OBJECTIVE: To examine the effects of 2 manual therapy methods compared with one counselling session with a physiotherapist with “advice-only to stay active” for treating low back pain/leg pain and disability.
DESIGN: A randomized, controlled trial with a 1-year follow-up.
SUBJECTS: A total of 134 subjects with low back disorders.
METHODS: Participants with acute to chronic first or recurrent low back pain, excluding those with “red flag” criteria, were assigned randomly to one of the 3 intervention groups: an orthopaedic manual therapy group (n = 45), a McKenzie method group (n = 52), and an “advice only to be active” group (advice-only) (n = 37). Data on leg and low back pain intensity and disability (Roland-Morris Disability questionnaire) were collected at baseline, and at 3-, 6-, and 12-month follow-up points.
RESULTS: At the 3-month follow-up point, significant improvements had occurred in all groups in leg and low back pain and in the disability index, but with no significant differences between the groups. At the 6-month follow-up, leg pain (–15 mm; 95% confidence interval (CI) –30 to –1), back pain (effect: –15 mm; –27 to –4), and disability index (–4 points; –7 to –1) improved (p < 0.05) more in the McKenzie method group than in the advice-only group. At the 1-year follow-up, the McKenzie method group had (p = 0.028) a better disability index (–3 points; –6 to 0) than did the advice-only group. In the orthopaedic manual therapy group at the 6-month and 1-year follow-up visits, improvements in the pain and disability index were somewhat better than in the advice-only group (p = 0.067 and 0.068, respectively). No differences emerged between the orthopaedic manual therapy and McKenzie method groups in pain- and disability-score changes at any follow-up.
CONCLUSION: The orthopaedic manual therapy and McKenzie methods seemed to be only marginally more effective than was one session of assessment and advice-only.
Key words: educational booklet, McKenzie method, orthopaedic manual therapy, low back pain, back pain.
J Rehabil Med 2008; 40: 858–863
Correspondence address: Markku Paatelma, Härkälahdenkuja 9, FI-00850 Helsinki, Finland. E-mail: markku.paatelma@tcr.fi
Submitted May 31, 2007; accepted June 12, 2008
INTRODUCTION
Back pain is extremely common all over the industrial world, with its high prevalence leading to personal and socioeconomic consequences. For example, in Finland, 33% of women and 29% of men reported having had low back pain (LBP) in the previous month, and 11% of women and 10% of men reported being diagnosed or treated by a physician for LBP in the previous year. Moreover, the prevalence of LBP has not changed over the last 30 years (1).
The European guidelines for management of LBP recommend the treatment of acute non-specific LBP (less than 6 weeks’ duration) with advice to “stay active and continue normal daily activities including work if possible”. They also recommend “considering spinal manipulation for those who are failing to return to normal activities” (2). For non-specific chronic (more than 12 weeks’ duration) LBP in conjunction with supervised exercise therapy “short courses of manipulative therapy can also be considered” (3).
One systematic review of the best synthesis of efficacy of manipulative therapy for LBP showed manual therapy providing either similar or better pain outcomes in the short- and long-term than did placebo or other treatments (4). Another systematic review of the McKenzie method showed that the approach resulted in a greater decrease in pain and disability in the short term than did standard therapies (5). One assessment by a physician and a physiotherapist compared with patients` continuation of daily activity as tolerated proved equally effective in recovery from LBP symptoms (6). In addition, intensive physiotherapy in combination with a neurophysiology education component was effective among patients with chronic LBP (7). One subgroup of patients with LBP with severe disability not responding to conservative treatment were recommended to be treated with a multidisciplinary approach (8). Moreover, the UK Back pain and Exercise And Manipulation (BEAM) Trial study for the effectiveness of physical treatments for back pain in primary care concluded that regarding “best care” in general practice, manipulation followed by exercise achieved a moderate benefit at 3 months and a small benefit at 12 months (9).
