OBJECTIVE: To critically summarize the effectiveness of physiotherapy in patients presenting clinical signs of shoulder impingement syndrome.
DESIGN: Systematic review.
METHODS: Randomized controlled trials were searched electronically and manually from 1966 to December 2007. Study quality was independently assessed by 2 reviewers using the Physiotherapy Evidence Database (PEDro) scale. If possible, relative risks and weighted mean differences were calculated for individual studies, and relative risks or standardized mean differences for pooled data, otherwise results were summarized in a best evidence synthesis.
RESULTS: Sixteen studies were included, with a mean quality score of 6.8 points out of 10. Many different diagnostic criteria for shoulder impingement syndrome were applied. Physiotherapist-led exercises and surgery were equally effective treatments for shoulder impingement syndrome in the long term. Also, home-based exercises were as effective as combined physiotherapy interventions. Adding manual therapy to exercise programmes may have an additional benefit on pain at 3 weeks follow-up. Moderate evidence exists that passive treatments are not effective and cannot be justified.
CONCLUSION: This review shows an equal effectiveness of physiotherapist-led exercises compared with surgery in the long term and of home-based exercises compared with combined physiotherapy interventions in patients with shoulder impingement syndrome in the short and long term; passive treatments cannot be recommended for shoulder impingement syndrome. However, in general, the samples were small, and different diagnostic criteria were applied, which makes a firm conclusion difficult. More high-quality trials with longer follow-ups are recommended.
Key words: shoulder impingement syndrome, physical therapy, treatment outcome, review.
J Rehabil Med 2009; 41: 870–880
Correspondence address: Thilo Oliver Kromer, Physiotherapiezentrum, Grube 21, DE-82377 Penzberg. E-mail: Thilo.Kromer@EPID.unimaas.nl, tok@ptz-physio.de
Submitted October 24, 2008; accepted June 29, 2009
INTRODUCTION
Many primary care patients with shoulder complaints show clinical signs of subacromial impingement and rotator cuff tendinopathy (1, 2). Subacromial impingement syndrome (SIS) of the shoulder is characterized by pain and functional restrictions, mostly during overhead activities (3). Many clinicians believe that the diagnosis shoulder pain is too broad to provide sufficient information to develop specific treatment protocols in daily practice. Systematic reviews on the rehabilitation of patients with SIS included studies in which patients had received surgery beforehand, used conflicting criteria defining the same condition (4–7), and sometimes included invasive interventions not relevant for physiotherapists (8, 9). The present review aims to summarize current evidence for the effectiveness of physiotherapy in the treatment of patients presenting with clinical signs indicative for SIS. Therefore, studies were included if shoulder patients were either diagnosed with SIS or showed pne of the following positive clinical signs indicating SIS: pain aggravating with overhead activity; a painful arc; a Neer impingement test; or a Hawkins-Kennedy test. Although the diagnostic value of these tests in terms of sensitivity and specificity is not clear (10), focusing on important clinical signs guiding inclusion criteria for a review seems to correspond better with daily clinical practice. In primary care general practitioners and physiotherapists often rely solely on clinical signs and symptoms to establish a diagnosis and to determine the focus of treatment (11, 12). To further strengthen this review only randomized controlled trials of high methodological quality were included.
METHODS
Literature search/search strategy
The following databases were searched electronically: MEDLINE (from 1966 to December 2007), EMBASE (from 1988 to December 2007), CINAHL (from 1982 to December 2007), the Cochrane database of systematic reviews (to December 2007), the Cochrane Central Register of Controlled Trials (to December 2007), Physiotherapy Evidence Database (PEDro) (to December 2007). We therefore used the following MeSH terms and key words: physiotherapy, physical therapy specialty, physical therapy modalities, musculoskeletal manipulations, shoulder impingement syndrome, shoulder joint, shoulder pain, tendinopathy, rotator cuff, exercise therapy, exercise movement technique, electric stimulation therapy, massage. Additionally, the “Cochrane optimum trial search strategy” (13) was executed in MEDLINE. Furthermore, reference lists from retrieved articles and systematic reviews were screened for additional relevant publications.
Inclusion criteria
To minimize bias this review contains only randomized controlled trials. Articles written in English, German and Dutch were considered eligible. All identified articles were judged for eligibility by title and abstract (TOK). If eligibility was unclear, a full text version of the article was retrieved. For the screening process a standardized eligibility form was used. Unclear articles were read by a second reviewer (UGT) and discussed until consensus was reached.
For inclusion of a study, participants must demonstrate the clinical pattern of SIS. Therefore, studies in which participants have been diagnosed with SIS were included. Furthermore, other studies were also included if the patients showed at least one of the following signs typical for SIS: pain with overhead activities; painful arc sign; Neer impingement sign; or a positive Hawkins-Kennedy sign. All subjects had to be older than 16 years of age. Studies including subjects with adhesive capsulitis, frozen shoulder, osteoarthritis, fractures, systemic infections and systemic diseases, neoplasm or metastasis, and professional athletes were excluded. All forms of active and passive physiotherapeutic interventions, including exercises, proprioceptive training, manual therapy, massage therapy, education, and electrophysical procedures, were included. They could have been compared with no intervention, placebo treatment, other physiotherapeutic procedures, to each other, or even to surgical interventions. If a combination of therapies was applied, the main intervention and the co-interventions must have been clearly defined to assign the study to a specific intervention. If the main intervention was not defined or was unclear, it was assigned to the group of “combined physiotherapy interventions”. Comparisons between invasive techniques, such as acupuncture, injections, or surgical interventions, were not considered.
Outcome measures
The focus of this review lies on outcome measures for pain and functioning.
