Patients after stroke conventionally receive much of their rehabilitation in hospital. Services have been developed that offer patients an early discharge from hospital with more rehabilitation at home (early supported discharge). This paper sets out a systematic review of all randomized trials of early supported discharge services that included 12 trials (1659 patients). There was a reduced odds of death or dependency equivalent to 5 fewer adverse outcomes (95% confidence interval 1–10) for every 100 patients receiving an early supported discharge service (p = 0.04). Patients receiving early supported discharge services showed an 8 day reduction (p < 0.0001) in the length of hospital stay. The greatest benefits were seen in the trials evaluating a co-ordinated multidisciplinary early supported discharge team and with patients with mild-moderate disability. The experience of a trial from Stockholm is described in order to explore the potential mechanism of action of early supported discharge services. In conclusion, an illustrative case report is set out, indicating a typical patient pathway in an early supported discharge service.
J Rehabil Med 2007; 39: 103–108
Correspondence address: Peter Langhorne, Academic Section of Geriatric Medicine, Level 3, Centre Block, Royal Infirmary, Glasgow G4 0SF, UK. E-mail: P.Langhorne@clinmed.gla.ac.uk
Submitted November 30, 2006; accepted January 12, 2007
*This paper is based partly on a lecture given at the international
symposium ”Evidence for stroke rehabilitation – bridging into the future”, in Göteborg, Sweden, 26–28 April, 2006.
BACKGROUND
Stroke services in developed countries are usually focused around a period of care in hospital, and patients can expect to be admitted to hospital for acute care and some rehabilitation (1). In recent years, services have been developed that challenge this emphasis on rehabilitation in hospital. These can be considered as having 2 approaches:
• Admission avoidance – services which attempt to prevent hospital admission and provide rehabilitation at home. This has been the focus of only a limited amount of research work, but the available results are not promising (2, 3).
• Early supported discharge (ESD) – these services aim to accelerate the patient's discharge home and provide an equivalent level of rehabilitation input in the patient's own home in comparison with conventional hospital care and discharge arrangements (4, 5). A number of randomized trials of ESD services have been carried out around the world, but the effectiveness of such an approach has remained uncertain. For this reason a group of trialists (the ESD trialists) carried out a collaborative systematic review of all the available clinical trials of ESD services (4, 5). The objective was to establish whether ESD services, in comparison with conventional hospital care and discharge arrangements, could improve patient outcomes and reduce the length of hospital stay. In this article we describe the ESD review and provide some examples of practical aspects of running an ESD service.
REVIEW OF EARLY SUPPORTED DISCHARGE TRIALS
The original ESD review (4, 5) aimed to establish if, compared with conventional care, ESD services could:
• accelerate the return home of patients after stroke who are admitted to hospital;
• produce equivalent or better patient and carer outcomes; and
• provide a cost-effective alternative to conventional services.
This analysis was done using Cochrane Review methodology (6) and appears in an expanded version in the Cochrane Library. The Cochrane Stroke Group search strategy (7) was used, supplemented by discussions with trialists. In order to avoid publication bias, comprehensive searching and inclusion of published and unpublished data was carried out.
The analysis included randomized trials that recruited patients in hospital with a clinical diagnosis of stroke to receive either conventional care or an ESD intervention. An ESD intervention was defined as one that aims to accelerate discharge from hospital with the provision of rehabilitation and support in a community setting. Trials recruiting a mixed patient group were excluded. The specific type of intervention was recorded but not used as an exclusion criterion.
The identified trialists were asked to provide a description of their intervention and control services and provide basic individual patient data. Where this was not available (2 trials) standardized tabular outcome data was sought. Descriptive information about service characteristics was collected using a standard questionnaire prior to the identification and analysis of outcome data.
