the patient’s temporo-spatial gait parameters were assessed quantitatively using gait analysis tools (Gaitrite®) both prior to treatment and after one month.
RESULTS: Before the fitting, the patient was not able to walk alone or to maintain an upright position and he suffered from foot pain. One month after the fitting was applied, the patient was able to walk alone and to maintain an upright position for 1 hour. His pain disappeared. Quantified study of the patient’s gait parameters shows that the temporo- spatial parameters are close to normal with fitting.
CONCLUSION: Clinical and quantitative data both confirm the subjective improvements reported by the patient.
Key words: distal spinal muscular atrophy, orthosis, orthopaedic shoes.
J Rehabil Med 2007; 39: 181–184
Correspondence address: Laurent Bensoussan, University Hospital la Timone, 264 rue Saint-Pierre, FR-13385 Marseille cedex 05, France. E-mail: laurent.bensoussan@ap-hm.fr
Submitted March 17, 2006; accepted October 18, 2006.
Introduction
Spinal muscular atrophy (SMA) covers a large, heterogeneous group of disorders characterized by the degeneration of spinal cord anterior horn cells (and possibly also of brain-stem neurones) (1–6). There are 3 principal forms of SMA and other forms exist, which are less well known, such as distal SMA. Distal SMA (7) seems to involve chromosome 12 (6, 8). Males are more often affected than females. The onset of the disease occurs before the age of 20 years. The main symptoms are a distal, symmetrical wasting and weakness of the leg muscles. Patients show entirely normal clinical sensory activity. Electromyography (EMG) and muscle biopsies have shown the occurrence of denervation despite the normal nerve conduction velocities recorded. The nerve biopsy data are normal. The evolution of the disease is very slow, but patients can show various disabilities, and the effects on upright stance and gait differ from one patient to another.
There is no aetiological treatment available for these pathologies. Symptomatic treatment is therefore usually proposed, including physical therapy, fitting orthoses, and, sometimes, surgery. The success of these therapeutic solutions has not so far been properly assessed in patients with these pathologies. Orthoses are a useful means of improving gait and posture in patients with conditions of this kind, because, unlike surgery, they are not an irreversible or invasive form of therapy. They can also be adapted in the case of evolving pathologies.
The aim of this paper was therefore to report on the rehabilitation and physical medicine outcome achieved in the case of a patient with distal SMA affecting only the lower limbs. This patient was given a limb fitting consisting of a patellar tendon-bearing orthosis and orthopaedic shoes, and the results were assessed one month later. To our knowledge, no cases of patients with distal SMA benefiting from fittings of this kind have been described so far in the literature.
Subject
The patient was a 28-year-old male Moroccan cook, who was married and had one child. The disease began at the age of 5 years, when he started to walk on tip-toe. The situation gradually worsened, becoming bilateral and leading to digitigrade standing. From the age of 16–18 years, he reported a rapid aggravation of the condition, which was responsible for a decline in his physical abilities (he could no longer practice sports). There was no history of acute anterior poliomyelitis, no parental consanguinity and there were no personal or family antecedents. The patient underwent a neurological check-up at the age of 19 years. EMG showed the presence of neurological deficits, without any sensory impairment in the lower limbs. The nerve biopsy, brain therapeutic drug monitoring, medullar magnetic resonance imaging, cardiac ultrasonography, biological assessment and ophthalmological findings were all normal. The diagnosis was distal SMA.
At the age of 21 years he was referred by the neurological ward to the physical and rehabilitation medicine ward because of gait and upright stance difficulties associated with neurological equinus feet. He also suffered from foot pain.
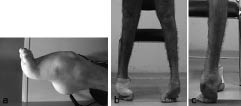
A clinical examination was performed. Concerning impairments, the clinical sensory examination were normal, there was no upper motor-neurone syndrome, the patellar reflexes were present, and the calcaneus tendon reflexes were abolished. There was a bilateral pes cavus with a varus, an irreducible extension of the talo-crural joint at 90° (9) (Fig. 1a). There was laxity of the sub-talar joint and an anterior projection of the talus. The forefeet were in adduction with an extension of the metatarso-phalangeal joints. Painful keratosis had developed at the contact points. Strength assessments performed using the Medical Research Council’s clinical method (10) showed the presence of symmetrical deficits in the tibialis anterior, scoring 0/5. Other lower limb muscles were rated 4/5 or 5/5. Concerning disabilities, he could not walk barefoot without assistance. Upright stance and gait were on the toes, with a very narrow foot contact area (Figs 1b and c). He could not maintain his balance because this supporting area was so small. There was an increase in the varus, which was not controlled. Gait was also difficult because of the painful toes. He required help with his personal care and catering tasks. The situations in which he was handicapped were all those involving walking. His quality of life would be improved if he could work again.