Quality assessment
All studies were scored with the PEDro critical appraisal tool for experimental studies in physiotherapy (http://www.pedro.fhs.usyd.edu.au). PEDro is a reliable tool (14) and contains 8 criteria for assessing internal validity of a study, and 2 criteria for assessing sufficiency of the statistical information displayed. Each criterion can be answered with “yes” or “no”. “Yes” was rated with 1 point, “no” with zero points. Thus, the possible maximum score is 10 points. A detailed description of the PEDro criteria is provided in Table I. If a criterion was unclear even after discussion, no points were awarded. All articles were independently rated by a second reviewer (UGT); inconsistency of the ratings was discussed and solved by consensus. To improve the validity of the results, only studies of a high methodological quality, defined as a minimum PEDro score of 5 out of 10, were included in this review.
| Table I. Criteria of the Physiotherapy Evidence Database (PEDro) critical appraisal tool for randomized controlled trials |
| 1 | Subjects were randomly allocated into groups (in a crossover study, subjects were randomly allocated in order in which treatments were received) |
| 2 | Allocation was concealed |
| 3 | The groups were similar at baseline regarding the most important prognostic indicators |
| 4 | There was blinding of all subjects |
| 5 | There was blinding of all therapists who administered the therapy |
| 6 | There was blinding of all assessors who measured at least one key outcome |
| 7 | Measures of at least one key outcome were obtained from more than 85% of the subjects initially allocated |
| 8 | All subjects for whom outcome measures were available received the treatment or control condition as allocated or, where this was not the case, data for at least one key outcome was analysed by “intention to treat” |
| 9 | The results of between-group statistical comparisons are reported for at least one key outcome |
| 10 | The study provides both, point measures and measures of variability for at least one key outcome |
Data extraction and analysis
Data from studies were extracted with the help of a standardized data extraction form. When sufficient data were provided, relative risks (RR) with a 95% confidence interval (95% CI) were calculated for dichotomous data, weighted mean differences (WMD) with 95% CI were calculated for continuous data. When possible and appropriate, studies were pooled for meta-analytical purposes. Data were calculated with Review Manager (ver. 4.2.9) from the Cochrane Collaboration (15). When pooling was not possible a best-evidence synthesis was performed using the levels of evidence described by van Tulder et al. (16), provided in Table II. Consistency of results was given if more than 75% of the studies showed results in the same direction.
| Table II. Levels of evidence |
| Strong | Consistent findings among multiple high-quality RCTs |
| Moderate | Consistent findings among multiple low-quality RCTs and/or CCTs and/or one high-quality RCT |
| Limited | One low-quality RCT and/or CCT |
| Conflicting | Inconsistent findings among multiple trials (RCTs and/or CCTs) |
| No evidence from trials | No RCTs or CCTs |
| CCT: controlled clinical trial, RCT: randomized controlled trial. |
RESULTS
Search results
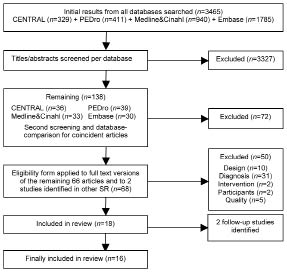
The initial search resulted in 3465 hits. After screening the articles by title and abstract, and after deleting duplicates, 66 articles remained. Additional screening of identified systematic reviews added another 2 articles. The Cochrane optimum search strategy executed in Medline identified no additional papers. Therefore, 68 full text papers were retrieved for detailed evaluation with the help of a standardized eligibility form. Of these, 45 papers were excluded because of inappropriate diagnosis, study design, intervention, or participants. Another 5 studies (17–21) were excluded because of a methodological quality score below 5 out of 10. A total of 18 articles were included in this review. Of these, 2 studies (22, 23) were follow-ups of the initial studies (24, 25), thus, a final total of 16 studies remained. A flow-chart of the search process is shown in Fig. 1.
Fig. 1. Search and screening process. SR: systematic reviews.
Quality of studies
The mean methodological quality of all studies included was 6.8 (range 5–9) out of 10; results of the methodological quality scorings for included studies are shown in Table III. Although random allocation was performed in all studies, in only 4 studies was treatment allocation concealed (25–28) but not properly described. Subjects were blinded in 6 studies (29–34), therapists in 4 (29–32) and assessors in 12 studies (24, 27–37). In all studies except one (26) groups were comparable at baseline. Only one study (34) lost more than 15% of the patients who were initially allocated to the groups during follow-up. The median follow-up time of the included studies was 11 (range 3–416) weeks.
| Table III. Scorings of methodological quality of included studies |
| Study | 1. Random allocation | 2. Concealed allocation | 3. Baseline comparability | 4. Blinding subject | 5. Blinding therapists | 6. Blinding assessors | 7. Outcome data > 85% | 8. Intention-to-treat | 9. Between-group results | 10. Point measures/ measures of variability | PEDro score |
| Aktas et al. (32) | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 0 | 1 | 1 | 8 |
| Bang & Deyle (36) | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 0 | 1 | 1 | 6 |
| Binder et al. (33) | 1 | 0 | 1 | 1 | 0 | 1 | 1 | 0 | 1 | 0 | 6 |
| Brox et al. (22, 24) | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 7 |
| Chard et al. (34) | 1 | 0 | 1 | 1 | 0 | 1 | 0 | 0 | 1 | 0 | 5 |
| Conroy & Hayes (37) | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 0 | 1 | 1 | 6 |
| Dickens et al. (27) | 1 | 1 | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 8 |
| Ginn & Cohen (35) | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 0 | 1 | 1 | 6 |
| Haahr et al. (23, 25) | 1 | 1 | 1 | 0 | 0 | 0 | 1 | 1 | 1 | 1 | 7 |
| Johansson et al. (28) | 1 | 1 | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 8 |
| Ludewig & Borstad (26) | 1 | 1 | 0 | 0 | 0 | 0 | 1 | 1 | 1 | 1 | 6 |
| Nykänen (29) | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 0 | 1 | 1 | 8 |
| Saunders (30) | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 9 |
| Vecchio et al. (31) | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 0 | 1 | 1 | 8 |
| Walther et al. (38) | 1 | 0 | 1 | 0 | 0 | 0 | 1 | 1 | 1 | 0 | 5 |
| Werner et al. (39) | 1 | 0 | 1 | 0 | 0 | 0 | 1 | 1 | 1 | 0 | 5 |
| PEDro: Physiotherapy Evidence Database. |
Population
The median sample size of the included studies was 56 (range 14–138) patients. All studies except one (26) included men and women with a similar mean age. Unfortunately, information about the duration of symptoms was missing in 4 studies (26, 27, 29, 37). A detailed description of the population is given in Table IV.