The primary patient outcome was death or dependency (defined as a Barthel Index of < 19/20 or a Rankin score of > 2) recorded at the end of scheduled follow-up. The secondary outcomes were death, place of residence, activities of daily living (ADL) score, extended ADL score, subjective health status, mood or depression score, carer outcomes (mood and subjective health), plus patient and carer satisfaction. The primary resource outcome was the length of the index hospital admission. Other resource outcomes included the number of re-admissions and total cost of service interventions reported in the original trials. Pre-specified subgroup analyses were planned based on patient age, sex, the presence of a carer and the initial stroke severity. Pre-specified service comparisons included whether care was planned and provided by a specialist multidisciplinary team whose work was co-ordinated through regular meetings.
Clinical outcomes in the ESD review
Our original review identified 11 trials that met our selection criteria. However, a recent update found one new small trial (8), giving a total of 12 randomized clinical trials (n = 1659 participants). The median follow-up was 6 months (range 3–12 months). In 7 trials a single multidisciplinary ESD team co-ordinated hospital discharge and provided rehabilitation at home (4, 5). In 3 trials the ESD team co-ordinated discharge and provided immediate post-discharge care, but not ongoing rehabilitation (4, 5, 8). The remaining 2 trials evaluated un-coordinated community services or input from healthcare volunteers (4, 5).
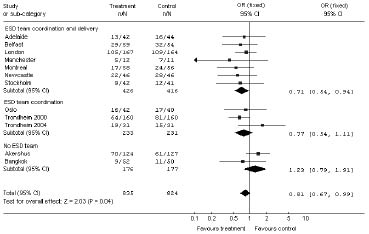
Patients who received ESD services were significantly less likely (p = 0.04) to be dead or dependent at the end of scheduled follow-up than those who received conventional care (Fig. 1). Thus they had a greater chance of being alive and independent at follow-up (Table I). A similar pattern was seen (Table I) for the number of patients who were alive and living at home at the end of follow-up (p = 0.02). No significant differences in outcome were seen for death, ADL score, subjective health status, or mood scores. Patients who received ESD services were more likely to report satisfaction with outpatient services (p = 0.02). Carer outcomes (including subjective health status, mood, satisfaction) did not differ significantly between the 2 groups.
Fig. 1. Early supported discharge (ESD) services vs conventional care: death or dependency at the end of follow-up. The figure shows the odds ratio (OR) (95% confidence interval (CI)) for the combined outcome of death or dependency at the end of scheduled follow-up (median 6 months) together with the number (n) of patients who had outcome events of all those randomized (N) to ESD or conventional services. Results are presented for individual trials, groups of trials stratified by ESD team characteristics, and for all trials together. Adapted from (4).
| Table I. Summary of main outcomes in the early supported discharge (ESD) trials. Results are presented as the proportion with an outcome at the end of scheduled follow-up plus the risk difference (absolute difference expressed as numbers per 100 treated) between ESD and control groups |
| Outcome at end of scheduled follow-up | ESD service (%) | Conventional care (%) | Risk difference (95% CI) | p |
| Alive | 91 | 90 | 0 (–3, 2) | 0.76 |
| Living at home | 82 | 77 | 5 (1, 9) | 0.02 |
| Independent in daily activities | 55 | 50 | 5 (0, 9) | 0.04 |
| Patients reporting satisfaction with outpatient care | 69 | 61 | 9 (2, 17) | 0.02 |
| Carers reporting satisfaction with outpatient care | 82 | 74 | 7 (–2, 17) | 0.14 |
| CI: confidence interval. |
Subgroup analysis indicated no alteration of the effect of ESD services with the patient age, sex, or whether they lived with a carer (4, 5). However, ESD services appeared to be more effective in patients with moderately severe stroke (baseline Barthel index of > 45/100). In addition, ESD services were more likely to be effective when provided by a specialist multidisciplinary ESD team (comprising physiotherapy, occupational therapy, and speech and language therapy staff with medical, nursing, and social work support) whose work is co-ordinated through regular (weekly) meetings. ESD services appeared to be effective even when compared with high-quality standard care based in a stroke unit (4, 5).
