OBJECTIVE: To compare the effect of Scientific Exercises Approach to Scoliosis (SEAS) exercises with “usual care” rehabilitation programmes in terms of the avoidance of brace prescription and prevention of curve progression in adolescent idiopathic scoliosis.
DESIGN: Prospective controlled cohort observational study.
Patients: Seventy-four consecutive outpatients with adolescent idiopathic scoliosis, mean 15° (standard deviation 6) Cobb angle, 12.4 (standard deviation 2.2) years old, at risk of bracing who had not been treated previously.
METHODS: Thirty-five patients were included in the SEAS exercises group and 39 in the usual physiotherapy group. The primary outcome included the number of braced patients, Cobb angle and the angle of trunk rotation.
RESULTS: There were 6.1% braced patients in the SEAS exercises group vs 25.0% in the usual physiotherapy group. Failures of treatment in the worst-case analysis were 11.5% and 30.8%, respectively. In both cases the differences were statistically significant. Cobb angle improved in the SEAS exercises group, but worsened in the usual physiotherapy group. In the SEAS exercises group, 23.5% of patients improved and 11.8% worsened, while in the usual physiotherapy group 11.1% improved and 13.9% worsened.
CONCLUSION: These data confirm the effectiveness of exercises in patients with scoliosis who are at high risk of progression. Compared with non-adapted exercises, a specific and personalized treatment (SEAS) appears to be more effective.
Key words: idiopathic scoliosis, physical exercise, physical therapy, brace.
J Rehabil Med 2008; 40: 451–455
Correspondence address: Stefano Negrini, c/o ISICO, Via Roberto Bellarmino 13/1, IT-20141 Milano, Italy. E-mail: stefano.negrini@isico.it
Submitted October 16, 2007; accepted January 9, 2008
Introduction
The so-called “exercise-dogma”, which states that exercise is of no use in idiopathic scoliosis without proof, is prevalent in certain countries (1). However, in other countries exercises are widely used to treat adolescent idiopathic scoliosis (AIS), especially lower grade cases (2). A few recent systematic reviews have shown the possible effects of exercise on scoliosis in terms of Cobb angle, based on concordant controlled studies, which were mainly observational and partly prospective (2–4). Such results have led to the evidence on exercises being judged as efficacious for avoiding, or at least reducing, the worsening of curvature with a level of evidence of C (multiple controlled non-randomized studies, whose results are consistent with each other) by the Italian Guidelines Committee (5), while the international scientific Society On Scoliosis Orthopedic and Rehabilitation Treatment (SOSORT) has proposed their use and indications (6). Moreover, it has been shown that physical exercises can have a positive influence on breathing function, strength and postural balance, and that they are useful in reducing specific impairments and disabilities of patients with AIS (7–10).
Studies evaluating exercises have, up to now, focused on their efficacy in terms of Cobb angle (2, 4), but no study has reported their usefulness in reducing brace prescription. From the patient’s perspective, avoiding bracing is a key goal, and simply postponing its use for some months could also be important (11). In fact, as treatment ends when growth stops, postponing the start of bracing will reduce the total length of this type of treatment.
A study focusing on brace prescription might look at exercise treatment vs non-treatment, but any active therapy should be compared with another one (or at least a placebo treatment) in order to reduce or eliminate bias. In rehabilitation this might be even more important, due to the key role of human factors. In this respect, Italy represents an ideal opportunity for research into exercise treatment, due to its widespread use, combining the approaches and input of many different schools (12, 13). Today, every rehabilitation centre has its own exercise protocol, as does every physiotherapist. In most cases, the patients perform the same exercises in groups, which are usually not homogeneous with respect to the scoliosis parameters and type of treatment used (e.g. bracing or not). Moreover, these standard treatments may be different in terms of quality, the duration of each session and repetitions per week. Thus, it is evident that these differences may result in a highly variable outcome.
In a previous preliminary study we have shown the efficacy of Scientific Exercises Approach to Scoliosis (SEAS) exercises in reducing the rate of progression of scoliosis compared with usual care, while brace prescription was greatly reduced but this last results was not statistically significant (14). That study included patients who had been treated previously, which could have affected the results. The objective of the current controlled prospective study was to compare the effect of this same protocol of exercises vs usual-care rehabilitation programmes in a group of adolescent patients with low-degree idiopathic scoliosis who had not been treated previously. The primary outcome was to avoid braces, while secondarily we examined the prevention of progression in curvature. The results were also compared with published data on the natural history of AIS and its treatment using exercises (2).