A number of conservative treatment methods have been studied for LBP, but controversy remains as to the most effective. Despite those promising studies, no data currently have compared orthopaedic manual therapy (OMT) or the McKenzie method with advice to stay active in subjects with acute to chronic LBP. The aim of this study was to compare the effectiveness of OMT, the McKenzie method, and advice-only to stay active (advice-only) for low back and leg pain intensity and disability among a working-age population.
Material and Methods
Procedure
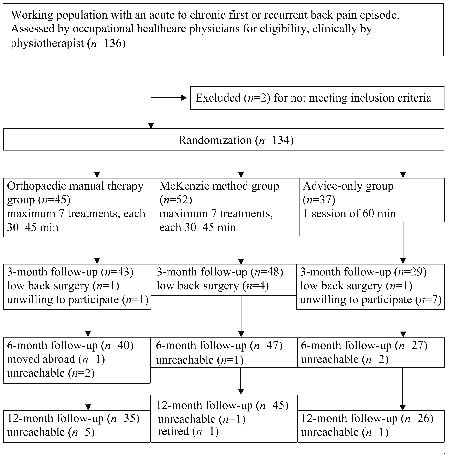
Participants were recruited from 4 occupational health care centres in the city of Jyväskylä, Finland. Occupational physicians were instructed to identify eligible subjects. Everyone who visited the occupational health care centre because of low back trouble and fulfilled the inclusion criteria was recruited. Those patients who visited their occupational physicians 0–7 days after their last episode of LBP had started commenced treatment on day 8, and latest on day 14. Participants completed the questionnaires, were assessed physically, and randomized into the study groups. Outcome measures, which included a battery of self-reported measures (use of healthcare services due to other problems and other back pain treatments) were assessed at 3-, 6-, and 12-month visits (Fig. 1). The measurements were made by one research assistant and coded by another who was blinded to the patient’s group assignment. All the subjects provided written informed consent before the study, and the study protocol was approved by the local ethics committee.
Participants and eligibility
Participants were selected according to the following inclusion criteria: 18–65-year-old employed people with current non-specific LBP with or without radiating pain to one or both lower legs. The back pain episode could be acute to chronic, the first or recurrent. Exclusion criteria were: pregnancy, low back surgery less than 2 months previously, and “red flags” that indicate serious spinal pathology (10).
Randomization
Randomization of the participants into the treatment groups was by a stack of sealed envelopes, numbered in an order prepared from a random number table. The aim was to investigate 180 patients during 3 years, but the final number of participants available was 136, which explains the imbalance in the number of subjects between groups: 45 had been allocated to the OMT group, 52 to the McKenzie, and 37 to the advice-only group. In addition, 2 subjects were excluded as not fulfilling the inclusion criteria (Fig. 1). No significant differences existed between groups at baseline in age, gender, or clinical characteristics (Table I).
Fig. 1. Flow of patients through the trial.
| Table I. Baseline demographics of 134 patients |
| | Groups |
| OMT (n = 45) | McKenzie (n = 52) | Advice-only (n = 37) | p-value |
| Age, years, mean (SD) | 44 (10) | 44 (9) | 44 (15) | 0.93 |
| Gender, female/male | 19/26 | 15/37 | 13/24 | |
| History of previous LBP | | | | 0.64 |
| First episode, % | 9 | 11 | 6 | |
| 1–5 episodes, % | 39 | 45 | 44 | |
| ≥ 6 episodes, % | 52 | 44 | 50 | |
| On sick-leave because of LBP, % | 16 | 17 | 8 | |
| Symptom location | | | | 0.23 |
| Low back pain only, % | 29 | 19 | 31 | |
| Radiating pain to buttock above knee, % | 30 | 54 | 37 | |
| Radiating pain below knee, % | 41 | 27 | 32 | |
| Physical work | | | | 0.43 |
| Sedentary, % | 38 | 33 | 54 | |
| Light, % | 51 | 61 | 32 | |
| Heavy, % | 11 | 6 | 14 | |
| OMT: orthopaedic manual therapy; LBP: low back pain; SD: standard deviation. |
Clinical examination
An LBP history was taken, and a structured examination lasting 45–60 min was carried out by the research assistant before randomization.