| Table IV. Overview of included studies – quality, population, and intervention |
| Study Quality score | Population | Diagnosis Inclusion criteria | Intervention |
| Dickens et al. (27) 8 | Sample: n = 85, (37 f, 48 m) mean (range) age 55 years (27–68), all on a waiting list for surgery Duration of symptoms: NA Follow-up: 6 months Drop-outs: 12 | Diagnosis: subacromial impingement syndrome. Inclusion criteria: (i) clinical history and examination; (ii) radiographic findings; (iii) diagnostic local anaesthetic injections into the subacromial space and ac-joint. | Group 1 (n = 45): individualized rehabilitation programme based on the findings from the initial assessment. all patients received all or some of the following modalities: physiotherapy once or twice a week including mobilization of acromioclavicular joint, cervical spine, thoracic spine, glenohumeral joint, postural advice, strapping, electrotherapy; progressive exercise therapy (for scapulothoracic and rotator cuff muscles) with Theraband resistance; after sufficient instruction, exercises were performed twice a day at home. Group 2 (n = 40): no intervention. Additional interventions for both groups: analgesics as necessary. |
| Ludewig & Borstad (26) 6 | Sample: n = 67, all male, mean age 49 years Duration of symptoms: NA Follow-up: 10 weeks Drop-outs: no | Diagnosis: impingement syndrome. Inclusion criteria: (i) current pain in the glenohumeral joint region; (ii) at least 2 positive impingement signs (Neer, Hawkins/Kennedy, Yocum, Jobe, Speeds test) and pain reproduction during 2 of the 3 categories: (i) painful arc with active abduction; (ii) tenderness with palpation of the rotator cuff or biceps tendon; (iii) pain with one or more glenohumeral joint movements (FLEX, ABD, IR, ER). | Group 1 (n = 34): daily home-based exercises for 10 weeks including pectoralis minor stretch, posterior shoulder stretch, trapezius relaxation exercise, strengthening of serratus anterior with dumbbells, and of shoulder ER with Theraband resistance. Group 2 (n = 33): no intervention. Group 3 (n = 25, healthy controls): no intervention. |
| Walther et al. (38) 5 | Sample: n = 60 (26 f, 34 m), mean (range) age Group 1: 52 years (40–66); Group 2: 51.5 years (37–66); Group 3: 48.6 years (25–61) Duration of symptoms (mean): Group 1: 23 months; Group 2: 32 months; Group 3: 27 months Follow-up: 6, 12 weeks Drop-outs: no | Diagnosis: impingement syndrome. Inclusion criteria: (i) clinical examination; (ii) radiographs in 3 planes; (iii) ultrasound; (iv) subacromial injection of 10 ml bupivacaine (Neer test). | Group 1 (n = 20): exercises 5 times a week for 12 weeks including isometric strengthening of shoulder ABD, ER and EXT, and rowing with a Theraband; trapezius and supraspinatus stretching, pendulum exercises with a dumbbell. Group 2 (n = 20): physiotherapy for 12 weeks (mean: 30 sessions). Instructions were “centring training for the shoulder rotators and stretching”. Group 3 (n = 20): functional brace for 12 weeks during the day and night if possible. Additional interventions for both groups: NSAIDs as necessary. |
| Werner et al. (39) 5 | Sample: n = 40, (20 f, 20 m) mean (range) age Group 1: 52 years (40–66); Group 2: 51.5 years (37–66) Duration of symptoms (mean): Group 1: 23 months; Group 2: 32 months Follow-up: 6, 12 weeks Drop-outs: no | Diagnosis: impingement syndrome Inclusion criteria: (i) clinical examination; (ii) radiological examination; (iii) sonographic assessment. | Group 1 (n = 20): exercises 5 times a week for 12 weeks, including isometric strengthening of shoulder ABD, ER and EXT, and rowing with a Theraband; trapezius and supraspinatus stretching, pendulum exercises with a dumbbell. Group 2 (n = 20): physiotherapy for 12 weeks (mean: 30 sessions). instructions were “centring training for the shoulder rotators and mobilization”. Additional interventions for both groups: NSAIDs as necessary. |
| Ginn & Cohen (35) 6 | Sample: n = 138, (56 f, 82 m) mean age years (range) 55 years (22–90), subgroup impingement: n = 61 Duration of symptoms (mean): Group 1: 7.4 months; Group 2: 7.3 months; Group 3: 7.4 months Follow-up: 5 weeks Drop-outs: subgroup impingement: 5 | Diagnosis: shoulder pain Inclusion criteria: (i) over 18 years of age; (ii) unilateral shoulder pain with local mechanical origin; (iii) more than 1 months duration; (iv) pain exacerbated with active movements; (v) all patients in the impingement subgroup showed a painful arc of flexion and/or abduction. | Group 1 (n = 48): single subacromial injection with methylprednisone acetate. Group 2 (n = 48): daily home-based exercises for 5 weeks, individualized for each patient on the basis of the initial assessment, supervision once a week for progression; exercises to restore dynamic stability and co-ordination of the shoulder muscles including stretching of shortened muscles, strengthening of weak muscles, motor retraining to improve scapula-humeral rhythm and co-ordination between muscles. Group 3 (n = 42): electrophysical modalities (interferential therapy, ultrasound, ice packs, hot packs) twice a week; passive joint mobilization of the glenohumeral, acromioclavicular and sternoclavicular joints twice a week based on the information from the initial examination; daily ROM exercises (ABD, FLEX, EXT, horizontal FLEX and EXT, HBB) against elastic resistance for 5 weeks to increase range of hand placement. Additional interventions for both groups: patients were requested not to commence or change medication during the study. |