Material and Methods
Patients
Between May 2003 and July 2005, 74 consecutive outpatients with AIS were enrolled in the study. Each patient was attending their first medical evaluation at our institute, none had been treated previously, and all were prescribed exercises to avoid bracing. All patients provided written informed consent to the blind research management of their clinical data. Inclusion criteria were: adolescent idiopathic scoliosis not previously treated, and diagnosed as at risk of bracing according to the Italian Clinical Guidelines and expert medical judgment (5). The data from the medical evaluation included history, scoliosis and growth parameters, sagittal profile, posture, and motor-neurone control. These data can be summarized by the following clinical pictures (which, nevertheless, are not totally inclusive of all cases): (i) proven radiographic progression; (ii) Cobb angle exceeding 15° or Bunnell Angle of Trunk Rotation (ATR) exceeding 7°, first signs of puberty, pre-menarchal and Risser value 0–1; (iii) Cobb angle exceeding 20° and Risser value of 2 or 3. Exclusion criteria were: secondary scoliosis and pathologies known as possible causes of scoliosis (15), neurological deficits, a difference in inferior limb length exceeding 10 mm, previous treatment for scoliosis (brace, exercises or surgery) and Risser value exceeding 3.
The patients themselves decided whether they preferred to be treated according to our exercise protocol (the SEAS group) or by a rehabilitation centre or single physiotherapist of their choice (the usual physiotherapy (UP) group). They were thus divided into 2 groups through self-selection: 35 patients entered the SEAS group (25 females, mean age 12.7 (standard deviation (SD 2.2) years) and 39 entered the UP group (27 females, mean age 12.1 (SD 2.1) years). The mean Cobb angle at the start of treatment was 15° (SD 6°), while the mean ATR was 7° (SD 2°).
Study design
This was a prospective controlled cohort observational study on consecutive outpatients. Moreover, it was a clinical everyday practice study in which the physicians were neutral observers because they were not aware of the study being performed and they were focused only on the patients’ needs, although they were not blinded to the treatment applied. Due to the observational setting, ethical approval was not required. Each patient underwent a complete medical evaluation, during which a physician with expertise in scoliosis measured the Bunnell ATR and radiographic Cobb angles. Clinical evaluations were performed every 6 months and radiographic measurement was performed after 12 months of treatment, when the studied ended.
Treatment
The SEAS group performed SEAS exercises in its 2002 version (2002: SEAS.02) according to the Italian Scientific Spine Institute (ISICO) approach (14, 16). This consists of individually adapted exercises that are taught to the patients in a structure totally dedicated to scoliosis treatment. The patients perform a single session of 1.5 h duration every 2–3 months at our institute, in which they are evaluated by a physiotherapist with expertise in scoliosis, learn a SEAS exercise protocol that is personalized according to medical and physiotherapic evaluations, receive a video record of their performance with physiotherapist’s suggestions, and participate in a family counselling meeting with regard to scoliosis. The patients continue treatment at a rehabilitation facility near their home (by themselves or with their parents) twice a week (40 min per session) plus one daily exercise at home (5 min). The SEAS.02 exercises are based on Active Self-Correction (ASC) (17), which is an active movement performed in order to achieve the maximum possible correction, the goal of which is to activate motor-neurone reflex corrective response (16, 17). The exercises are all performed with respect to ASC and are aimed at spinal stabilization, strengthening of the tonic antigravity muscles, improvement of balance and co-ordination, recovery and maintenance of physiological sagittal curves, and full functional improvement according to physiotherapeutic and medical evaluations (16, 18). Therapists avoid increasing the spine’s range of motion (12, 16, 19, 20), but instead focus mainly on spinal stability.
The UP group participants performed many different exercise protocols at a local facility according to the preferences of their single therapist. In most cases the exercises were performed in a group context, while in all cases they lasted 45–90 min and were performed 2 or 3 times per week. In some cases, the patients were required to repeat their exercises daily at home.
All patients in both groups were also required to participate in sports as a complementary aspect of therapy, without focusing on any particular sports activity.