Fig. 1. (a) Pes cavus equinus foot. (b and c) Bilateral digitigrade standing position (b: frontal view; c: lateral view).
Rehabilitation intervention
After a multidisciplinary consultation with a surgeon and a physiatrist, 2 alternative therapeutic strategies were proposed: surgery and limb fitting. The surgery consisted of a trapezoidal tarsectomy to correct the feet deformities, but the patient decided, for personal and professional reasons, not to undergo this procedure at that time. A moulded fitting with a patellar tendon-bearing orthosis placed inside orthopaedic shoes and physical therapy were therefore applied.
The aim of the fittings was to improve balance by increasing the contact area, the supporting area and stabilizing the ankle, as well as to decrease the constraints and the pain in the toes. These fittings are always made in the presence of a team consisting of an orthotist, a pedorthist and a physiatrist: defining the fitting specifications is an interdisciplinary job. The follow-up is also interdisciplinary. The therapeutic objectives and details of the orthopaedic shoes (11) were specified as regards the upper, the plantar orthosis, the external soles, the first contact point and the fastener. The therapeutic objectives and details of the patellar tendon-bearing orthosis (12) were specified as regards the tip, the stiffness and the number of valves.
The orthotist then made a mould of the patient’s foot and leg. From the mould, he prepared a plaster copy of the patient’s limb, which was then corrected. When preparing the fitting, the orthotist and the physiatrist work together to make any changes required to improve the functional results. Once the orthotist had prepared the orthosis, the pedorthist prepared a mould of the foot wearing the orthosis and made another plaster copy of the foot. The first shoe was a transparent plastic one. The physiatrist, the orthotist and the pedorthist attended the fitting session, looking in particular for conflict zones. After the corrections made by the pedorthist, the final shoe was made and delivered to the patient. One month later, the efficacy of the fitting and the patient’s tolerance were assessed.
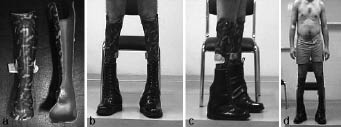
The orthosis was made of polypropylene (Fig. 2) and fitted with 2 valves: an anterior shell bearing on the patellar tendon and a posterior shell with a counter bearing placed in the popliteal fossa. The shells were fitted to the equinus. They stabilized the ankle by controlling the varus. The pressure thus applied to the patellar tendon reduced the constraints exerted on the toes. Each orthosis weighed 350 g. The orthopaedic shoes (Fig. 2) and the plantar orthosis were fitted to the patellar tendon-bearing orthosis. The orthopaedic shoes therefore included the patellar tendon-bearing orthosis and the plantar orthosis. They had wide soles, giving a large base support area. The plantar orthosis compensated for the equinus and enabled the patient to make contact, not only with the toes, but also with the forefoot and heel. The foam rubber components absorbed the loads. The weight of each shoe, including the plantar orthosis, was 1500 g. The total weight of the fitting was 3700 g. The patient’s balance was improved by the plantar orthosis supporting the heel, the wide soles of the orthopaedic shoes, and the patellar tendon-bearing orthosis stabilizing the ankle.
Fig. 2. Ankle and foot orthosis. (a) Frontal view of the two shells. (b, c and d) Patient with the fitting: orthopaedic shoes and tendon-bearing orthosis, in the upright position.
Methods of assessment
Clinical examinations were carried out before and after the fitting procedure to determine whether the therapeutic objectives had been achieved and to assess the efficacy of the treatment and the patient’s tolerance. A qualitative gait assessment was carried out with a digital video camera.
The quantitative gait assessment was performed with the Gaitrite® system (Cir Systems, Inc., Pennsylvania, USA) (13), an electronic walkway connected to a computer. The Gaitrite® electronic walkway contains many sensors on a 427-cm long, 61-cm wide active area. Acquisition frequency is 32.2–38.4 Hz. The spatial parameters recorded are the step length and width. The temporal parameters recorded are the velocity, cadence, and the stance and swing phases percentage of the total gait cycle. The patient was asked to walk on the walkway at his own speed.