It is important to remember that the original question of this review was whether a policy of early hospital discharge with support at home could be as effective and efficient as conventional hospital care (including pre-discharge care, discharge planning, and post-discharge care). Therefore the inclusion criteria were kept broad and focused on trials that compared 2 policies of care for patients after stroke in hospital. Although the ESD trialists anticipated that a “core” group of trials would have explored the impact of a specialist multidisciplinary ESD team established specifically for this role, other trials were included that incorporated the testing of a policy of early discharge with support. This broad approach allowed the examination of both the effectiveness of a specific co-ordinated ESD team care and the service factors that might influence patient outcomes.
The length of hospital stay for those receiving ESD services was, on average, reduced by 8 days (95% confidence interval (CI) 5–11; p < 0.001) while hospital readmission rates during follow-up were similar between the 2 groups (27% vs 25%).
Economic analyses have been reported for several trials of ESD services (9–13). Although the underlying assumptions and costs were generally different for each analysis, all concluded that the potential savings (from hospital bed days released) was greater than the cost of the community components of the ESD service. In practice, realizing such cost savings may be difficult, but ESD services do appear to offer one way to manage the rising demand for a finite number of hospital beds.
A number of uncertainties remain. Firstly, do more severely disabled patients after stroke (those with a baseline Barthel < 50/100) truly not benefit from ESD services. Secondly, can ESD services be effectively implemented in more dispersed rural populations; most trials took place in an urban setting. Finally, there is little information about how best to implement ESD services.
One obvious question arising from this review is how could ESD services improve patient outcomes? Unfortunately the different components of ESD services cannot be adequately separated within these trials. However, potential reasons for better results with ESD services include (Table II); avoiding some of the complications of hospital admission, improving discharge planning, improving patient and carer morale, allowing a focus on more realistic rehabilitation goals, providing rehabilitation in a more relevant environment, or simply because ESD services could provide higher levels of support and therapy after discharge. The next section illustrates some of these issues.
| Table II. Potential advantages of early supported discharge (ESD) services |
| Stage in pathway | Potential benefit of ESD |
| In hospital | Avoiding some complications of hospital admission |
| Discharge planning | Improving patient and carer morale |
| | Focusing on more realistic rehabilitation goals |
| Home rehabilitation | Providing rehabilitation in a more relevant environment |
| | Encouraging more focus on self-directed recovery |
| | ESD services able to provide higher levels of therapy input over the whole patient journey |
| Discharge from ESD service | More realistic understanding of future recovery |
ILLUSTRATIVE EXAMPLE OF AN ESD SERVICE
One of the best-described trials in the review was the ESD service in Southwest Stockholm. It consisted of an outreach multi-disciplinary team associated with a stroke unit, which co-ordinated the discharge of the patients and provided continued rehabilitation at home (14). The following details provide an example of the workings of this service and how it may have influenced recovery.
In-hospital and discharge planning
This requires special planning, since discharge from the hospital is considered to be one of the major crisis points in the course of patients’ recovery after stroke. The appointment of a case manager or “key worker” (a member of the multidisciplinary team) based in the stroke unit offers several advantages. The case manager constituted the link between the stroke unit and the out-patient care, guaranteeing continuity in both time and personnel, and enabling the smooth transition from the protected hospital environment to the home. In practice, the case manager conducted the first assessment and initial treatment, and the first home visit while the patient after stroke was still at the stroke unit. Despite the early discharge procedure there was no indication that that patients experienced less involvement in discharge planning than those receiving routine rehabilitation (15).
The physiotherapist, occupational therapist or speech and language therapist from the multidisciplinary team involved with any given patient could become the team leader for that patient. This case manager focused on wider domains of functioning of the patient than was usual in routine stroke rehabilitation and used the other therapists on a consultant basis. Management protocols and meetings ensured that the activities were inter-disciplinary and the training focused on speech and communication, ADL and ambulation (16). The case manager also ensured that the service was audited by active follow-up of patients. They also co-ordinated the service through liaison with primary care, local municipalities and private therapists.