Outcome measures
The primary measures of outcome included: the number of braced patients, Cobb angle and ATR. Regarding Cobb angle, a modification of > 5° was considered significant (5, 21–23), while for ATR a modification of > 2° was considered significant (5, 23). In a previous study we found a Cobb angel of 3° was the limit of detection of outcome, taking into account intra-observer variations (17). Accordingly, progression was considered clinically significant when it led to a change of treatment (brace prescription), while it was deemed as present when it was greater than the minimal detectable change according to the instruments used. Secondary outcome measures included the sagittal profile, which was assessed by measuring the distance from the plumb-line at the C7 and L3 levels. The method applied has already been validated, and its intra- and inter-operator repeatability measured (24). We also calculated the compliance rate by dividing the number of exercises sessions performed by the expected frequency of 2 sessions per week.
Statistical analysis
The Cobb angle and the ATR were measured for each single curve, and analysis was performed both for the single patients’ average of curves and worst curve. The distribution of variables was first evaluated, and then a full set of paired sample comparisons employed, using parametric or non-parametric tests, as appropriate. The t-test, Mann-Whitney U, Fisher’s exact and χ2 tests were used. A p-value < 0.05 was considered statistically significant.
Results
No statistically significant difference was found between the 2 groups at baseline for any of the scoliosis parameters. The number of sessions per week was 2.0, min per session 48, and compliance rate 95%. In addition, no difference was found between the 2 groups with respect to these parameters. There were 5 drop-outs: 2 females in the SEAS group and 3 (1 male) in the UP group.
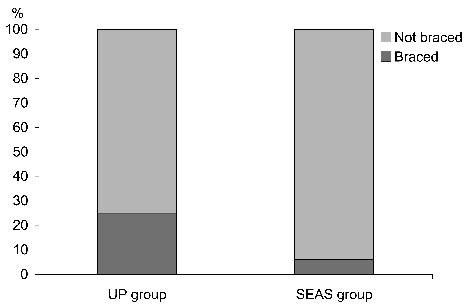
Regarding the 11 braced patients, 81.8% were in the UP group, and the difference between the groups was statistically significant (braced patients comprising 6.1% of the SEAS group vs 25.0% of the UP group) (Fig. 1). A worst-case analysis was performed, considering all drop-outs as braced patients, and the statistical difference remained, while the percentages of failures changed to 11.5% and 30.8% for the SEAS group and UP group, respectively.
Fig. 1. Specific exercises reduce brace prescription in patients at risk: in the UP (usual physiotherapy) group, 9 patients (25%) have been braced due to progression, vs 2 (6%) in the SEAS (Scientific Exercises Approach to Scoliosis) exercises group. The difference was statistically significant (p < 0.05).
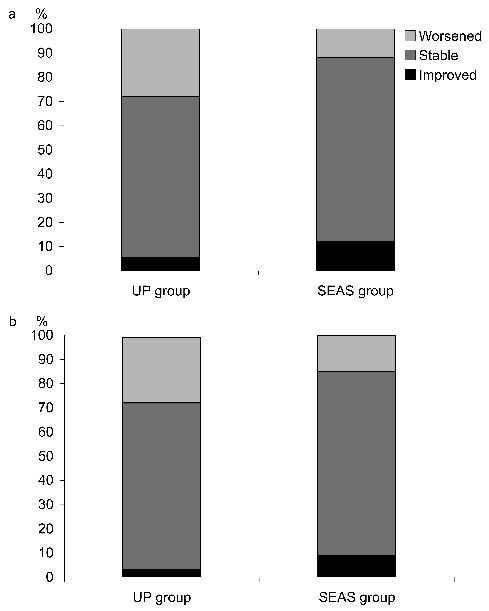
The Cobb angle improved in the SEAS group but worsened in the UP group. Even if they are statistically significant (p < 0.05), these changes cannot be considered clinically significant due to their low values (Table I). Regarding the clinical changes on an individual basis, in the SEAS group we found that 23.5% of patients improved and 11.8% worsened in terms of Cobb angle, vs 11.1% and 13.9%, respectively, in the UP group (Fig. 2a). Examining ATR, in the SEAS group 9.1% improved and 15.1% worsened vs 2.8% and 27.8%, respectively, in the UP group (Fig. 2b). No statistically significant differences were detected in the sagittal profile of the spine.