| Bang & Deyle (36) 6 | Sample: n = 52, (22 f, 30 m,) mean (SD) age 43 years (9.1) Duration of symptoms (mean): Group 1: 5.6 months; Group 2: 4.4 months Follow-up: after treatment & 2 months Drop-outs: 2 | Diagnosis: impingement syndrome Inclusion criteria: one test of category 1 must be positive together with one positive test of category 2 or 3. Category 1: passive shoulder flexion with scapula stabilized, passive internal rotation at 90° shoulder flexion in the scapular plane and in progressive degrees of shoulder adduction. Category 2: active shoulder abduction. Category 3: resisted break-test in ABD, resisted break-test in ER or IR. | Group 1 (n = 28): 6 sessions of physiotherapist-led exercises (see Group 2) plus manual therapy within 3 weeks; application of manual therapy techniques based on information from a detailed examination of the patient aiming to restore mobility of the glenohumeral joint, shoulder girdle, thoracic spine, and cervical spine; other treatments were soft tissue massage and stretching of the pectoralis major, infraspinatus, teres minor, upper trapezius, sternocleidomastoid, and scalenus musculature; specific home exercises were given to the patient to reinforce manual treatment. Group 2 (n = 23): 6 physiotherapist-led sessions of a standardized flexibility and strengthening program in 6 levels of tubing resistance within 3 weeks including shoulder FLEX, scaption, rowing, horizontal extension-external rotation, seated press up, elbow push up plus, stretches for the anterior and posterior shoulder musculature. Additional interventions for both groups: patients remained on current medication levels during the study. |
| Conroy & Hayes (37) 6 | Sample: n = 14, (6 f, 8 m) mean age 52.9 years Duration of symptoms: NA Follow-up: after treatment Drop-outs: 1 | Diagnosis: primary impingement syndrome Inclusion criteria: pain about the superolateral shoulder region and one or more of the following: (a) active ROM deficits in humeral elevation; (b) painful subacromial compression; (c) limited functional movement patterns in an elevated position. | Group 1 (n = 7): 9 sessions within 3 weeks (see Group 2) plus manual mobilization of the subacromial and glenohumeral joints including inferior, posterior, and anterior glides, and long-axis traction depending on the results of the initial examination. Group 2 (n = 7): 9 physiotherapist-led sessions within 3 weeks including: hot packs; stretching exercises (cane-assisted FLEX and ER, towel-assisted IR, arm-assisted horizontal adduction); strengthening exercises (chair press, IR and ER isometrics); pendulum exercises and exercises for postural correction; 10 min of soft tissue mobilization (effleurage, friction and kneading techniques). |
| Brox et al. (22, 24) 7 | Sample: n = 125, f (%): age years (range): 18–66 Group 1: 36; Group 2: 50; Group 3: 56; Duration of symptoms ITT, n Group 1: < 6 months: 8; 6–12 months: 8; 1–3 years: 9; > 3 years: 20 Group 2: < 6 months: 5; 6–12months: 5; 1–3 years: 5; > 3 years: 14 Group 3: < 6 months: 6; 6–12 months: 6; 1–3 years: 13; > 3 years: 25 Follow-up: 3, 6 months, 2.5 years. Drop-outs: 25 at 3 months, 5 at 6 months, 12 at 2.5 years | Diagnosis: stage 2 impingement Inclusion criteria: (i) 18–66 years of age; (ii) shoulder pain for at least 3 months resistant to physiotherapy and non-steroid and steroid anti-inflammatory medication; (iii) dysfunction or painful arc on ABD; (iv) pain (2 out of 3) with resisted or eccentric ABD in 0°, ABD in 30° or ER of the shoulder; (v) positive impingement tests; (vi) normal glenohumeral ROM; diagnosis was confirmed with subacromial injection of Lignocaine (pain-free after 15 min). | Group 1 (n = 45): arthroscopic surgery consisting of bursectomy and resection of the lateral and anterior part of the acromion and the coracoacromial ligament followed by physiotherapy and exercises. Group 2 (n = 30): 12 sessions of placebo laser within 6 weeks. Group 3 (n = 50): 2 supervised exercise sessions per week plus home exercises on the other days for 3–6 months with supervision gradually being reduced; initially relaxed repetitive movements for rotation, FLEX, EXT, ABD, and ADD; then gradually added resistance to strengthen the short rotators and the scapula-stabilizing muscles; 3 lessons of education about shoulder anatomy and function, ergonomics, and pain management. Additional interventions for both groups: NSAIDs and analgesics were allowed. |
| Haahr et al. (23, 25) 7 | Sample: n = 84, (58 f, 26 m) mean (SD) age 44.4 years (7, 8) Duration of symptoms, n Group 1: < 6 months: 3; 6–12 months: 10; > 12 months 29 Group 2: < 6 months: 4; 6–12 months: 3; > 12 months 34 Follow-up: 3, 6, 12 months; 4, 8 years Drop-outs: 5 at 4–8 years follow-up | Diagnosis: subacromial impingement syndrome Inclusion criteria: (i) 18–55years of age; (ii) shoulder pain; (iii) symptoms between 3 months and 3 years; (iv) painful arc on ABD; (v) positive impingement sign (Hawkins sign), (vi) positive impingement test. | Group 1 (n = 43): 19 sessions physiotherapy (up to 60 min each) within 12 weeks including heat application, cold packs or soft tissue treatments; active training of the periscapular muscles; strengthening of the rotator cuff. active exercises were done at home daily for another 12 weeks, then the frequency was reduced to 3 times a week. Group 2 (n = 41): subacromial decompression (bursectomy with partial resection of the antero-inferior part of the acromion and the coracoacromial ligament) followed by active home exercises including rotator cuff exercises for 6–8 weeks. |
| Nykänen (29) 8 | Sample: n = 73, (11 f, 62 m) mean (SD) age Group 1: 66 (6); Group 2: 67 (9) Duration of symptoms: NA Follow-up: 1, 4, 12 months Drop-outs: 8 | Diagnosis: painful shoulder Inclusion criteria: (i) shoulder pain of at least 2 months duration, (ii) painful arc between 40°–120° of ABD or other painful movements, (iii) painful supraspinatus test. | Group 1 (n = 36): 10 min of ultrasound (pulse ratio 1:4, intensity 1 w/cm2, frequency 1.0 mHz); 10–12 sessions within 3–4 weeks. Group 2 (n = 37): sham treatment. Additional interventions for both groups: massage of neck and shoulder muscles; group gymnastics to stretch and strengthen the scapulo-humeral and cervical musculature; NSAIDs and analgesics as necessary. |
