OBJECTIVE: Camptocormia, or bent spine syndrome, is an acquired postural disease leading to lumbar kyphosis observed when the patient stands up. Classic orthoses and physiotherapy programmes provide little correction and are often poorly tolerated. The aim of this study was to evaluate the effectiveness and tolerance of a new orthosis combined with physiotherapy for treating camptocormia.
METHODS: Fifteen patients (5 men and 10 women, 71.4 (standard deviation (SD) 7.3) years old) consulting for camptocormia were consecutively included in the study. Patients who had pain when they straightened up were excluded. Patients equipped with the orthosis were hospitalized for 5 days in order to learn a self-rehabilitation programme. They were evaluated before and after hospitalization, then at 30 and 90 days.
RESULTS: In comparison with day 0 (without orthosis), the mean increase in lumbar lordosis with the orthosis was 10.1° (SD 9.9) at day 30 (p < 0.05) and 12.5° (SD 9.7) at day 90 (p < 0.001). Average pain values showed a reduction of 69% (SD 36) and 70% (SD 35) in the initial pain at days 30 and 90, respectively. The average increase in quality of life was 87% and 92% at days 30 and 90, respectively.
CONCLUSION: This new orthosis, relying on the principle of thoraco-pelvic anterior distraction, gives excellent results in the treatment of camptocormia.
Key words: camptocormia, treatment, orthosis.
J Rehabil Med 2008; 40: 761–765
Correspondence address: Mathieu de Sèze, Service de Médecine Physique et Réadaptation, Hôpital Pellegrin, FR-33076
Bordeaux, France. E-mail: Mathieu.de-seze@chu-bordeaux.fr
Submitted January 25, 2008; accepted May 29, 2008
Introduction
Camptocormia (or bent spine syndrome) is defined as abnormal posture with marked flexion of the thoraco-lumbar spine. The disorder, which is often attributed to normal ageing, increases during walking and disappears in the supine position or when patients push their hands against their thighs or lean against a wall (1). Camptocormia induces compensation with retroversion of the pelvis and flexion of the knees in order to maintain the centre of mass over the feet. It may cause considerable discomfort and disability. Souques & Rosanoff (1) first described it in 1915 as a psychogenic disorder, but the psychogenic aetiology of camptocormia is rare. The principal organic aetiologies are neurodegenerative and neuromuscular diseases, such as Parkinsonian syndrome, which induces an axial dystonia (2–7), and paravertebral myopathy involving the paravertebral muscles confined to the spinal erector muscles (8–16). However, endocrine-metabolic myopathies (hypothyroidism) and deformities such as osteoarthritis, scoliosis and narrow lumbar spine inducing a biomechanical imbalance may also be involved (8, 17, 18). Camptocormia may reveal a wide range of pathologies (5, 18). It does not have a unique physiopathology and an association of neuromuscular disease and degenerative spine processes is thought to explain its occurrence (5, 19, 20). While adequate treatment may be available (18, 21–23), pharmacological treatment is currently unsatisfactory in most cases (2, 3, 5, 9). Physiotherapy and orthoses are often proposed (17). However, orthoses are rarely reported to be efficient because they are often poorly tolerated and patients stop wearing them (24). The aim of this study was to assess the efficacy and tolerability of a new orthosis on the principle of thoraco-pelvic anterior distraction (TPAD).
Material and MethodS
Patients
A total of 15 patients using the TPAD orthosis were included in the study. Every patient presenting consecutively at the orthopaedic medical unit in Bordeaux for treatment of camptocormia was offered inclusion in the study. Camptocormia was defined as forward flexion of the thoraco-lumbar spine that disappeared in the recumbent position. Patients were excluded if they were not able to stand up or to walk, did not want to wear an orthosis, or experienced back pain when they straightened up.
Study design
The study conformed to the Helsinki protocol for clinical trials. The study was approved by local ethics committee: Comité de protection des personnes Bordeaux A.