| Table 1. Mean changes of Cobb angle and Angle of Trunk Rotation (ATR) in the SEAS - Scientific Exercises Approach to Scoliosis exercises group (SEAS group) and usual physiotherapy group (UP group) |
| | Braced Patients | Cobb M | Cobb AC | ATR M | ATR AC |
| Efficacy analysis | Worst-case analysis |
| SEAS group | 2/33 (6%)* | 4/35 (11.5%)* | –0.33 | –0.67* | –0.33 | +0.12 |
| UP group | 9/36 (25%)* | 12/39 (30.8%)* | +1.12 | +1.38* | +0.15 | +0.52 |
| *p < 0.05. Cobb M: changes of Cobb angle of the maximum curve; Cobb AC: changes of Cobb angle of all curves; ATR M: changes of ATR degrees of the maximum curve; ATR AC: changes of ATR degrees of all curves. – reduction (improvement); + increase (worsening). |
Fig. 2. (a) Number of patients radiographically changed (Cobb angle) after treatment in the 2 groups. (b) Number of patients clinically changed (Bunnell Angle of Trunk Rotation (ATR) (degrees)) after treatment in the 2 groups. UP: usual physiotherapy; SEAS Scientific Exercises Approach to Scoliosis
DISCUSSION
The main finding of this study is that specific personalized exercises are more effective than usual care with respect to countering scoliosis and avoiding the prescription of a brace. For adolescent patients, who comprise a group who are at risk of worsening scoliosis, the more specific treatment (SEAS) led to significant improvements in the mean values of all primary outcome measures. Considering the number of braces prescribed, the difference was impressive: 81.8% of braces have been prescribed in the UP group. This parameter documents the clinical value of SEAS and confirms our previous preliminary results in a less homogeneous, more select group of patients (14).
This study was a prospective controlled cohort observational study performed with consecutive outpatients. Moreover, the research was carried out in everyday clinical practice, which has inherant advantages over the disadvantages of the absence of randomization. These advantages include the fact that the treating physicians and physiotherapists were not aware that the study was being performed, and they were focused only on the patient’ needs; this did not require (nor allowed) any blindness. Moreover, the study was based on the everyday feasibility of the treatments, and the outcome parameters reflected the clinical reality. Disadvantages included possible polarization of the population (according to economic, geographic, or other unknown factors) and the absence of blindness.
The main outcome considered (“brace prescription”) is clearly not a fixed term, but is affected by many different individual factors due to the physician (e.g. choice of treatment, fear of progression, etc.) and to the patient and family (e.g. willingness to use a brace, fear of progression, etc.) (11). In this respect the outcome “rate of bracing” is comparable to the outcome “rate of surgery”, which is currently used in the literature as one of the main end-points of scoliosis treatment (25, 26). We are aware of these limitations, but, although inaccurate and affected by the prescribing physician’s attitude and the patient’s perception, “brace prescription” is a clear-cut change of treatment, implying increased human and social costs; and, in this respect, brace prescription can be considered an outcome, particularly in a clinical everyday practice study such as this one, where the physician is always the same and is focused on the patient’s needs and not on the research results.
There are no published data on other exercise protocols that might lead to a reduction in the rate of brace prescription, but there are comparable data on radiographic results in controlled studies (Table II). In a similar population, but using retrospective groups (not including drop-outs), Mollon & Rodot (27) found, at the end of treatment with specific Lyon exercises, that 63% of patients improved vs 20% in the control group. Such data was confirmed in similar studies by Ducongé (28), and by Klisic & Nicolic (29), who found that 58% improved with exercises vs 23% and 26%, respectively, in controls. In all of these studies, a change of ± 3° in the Cobb angle was considered significant, which could explain why the authors found only 5% of stable patients compared with our findings. In order to compare our results with those published previously, we considered the proportion of patients who changed at least 3° in either direction (Table II): this limit was chosen to match that used in the previous papers (27–29), but was also in agreement with a study we performed in which we found, in these small degree curves, an intra-observer variation of 3° was significant to detect a change in either direction (17). The rate of improvement in the UP group was similar to that of the control groups reported above (28%), while the rate of progression was slightly lower than that of the exercise groups (28% vs 34–42%). This means that the UP group also had some efficacy when compared with the literature. This holds true even when taking into account the fact that our results refer to one year of treatment, while previous studies refer to the entire treatment period (3–4.7 years) (25–27). The number of improved patients in the SEAS group was only slightly lower than reported previously, while it appears that the number of worsened patients has been reduced dramatically (to 13%). In general, SEAS exercises have some reduction of efficacy (10%) but are much “safer” (reducing failure by a factor of 2–3). If, in the future, this result of SEAS is confirmed at the end of treatment, further research will be required into the technical explanations for the types of exercises performed.