| Johansson et al. (28) 8 | Sample: n = 85, (59 f, 26 m) mean (SD) age Group 1: 49 (7); Group 2: 49 (8) Duration of symptoms, n Group 1: 2–3 months: 13; 4–6 months: 8; 7–12 months: 10; > 12 months: 13 Group 2: 2–3 months: 11; 4–6 months: 10; 7–12 months: 11; > 12 months: 9 Follow-up: 5 weeks; 3, 6, 12 months Drop-outs: 21 | Diagnosis: impingement syndrome Inclusion criteria: (i) 30–65 years of age; (ii) pain located in the proximal lateral aspect of the upper arm, especially during arm elevation; (iii) positive Neer impingement test; (iv) at least 2 months duration. | Group 1 (n = 44): 10 sessions acupuncture (30 min each) within 5 weeks; needling of 4 local and one distal point. Group 2 (n = 41): 10 sessions of continuous ultrasound for 10 min each (intensity 1 w/cm2, frequency 1.0 mHz) within 5 weeks, located inferior to the anterior and lateral part of the acromion. Additional interventions for both groups: daily home exercises for 5 weeks: active/assistive FLEX; active ER; isometric FLEX, EXT, IR and ER, ABD; ER with a rubber tube; medication if necessary. |
| Saunders (30) 9 | Sample: n = 24, (12 f, 12 m) mean (SD) age 50.3 years (8.2) Duration of symptoms (mean): Group 1: 3.86 months; Group 2: 3.32 months Follow-up: 3 weeks Drop-outs: no | Diagnosis: supraspinatus tendinitis Inclusion criteria: (i) full passive ROM of the shoulder; (ii) impingement on full elevation; (iii) pain on resisted ABD in an “empty can position”; (iv) tenderness on palpation of the tendon. | Group 1 (n = 12): 180 sec laser treatment, 3 sessions per week for 3 weeks; intensity 40 mW, 30 J/cm2 at the surface, located at the point of maximum tenderness at the anterior shoulder and the tendon below the acromion with the patient`s hand placed behind the back. Group 2 (n = 12): sham laser. Additional interventions for both groups: advice on how to use the arm with tape and written instructions. |
| Vecchio et al. (31) 8 | Sample: n = 35, (25 f, 10 m,) mean (range) age 54.4 years (17–77) Duration of symptoms (mean): 14.9 months (whole sample) Follow-up: 4, 8 weeks Drop-outs: no | Diagnosis: rotator cuff tendinitis Inclusion criteria: (i) painful arc between 40°–120° of ABD; (ii) painful resisted movement of ABD, IR or ER. | Group 1 (n = 19): 2 laser sessions of 10 min twice a week for 8 weeks; intensity 30 mW, 1 J/3 mm2; 3 pulses (3 J) to 5 points of maximum tenderness in the subacromial and anterior shoulder regions found on clinical examination. Group 2 (n = 16): sham treatment. Additional treatment for both groups: home exercises including: pendulum exercises in FLEX and EXT, ABD and ADD, wall-climbing exercises; 2 mg paracetamol daily if necessary. |
| Aktas et al. (32) 8 | Sample: n = 46, (30 f, 10 m) (without drop-outs); mean (SD) age Group 1: 48.7 (9.0); Group 2: 53.9 (11.2) Duration of symptoms (mean): Group 1: 4.8 months; Group 2: 4.8 months Follow-up: 3 weeks Drop-outs: 6 | Diagnosis: subacromial impingement syndrome Inclusion criteria: (i) radiography and magnetic resonance imaging; (ii) positive subacromial injection test; (iii) positive impingement tests (Neer, Hawkins-Kennedy, painful arc). | Both groups: Codman’s pendulum exercises for 3 weeks, 5 times a day and subsequent cold application for 20 min, meloxicam tablet 15 mg daily. Group 1 (n = 23): 25 min pulsed electromagnetic field therapy, 5 days a week for 3 weeks. Group 2 (n = 23): sham treatment. |
| Binder et al. (33) 6 | Sample: n = 29, (8 f, 21 m) mean age Group 1: 54.4; Group 2: 53.2 Duration of symptoms (mean) Group 1: 9.2 months; Group 2: 9.5 months Follow-up: 4, 6, 8, 16 weeks Drop-outs: no | Diagnosis: rotator cuff tendinitis Inclusion criteria: (i) shoulder pain aggravated by movement against resistance in ABD, IR or ER; (ii) active movements limited by pain; (iii) full passive ROM; (iv) painful arc on ABD. | Group 1 (n = 15): daily pulsed electromagnetic field therapy for 8 weeks; patients used the coil for 5–9 h with each treatment session lasting at least 1 h. Group 2 (n = 14): sham treatment (4 weeks), then real treatment (4 weeks). Additional treatment for both groups: paracetamol as necessary. |
| Chard et al. (34) 5 | Sample: n = 49, (18 f, 25 m) (without drop-outs), mean age (without drop-outs) Group 1: 50.1 Group 2: 52.8 Duration of symptoms (mean) Group 1: 14.6 months; Group 2: 14.2 months Follow-up: 2, 4, 6, 8 weeks Drop-outs: 6 | Diagnosis: rotator cuff tendinitis Inclusion criteria: (i) shoulder pain aggravated by movement against resistance in ABD, IR or ER; (ii) active movements limited by pain; (iii) full passive ROM; (iv) painful arc on ABD. | Group 1 (n = 25): low-dose electromagnetic field therapy for 2 h daily; application with a “live unit” and a coil switching off after 2 h; patients wore the unit for 8 h daily. Group 2 (n = 24): low-dose electromagnetic field therapy for 8 h daily; application with a “live unit” 8 h daily. Additional treatment for both groups: NSAIDs as necessary. |
| ABD: abduction; ADD: adduction; ER: external rotation; EXT: extension; f: female; FLEX: flexion; HBB: hand behind back; IR: internal rotation; ITT: intention to treat; m: male; NA: not available; NSAIDs: non-steroidal anti-inflammatory drugs; ROM: range of motion; SD: standard deviation. |
Outcome measures
All studies measured pain and functioning, but with a wide range of different types of assessment methods and tools. The measurement instruments used in each study are described in Table V.