Patient motivation and focusing on more realistic rehabilitation goals
There is a consensus among professionals in stroke rehabilitation that the patients’ degree of motivation will influence the outcome of an intervention (17). Patient involvement in activities and goals in the rehabilitation process appeared to have a positive impact on patients’ motivation. Although stroke units meet important medical needs during the early crisis of stroke, the hospital environment does not always promote active involvement of the patient. In addition, restriction in participation in life situations after stroke is hard to fully recognize in the hospital environment.
The influence of the environment on behaviour was observed in both the patients after stroke and therapists (18). Patients undergoing rehabilitation at home more frequently took the initiative and expressed their goals more often than those patients undergoing hospital rehabilitation. Also the patient was observed to have a wider variety of roles while in his own home environment. Consequently, identification of problem areas became more readily apparent to the therapist, as well as more relevant to the patient.
Partnership between patient and therapist
The level of patient involvement in the rehabilitation process may have been due to partnership between the therapist and the patient after stroke (18). In the hospital setting the observed behaviour was that the therapist gave the patients instructions about what to do. Neither the therapists nor the patients were discussing or referring to any activity goals. However, at home the most apparent behaviour was a dialogue and a partnership between the patient and the therapist. Giving the patient some control over practise conditions may have encouraged their problem-solving abilities, by empowering them to view the therapist as resource.
In addition, significantly more patients receiving the ESD service in Southwest Stockholm reported that they were actively involved in planning their rehabilitation (15). Hence, rehabilitation at home has the potential of supplying a more advantageous context than the hospital environment when the aim is to make patients after stroke participate actively in the rehabilitation process and to become more autonomous in their training.
Providing rehabilitation in a more relevant context
The ESD service in Southwest Stockholm emphasized a task and context specific approach. The training sessions at home consisted of different task-specific activities, based on the patients’ personal interests. The home environment rendered it possible to set functional, achievable and measurable goals, which were of primary concern to the patient (16).
Falling and fear of falling were important issues that needed to be dealt with by the ESD service team, and there was no indication that the early discharge procedure lead to an increase in falls (15). A key aspect in providing rehabilitation in the home environment involved home adaptation and technical aids that led patients more frequently to have supporting handles installed in the home (15).
Encouraging more focus on self-directed activities
One important implicit message to patients and spouses during the home rehabilitation sessions was that post-stroke recovery was possible after discharge from hospital care and that the home environment offered ample opportunities for practice. The ESD service in Southwest Stockholm encouraged a focus on self-directed activities and a considerable amount of the training at home was left to patient self-directed activities, on average 1.5 hours per day (18). By comparison, patients in hospital after stroke appear to spend a high proportion of their time inactive and often only 1% of their time exercising on their own (19).
More realistic understanding of future recovery
The active involvement of patients in planning and carrying out training may also be important aspects for preventing patients and carers from gaining the impression that post-stroke rehabilitation is a passive process that automatically leads to recovery. The ESD service in Southwest Stockholm entailed an individualized rehabilitation program based on patient’s need (16), which varied in duration (4–29 weeks), content and frequency of home visits (3–31). The interval between the home visits increased gradually until the final discharge from the home rehabilitation programme. The case manager ensured that discharge from therapy was a gradual process and not a sudden event. When active therapy stopped, patients could be visited informally or contacted by telephone for a period of time. Important functions of the case manager were to ensure, as far as possible, that the patients were re-integrated into their previous social roles and leisure activities, and to be alert for mood disorders.
An interesting observation in the trial of the ESD service in Southwest Stockholm (seen at 5 years follow-up after stroke) was an increased independence in extended ADL, frequency of household activities (20) and a favourable outcome as regards resource use (21). This may be partially attributable to the higher degree of patients’ involvement in the rehabilitation process. The intervention may have given the stroke patients the tools to solve problems on their own, and to be less therapist-dependent. It appears that the intervention started a process that continues after the end of the home rehabilitation program.
ILLUSTRATIVE CASE REPORT
Although the trials and systematic review provide evidence of the effectiveness of ESD services, there are substantial challenges in interpreting and implementing the results of such complex interventions. Therefore, a “typical” ESD service (4, 5) and patient pathway (Fig. 2) is described below in the form of an illustrative case report.