| Table II. Percentage of patients improved or worsened in our study and in all comparable controlled studies in the literature. To compare our results with those reported in the other studies, we considered individual variations of 3 Cobb degrees as positive or negative changes. |
| Study | Improved (%) | Worsened (%) |
| Exercises | Controls | Exercises | Controls |
| Mollon & Rodot (27) | 63 | 20 | 34 | 75 |
| Klisic & Nikolic (29) | 58 | 26 | 37 | 64 |
| Ducongè (28) | 58 | 23 | 42 | 77 |
| Our study: SEAS group | 45 | | 13 | |
| Our study: UP group | 28 | | 28 | |
| *p < 0.05. SEAS group: Scientific Exercises Approach to Scoliosis (SEAS) exercises group; UP group: usual physiotherapy group. – reduction (improvement); + increase (worsening). |
The other controlled studies in the literature, including the only one whose results were negative (but which had the weakest methodology) (2, 30), and the only one that was prospective and controlled (although it had different treatment teams) (31), are not comparable because of the differences in methodology and patient selection (2). Only one previous study compared 2 treatment protocols (32), but it found no difference according to the protocol used. A multiple linear regression analysis for the changes in Cobb angle as a function of compliance, physical therapist and potentially confounding variables allows one to detect that maximal participation in physical exercise therapy (> 30 min per day), compared with minimal participation (< 10 min per day) could slow down or even halt the progression of the deformity (difference between the groups of 9° Cobb).
Compared with other exercises (UP group), the most specific exercises (SEAS group) showed a better effect in reducing brace prescription at one year. This is an important goal of therapy, particularly from the patient’s perspective (33). Bracing is a psychologically demanding treatment approach (34–37) and compliance has proved to be a major issue (38, 39). The end of bracing is a fixed point that corresponds to the end of growth, so starting bracing one year later is an improvement because it reduces the total time of this type of treatment. Moreover, a new therapeutic tool (instead of simple observation or wait-and-see) can reduce the use of other more invasive treatments, and avoiding scoliosis progression will reduce the severity of the condition of patients who do eventually need bracing. A treatment that can reduce the use of another, more demanding, treatment is always advisable, although future research should also evaluate it in terms of cost vs benefits.
Certain limitations are implicit in the study, since the results relate to only one year of treatment. Although this is usually the most important year, and although this study shows that the use of a brace has been reduced at least for one year in the SEAS group, we will continue to follow these patients until they stop growing. Another aspect is related to the UP group, which was not a placebo group but included different kinds of treatments. We cannot exclude that some patients could have worsened due to poor treatment (although the results were better than the control groups in other studies). Another limitation could be the main measure of outcome. In fact, brace prescription by the treating physician could have been influenced by knowing the types of exercises performed by the patients.
This study is the first to have examined “brace prescription” as an outcome, which is an important factor, both from the patient’s perspective and in terms of cost. The study included a worst-case analysis, in which all drop-outs were considered as failures, and it is the first controlled prospective study published in which both groups were observed by the same physicians.
In conclusion, the results of this study confirm the effectiveness of exercises in adolescent scoliosis patients who are at high risk of progression (2, 4, 5). Moreover, specific and personalized treatment appears to be more effective than usual physiotherapy in reducing the progression of scoliosis.
References
1. Hawes MC. The use of exercises in the treatment of scoliosis. An evidence-based critical review of the literature. In: Hawes MC, O’Brien JP, editors. 4th International Conference on Conservative Management of Spinal Deformities. Boston: SOSORT (Society on Scoliosis Orthopaedic and Rehabilitation Treatment); 2007.
2. Negrini S, Antonini G, Carabalona R, Minozzi S. Physical exercises as a treatment for adolescent idiopathic scoliosis. A systematic review. Pediatr Rehabil 2003; 6: 227–235.