Clinical trial
Orthopaedic manual therapy. The OMT group underwent spinal manipulation if indicated (11), specific mobilization, and muscle-stretching techniques (12, 13). In addition, the following mobilization or high velocity, low-force manipulation techniques were performed: (i) translatoric thrust manipulation or mobilization of the thoracic-lumbar junction with the patient supine or lying on their side; (ii) translatoric thrust manipulation or mobilization of L1 to L5 with the patient prone or lying on their side; (iii) the sacroiliac manipulation/mobilization technique used in this study was a ventral or dorsal gliding of the ileum on the sacrum with the patient prone. Furthermore, these patients were taught to perform self-mobilization and stretching exercises at home once a day. Usually 3–5 individually selected home-exercises were prescribed to actively mobilize the low back, with 2–3 sets of 15–20 repetitions for each exercise, and lumbar stabilization exercises with 10 repetitions of 10 sec, and stretching exercises to be performed once a day for 45–60 sec.
McKenzie method of mechanical diagnosis and therapy. In the McKenzie method group, the participants were clinically assessed and classified into the mechanical syndromes. If a non-mechanical syndrome was present, the subjects were transferred from conservative care for further investigations. If a syndrome was present, then one of the treatment principles of mechanical therapy was selected as the management strategy. This consisted of an educational component, supported with the book Treat Your Own Back (14, 15), and an active therapy component provided instructions in exercises repeated several times a day according to the principles of the approach (10–15 repetitions every 1–2 h with or without a sustained end-range position on a regular basis according to symptom response). On occasions, if improvements were not sustained or were too slow developing, patient-generated forces were supplemented by clinician-generated forces: therapist’s over-pressure or mobilization or both within same treatment direction principle of management. “High velocity, low-force” manipulation techniques were avoided in this group during this trial (16).
Advice only. Subjects in the advice-only group received 45–60 min counselling from a physiotherapist concerning the good prognosis for LBP and concerning pain tolerance, medication, and early return to work. The patients in this group were told to avoid bed rest and advised to continue their routine as actively as possible, including exercise activities, within the limits permitted by their back pain. They were also instructed to contact their physicians if their symptoms worsened. For support, a 2-page educational back booklet (translated into Finnish from Burton et al. (18)) was also supplied (17). Other treatments during follow-up were minimal, with no differences between groups.
Number of visits
The number of visits was one for subjects in the advice-only group, and ranged from 3 to 7 in the OMT and McKenzie groups (mean 6 treatments in each group).
Therapists
In both treatment groups, the physical therapists treated their subjects independently by the method in which they were certified. All treatments were provided to each individual participant by the same therapist. The OMT was carried out by a physiotherapist (MP) with 20 years of clinical experience in this field. The McKenzie method was carried out by a physiotherapist (SK) with 10 years of experience in this therapy method. The physiotherapist (RS) who advised the subjects to stay active and continue normal daily living had 5 years of clinical experience in treating patients with LBP.
Outcome measures
Intensity of leg and low back pain. A visual analogue scale (VAS) allowed the subject to rate his or her current intensity of leg and LBP from 0 (no pain/symptoms) to 100 (worst imaginable pain/symptoms) (19).
Disability. A 0–24-point scale Roland-Morris Disability Questionnaire allowed measurement of disability in daily activities in relation to low back trouble in the previous 3 months (20).
Data analysis
The data was analysed by the intention-to-treat principle with post hoc tests using analysis of variance (ANOVA). Post hoc between-group comparisons were performed using Sheffe’s adjustment for multiple comparison. An alternative analysis was conducted that accounted for drop-outs at follow-up, whereby missing values were replaced with imputed values generated by a series of estimated marginal means of measuring 2-tailed equations; subjects’ previous scores were used to determine a predicted value that reduced the variance of the value for each variable. Baseline characteristics were summarized for descriptive purposes with medians and quartiles used for continuous measures and percentages for categorical measures. For all comparisons, a probability of < 0.05 was considered statistically significant (2-tailed) (21, 22).