Results
The main clinical changes induced by the fitting are summarized in Table I. Due to these improvements, the patient was able to return to his work as a cook. The main quantified parameters of the patient’s gait with the fitting are summarized in Table II. These parameters had become quite normal (14).
| Table I. Abilities with and without bracing |
| | Barefoot, without assistance | With bracing |
| Gait | Impossible | Possible |
| Upright position | Impossible | Possible |
| Walking perimeter on flat ground | 0 meter | >500 metres |
| Up and down stairs | Impossible | Possible with banister |
| Pain | Pain under the feet | No pain |
| FAC | 2 | 6 |
| Motor FIM | 3 | 12 |
| FAC: Functional Ambulation Categories; FIM: Functional Independence Measure. |
| Table II. Temporo-spatial parameters of gait recorded with the Gaitrite® system. Results with fitting |
| Parameters | Values Mean (SD), range | Normal values (means) * |
| Speed (m/sec) | 1.04 | 0.8–1 |
| Cadence (steps/min) | 94.6 | 75 |
| Right step length (cm) | 70.3 (2.1), 68–74.2 | 75 |
| Left step length (cm) | 62.8 (4.4), 57–68.7 | 75 |
| Right step width (cm) | 16.5 (1.6), 14.1–18.8 | 10–12 |
| Left step width (cm) | 16.4 (1.5), 14.6–17,8 | 10–12 |
| Right swing phase (%) | 40.2 (2.6), 38.0–43.1 | 40 |
| Left swing phase (%) | 38.4 (0.8), 37.7–39.5 | 40 |
| Right stance phase (%) | 59.8 (2.6), 56.9–62 | 60 |
| Left stance phase (%) | 61.6 (0.8), 60.5–62.3 | 60 |
| SD: standard deviation. *According to Delarque & Pellas (14). |
Discussion
Our aim was to initiate more systematic methods of describing and assessing the therapeutic solutions used on patients with SMA. This is the first paper describing a fitting of this kind applied to a patient with SMA. All previous papers (2–7) on this pathology have given clinical and genetic data without addressing the therapeutic issues.
In our patient presenting with deformations of both feet and suffering from pain and from the resulting functional disability, the first solution envisaged was surgery of the resection/arthrodesis type in order to give the patient plantar support and to counterbalance the pathological impediments to walking and maintaining an upright stance. However, in the setting of neurological pathologies, one has to be careful because these disabilities are liable to evolve with a risk of recurrence of the disease (15). Applying a suitable fitting is the alternative therapeutic strategy. This solution is not invasive and does not require a long period of immobilization. The aim of this fitting was to help the patient to recover gait while improving his balance and decreasing the loads applied at the pressure points. A patellar tendon-bearing orthosis and orthopaedic shoes were used here because it is difficult to decrease the pressure points on the foot and to stabilize the subtalar joint using orthopaedic shoes alone. The use of an orthosis makes it possible to transfer pressure points to the knee, gives a better distribution of the constraints over the leg and stabilizes the ankle, as well as reducing the pressure under the feet. Shoes equipped with an orthosis also absorb the loads due to the foam rubber components, and induce a normal pattern of foot movement during the stance phase: the first contact is made with the heel, followed by plantar and then toe contact. The main disadvantage is the patient’s dependence on the shoes and orthosis, and walking barefoot is therefore impossible. In addition, the volume and weight of these fittings might bother some patients, although orthotists are now attempting to use lighter materials. The aesthetic aspects of these fittings should be taken into account. This fitting needs to be checked frequently as the pathology evolves, and the possibility of foot surgery as a means of ensuring long-term benefits should be mentioned regularly to the patient.
Patients always make their own decision after being fully informed about the advantages and disadvantages of the 2 solutions available. In the present case, the patient systematically refused the surgical solution for several reasons: for personal and professional reasons, and because he was told that wearing orthopaedic shoes and a patellar tendon-bearing orthosis would alleviate the pain and give him greater freedom of movement. Suitably wide-legged trousers can easily be worn to hide the fitting.
The clinical improvement in the patient’s gait was confirmed by the Gaitrite® system records. The use of a walkway makes it possible to asses the patient’s gait quantitatively and shows up any subnormal gait parameters, such as speed, the distribution of the different phases in a cycle and that of the pressure points on the ground. The values recorded with our tall subject were compared with those obtained in a typical population of normal subjects of normal height. One must bear in mind that in our case we have quite normal value in a tall man that he has greater step length than a subject of normal body height. Another comment needs to be made about the asymmetry of the step length. This asymmetry may have been due to the fitting, but it was not possible to determine whether this was the case: we could not assess the patient barefoot with the Gaitrite® system prior to the fitting because he was unable to walk without assistance at that stage. The Functional Ambulation Categories (FAC) and FIM™ locomotion (walking/wheelchair and stairs) assessments showed the occurrence of a distinct quantitative improvement.