3. Negrini S, Romano M. On “effect of bracing...” Lenssinck et al. Phys Ther 2005; 85: 1329–1339. Phys Ther 2007; 87: 112; author reply –3.
4. Lenssinck ML, Frijlink AC, Berger MY, Bierman-Zeinstra SM, Verkerk K, Verhagen AP. Effect of bracing and other conservative interventions in the treatment of idiopathic scoliosis in adolescents: a systematic review of clinical trials. Phys Ther 2005; 85: 1329–1339.
5. Negrini S, Aulisa L, Ferraro C, Fraschini P, Masiero S, Simonazzi P, et al. Italian guidelines on rehabilitation treatment of adolescents with scoliosis or other spinal deformities. Eura Medicophys 2005; 41: 183–201.
6. Weiss HR, Negrini S, Rigo M, Kotwicki T, Hawes MC, Grivas TB, et al. Indications for conservative management of scoliosis (guidelines). Scoliosis 2006; 1: 5.
7. Mooney V, Gulick J, Pozos R. A preliminary report on the effect of measured strength training in adolescent idiopathic scoliosis. J Spinal Disord 2000; 13: 102–107.
8. Athanasopoulos S, Paxinos T, Tsafantakis E, Zachariou K, Chatziconstantinou S. The effect of aerobic training in girls with idiopathic scoliosis. Scand J Med Sci Sports 1999; 9: 36–40.
9. Weiss HR. The effect of an exercise program on vital capacity and rib mobility in patients with idiopathic scoliosis. Spine 1991; 16: 88–93.
10. Wong MS, Mak AF, Luk KD, Evans JH, Brown B. Effectiveness of audio-biofeedback in postural training for adolescent idiopathic scoliosis patients. Prosthet Orthot Int 2001; 25: 60–70.
11. Negrini S, Carabalona R. Social acceptability of treatments for adolescent idiopathic scoliosis: a cross-sectional study. Scoliosis 2006; 1: 14.
12. Negrini A, Sibilla P, Negrini S. La cinesiterapia nel trattamento della scoliosi: nuovi orientamenti metodologici [Exercises in scoliosis treatment: new methodological approaches]. Riabilitazione oggi 1992; 9: 11–15 (in Italian).
13. Sibilla P. Il trattamento conservativo attivo della scoliosi idiopatica in Italia [Active conservative treatment of idiopathic scoliosis in Italy]. In Negrini S, Sibilla P, editors. Le deformità vertebrali: stato dell’arte. Vigevano: Gruppo di Studio Scoliosi e patologie vertebrali, 2001: 20–41 (in Italian).
14. Negrini S, Negrini A, Romano M, Verzini N, Negrini A, Parzini S. A controlled prospective study on the efficacy of SEAS.02 exercises in preventing progression and bracing in mild idiopathic scoliosis. Stud Health Technol Inform 2006; 123: 523–526.
15. SRS. Scoliosis Reseach Society. Definition of scoliosis term, 2004 [accessed April, 27, 2004] Available at: http://www.srs.org/patient/glossary.asp
16. Negrini S, editor. The evidence-based ISICO approach to spinal deformities, 1st edn. Milan: ISICO, 2007.
17. Negrini A, Negrini S, Romano M, Verzini N, Parzini S, Monticone M, Negrini A. A blind radiographic controlled study on the efficacy of Active Self-Correction according to SEAS.02. In: Kotwicki T, editor. 3rd International Conference on Conservative Management of Spinal Deformities. Poznan (Poland): SOSORT (Society on Scoliosis Orthopaedic and Rehabilitation Treatment); 2006.
18. Romano M, Gerosa L, Ferrari E, Negrini S. Functional evaluation for idiopathic scoliosis: comparison with a normal control group. In: Rigo M ed. 1st International Conference on Conservative Management of Spinal Deformities. Barcelona: SOSORT (Study group on Scoliosis Orthopaedic and Rehabilitation Treatment); 2004.
19. Mollon G. Kinesitérapie des scolioses. Encycl Med Chir 26300.A.104.6.07.
20. Stagnara P, Mollon G, De Mauroy J, editors. Reeducation des scoliosesed. Paris: Expansion Scientifique Francaise; 1990.