Results
The absolute values of pain and disability indices at the 3-, 6-, or 12-month follow-up are shown in Table II.
| Table II. Outcome measures at baseline, 3-, 6-, and 12-month follow-up visits, median (25th and 75th quartiles) |
| | Groups |
| OMT (n = 45) | McKenzie (n = 52) | Advice only (n = 37) |
| Baseline values | | | |
| Leg pain, VAS, mm* | 20 (0, 54) | 16 (0, 30) | 16 (0, 30) |
| Low back pain, VAS, mm* | 35 (20, 50) | 32 (20, 42) | 37 (21, 50) |
| Roland-Morris, 0–24† | 9 (5, 8) | 9 (4, 6) | 8 (4, 1) |
| Outcome measures at 3 months | | | |
| Leg pain, VAS, mm* | 6 (0, 14) | 1 (0, 3) | 4 (0, 10) |
| Low back pain, VAS, mm* | 18 (11, 28) | 10 (2, 22) | 17 (10, 28) |
| Roland-Morris, 0–24† | 2 (0, 5) | 1 (0, 6) | 0 (0, 3) |
| Outcome measures at 6 months | | | |
| Leg pain, VAS, mm* | 4 (0, 11) | 1 (0, 4) | 8 (5, 24) |
| Low back pain, VAS, mm* | 14 (10, 21) | 10 (5, 15) | 22 (15, 39) |
| Roland-Morris, 0–24† | 1 (0, 4) | 0 (0, 4) | 1 (0, 7) |
| Outcome measures at 12 months | | | |
| Leg pain, VAS, mm* | 2 (0, 10) | 0 (0, 8) | 8 (0, 21) |
| Low back pain, VAS, mm* | 11 (3, 22) | 8 (0, 23) | 16 (7, 33) |
| Roland-Morris, 0–24† | 0 (0, 2) | 1 (0, 2) | 0 (0, 3) |
| *Self-reported measures included a VAS. †0–24-point scale on Roland-Morris Disability questionnaire. OMT: orthopaedic manual therapy; VAS: visual analogue scale. |
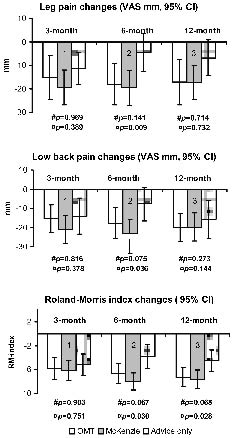
At the 3-month follow-up, improvements occurred in all groups in leg pain (from 11 to 19 mm), LBP (from 14 to 21 mm), and in the Roland-Morris index (from 5 to 6 index-points), but with no significant differences between groups (Fig. 2).
After the 6-month follow-up, the improvement in back pain was better in the McKenzie group (effect: –15 mm; 95% CI: –27 to –4; p = 0.009) and in the disability index (–4 index-points; –7 to –1; p = 0.003), than in the advice-only group. In addition, leg pain improved significantly or almost significantly more in the McKenzie method group (–15 mm; –30 to –1; p = 0.036) and in the OMT group (–14 mm; –28 to 1; p = 0.075) than in the advice-only group (Table III). Leg pain decreased 18 mm in the OMT group, 19 mm in the McKenzie group, and 4 mm in the advice-only group (Fig. 2). The corresponding reductions in back pain was 17 mm in the OMT group, 21 mm in the McKenzie method group, and 8 mm in the advice-only group; and the Roland-Morris index changes were 7, 8, and 4 points, respectively (Fig. 2).
