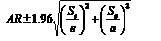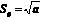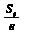OBJECTIVE: A follow-up of accident rate and driving patterns of patients 6–9 years after brain injury.
DESIGN: Postal questionnaire sent to patients with brain injury who were assessed consecutively in the period 1997–2000 and who were re-issued.
SUBJECTS: A total of 93 persons, 69 men and 24 women, mean age 57 years, average 9 years post-injury, 65 persons with brain injury after cerebrovascular accidents and 28 with traumatic brain injury.
METHODS: The questionnaire covered self-reported driving accidents pre- and post-injury, yearly distance driven, behaviour in traffic and self-reported care taken in driving.
RESULTS: The cerebrovascular accident group had reduced their driving significantly post-injury and had also changed their driving patterns. No significant changes were found in distance driven and driving patterns for the group with traumatic brain injury. Compared with normative data, reported accidents post-injury in the cerebrovascular accident group showed no increased accident rate, while the accident rate in the traumatic brain injury-group was more than 2 times higher.
CONCLUSION: Patients with traumatic brain injury represent a risk group for accidents post-injury, while those with brain injury after cerebrovascular accidents do not. Possible causes for this difference are discussed.
Key words: driving, brain injury, accidents.
J Rehabil Med 2008; 40: 733–736
Correspondence address: Anne-Kristine Schanke, Research Unit, Sunnaas Rehabilitation Hospital, 1450 Nesoddtangen, Norway. E-mail: Anne-kristine.schanke@sunnaas.no
Submitted October 1, 2007; accepted May 29, 2008
INTRODUCTION
The need to identify safe drivers among persons with brain injury has been an issue for the last 3 decades (1–8). Today, there is considerable agreement to use multidisciplinary assessments in order to determine whether a person with brain injury should drive, including medical evaluations, neuropsychological assessments, driving simulators and on-road evaluations (3, 6, 9–11). The most valid outcome measure is accident rate. Accident rates for patients not cleared for driving are reported to be high in several studies (12–14). Patients who are permitted to resume driving after thorough assessment, however, show more normal accident rates (3, 15, 16). The aim of the present study was to investigate the accident rate and changes in driving fitness and driving patterns 6–9 years post-injury for patients with traumatic brain injury (TBI) and cerebrovascular accident (CVA) who have been found suited to continue holding a driver’s license.
METHODS
Subjects
Subjects were selected from all patients with CVA and TBI who had been assessed for driving fitness at Sunnaas Rehabilitation Hospital between 1997 and 2000. The assessment included a medical evaluation focusing on cardiovascular diseases, diabetes, seizures, vision/visual field and medication that influenced driving ability and motor control. If no medical contraindications were found, the patients were neuropsychologically assessed, focusing on visual field, visual attention, auditory attention, simple reaction time, motor speed, psychomotor speed, verbal function, visuospatial and visuoconstructive functions and executive function (for description, see Schanke & Sundet (9)). The majority also underwent a practical driving test. From a total of 287 patients assessed, 158 (55%) were found suited. By July 2006, 23 had deceased, reducing the group to 135.
Data collection
Data were collected by postal questionnaire, 100 (74%) patients agreed to participate, 7 had stopped driving and were dropped from the study, leaving 93 subjects for analysis. The 26 non-responders did not differ from the study group with regards to mean age or medical characteristics. Medical characteristics are described in Table I. There were significantly more men with multifocal lesions in the TBI group, 16 out of 28 (57%) were injured in motorcycle or car accidents, and risk behaviour was also a component in many of the other subject’s accidents. Anamnestic data on psychiatric disorders were not collected. The CVA group were significantly older and had held their driver’s licenses longer. Only 5 persons had new diseases affecting driving (3 with CVA and 2 with TBI). The study was approved by the Regional Committee for Medical Research Ethics, East-Norway.