After obtaining the patient’s written informed consent, an orthosis was fitted and hospitalization was scheduled for the following 15 days. Clinical and radiological assessments were performed 30 and 90 days later and were compared with the initial data obtained before fitting.
Treatment procedure
TPAD, which is based on the notion that the trunk is composed of 2 thoracic and pelvic girdles linked dorsally by the spine, involves an orthosis comprised of 2 belts encircling the pelvis and thorax that are linked by an anterior upright. In the standing position, the weight of the trunk is supported by the pelvis. The length of the upright may be adjusted by the patients themselves according to their activities (Figs 1 and 2). The patients were hospitalized for 5 days training in the use of the orthosis within 15 days of being fitted with the orthosis. Thereafter, they were encouraged to perform the routine daily and to wear the orthosis as long as they could, but only in situations in which they considered it useful.
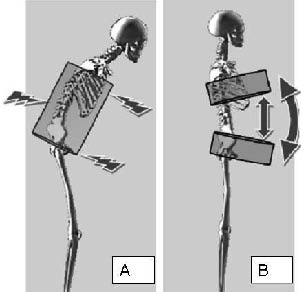
Fig. 1. (A) Effect of a classic orthosis. Arrows show the 3 main points of pressure applied by the orthosis on the trunk. (B) Effect of the thoraco-pelvic anterior distraction orthosis. Circles are the 2 belts of the orthosis and ventral arrows indicate the effect of the upright.
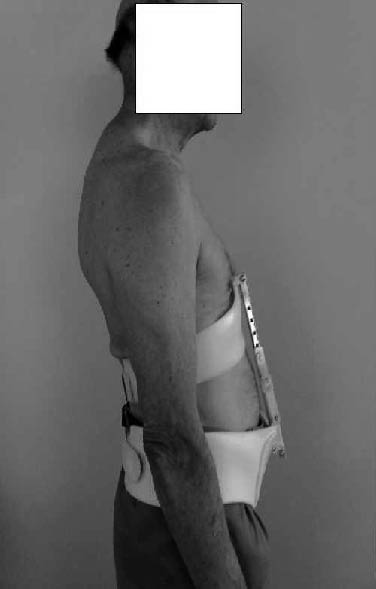
Fig. 2. A patient wearing the thoraco-pelvic anterior distraction orthosis.
Parameters measured included sex, age, medical history, onset of camptocormia, and previous treatments. Pain was assessed on a visual analogue scale (VAS) (where 0 and 100 corresponded to “no pain” and “maximal pain”, respectively). Quality of life was evaluated by a VAS (where 0 and 10 correspond to “very poor quality” and “excellent quality of life”, respectively). Satisfaction was evaluated by a VAS (where 0 and 10 correspond to “total dissatisfaction with orthosis” and “maximal satisfaction with orthosis,” respectively). Orthosis-wearing time per day was evaluated by interviewing the patient at each follow-up. Spine deformity was evaluated in a natural standing posture. In the sagittal plane, it was evaluated as the distance from the C7, T6 and L3 spinous processes to a plumb line tangential to the centre of the buttock. Coronal balance was defined as the distance from the plumb line to the projection of the C7 spinous process in the coronal plane. Radiological assessments of spine curves were evaluated by classical radiological criteria (25, 26) on radiographs performed by a radiologist not involved in the study. Thoracic sagittal kyphosis was measured from the superior endplate of T4 to the inferior endplate of T12. Lumbar lordosis was measured from L1–L5 and was
considered positive or negative when lumbar lordosis or kyphosis was present, respectively. Sagittal balance was measured by joining the line from the centre of T9 to the centre of the femoral head segment, then measuring the angle between the line and the vertical. It was considered positive or negative when T9 was posterior or anterior to the centre of the femoral head segment, respectively. The sacral slope was defined as the angle between the horizontal line and the tangential line to the superior endplate of S1. Scoliosis was measured using the Cobb angle.
The principal criterion for correction was the lumbar lordosis angle, as assessed on profile radiographs.