21. Negrini S, Negrini A, Santambrogio GC, Sibilla P. Relation between static angles of the spine and a dynamic event like posture: approach to the problem. In: D’Amico M, Merolli A, Santambrogio GC, editors. Three Dimensional analysis of spinal deformities. Amsterdam: IOS Press – Ohmsha; 1995, p. 209–214.
22. Zmurko MG, Mooney JF 3rd, Podeszwa DA, Minster GJ, Mendelow MJ, Guirgues A. Inter- and intraobserver variance of Cobb angle measurements with digital radiographs. J Surg Orthop Adv 2003; 12: 208–213.
23. Grosso C, Negrini S, Boniolo A, Negrini AA. The validity of clinical examination in adolescent spinal deformities. Stud Health Technol Inform 2002; 91: 123–125.
24. Zaina F, Negrini S, Romano M, Aulisa AG. Repeatability of different methods to collect in everyday clinics the sagittal profile of patients with adolescent idiopathic scoliosis. In O’Brien JP, Hawes MC, editors. 4th International Conference on Conservative Management of Spinal Deformities. Boston: SOSORT (Society on Scoliosis Orthopaedic and Rehabilitation Treatment); 2007.
25. Richards BS, Bernstein RM, D’Amato CR, Thompson GH. Standardization of criteria for adolescent idiopathic scoliosis brace studies: SRS Committee on Bracing and Nonoperative Management. Spine 2005; 30: 2068–2075; discussion 2076–2077.
26. Dolan LA, Weinstein SL. Surgical rates after observation and bracing for adolescent idiopathic scoliosis: an evidence-based review. Spine 2007; 32: S91–S100.
27. Mollon G, Rodot J. Scolioses structurales mineures et kinèsitherapie. Etude statistique compareative des rèsultas. Kinesithérapie scientifique 1986; 244: 47–56.
28. Ducongè P. La rèèducation de la scoliose. Mythè ou rèalitè? Rèsonance Europeennes Du Rachis 2002; 10: 1229–1236.
29. Klisic P, Nikolic Z, editors. Scoliotic attitudes and idiopathic scoliosis. Proceedings of the International Congress on Prevention of Scoliosis in Schoolchildren. Milan: Edizioni Pro-Juventute; 1985, p. 91–92.
30. Stone B, Beekman C, Hall V, Guess V, Brooks HL. The effect of an exercise program on change in curve in adolescents with minimal idiopathic scoliosis. A preliminary study. Phys Ther 1979; 59: 759–763.
31. Weiss HR, Weiss G, Petermann F. Incidence of curvature progression in idiopathic scoliosis patients treated with scoliosis in-patient rehabilitation (SIR): an age- and sex-matched controlled study. Pediatr Rehabil 2003; 6: 23–30.
32. Ferraro C, Masiero S, Venturin A. Effect of exercise therapy on mild idiopathic scoliosis. Europa Medicophysica 1998; 34: 25–31.
33. Negrini S, Brambilla C, Carabalona R. Social acceptability of treatments for adolescent idiopathic scoliosis. Pediatr Rehabil 2004; 7: 52–53.
34. Lindeman M, Behm K. Cognitive strategies and self-esteem as predictors of brace-wear noncompliance in patients with idiopathic scoliosis and kyphosis. J Pediatr Orthop 1999; 19: 493–499.
35. Freidel K, Petermann F, Reichel D, Steiner A, Warschburger P, Weiss HR. Quality of life in women with idiopathic scoliosis. Spine 2002; 27: E87–E91.
36. Andersen MO, Andersen GR, Thomsen K, Christensen SB. Early weaning might reduce the psychological strain of Boston bracing: a study of 136 patients with adolescent idiopathic scoliosis at 3.5 years after termination of brace treatment. J Pediatr Orthop B 2002; 11: 96–99.
37. Reichel D, Schanz J. Developmental psychological aspects of scoliosis treatment. Pediatr Rehabil 2003; 6: 221–225.
38. Nicholson GP, Ferguson-Pell MW, Smith K, Edgar M, Morley T. Quantitative measurement of spinal brace use and compliance in the treatment of adolescent idiopathic scoliosis. Stud Health Technol Inform 2002; 91: 372–377.
39. Edgar M. Brace wear compliance [Scoliosis Research Society Internet]. 2003 [accessed 2006 January 8]. Available from: http://www.srs.org/professionals/bracing_manuals/section3.pdf