The main reason why no similar cases treated with fittings have been reported in the literature is that SMA is such a rare and variable disease. In the case of this patient, although the deficits were restricted to the distal muscles of the lower limbs, the extent of the lesions was spectacular and it is possible that these disorders might have been amenable to treatment at an earlier stage. Apart from the patient’s difficulty in maintaining an upright stance and walking, he had no symptoms that were detrimental to his vital prognosis. His main request was therefore simply to have these disorders corrected. The walking analysis performed with Gaitrite® show that fitting the patient with orthopaedic shoes and a patellar tendon-bearing orthosis was a highly effective therapeutic strategy. This therapy has made gait possible (on flat ground and on stairs) for a patient who was previously unable to stand upright without assistance. This treatment can therefore be used to replace surgery for a long period, depending on the patient’s wishes. However, as this is the only case of this kind to have been reported so far, this therapeutic approach cannot yet be generalized, and it would be interesting to know what other modes of treatment have been used and what results have been obtained in different patients suffering from similar disorders.
AcknowledgEmentS
We thank Mr François Maioli, Certified Pedorthist, and Mr Bertrand Tourret-Couderc, Certified Prothetist Orthotist.
References
1. Dubowitz V. Chaos in the classification of SMA: a possible resolution. Neuromuscul Disord 1995; 5: 3–5.
2. Adams C, Suchowersky O, Lowry RB. Congenital autosomal dominant distal spinal muscular atrophy. Neuromuscul Disord 1998; 8: 405–408.
3. Harding AE, Thomas PK. Hereditary distal spinal muscular atrophy. A report on 34 cases and a review of the literature. J Neurol Sci 1980; 45: 337–348.
4. Boylan KB, Cornblath DR, Glass JD, Alderson K, Kuncl RW, Kleyn PW, et al. Autosomal dominant distal spinal muscular atrophy in four generations. Neurology 1995; 45: 699–704.
5. Groen RJ, Sie OG, van Weerden TW. Dominant inherited distal spinal muscular atrophy with atrophic and hypertrophic calves. J Neurol Sci 1993; 114: 81–84.
6. Mercuri E, Messina S, Kinali M, Cini C, Longman C, Battini R, et al. Congenital form of spinal muscular atrophy predominantly affecting the lower limbs: a clinical and muscle MRI study. Neuromuscul Disord 2004; 14: 125–129.
7. Serratrice G, Pellissier JF, Pouget J. Amyotrophies spinale progressives. In: Serratrice G, Pellissier JF, Pouget J, eds. Les maladies neuro-musculaires. Paris: Masson; 1997, pp. 211–216.
8. De Angelis MV, Gatta V, Stuppia L, Passamonti L, Gambi D, Uncini A. Autosomal dominant distal spinal muscular atrophy: an Italian family not linked to 12q24 and 7p14. Neuromuscul Disord 2002; 12: 26–30.
9. Cave EF, Roberts SM. A method of measuring and recording joint function. J Bone Joint Surg 1936; 18: 455–466.
10. Medical research council. Aids to the examination of the peripheral nervous system. Memorandum no. 45. London: HMSO; 1976.
11. Delarque A, Biausser JP, Courtade D, Heurley G. Chaussures orthopédiques. Encyclopédie Médico-chirurgicale 1995; 26-161-A-50.
12. Lehmann JF, Warren CG, Pemberton DR, Simons BC, DeLateur BJ. Load-bearing function of patellar tendon bearing fittings of various designs. Arch Phys Med Rehabil 1971; 52: 366–370.
13. Bilney B, Morris M, Webster K. Concurrent related validity of the GaitRite walkway system for quantification of the spatial and temporal parameters of gait. Gait Posture. 2003; 17: 68–74.
14. Delarque A, Pellas F. Bilan fonctionnel des membres inférieurs. In: Held JP, Dizien O, eds. Traité de Médecine Physique et de Réadaptation. Paris: Flammarion Médecine-Sciences; 1998, pp. 119–131.
15. Wetmore RS, Drennan JC. Long-term results of triple arthrodesis in Charcot-Marie-Tooth disease. J Bone Joint Surg Am 1989; 71: 417–422.