Statistical analysis
Analysis of variance (ANOVA) with Tukey’s multiple comparison were performed to analyse possible differences between initial values without the orthosis and those recorded at days 30 and 90 with the orthosis. The Student’s t test was performed to analyse possible differences between values of satisfaction and orthosis wearing time recorded at days 30 and 90. A p-value of < 0.05 was considered to be significant.
Results
Clinical features of patients
Fifteen patients were included in this study (5 men and 10 women). Their mean age was 71.4 (standard deviation (SD) 7.3) years. Among the 15 patients, 3 presented scoliosis, 3 an idiopathic primary paravertebral myopathy, 2 had Parkinson’s disease, 2 had Steinert’s myopathy and one had vertebral settling. Four patients presented more than one disease: 2 had Parkinson’s disease with scoliosis, one had Parkinson’s disease with vertebral settling and one had scoliosis with vertebral settling. The mean duration of camptocormia was 23 (SD 13) months (range 6–36 months). In 4 patients, there had been an acute onset (one rupture after laparotomy, one inguinal hernia surgery procedure, one lumbar stenosis surgery and one vertebral settling). Among the 15 patients, 7 had already worn an orthosis. Only one patient was lost to follow-up because of a pelvic tumour diagnosis and another was unable to respond on the VAS because of cognitive disability. Comparison of the data between days 30 and 90 did not show any significant statistical difference (p > 0.05).
Comparison of clinical data
No patient was worsened on any clinical parameters. Average pain values showed significant differences between day 0 (without orthosis) and days 30 and 90 (with orthosis), corresponding to pain reduction of 69% (SD 36) and 70% (SD 35), respectively (Table I). Among the 8 patients experiencing pain, at day 90 the decrease in the initial pain was less than 25% for one patient, between 25% and 75% for 3 patients and more than 75% for 4 patients. The mean increase of 87% and 92% in quality of life was statistically significant at days 30 and 90, respectively. VAS satisfaction scores were similar at day 30 (70.7, SD 19 mm) and day 90 (79.2, SD 18 mm). On average, patients wore the orthosis 7.6 (SD 4) and 7.5 (SD 4) h a day at days 30 and 90, respectively (p > 0.05). Orthosis wearing times per day were more than 8 h for 6 patients, between 4 and 8 h for 5 patients and less than 4 h for 3 patients.
| Table I. Clinical data |
| | Day 0 Mean (SD) | Day 30 Mean (SD) | p | Day 90 Mean (SD) | p |
| Pain VAS, mm | 42.1 (40) | 12.3 (20) | < 0.01* | 11.5 (18) | < 0.01* |
| QoL VAS, mm | 41.1 (23) | 76.9 (17) | < 0.001* | 79.2 (18) | < 0.001* |
| Satisfaction VAS, mm | | 70.7 (19) | | 69.6 (18) | > 0.05† |
| Wearing, h | | 7.6 (4) | | 7.5 (4) | > 0.05† |
| SB at C7, cm | 18.3 (10) | 8.1 (3) | < 0.001* | 7 (3) | < 0.001* |
| SB at T6, cm | 6.5 (5) | 1.6 (1) | < 0.001* | 1 (2) | < 0.001* |
| SB at L3, cm | 3.8 (3) | 3.4 (2) | > 0.05* | 3.6 (1) | > 0.05* |
| CB at C7, cm | 4 (6) | 3 (5) | > 0.05* | 2.5 (5) | < 0.05* |
| *p-value of analysis of variance between day 0 and day 30 or day 90. †p-value of Student’s t-test between day 30 and day 90. VAS: visual analogue scale; QoL: quality of life; SB: sagittal balance; CB: coronal balance; p: probability value; SD: standard deviation. |
Sagittal balance at C7 and T6 improved significantly between day 0, day 30 and day 90 (Table I). Sagittal arrow reductions at C7 were 10.2 (SD 10) cm and 11.3 (SD 9.9) at day 30 and day 90, respectively. Sagittal arrow reductions at T6 were 5 (SD 4.8) cm and 5.5 (SD 4.7) cm at day 30 and day 90, respectively. Sagittal balance at L3 was not statistically different between days 0, 30 and 90.