| Table III. Therapy-group differences compared with the advice-only group (mean, 95% confidence interval (CI)) at 3-, 6-, and 12-month visits in pain and disability variables by intention-to-treat analysis |
| | OMT group | McKenzie group |
| Difference (95% CI) | p-value1 | Difference (95% CI) | p-value1 |
| 3-month follow-up | | | | |
| Leg pain, (VAS, mm) | –4 (–18 to 11) | 0.810 | –8 (–22 to 6) | 0.378 |
| LBP, (VAS, mm) | –1 (–14 to 12) | 0.396 | –7 (–20 to 6) | 0.389 |
| Roland-Morris, (0–24) | –1 (–4 to 3) | 0.903 | –1 (–4 to 2) | 0.751 |
| 6-month follow-up | | | | |
| Leg pain, (VAS, mm) | –14 (–28 to 1) | 0.075 | –15 (–30 to –1) | 0.036 |
| LBP, (VAS, mm) | –10 (–22 to 2) | 0.141 | –15 (–27 to –4) | 0.009 |
| Roland-Morris, (0–24) | –3 (–6 to 0) | 0.067 | –4 (–7 to –1) | 0.003 |
| 12-month follow-up | | | | |
| Leg pain, (VAS, mm) | –10 (–25 to 5) | 0.273 | –10 (–23 to 2) | 0.144 |
| LBP, (VAS, mm) | –4 (–17 to 9) | 0.714 | –4 (–17 to 9) | 0.732 |
| Roland-Morris, (0–24) | –3 (–6 to 0) | 0.068 | –3 (–6 to 0) | 0.028 |
| 1p-values are for the between-group differences in the ANOVA (analysis of variance). OMT: Orthopaedic manual therapy; LBP: low back pain; VAS: visual analogue scale; CI: confidence interval. |
After the 12-month follow-up, improvements on the disability index were 3 index-points larger in the McKenzie method group (95% CI: –6 to 0; p = 0.028) and in the OMT group (95%CI; –6 to 0; p = 0.068) than in the advice-only group (Table III). Leg pain decreased in all groups from 7 mm to 17 mm (Fig. 2), back pain from 15 mm to 20 mm (Fig. 2), and Roland-Morris index from 4 to 8 points (Fig. 2).
No significant differences emerged between the OMT and McKenzie method groups in pain and disability scores at any follow-up point. In addition, no inter-group differences emerged during follow-up in visits to physicians or other healthcare professionals or in the use of pain-killers.
Drop-outs
The drop-out rate during the follow-up year ranged from 14% in the McKenzie method group, to 22% in the OMT group, to 30% in the advice-only group. Fig. 1 reveals drop-outs at different follow-up points and shows the reasons for withdrawal. The baseline background values and outcome measures for those subjects who had withdrawn did not differ from those of participants who completed the study except with regards to leg pain. Six participants who had low back surgery during the follow-up period were excluded from this analysis: one each from the OMT and advice-only groups and 4 from the McKenzie method group.
Discussion
The short-term outcomes of this study are in accordance with those of other recent studies (23, 24) showing that the majority of acute LBP disorders are resolved within a 4-week period. This may indicate spontaneous LBP recovery in the short term, but recurrences of LBP are frequent (25). Our results seemed to be somewhat inconsistent. We found no treatment effect immediately after the treatment period at the 3-month check-up. Our results showed small treatment effects only at the 6-month follow-up point in back pain and disability index in favour of the McKenzie method group; the treatment effect was almost significant in leg pain in favour of the OMT and McKenzie method groups and, in addition, at the 12-month follow-up point, the treatment effect was detected in the disability index in the McKenzie method group and also a trend in the OMT group. Our results are in line with those of Cherkin et al. (27), who found that differences in extent of dysfunction among physical therapy, chiropractic manipulation, and educational booklet groups were small and non-significant and approached significance only at one year, with greater dysfunction in the booklet group than in the other 2 groups (27). In addition, the UK BEAM Trial study showed a moderate benefit at 3 months and a small benefit at 12 months after manipulation followed by exercise (9).
In the present study, the drop-out rate was rather high, and was highest in the advice-only group. This is an obvious weakness of this study. Reasons for the rather high drop-out rate in the advice-only group included disappointment that having only one treatment possibility, for many subjects being unreachable because of working in a paper mill with much travelling due to required work responsibilities. It is also possible that those patients who suffered no more LBP during the follow-up were less willing to participate in follow-up measurements. However, the fact that drop-outs did not differ in outcome measures from those who completed the follow-ups strengthens validity. Furthermore, sample size was quite small for a 3-arm trial, making type II error possible. For example, the confidence intervals in Fig. 2 seem to indicate differences, especially between the therapy groups and the advice-only group. A small number of subjects usually makes confidence intervals larger and thus weakens results. Unfortunately, we did not calculate sample size beforehand, but the power analysis shows that the F tests will detect differences between groups equal to those implied by the sample difference.