| Table V. Overview of included studies – outcome measures and results |
| Study | Outcome measures (pain and function) | | Results for between-groups comparison | WMD (95% CI) (fixed effects model) | RR (95% CI) (fixed effects model) |
| Dickens et al. (27) | Patients refused surgery after intervention | 6 months | + | | 21.93 (1.34–360.2) |
| Ludewig & Borstad (26) | Shoulder rating questionnaire (for function). Work related pain (6 items scored on a 1–10-point scale). Work related disability (4 items scored on a 1–10-point scale). | 10 weeks 10 weeks 10 weeks | + (G1 vs G2) + (G3 vs G1) + (G1 vs G2) + (G3 vs G1) + (G1 vs G2) + (G3 vs G1) | 6.9 (0.6–13.2) 16.0 (9.1–22.9) 1.3 (0.5–2.1) 1.4 (0.5–2.3) 1.2 (0.4–2.0) 1.2 (0.3–2.1) | |
| Walther et al. (38) | Constant-Murley-Score (total score only) (ranges from 0 to 100 points, with higher scores indicative of better function. Subscales for function (60 points), pain (15 points), and strength (25 points). | | 0 between all groups and for all follow-ups | | |
| Werner et al. (39) | Constant-Murley-Score (total score only) (ranges from 0 to 100 points with higher scores indicative of better function). Subscales for function (60 points), pain (15 points), and strength (25 points). | | 0 for all follow-ups | | |
| Ginn & Cohen (35) | Pain with a standardized reaching task (rated on a VAS 0–10). Self-reported functional limitation score (9 items scored on a 0–4-point scale). | 5 weeks 5 weeks | 0 between all groups 0 between all groups | | |
| Bang & Deyle (36) | Self-reported functional assessment questionnaire (9 items, 0–5 point scale). Pain composite score (active ABD, resisted ABD, IR, ER, and functional pain, all scored on a VAS). Functional pain score (9 items scored on a VAS). | AT 2 months AT AT 2 months | + + + + + | 4.7 (1.3–8.6) 186.2 (55.3–317.2) 128.7 (39.4–218.0) | |
| Conroy & Hayes (37) | Maximum 24 h pain (scored on a VAS 0–10) after treatment. Pain with subacromial compression (scored on a VAS 0–10). Overhead function (3 overhead activities scored on a 3-point scale). | AT AT AT | + + 0 | 33.4 (6.4–60.4) 31.1 (4.6–57.6) | |
| Brox et al. (22, 24) | Neer shoulder score > 80 points (ranges 10–100 points with higher scores indicative of better function. Subscales for pain (35 points), function (30 points), active ROM (25 points), anatomical & radiological evaluation (10 points)). Neer shoulder score > 80 points. Pain with activity, at rest, and at night (scored on a 1–9 point scale). Two functional activities (“can you carry a shopping bag?”, “can you take something from a wall cupboard?”). | 6 months (ITT) 2.5 years (ITT). 3 & 6 months 2.5 years 2.5 years | + (G1 vs G2) + (G3 vs G2) 0 (G1 vs G3) + (G1 vs G2) + (G3 vs G2) 0 (G1 vs G3) + (G1 & 3 vs G2) + (G1 vs G3) + (G1 & 3 vs G2) 0 (G1 vs G3) + (G1 & 3 vs G2) 0 (G1 vs G3) | | 2.7 (1.4–5.4) 2.5 (1.2–4.9) 0.9 (0.7–1.2) |
| Haahr et al. (23, 25) | Change in Constant score (ranges from 0–100 points with higher scores indicative of better function. Subscales for function (20 points), ROM (40 points), pain (15 points), and strength (25 points). PRIM score (questionnaire to assess pain and dysfunction, ranges from 0 to 36 points with lower scores indicative of better function). Change in PRIM score. Recovered or improved in PRIM score. DREAM-indices (index of marginalization, sick leave and disability pension in Denmark). | 3 months 6 months 12 months 12 months 4–8 years 8 years 4 years | 0 0 0 0 0 0 0 | 4.6 (–3.3 to 12.5) 1.4 (–7.6 to 10.4) 4.2 (–5.1 to 13.5) 0.0 (–11.8 to 11.8) 2.3 (–2.1 to 6.7) | 1.1 (0.8–1.6) |
| Nykänen (29) | Self reported ADL-index. Self reported pain-index. Supraspinatus pain test (scored on 0–3 point scale). Arc of initial pain with active abduction (in degrees). | 4 weeks 4 months 12 months 4 weeks 4 months 12 months 4 weeks 4 weeks | 0 0 0 0 0 0 0 0 | 0.1 (–0.3 to 0.5) –0.5 (–1.6 to 0.6) –0.3 (–1.4 to 0.8) –0.2 (–0.8 to 0.4) 0.0 (–2.2 to 2.2) 0.0 (–2.2 to 2.2) 0.0 (–0.3 to 0.3) 4.0 (–15.9 to 23.9) | |
| Johansson et al. (28) | Mean of the total scores of 3 shoulder-specific assessment scales (Constant-Murley Shoulder Score, Adolfsson-Lysholm S houlder Score, UCLA Score). | 5 weeks (ITT) 3 months (ITT) 6 months (ITT) 12 months (ITT) | 0 0 0 0 | –3.0 (–7.3 to 1.3) –3.0 (–8.3 to 2.3) 0.0 (–6.8 to 6.8) –3.0 (–8.8 to 2.8) | |
| Saunders (30) | Pain (scored on a pain analogue scale). Pain diary (self-rating on a pain analogue scale). | 3 weeks 3 weeks | + + | | 5.0 (1.4–18.2) 2.0 (1.0–4.1) |
| Vecchio et al. (31) | Painful arc score (scored on a 0–3 point scale). Change scores for night pain (scored on a VAS). Change scores for rest pain (scored on a VAS). Change scores for movement pain (scored on a VAS). Change score of functional limitation of ADL (scored on a VAS). | 4 weeks 8 weeks 4 weeks 8 weeks 4 weeks 8 weeks 4 weeks 8 weeks 4 weeks 8 weeks | 0 0 0 0 0 0 0 0 0 0 | 0.0 (–0.7 to 0.7) 0.3 (–0.6 to 1.2) 1.3 (–1.1 to 366) 1.2 (–1.7 to 4.1) 0.8 (–0.9 to 2.5) 1.7 (–0.7 to 4.1) 1.5 (–1.0 to 4.0) 1.8 (–1.1 to 4.7) 0.9 (–1.1 to 2.9) 0.7 (–1.5 to 2.9) | |
| Aktas et al. (32) | Rest pain (scored on a VAS). Activity pain (scored on a VAS). Pain disturbing sleep (scored on a VAS). Constant score (ranges from 0 to 100 points with higher scores indicative of better function. Subscales for function (20 points), ROM (40 points), pain (15 points), and strength (25 points)). Shoulder disability questionnaire (pain-related disability questionnaire with 16 items; ranges from 0 to 100 with lower scores indicative for less disability). | 3 weeks 3 weeks 3 weeks 3 weeks 3 weeks | 0 0 0 0 0 | 0.1 (–0.9 to 1.0) –0.1 (–1.5 to 1.4) –1.5 (–3.0 to 0.1) 0.7 (–9.0 to 10.3) –0.5 (–17.9 to 17.0) | |
| Binder et al. (33) | Pain score (sum of pain at night, movement, at rest scored on a VAS). Pain on resisted movements; painful arc score (scored on a 4-point scale). Minor residual or no symptoms. | 2 & 4 weeks 6, 8 & 16 weeks 2 & 4 weeks 6, 8 & 16 weeks 16 months | + 0 + 0 0 | | 1.1 (0.9–1.4) |
| Chard et al. (34) | Pain scores (at night, on movement, at rest, summated score, all scored on a VAS). Pain on resisted movements (ABD, ER and IR, all scored on a 0–3 point scale). Painful arc score (scored on a 0–3 point scale). | | 0 all follow-ups 0 all follow-ups 0 all follow-ups | | |
| ABD: abduction; ADL: activities of daily life; AT: after treatment; 95% CI: 95% confidence interval; ER: external rotation; G: group; IR: internal rotation; ITT: intention to treat; 0: no significant differences between groups as reported by the authors; PRIM: Project on Research and Intervention in Monotonous Work; RR: relative risk; VAS: visual analogue scale; WMD: weighted mean difference; +: significant in favour of the intervention group as reported by the authors. |
Interventions
A variety of interventions and comparisons were found throughout studies. An overview of the inclusion criteria and interventions is shown in Table IV; between-groups results for each study are shown in Table V. The different comparisons made by the authors are described below, results are summarized and the resulting level of evidence is given.