| Table I. Subject characteristics for persons with cerebrovascular accidents (CVA) and traumatic brain injury (TBI) who resumed driving after brain injury |
| | Total n = 93 | CVA n = 65 | TBI n = 28 | t-test/χ2 for differences between CVA and TBI |
| Men/women, % | 74/26 | 68/32 | 89/11 | p = 0.03 |
| Age, years (mean, SD) | 56.4 (13.5) | 61.0 (10.0) | 45.8 (14.8) | p = 0.00 |
| Duration of illness, years (mean, SD) | 9.1 (1.6) | 9.1 (1.7) | 8.9 (1.4) | p = 0.61 |
| Localization of lesion, % | | | | |
| Right hemisphere | 30.1 | 35.4 | 17.9 | |
| Left hemisphere | 33.3 | 40.0 | 17.9 | |
| Multifocal | 29.0 | 18.5 | 53.6 | |
| Brainstem | 3.2 | 4.6 | 0.0 | |
| Uncertain | 4.3 | 1.5 | 10.7 | |
| Education, % | | | | |
| Elementary school 7–10 years | 18.3 | 21.5 | 10.7 | |
| High school, 1–2 years community college | 34.4 | 33.8 | 35.7 | |
| Graduates from high school | 17.2 | 18.5 | 14.3 | |
| College | 16.1 | 12.3 | 25.0 | |
| University | 14.0 | 13.8 | 14.3 | |
| Driver’s license, years (mean, SD) | 34.8 (13.5) | 38.4 (10.9) | 26.2 (15.2) | p = 0.000 |
| Driving pre-injury, years (mean, SD) | 26.3 (13.1) | 29.5 (10.9) | 18.4 (15.0) | p = 0.02 |
| Driving post-injury, years (mean, SD) | 9.1 (1.6) | 9.1 (1.7) | 8.9 (1.4) | p = 0.82 |
| SD: standard deviation. |
Measures
A 51-item questionnaire was developed, covering data pre- and post-injury of reported (to police or insurance companies) and unreported accidents, yearly driving distance, driving patterns, self-perceived traffic behaviour and information from close relatives about driving skills. The questionnaire was an elaborated version of the questionnaires used by Mosberg et al. (16) and Schultheis et al. (3). Not all data are included in this short-form presentation.
Statistical analysis
Data were analysed using SPSS for Windows (14.0). A p-value of less than 0.05 was considered statistically significant. Comparisons between the TBI and CVA group were made using independent samples t-tests, Mann-Whitney U-tests or Pearson’s χ2 tests, dependent on the data distributions. Comparisons of CVA and TBI pre- and post-injury were made using paired sample’s t-tests, Wilcoxon signed-rank tests and McNemar’s tests. Associations between ordinal data were analysed by Spearman’s correlation coefficient. The accident rate (AR) was calculated as the sum of all accidents in the group (a) divided by the total distance driven in the same group (e, exposure). Self-reported car accidents and weekly driving distance were used, reducing the original sample to 65 persons, 39 CVA and 26 TBI. Confidence intervals (95% CI) for AR were calculated according to Bjørnskau (17), taking into account the standard deviation of accident numbers (Sa) and exposure numbers (Se): .
Assuming a Poisson-distribution, . The yearly variation in the exposure data is unknown, but comparisons with Norwegian normative data indicate similar measures and a value of less than 0.2. The AR measurement unit is accidents per million kilometres of driving. For reference numbers, accident rates in the normal population in Norway were adopted from Bjørnskau (17). To examine factors influencing accident rate, a negative binominal regression analysis was used. The following independent variables were included: gender, diagnosis, mean age during the period, driving distance, cause of injury and accident rate pre-injury. Driving distance was included as the logarithm of kilometres driven. A total of 53 subjects were included in this analysis.
RESULTS
Driving patterns pre- and post-injury are shown in Table II. The CVA group had reduced their driving distance and consistently changed their driving patterns. There were no such changes for the TBI group. There were no significant differences in perceived driving skills between the groups (p = 0.27). A negative correlation between age and perceived driving skills was found (p = 0.013). Evaluation of driving skills reported by relatives revealed no significant differences. Table III shows the results from the regression analysis. Unadjusted analysis of the impact of diagnoses on the accident rate showed significant differences between the groups. However, an adjustment made in multiple analysis showed that this result was due to strong confounders, namely gender, driving distance, age, cause of injury and accident rate pre-injury. None of the coefficients were significant. This indicates that the univariate significant difference in accident rate between the CVA and TBI group can be explained by other group differences. Reported accidents were compared with corresponding Norwegian normative data (17). There was no significant difference between the number of reported accidents in the CVA group post-injury and normative data (5.2 vs 6.49 accidents per million km driven). There was a significant difference between the number of reported accidents in the TBI group and normative data (15.0 vs 6.25 accidents per million km driven). The unreported accidents rate post-injury was 3 times higher for the TBI group than for the CVA group (1.7 for 38 subjects in the CVA group and 5.8 for 22 subjects in the TBI group). Comparisons with normative data could not be made.