A 72-year-old woman with a history of hypertension and cigarette smoking was admitted to hospital after developing a left hemiparesis. The clinical diagnosis was of a right lacunar stroke and the computed tomography scan confirmed a right internal capsule infarct. She was admitted to the stroke unit but was not eligible for thrombolysis because of uncertainties about the time of symptom onset. Therefore, she was commenced on aspirin and began a program of rehabilitation. By the third day of hospital admission she was able to stand with assistance but could not move from bed to chair independently. She remained under the care of the multidisciplinary rehabilitation team who set goals for the following week of independent transfers into and out of a chair and on and off a toilet. The ESD team were notified of her admission and visited her the following day (Fig. 2).
| Hospital admission | |
| | Identify ESD team key worker Key worker contact with patient/carer Home assessment Plan discharge home Agree rehabilitation goals |
| Discharge home | |
| | Agree/develop rehabilitation goals Implement rehabilitation plan Access relevant services Multidisciplinary team review of progress Negotiate withdrawal of ESD service Late review of needs/problems |
| Discharge from ESD team | |
| Fig. 2. Pathway of care with early supported discharge (ESD) service. |
An ESD team member attended the stroke unit multidisciplinary meeting and introduced herself to the patient. They discussed a program of treatment beginning with an assessment of home circumstances prior to discharge home. The following day the team member (an occupational therapist) visited the patient’s and her husband’s home. Several potential barriers to discharge home were identified, including steep stairs and an upstairs toilet. Discharge home was arranged the following day (8 days after admission) at which point the patient could transfer safely with supervision. The ESD team agreed with the patient a number of goals to be achieved over the next 6 weeks, including independent walking in the house and on the stairs (with the aid of a stair rail). The patient also wished to return to attending her local church and bowling club.
Over the next 6 weeks the members of the ESD team visited initially 4 days/week but reduced this to 1 day/week as the individual goals were achieved. At 2 months post-stroke the patient was independently mobile indoors and outdoors and had attended church and a bowling club function in the company of her husband. A review of her rehabilitation needs was planned for 2 months later to ensure that she had maintained her level of recovery.
CONCLUSION
For stroke patients in hospital, input from an ESD service (that provides early assessment in hospital, co-ordinated discharge home, and post-discharge support) can accelerate their discharge home and increase their chance of being independent in the longer term. The best results are likely to be seen with well-resourced and co-ordinated ESD teams and with patients with less severe stroke symptoms. Uncertainties remain about the essential characteristics of an effective ESD service, whether they can be effective in more dispersed rural communities, and the balance of cost and benefit in different patient groups.
ACKNOWLEDGEMENTS
This article is based on a collaborative systematic review carried out by the Early Supported Discharge trialists (Peter Langhorne, Gillian Taylor, Gordon Murray, Torunn Askim, Martin Dennis, Craig Anderson, Erik Bautz-Holter, Paola Dey, Bent Indredavik, Nancy Mayo, Michael Power, Helen Rodgers, Ole Morten Ronning, Anthony Rudd, Nijasri Suwanwela, Lotta Widen-Holmqvist and Charles Wolfe). We are grateful to the Cochrane Stroke Group for invaluable editorial advice and assistance with trial searching. Updated versions of this review will appear in the Cochrane Library. The original project was supported by the Stroke Association and Chest Heart and Stroke Scotland. The funders had no role in the conduct of the review.
Conflict of interest
The authors have no relevant financial interests to disclose.
REFERENCES
1. Warlow CP, Dennis MS, van Gijn J, Hankey GJ, Sandercock PAG, Bamford JM, et al, editors. Stroke: a practical guide to management. Edinburgh: Blackwell Science; 2001.
2. Kalra L, Evans E, Perez I, Knapp M, Donaldson N, Swift C. Alternative strategies for stroke care: a prospective randomised controlled trial. Lancet 2000; 356: 894–899.