Comparisons of interventions
Physiotherapy vs no-intervention. Dickens et al. (27) compared physiotherapy with no intervention in 85 patients with SIS, all of them already planned for shoulder surgery. Physiotherapy treatment (n = 45) included passive manual joint mobilization, home-based strengthening exercises for the rotator cuff, strapping, advice on posture, and electrotherapy once or twice a week. After 6 months, 11 out of 42 patients refused surgery. In contrast, all patients of the control group (n = 40) underwent surgery as planned. This was a significant difference in favour of the physiotherapy group. Unfortunately, there was no information available at baseline about patient expectations of surgery or physiotherapy. Nevertheless, the authors stated that it could have influenced the outcome in favour of the physiotherapy group.
There is limited evidence (85 patients) that physiotherapy consisting of manual mobilization, strengthening exercises, strapping, advice about posture, and electrotherapy effectively improves functioning at 6 months follow-up and therefore may prevent patients with SIS from (undergoing) shoulder surgery.
Home-based exercises vs no intervention. Ludewig & Borstad (26) investigated the effect of standardized home-based exercises of 10 weeks’ duration, including 6 stretching and strengthening exercises in 76 male construction workers. They found significant improvements in work-related pain and disability, and the shoulder rating questionnaire assessing shoulder specific activities in the exercise group (n = 34) after 10 weeks, compared with a control group (n = 33) receiving no treatment.
There is limited evidence (67 patients) that home-based exercises are an effective treatment for male construct workers with SIS compared with no treatment at 10 weeks follow-up.
Physiotherapy including “centring training for the shoulder” vs home-based exercises including isometric strengthening. Three studies compared physiotherapy with home-based exercises (35, 38, 39). In 2 studies (38, 39) instructions on the prescription for physiotherapy were “centring training” and, if necessary “mobilization”. There were no further instructions or written protocols, and treatment decisions were left to the physiotherapists. In contrast, the standardized exercise protocol included defined exercises aiming at centring the humeral head and included isometric strengthening on a handout. After instruction the patients performed the exercises at home. No difference was found between the physiotherapy groups and the exercise groups. Additionally, the study of Walther et al. (38) also included a control group wearing a functional shoulder brace for 12 weeks. This group also showed no significant differences compared with exercises or physiotherapy. Ginn & Cohen (35) compared the effect of home-based exercises with a single corticosteroid injection into the subacromial space and with a group receiving “multiple physical modalities” (MPM) in shoulder pain patients including a subgroup of patients with SIS (n = 61). The MPM group was taken as the physiotherapy group because of its typical physiotherapeutic content. The exercise group performed an individually planned shoulder programme based on the information of the initial assessment, including strengthening and stretching exercises and exercises to gradually improve functional tasks. The programme was supervised and adapted once a week. MPM was a combination of electrophysical means, passive joint mobilization of the shoulder complex (twice a week), global range of motion (ROM) and strengthening exercises for the upper extremity to increase hand placement. After 5 weeks no difference between the 3 groups could be found. Given the restricted similarity in interventions there is only moderate evidence about the effectiveness.
There is moderate evidence (141 patients) that there is no difference in effects on functioning between a standardized shoulder-specific isometric exercise programme at home and physiotherapy addressing centring of the shoulder in patients with SIS at 5–12 weeks follow-up.
Physiotherapist-led exercises vs physiotherapist-led exercises plus manual therapy. In the studies by Bang & Deyle (36) (n = 52) and Conroy & Hayes (37) (n = 14) the groups receiving physiotherapist-led exercises plus manual therapy showed significantly better results in the short term for pain and functioning than the control groups in both trials that received only physiotherapist-led exercises. The pooled effect size (standardized mean difference (95% CI) for pain after treatment was 0.88 (0.36–1.40). A standardized mean difference was calculated because different measurement scales were used in the trials. The random effects model was chosen because an identical effect for both studies could not be assumed due to variations of the manual therapy protocol and a different frequency of its application. However, the small study populations and the limited simultaneity in timing of the measures do not justify a strong evidence level.
There is moderate evidence (66 patients) that adding manual therapy to a standardized shoulder-specific exercise programme is superior in pain improvement compared with an isolated exercise regimen at 3 and 8 weeks follow-up.
Physiotherapist-led exercises vs surgery. Brox et al. (22, 24) assigned 125 patients with SIS to 3 groups. The first group underwent subacromial decompression followed by physiotherapy, the second group had placebo laser and was used as the control group, and the third group received physiotherapist-led exercises. Using an intention-to-treat analysis, the median Neer score measuring shoulder functioning reached statistical significance in favour of the active treatment groups at 6 months and 2.5 years follow-up. Haahr et al. (23, 25) made the same comparison in a sample of 84 patients, but without the use of a placebo group. They found no differences between groups at any follow-up point, either for the Constant score or for the Project on Research and Intervention in Monotonous Work score assessing shoulder pain and disability.
There is moderate to strong evidence (209 patients) that surgery is not more effective than physiotherapist-led exercises in the treatment of pain and disability in patients with SIS at 6 months, and 1, 2.5, 4 and 8 years follow-up.
Ultrasound vs sham treatment. Nykänen (29) compared ultrasound with sham treatment in 73 patients. Both groups additionally received group gymnastics and massage therapy. After 4 and 8 months the investigators could not find any significant differences in pain and functioning between both groups.