Comparison of radiological data
Lumbar lordosis increased significantly over the period of follow-up (Table II). An example of the radiological profiles of a patient with classic and TPAD orthoses is shown in Fig. 3.
In comparison with day 0, the average increase in lumbar lordosis was 10.1° (SD 9.9) at day 30 and 12.5° (SD 9.7) at day 90. Thoracic kyphosis increased (i.e. improved) statistically from day 0 to day 90 (p < 0.05) but not from day 0 to day 30 (p > 0.05). The average increase between day 0 and day 90 was 7° (SD 10). Sagittal balance at T9 increased significantly by 11.2° (SD 13.3) between day 0 and day 30 and by 11° (SD 13.8) between day 0 and day 90. There was an increase in the sacral slope between day 0 (21.8°, SD 11), day 30 (23.9°, SD 9) and day 90 (24.2°, SD 9) but it was not statistically significant. Cobb’s angle decreased significantly, by 3° (SD 4.5) between day 0 and day 30, and by 3.2° (SD 5) between day 0 and day 90. Thirteen of 15 patients were able to put the orthosis on by themselves (except one patient in an old people’s home and
another with dementia). Respiratory, digestive and skin tolerance was good. One patient experienced postprandial discomfort. When reported, dissatisfaction involved hindrance with the pole for some activities (5/15) and aesthetic concerns (5/15). Five patients used the orthosis principally for walking.
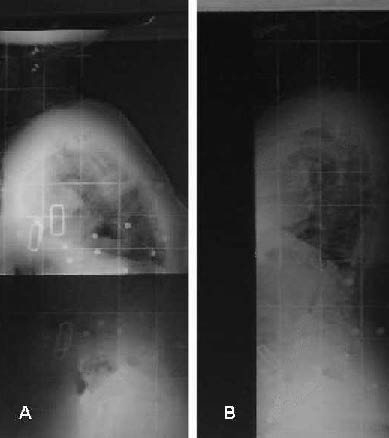
Fig. 3. Radiological profiles. (A) With a classic orthosis. (B) With the thoraco-pelvic anterior distraction orthosis. See the global correction of the forward bent spine between A and B.
| Table II. Radiological data |
| | Day 0 Mean (SD) | Day 30 Mean (SD) | p | Day 90 Mean (SD) | p |
| Lumbar lordosis, degrees | 15.2 (17) | 25.3 (13) | < 0.001 | 27.7 (13) | < 0.001 |
| Thoracic kyphosis, degrees | 29.2 (15) | 34.2 (16) | > 0.05 | 36.3 (17) | < 0.05 |
| Sagittal balance at T9, degrees | 3.1 (17) | 14.3 (9) | < 0.01 | 14.1 (9) | < 0.01 |
| Sacral slope, degrees | 21.8 (11) | 23.9 (9) | > 0.05 | 24.2 (9) | > 0.05 |
| Cobb, degrees | 17.4 (25) | 14.4 (23) | < 0.05 | 14.1 (22) | < 0.05 |
| p: probability value of analysis of variance (ANOVA) test between day 0 and day 30 or day 90; SD: standard deviation. |
Discussion
These findings based on clinical and radiological criteria show that the TPAD orthosis combined with a physiotherapy programme significantly reduced camptocormia and was well tolerated.