Fig. 2. Mean changes from baseline at 3-, 6- and 12-month follow-up points in leg pain, low back pain, and Roland-Morris disability index among 26 participants in the advice-only, 35 in the OMT, and 45 in the McKenzie method group who completed the 12-month follow-up. Error bars represents 95% confidence intervals and p-values indicate treatment effects in the OMT(#) and the McKenzie method(¤) groups compared with the advice-only group. CI: confidence interval; VAS: visual analogue scale.
This study had several strengths, e.g. its randomized controlled design and the fact that therapists in the OMT and McKenzie method therapy were very experienced, with over 20 and 10 years experience in the field as therapists as well as teachers. Furthermore, the validity of the VAS and Roland-Morris has been proven to be good (28, 29). Since our participants were recruited by routine referrals from occupational healthcare services, and interventions included commonly delivered treatments, our results can be generalized. According to subjects’ characteristics at baseline, our subjects were similar and corresponded to those of similar studies (30, 31).
The decrease in back pain in the treatment groups was in line with earlier findings (31–33). These studies showed changes similar (56–63% at 3–12 months follow-up on LBP) to those in this study. The Roland-Morris index improved in the treatment groups and the advice-only group much the same as in the studies of Frost et al. (34) and Wand et al. (31). They found from 18% to 69% changes in an up-to-12-month follow-up in their physiotherapy group or in their advice and therapy group. Their advice group showed changes from 10% to 57%, which was of the same magnitude as we observed.
In the present study, we did not classify patients into acute, subacute or chronic LBP, although it would have been useful to examine each of these subgroups separately. Because of our small sample size, however, such sub-group analyses based on duration of LBP could not be conducted. Earlier history, clinical signs of back problems, and other physical, psychosocial, and individual factors are associated with back pain-related outcomes among a working population (35) and should be taken into consideration in interpreting any results.
Clinical practice guidelines for management of sub-acute LBP recommend advice, mobilization, manipulation, exercise or analgesics or a combination of these. OMT and the McKenzie method include advice, exercise, and mobilization, and, if needed, manipulation. Ideally, there would be some way of identifying the subgroups most likely to benefit from one or all of these therapies, using for instance a prediction rule depending on the patient’s present status to achieve better results (36–38).
Previous studies (18, 30) and the recent study of Hancock et al. (39) suggest that advice supported by a booklet is a useful intervention compared with the usual care given by a general practitioner, but only if the information is reinforced by all involved in the patient’s care (18, 29). Counselling is cheap and quite easy to implement and probably well accepted, and thus should be an alternative treatment in non-specific LBP. Although the difference between OMT and McKenzie methods compared with advice-only favoured the therapy groups to some extent, this finding was not clinically meaningful at any stage of follow-up. However, in all groups, the reduction in pain and disability was clinically significant at one year. For example, a reduction of approximately 2 points (20 mm) or of approximately 30% (30 mm) on a VAS in LBP and 5 points or 50%, respectively, on the Roland-Morris Disability Index, represent a clinically important difference (40, 41).
In conclusion, some improvements appeared in all groups in leg and LBP and in disability. The OMT and McKenzie groups showed no consistent treatment effect at different follow-up points compared with the advice-only group in these quite heterogenic non-specified LBP patients. However, a slightly trend emerged that the OMT and McKenzie method groups showed some small treatment effect compared with the advice-only group.
References
1. Helakorpi S, Uutela A, Prättälä R, Puska P, editors. Health behaviour among Finnish adult population., Helsinki: Publications of the National Public Health Institute B 10/1997; Spring 1997.
2. van Tulder M, Becker A, Bekkering T, Breen A,Carter T, Real M, et al. European guidelines for the management of acute non-specific low back pain in primary care. 2004. Eur Spine J 2006; 15 Suppl 2: S169-S191.