| Table II. Driving pattern pre- and post-injury for persons with cerebrovascular accidents (CVA) and traumatic brain injury (TBI) who have resumed driving |
| | CVA, n = 65 | | TBI, n = 28 | t-test/ χ2 for differences between CVA pre–post and TBI pre–post |
| Pre-injury | Post-injury | p | Pre-injury | Post-injury |
| Km weekly (mean, SD) | 289.1 (357.7)* | 162.4 (125.5)† | 0.04 | 203.6 (141.3)‡ | 163.5 (128.3)§ | 0.08 |
| Driving frequency, % | | | | | | |
| Daily | 93.4 | 82.0 | | 88.9 | 81.5 | |
| Weekly | 6.6 | 16.4 | | 11.1 | 14.8 | |
| Seldom | 0 | 1.6 | 0.02 | 0 | 3.7 | 0.26 |
| Limiting driving, % | 13.3 | 43.3 | 0.00 | 22.2 | 40.7 | 0.12 |
| Types of limitations, % | | | | | | |
| Driving more slowly | 1.7 | 13.6 | 0.02 | 3.7 | 18.5 | 0.13 |
| Only in day-time | 1.7 | 13.6 | 0.02 | 3.7 | 11.1 | 0.63 |
| With others | 3.4 | 6.6 | 0.50 | 3.7 | 3.7 | 1.00 |
| Avoid highways | 1.7 | 6.8 | 0.25 | 0 | 3.7 | n.a. |
| Avoid cities | 1.7 | 10.2 | 0.06 | 3.7 | 3.6 | 1.00 |
| Avoid rush-times | 3.4 | 13.6 | 0.03 | 11.1 | 11.1 | 1.00 |
| Avoid unknown places | 3.4 | 10.2 | 0.22 | 3.7 | 7.4 | 1.00 |
| Drive only when feeling well | 5.1 | 23.7 | 0.003 | 7.4 | 3.7 | 1.00 |
| Driving Friday and Saturday evenings, % | | | | | | |
| Weekly | 55.4 | 41.1 | | 48.0 | 40.0 | |
| Monthly | 14.3 | 17.7 | | 36.0 | 28.0 | |
| Seldom | 30.4 | 41.1 | 0.02 | 16.0 | 32.0 | 0.08 |
| Place of driving, % | | | | | | |
| Highways | 40.7 | 40.7 | 1.00 | 38.5 | 34.6 | 1.00 |
| Cities | 70.7 | 59.3 | 0.03 | 61.5 | 61.5 | 1.00 |
| Small roads | 58.6 | 55.6 | 1.00 | 65.4 | 61.5 | 1.00 |
| Speeding tickets, % | 29.3 | 18.3 | 0.47 | 42.3 | 39.3 | 0.78 |
| *n = 37, †n = 42, ‡n = 25, §n = 26 SD: standard deviation; n.a.: not applicable. |
| Table III. Results from negative binomial regression analysis (n = 53): regression coefficients, standard deviations, and p-values. Dependent variable is number of reported accidents |
| Variable | Coefficient | SD | p-value |
| Constant | –3.365 | 2.2 | 0.13 |
| Driving distance | 0.207 | 0.18 | 0.24 |
| Sex | 0.926 | 0.62 | 0.14 |
| Diagnoses | 0.202 | 0.59 | 0.73 |
| Accident ratio pre-injury | 0.001 | 0.001 | 0.19 |
| Corrected age | –0.014 | 0.017 | 0.39 |
| Cause of injury | 1.022 | 0.62 | 0.10 |
| SD: standard deviation. |
DISCUSSION
This study had methodological advantages in terms of a long follow-up period (6–9 years) and a fairly high response rate (74%) for patients being comprehensively assessed after brain injury. The statistical analysis revealed a surprisingly consistent response pattern for the 2 groups, strengthening the reliability of the study. The results show that the CVA group has consistently changed their driving behaviour and driving pattern post-injury. The results are in line with the study conducted by Lundqvist et al. (10). The TBI group made no such changes, and took no precautions. This is in contradiction to the findings of Schultheis et al. (3), who found that the TBI group limited their driving in at least one respect compared with controls. The accident rate was high in the TBI group in this study compared with other studies where the subjects have been thoroughly assessed and cleared for driver’s license (3, 15, 16), but the follow-up periods were shorter in other studies. The most likely explanation for the high accident rate in the TBI group was a lack of adequate compensation for their cognitive deficits because of deficits in executive functioning. Moreover, this group is also assessed to have different pre-morbid characteristics. Executive deficits are more difficult to detect than focal deficits in medical and neuropsychological evaluations, and accident-prone behaviour may be suppressed in a limited driving test. Pietrapiana et al. (2) found that pre-morbid personality and driving style accounted for 72.5% of the variance in the outcome measure.