To our knowledge, only 2 retrospective studies to date have focused on the wearing of an orthosis associated with a similar physiotherapy programme for the treatment of camptocormia (24, 27). Despite the scarcity of such studies, orthoses are widely thought to be unsatisfactory (3, 5, 9, 18–20). This might be due to the inefficiency of previous orthoses in correcting the forward bent spine. Indeed, the 2 previous studies using objective criteria failed to report any good correction of camptocormia, and could only demonstrate acceptable tolerance of the orthosis and good subjective results (24, 28). In usual orthosis designs, the trunk is considered as flexible tubing and orthoses are designed to exert direct local pressure to correct abnormal posture. The correction obtained by orthoses is usually limited by the painful local pressure they produce. In designing the TPAD orthosis, we considered the trunk as 2 thoracic and pelvic girdles linked dorsally by the spine and separated ventrally by the abdomen, where the thoracic girdle is sustained by the abdominal cushion and the back muscles. Thus, the anterior distraction induced by the pole encourages straightening by anterior compensation of the weakness of the anatomic extensor system, without causing painful local pressure (Fig.1). For this reason, we think that the objective improvement we observed in the present study is mainly due to the new orthosis based on the TPAD technique. Recent flexible orthoses have demonstrated very good tolerance in the context of vertebral fractures caused by osteoporosis because they allow many activities of daily living, such as bending or getting up from a lying position (29, 30, 31). In our series, we think that tolerance was increased by the pole that the patients adjusted themselves, notably to reduce trunk extension when seated. A decrease in the thoracic kyphosis induced by wearing flexible orthoses has been reported in the management of vertebral fractures caused by osteoporosis (30). In our series, the thoracic kyphosis extended largely to the lumbar spine, inducing a globally bent spine and camptocormia. In this context we thought that patients needed stronger ventral compensation that that proposed by Pfeifer et al. (30). For this reason we proposed a ventral upright and not an abdominal pad linked to a metal splint along the spine, as suggested.
In our series, orthosis wearing time remained unchanged between day 30 and day 90 in most cases (n = 9). It increased in 3 patients and decreased in 2. In the management of vertebral fractures caused by osteoporosis the wearing of an orthosis for 2.5 h a day can reduce thoracic kyphosis associated with an increase in back spine strength (30). We did not measure the straightening of the patients when they took off their orthosis because it was not an end-point in the context of camptocormia. Nevertheless, the observation of one patient presenting a Steinert myopathy is interesting to report here. This patient considerably reduced his orthosis wearing time between day 30 and day 90 and wore it for only one h a day at the end of the follow-up. At day 90, he still needed it because camptocormia recurred after a few days without it. His case illustrates the fact that the lumbar spine lordosis is still deficient, and that it induces a sagittal imbalance if the orthosis is not worn. Moreover, about one-third of our patients developed camptocormia after an acute event such as abdominal rupture or vertebral settling, which induced an imbalance of the supporting system. A similar aetiology of the bent spine syndrome has been reported previously (2, 6, 17, 32). Thus, degenerative loss of lumbar lordosis can lead to precarious sagittal spine imbalance, which may be decompensated by a slight forward trunk incline during gait (or by a slight disturbance between the extensor and flexor of the applied forces). This is maybe why camptocormia is principally described in elderly persons and why idiopathic forms or multiple aetiologies, such as dystonia (4, 6, 7, 21–23) or primary myopathy (6, 8–10, 14, 15, 18, 28), have been described previously in the literature. Furthermore, this might account for the fact that our population was varied and could explain why we did not find any differences in efficacy, tolerance and satisfaction between the different classical aetiologies of camptocormia. Since we selected patients with a reducible forward bent curvature, we no longer found any differences between recent and former camptocormia.
The average lordosis values increased and sagittal balance at C7 decreased significantly between day 30 and day 90. However, during the same period, there was no statistically significant reduction in wearing time. It may be that the induced correction of the lordosis is not great enough to attain stable trunk balance. For this reason, further research seems necessary into whether a longer follow-up would demonstrate that such balance is re-established.
In our series, only one patient stopped wearing the orthosis, for a medical reason not associated with the orthosis. This drop-out rate is much lower than in previous studies in which 30–50% of patients stopped wearing their orthosis in the first 3 months because of lack of pain relief or functional discomfort (24, 27). In our series, 46% of the patients subsequently experienced no pain, and the good compliance observed was not due to pain reduction but to correction of the forward bent spine and its functional benefits.