3. Airaksinen O, Brox JI, Cedraschi C, Hildebrant J, Klaber-Moffet J, Kovacs F, et al. European guidelines for the management of chronic non-specific low back pain. 2004. Eur Spine J 2006 Mar; 15 Suppl 2: S192-S300.
4. Haas M, Evans RL, Bouter LM. Efficacy of spinal manipulation and mobilization for low back pain and neck pain: a systematic review and best evidence synthesis. Spine J 2004; 4: 335–356.
5. Clare H, Adams R, Maher C. A systematic review of efficacy of McKenzie therapy for spinal pain. Aust J Physiother 2004; 50: 209–216.
6. Karjalainen K, Malmivaara A, Pohjolainen T, Hurri H, Mutanen P, Rissanen P, et al. Mini-interventions for subacute low back pain: a randomized controlled trial. Spine 2003; 28: 533–540.
7. Moseley GL, Nicholas MK, Hodges PW. A randomized controlled trial of intensive neurophysiology education in chronic low back pain. Clin J Pain 2004; 20: 324–330.
8. Bogduk N. Management of chronic low back pain. Med J Aust 2004; 180: 79–83.
9. UK BEAM Trial Team. United Kingdom back pain exercise and manipulation (UK BEAM) randomised trial: effectiveness of physical treatments for back pain in primary care. BMJ 2004; 329: 1377.
10. Bigos S, editor. Acute low back problems in adults. Clinical practice guideline. Agency for Health Care Policy and Research, AHCPR Publication No. 95-0643: Rockville, USA; 1994.
11. Krauss J, Evjenth O, Creighton D, editors. Translatoric spinal manipulation. A Lakeview Media LLC Publication: Minneapolis, USA; 2006.
12. Kaltenborn FM, Evjenth O, Kaltenborn TB, Morgan D, editors. Manual mobilization of the joints. The Kaltenborn method of joint examination and treatment, valid. The spine. 4th edn. Norli Bokhandel: Oslo, Norway; 2003.
13. Evjenth O, Hamberg J, editors. Auto-stretching. Alfta Rehab Förlag: Alfta, Sverige; 1989.
14. McKenzie R, editor. Treat your own back. Waikanae, New Zealand: Spinal Publication Ltd; 1985.
15. Udermann B, Spratt KF, Donelson R, Mayer J, Graves J. Can a patient educational book change behaviour and reduce pain in chronic low back pain patients? Spine 2004; 4: 425–435.
16. McKenzie RA, May S, editors. The lumbar spine mechanical diagnosis and therapy. Waikanae, New Zealand: Spinal Publication Ltd; 2003.
17. Takala J-P, editor. Älä suotta kärsi selkäkivusta. [Don’t suffer needlessly]. Muskeli Project, 1995. University of Huddersfield, Spinal Research Unit: Back Pain; 1995 (in Finnish).
18. Burton A, Waddell G, Tillotson K, Summerton N. Information and advice to patients with back pain can have a positive effect. A randomized controlled trial of a novel educational booklet in primary care. Spine 1999; 24: 2484–2491.
19. Scott J, Huskisson E. Vertical and horizontal visual analogue scales. Ann Rheum Dis 1978; 38: 560.
20. Roland M, Fairbank J. The Roland – Morris Disability Questionnaire and the Ostwestry Disability Questionnaire. Spine 2000; 25: 3115–3124.
21. Hicks CM, editor. Research methods for clinical therapists. Applied project design and analysis (3rd edn) Churchill Livingstone, Edinburgh, UK: Harcourt Publisher Ltd; 2000.
22. Sim J, Wright C. Research in health care: concepts, design and methods. Cheltenham: Stanley Thornes; 2000.
23. Burton AK, McClune T, Clarke R, Main C. Long-term follow-up of patients with low back pain attending for manipulative care: outcomes and predictors. Manual Therapy 2004; 9: 30–35.