3. Langhorne P, Dennis M, Kalra L, Shepperd S, Wade D, Wolfe C. Services for helping acute stroke patients avoid hospital admission. In: The Cochrane library, issue 3. Oxford: Update Software; 2001.
4. Early Supported Discharge trialists. Services for reducing the duration of hospital care in stroke patients (Cochrane review). In: The Cochrane library, issue 2. Chichester, UK: John Wiley & Sons Ltd; 2005.
5. Langhorne P, Taylor G, Murray G, Dennis M, Anderson C, Bautz-Holter E, et al. Early supported discharge services for stroke patients: an individual patient data meta-analysis. Lancet 2005; 365: 501–506.
6. Clarke M, Oxman A (eds). Cochrane reviewers' handbook. Version 4.2.0 (updated March 2003). In: The Cochrane library, issue 4. Chichester, UK: John Wiley & Sons Ltd; 2003.
7. Sandercock P (ed.). The Cochrane library, issue 4. Chichester, UK: John Wiley & Sons Ltd; 2003.
8. Askim T, Rohweder G, Lydersen S, Indredavik B. Evaluation of an extended stroke unit service with early supported discharge for patients living in a rural community. A randomised controlled trial. Clin Rehabil 2004; 18: 238–248.
9. Teng J, Mayo NE, Latimer E, Hanley J, Wood-Dauphinee S, Cote R, et al. Costs and caregiver consequences of early supported discharge for stroke patients. Stroke 2003; 34: 528–536.
10. McNamee P, Christensen J, Soutter J, et al. Cost analysis of early supported hospital discharge for stroke. Age Ageing 1998; 27: 345–351.
11. Anderson C, Mhurchu CN, Rubenach S, Clark M, Spencer C, Winsor A. Hospital or home for stroke rehabilitation? Results of a randomised controlled trial. II: cost minimization analysis at 6 months. Stroke 2000; 31: 1032–1037.
12. Beech R, Rudd AG, Tilling K, et al. Economic consequences of early supported discharge to community-based rehabilitation for stroke in an inner-London teaching hospital. Stroke 1999; 30: 729–375.
13. von Koch L, de Pedro-Cuesta J, Kostulas V, Almazan J, Widen Holmqvist L, et al. Randomized controlled trial of rehabilitation at home after stroke: one-year follow-up of patient outcome, resource use and cost. Cerebrovasc Dis 2001; 12: 131–138.
14. Widén Holmqvist L, von Koch L, Kostulas V, Holm M, Widsell G, Tegler H, et al. A randomized controlled trial of rehabilitation at home after stroke in southwest Stockholm. Stroke 1998; 29: 591–597.
15. Widén Holmqvist L, von Koch L, de Pedro-Cuesta J. Use of health care, impact on family caregivers and patient satisfaction of rehabilitation at home after stroke. Scand J Rehabil Med 2000; 32: 164–170.
16. von Koch L, Widén Holmqvist L, Wohlin Wottrich A, Tham K, de Pedro Cuesta J. Rehabilitation at home after stroke: a descriptive study of an individualized intervention. Clin Rehabil 2000; 14: 574–583.
17. Widén Holmqvist L, von Koch L. Environmental factors in stroke rehabilitation. BMJ 2001; 322: 1501–1502.
18. von Koch L, Wohlin Wottrich A, Widén Holmqvist L. Rehabilitation in the home versus the hospital: the importance of context. Disabil Rehabil 1998; 20: 367–368.
19. Newell JT, Wood VA, Langton Hewer R, Tinson DJ. Development of a neurological rehabilitation environment: an observational study. Clin Rehabil 1997; 11: 146–155.
20. Thorsén A, Widén Holmqvist L, de Pedro Cuesta J, von Koch L. A randomized controlled trial of early supported discharge and continued rehabilitation at home after stroke. Five-year follow-up of patient outcome. Stroke 2005; 36: 297–302.
21. Thorsén AM, Widén Holmqvist L, von Koch L. Early supported discharge and continued rehabilitation at home after stroke: 5-year follow-up of resource use. J Stroke Cerebrovasc Dis 2006; 15: 139–143.