The straightening of the patients and the correction of the lordosis we report in our series can reduce the Cobb angle. A secondary consequence of this phenomenon may be that the TPAD orthosis provides progressive and small, but significant, improvement of frontal balance at C7 (p < 0.05) and of thoracic kyphosis (p < 0.05) at day 90.
A limitation of the present study is the variety of camptocormia aetiologies in this population. Further studies should select patients with a defined clinical context, such as Parkinson’s disease, which was the main aetiology in our series (n =5). Also, it would be interesting to perform a kinematic analysis of the improvement of camptocormia in more dynamic conditions, such as walking. Finally, it would be interesting to perform a controlled trial to compare the TPAD with other orthoses.
In conclusion, these results show that camptocormia can be efficiently corrected with this adapted comfortable orthosis.
ACKNOWLEDGEMENTS
The authors thank Philippe Wentzy (CPO) of the Lagarrigue group who managed the technical procedures. The authors received no contributions from industry for development of this new orthosis.
References
1. Karbowski K. The old and the new camptocormia. Spine 1999; 24: 1494–1498.
2. Bloch F, Houeto JL, Tezenas du Montcel S, Bonneville F, Etchepare F, Welter ML, et al., Parkinson’s disease with camptocormia. J Neurol Neurosurg Psychiatry 2006; 77: 1223–1228.
3. Bouzgarou E, Dupeyron A, Castelnovo G, Boudousq V, Collombier L, Labauge P, et al. Camptocormie révélatrice d’une maladie de Parkinson. Ann Readapt Med Phys 2007; 50: 55–59.
4. Djaldetti R, Mosberg-Galili R, Sroka H, Merims D, Melamed E. Camptocormia (bent spine) in patients with Parkinson’s disease – characterization and possible pathogenesis of an unusual phenomenon. Mov Disord 1999; 14: 443–447.
5. Lepoutre AC, Devos D, Blanchard-Dauphin A, Pardessus V, Maurage
CA, Ferriby D, et al. A specific clinical pattern of camptocormia in Parkinson’s disease. J Neurol Neurosurg Psychiatry 2006; 77: 1229–1234.
6. Shuper A, Keller A, Arbel N, Inbar D, Steinberg T. Trauma-induced dystonia and camptocormia in a child. Pediatr Neurol 2007; 36: 184–185.
7. Tolosa E, Compta Y. Dystonia in Parkinson’s disease. J Neurol 2006; 253 Suppl 7: vii7–vii13.
8. Charpentier P, Dauphin A, Stojkovic T, Cotten A, Hurtevent JF, Maurage CA, et al. Maladie de Parkinson, camptocormie primitive est une myopathie para-vertébrale. Rev Neurol (Paris) 2005; 161: 459–463.
9. Diaz-Guzman J, Nunez-Enamorado N, Ruiz-Jimenez J, Garcia E, Diez-Torres I, Ricoy-Campo JR. Parkinsonismo y camptocormia con miopatía focal espinal: descripción de un caso y respuesta al tratamiento [Parkinsonism and Camptocormia with focal spinal myopathy: case report and responsiveness to treatment]. Rev Neurol 2006; 43: 466–469 (in Spanish).
10. Diederich NJ, Goebel HH, Dooms G, Bumb A, Huber F, Kompoliti K, et al. Camptocormia associated with focal myositis in multiple-system atrophy. Mov Disord 2006; 21: 390–394.
11. Gomez-Puerta JA, Peris P, Grau JM, Martinez MA, Guanabens N. Camptocormia as a clinical manifestation of mitochondrial myopathy. Clin Rheumatol 2007; 26: 1017–1019.
12. Laroche M, Delisle MB. La camptocormie primitive est une myopathie para-vertébrale. Rev Rhum Ed Fr 1994. 61: 481–484.
13. Laroche M, Delisle MB, Aziza R, Lagarrigue J, Mazieres B. Is camptocormia a primary muscular disease? Spine 1995; 20: 1011–1016.
14. Ozer F, Ozturk O, Meral H, Serdaroglu P, Yayla V. Camptocormia in a patient with Parkinson disease and a myopathy with nemaline rods. Am J Phys Med Rehabil 2007; 86: 3–6.