24. Gudavalli M, Cambron J, McGregor M, Jedlicka J, Keenum M, Ghanayem A, et al. A randomized clinical trial and subgroup analysis to compare flexion-distraction with active exercise for chronic low back pain. Eur Spine J 2005; 8: 1–13.
25. Croft PR, Macfarlane GJ, Papageorgiou AC, Thomas E, Silman AJ. Outcome of low back pain in general practice: a prospective study. BMJ 1998; 316: 1356–1359.
26. Hides JA, Jull GA, Richardson CA. Long-term effects of specific stabilizing exercises for first-episode low back pain. Spine 2001; 26: E243–E248.
27. Cherkin D, Deyo R, Battié M, Street J, Barlow W. A comparison of physical therapy, chiropractic manipulation, and provision of an educational booklet for the treatment of patients with low back pain. N Engl J Med 1998; 339: 1021–1029.
28. Price D, McGrath P, Rafii A, Buchingham B. The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain 1983; 17: 45–56.
29. Rocchi M, Sisti D, Benedetti P, Valentini M, Bellagamba SA. Critical comparison of nine different self-administered questionnaires for the evaluation of disability caused by low back pain. Eura Medicophys 2005; 41: 275–281.
30. Little P, Roberts L, Blowers H, Garwood J, Cantrell T, Langridge J, et al. Should we give detailed advice and information booklets to patients with back pain? A randomised controlled factorial trial of self management booklet and doctor advice to take exercise for back pain. Spine 2001; 26: 2065–2072.
31. Wand B, Bird C, McAtrhur J, McDowell M, De Souza L. Early intervention of acute low back pain. A single-blind randomized trial of biopsychosocial education, manual therapy, and exercise. Spine 2004; 21: 2350–2356.
32. Niemisto L, Rissanen P, Sarna S, Lahtinen-Suopanki T, Lindgren KA, Hurri H. Cost-effectiveness of combined manipulation, stabilizing exercises, and physician compared to physician consultation alone for chronic low back pain: a prospective randomized trial with 2-year follow-up. Spine 2005; 30: 1109–1115.
33. Pengel L, Refshauge K, Maher C. Responsiveness of pain, disability, and physical impairment outcome patients with low back pain. Spine 2004; 29: 879–883.
34. Frost H, Lamb S, Doll H, Carver T, Stewart-Brown S. Randomized controlled trial physiotherapy compared with advice for low back pain. BMJ 2004; 239: 708–714.
35. Videman T, Ojajärvi A, Riihimäki H, Troup J. Low back pain among nurses. A follow-up beginning at entry to the nursing school. Spine 2005; 30: 2334–2341.
36. Childs J, Fritz J, Flynn T, Irrgang J, Johnson K, Majkowski G, Delitto A. A clinical prediction rule to identify patients with low back pain most likely to benefit from spinal manipulation: a validation study. Ann Intern Med 2004; 141: 920–928.
37. Laslett M, McDonald B, Tropp H, Aprill CN, Oberg B. Agreement between diagnoses reached by clinical examination and available reference standards: a prospective study of 216 patients with lumbopelvic pain. BMC Musculoskelet Disord 2005; 6: 28.
38. Laslett M, McDonald B, Aprill CN, Tropp H, Oberg B. Clinical predictors of screening lumbar zygapophyseal joint blocks: development of clinical prediction rules. Spine J 2006; 6: 370–379.
39. Hancock MJ, Maher CG, Latimer J, McLachlan AJ, Cooper CW, Day RO, et al. Assessment of diclofenac or spinal manipulative therapy, or both, in addition to recommended first-line treatment for acute low back pain: a randomised controlled trial. Lancet 2007; 370: 1638–1643.
40. Lauridsen HH, Hartvigsen J, Manniche C, Korsholm L, Grunnet-Nilsson N. Responsiveness and minimal clinically important difference for pain and disability instruments in low back pain patients. BMC Musculoskelet Disord 2006; 25: 82.
41. Farrar JT, Young JP Jr, LaMoreaux L, Werth JL, Poole RM. Clinical importance of changes in chronic pain intensity measured on an 11-point numerical pain rating scale. Pain 2001; 94: 149–158.