Further research should include larger study groups (multicentre studies), 5–10 years follow-up period and accident rate as an outcome measure for subjects thoroughly assessed for driving fitness. Data on follow-up should include self-reported data, data from close relatives and data from official files. Accident rate post-injury should be compared with the national normative population. Detailed medical and demographic data should be collected, including computer tomography/magnetic resonance imaging scans and Glasgow Coma Scale scores, but also cause of injury, previous accidents and risk behaviour. The neuropsychological assessments should include tests sensitive for executive deficits. Metacognition and personality traits should be assessed by questionnaires, and qualitative observations should be part of the decision-making process.
ACKNOWLEDGEMENTS
The authors would like to thank the subjects for participating in the study, the Health Region of East-Norway for grants and Kathrine Frey Frøslie and Torkel Bjørnskau for help with statistical analysis.
REFERENCES
1. Van Zomeren AH, Brouwer W, Minderhoud JM. Acquired brain damage and driving: a review. Arch Phys Med Rehab 1987; 68: 697–705.
2. Pietrapiana P, Tamietto M, Torrini G, Mezzanato T, Rago R, Perino C. Role of premorbid factors in predicting safe return to driving after severe TBI. Brain Inj 2005; 9: 197–211.
3. Schultheis MT, Matheis RJ, Nead R, Deluca J. Driving behaviours following brain injury: self-report and motor vehicle records. J Head Trauma Rehabil 2002; 17: 38–47.
4. Akinwuntan AE, Feys H, De Weerdt W, Baten G, Arno P. Kiekens C. Prediction of driving after stroke. Neurorehab Neur Repair 2006; 20: 417–423.
5. Lundberg C, Hakamies-Blomqvist L, Almkvist O, Johansson K. Impairments of some cognitive functions are common in crash-involved older drivers. Accident Analysis Prev 1998; 30: 371–377.
6. Bieliauskas LS. Neuropsychological assessment of geriatric driving competence. Brain Inj 2005; 19: 221–226.
7. Goode KT, Ball KK, Sloane M, Roenker DL, Roth DL, Myers RS, Owsley C. Useful field of view and other neurocognitive indicators of crash risk in older adults. J Clin Psych Med Settings 1998; 5: 425–440.
8. Coleman RD, Rapport LJ, Ergh TC, Hanks RA, Ricker JH, Millis SR. Predictors of driving outcome after traumatic brain injury. Arch Phys Med Rehabil 2002; 83: 1415–1422.
9. Schanke AK, Sundet K. Comprehensive driving assessment: neuropsychological testing and on-road evaluation of brain injured patients. Scand J Psych 2000; 41: 113–121.
10. Lundqvist A, Gerdle B, Rönnberg J. Neuropsychological aspects on driving after stroke in the simulator and on the road. Appl Cogn Psych 2000; 14: 135–148.
11. Lew HL, Poole JH, Lee EH, Jaffe DL, Huang HC, Brodd E. Predictive validity of driving-simulator assessments following traumatic brain injury: a preliminary study. Brain Inj 2005; 19: 177–188.
12. Boake C, MacLeod M, High WM Jr, Lehmkul LD. Increased risk of motor vehicle crashes among drivers with traumatic brain injury [abstract]. J Int Neuropsych Soc 1998; 4: 75.
13. Formisano R, Bivona U, Brunelli S, Giustini M, Longo E, Taggi F. A preliminary investigation of road traffic accident rate after severe brain in jury. Brain Inj 2005; 19: 159–163.
14. Leon-Carrion J, Dominguez-Morales MR, Barroso Y, Martin JM. Driving with cognitive deficits: neurorehabiliation and legal measures are needed for driving again after severe brain injury. Brain Inj 2005; 19: 213–219.
15. Haselkorn JK, Mueller BA, Rivara FA. Characteristics of drivers and driving record after traumatic and nontraumatic brain injury. Arch Phys Med Rehabil 1998; 79: 738–742.
16. Mosberg A, Østen PE, Schanke A-K. Bilkjøring etter hjerneskade [Driving after brain injury]. J Norwegian Med Assoc 2000; 120: 3392–3395 (in Norwegian with English abstract).
17. Bjørnskau T. Road traffic risk in Norway 2001–2002. Report 694/2003. Oslo: Institute of Transport Economics.