15. Schabitz WR, Glatz K, Schuhan C, Sommer C, Berger C, Schwaninger M, et al. Severe forward flexion of the trunk in Parkinson’s disease: focal myopathy of the paraspinal muscles mimicking camptocormia. Mov Disord 2003; 18: 408–414.
16. Zwecker M, Iancu I, Zeilig G, Ohry A. Camptocormia: a case of possible paraneoplastic aetiology. Clin Rehabil 1998; 12: 157–160.
17. Azher SN, Jankovic J. Camptocormia: pathogenesis, classification, and response to therapy. Neurology 2005; 65: 355–359.
18. Delcey V, Hachulla E, Michon-Pasturel U, Queyrel V, Hatron PY, Boutry N, et al. La camptocormie: un signe de myopathie axiale; A propos de 7 observations. Rev Med Interne 2002; 23: 144–154.
19. de Sèze M, Lavignolle B, Mazaux J, Schaeverbeke T, Tison F, Vital J. Déviations rachidiennes et maladie de Parkinson. Revue de Rhumatisme 2004: 290–296.
20. Mayoux-Benhamou MA. La camptocormie. Ann Readapt Med Phys 2007; 50: 60–61.
21. Hellmann MA, Djaldetti R, Israel Z, Melamed E. Effect of deep brain subthalamic stimulation on camptocormia and postural abnormalities in idiopathic Parkinson’s disease. Mov Disord 2006; 21: 2008–2010.
22. Micheli F, Cersosimo MG, Piedimonte F. Camptocormia in a patient with Parkinson disease: beneficial effects of pallidal deep brain stimulation. Case report. J Neurosurg 2005; 103: 1081–1083.
23. Nandi D, Parkin S, Scott R, Winter JL, Joint C, Gregory R, et al. Camptocormia treated with bilateral pallidal stimulation: case report. Neurosurg Focus 2002; 12: ECP2.
24. Pardessus V, Compere S, Tiffreau V, Blanchard A, Thevenon A. Appareillage par corset cuir des postures camptocormiques: A propos de 31 cas. Ann Readapt Med Phys 2005; 48: 603–609.
25. Diard F, Chateil JF, Hauger O, Moinard M, Ducou-Lepointe H. Imagerie des scolioses de l’enfant et de l’adolescent. J Radiol 2002; 83: 1117–1139; discussion 1141–1142.
26. Lowenstein JE, Matsumoto H, Vitale MG, Weidenbaum M, Gomez JA, Lee FY, et al. Coronal and sagittal plane correction in adolescent idiopathic scoliosis: a comparison between all pedicle screw versus hybrid thoracic hook lumbar screw constructs. Spine 2007; 32: 448–452.
27. Eisennman H, Boyot M, Guillet C, Mulot P. Rachis dégénératif décompensé du sujet âgé: une solution thérapeutique par le corset du vésinet. Revue de Médecine Orthopédique 1991: 42–46.
28. Schranz C, Meinck HM. Primär neurogene und myogene Störungen der Körperhaltung. Orthopade 2004; 33: 583–590.
29. Fink M, Kalpakcioglu B, Karst M, Bernateck M. Efficacy of a flexible orthotic device in patients with osteoporosis on pain and activity of daily living. J Rehabil Med 2007; 39: 77–80.
30. Pfeifer M, Begerow B, Minne HW. Effects of a new spinal orthosis on posture, trunk strength, and quality of life in women with postmenopausal osteoporosis: a randomized trial. Am J Phys Med Rehabil 2004; 83: 177–186.
31 Vogt L, Hubscher M, Brettmann K, Banzer W, Fink M. Postural correction by osteoporosis orthosis (Osteo-med): a randomized, placebo-controlled trial. Prosthet Orthot Int 2008; 32: 103–110.
32. Abdulhadi HM, Kerrigan DC. Camptocormia: a biomechanical analysis. A case report. Am J Phys Med Rehabil 1996; 75: 310–313.