There is limited evidence (73 patients) that ultrasound therapy is not more effective in improving pain and functioning than sham treatment when added to group gymnastics and massage therapy at 4 weeks, 4 or 12 months follow-up.
Ultrasound vs acupuncture. Johansson et al. (28) compared ultrasound therapy with acupuncture. Additionally, both groups performed home-based exercises on a daily basis for 5 weeks. Although both groups improved significantly, no differences could be seen between groups after 3, 6, or 12 months.
There is limited evidence (85 patients) that ultrasound therapy is not more effective than acupuncture in combination with home-based exercises in the treatment of patients with SIS.
Low-level laser therapy vs sham treatment. Both, Saunders (30) and Vecchio et al. (31) compared low-level laser therapy (LLLT) with sham treatment. In the study of Saunders (30) real treatment had a significantly better effect on pain than sham treatment after 3 weeks. In contrast, Vecchio et al. (31) found no differences between the 2 groups after 4 and 8 weeks.
There is conflicting evidence (59 patients) about the effectiveness of LLLT for the treatment of SIS.
Electromagnetic field therapy. Binder et al. (33) compared 8 weeks of electromagnetic field therapy (EMFT) with 4 weeks of sham treatment followed by 4 weeks of real treatment. A significant difference between groups was seen after 4 weeks for pain on resisted movements and the painful arc score in favour of the EMFT group, but not after 6, 8 and 16 weeks. This result could not be confirmed by Aktas et al. (32). They compared EMFT with sham treatment and found no differences between groups for pain and functioning after 3 weeks. Chard et al. (34) compared 8 h of low-dose EMFT with 2 h of high-dose EMFT. No difference could be seen for any outcome measure at any follow-up.
There is conflicting evidence (124 patients) that EMFT is more effective in improving pain and function than sham treatment in the short term, regardless of whether high or low doses of EMFT are applied.
DISCUSSION
This review summarized the effectiveness of physiotherapy in patients with SIS. According to our best-evidence synthesis, moderate evidence was found for an equal effectiveness of physiotherapist-led exercises and surgery in patients with SIS, especially in the long term (22–25). Although the quality score of 7/10 and the number of 209 included patients suggests a stable result, more high-quality trials are necessary to confirm these results. These results suggest that patients should not undergo surgery before having been treated conservatively. In addition, exercise therapy seemed to cause less costs than surgery (24). Surgery should be handled with care, and clear indications for its application need to be established. Moderate evidence was also found for manual therapy combined with exercises compared with exercises alone in patients with SIS (36, 37). In both (small) studies manual treatment combined with physiotherapist-led exercises led to statistically significant improvements in pain levels compared with physiotherapist-led exercises alone. However, only the protocol of Bang & Deyle (36) additionally led to a significant improvement in functional activities. The fact that Bang & Deyle (36) also included the adjacent joints in their manual treatment, regularly rechecked and adapted their interventions, and that all patients received individually designed home exercises to reinforce the effect of manual treatment, may have contributed to this. However, the moderate evidence statement was valid only for pain, but not for functioning. Unfortunately, neither study provided sufficient data to judge the minimal difference between groups in treatment effect and, therefore, the clinical importance of the results cannot be determined exactly. Moreover, both studies had short follow-ups and small sample sizes and despite a quality score of 6/10, some important quality items, such as allocation concealment, blinding of subjects and therapists, and intention-to-treat analysis were not fulfilled. This review further revealed moderate evidence for an equal effectiveness of combined physiotherapy interventions and home-based exercises on pain and functioning (35, 38, 39). Unfortunately, instructions for physiotherapy in 2 studies (38, 39) were quite similar to the protocol of the exercise groups and therefore similar results could be expected. The fact that, in the study of Werner et al. (39), participants were significantly more satisfied with home-based exercises beings into question the quality of the 30 physiotherapy sessions. Even Ginn & Cohen (35) could not reveal any differences between both interventions, perhaps because the study was highly likely to be underpowered (n = 61) to detect any difference. Their treatment for the exercise group was individualized for each patient, and covered exercises to improve strength, flexibility, co-ordination, posture, and motor control. Unfortunately, this exercise programme was withheld from the MPM group, replaced with standardized range of motion exercises, and only manual joint mobilization was individualized. Therefore, the benefit of manual mobilization and electrophysical means in addition to an individualized home-based exercise programme remained unclear. Although Dickens et al. (27) found that combined physiotherapy interventions are significantly more effective than no intervention, this was also true for home-based exercises (26), and thus the application of this more complex intervention must be justified in future studies. Both the combination of the exercises used in the exercise protocols (24–26) and the combination of physiotherapy interventions (27, 35, 38, 39) varied considerably between studies. Reasons for their selection were often not explained and therefore remained unclear. This suggests that no clear criteria exist for determining the content of an exercise protocol or the combination of physiotherapy interventions, which might also have limited the effect. A detailed description of the interventions is shown in Table IV.
The results for a passive treatment were that ultrasound (29) was not more effective than sham application and evidence for the effect of LLLT (30, 31) or EMFT (32, 33) was conflicting. Thus, moderate evidence exists that passive treatment modalities are not more effective than sham application and their use can therefore not be recommended.
Methodological limitations of this review
There are some methodological limitations of this review. Although only those studies were included in which subjects presented typical clinical signs and symptoms for SIS, more than 30 different inclusion criteria and more than 40 different exclusion criteria were used across all studies. This may reflect the need for a valid and practical classification system for patients with shoulder complaints in general. Considerable clinical heterogeneity regarding interventions and outcome measures, and missing or incomplete data often made it impossible to pool study results or to calculate any effect size. Furthermore, only a few studies could be summarized per comparison.
The cut-off point chosen for the definition of a high-quality study (5/10) was based on the impossibility of blinding therapists and participants with most active physiotherapeutic interventions, but remains to some extent subjective. This may have affected the resultant level of evidence statements and, in combination with the average methodological quality of included studies of 6.8/10 (range 5–9), the stability of the review results must be questioned. When applying the CONSORT (Consolidated Standards of Reporting Trials) statement for trials assessing non-pharmacological treatments (40, 41) to the included studies it becomes obvious that the conclusions of this systematic review are limited by missing quality aspects, such as sequence generation, allocation concealment, blinding, intention to treat-analysis, or incomplete outcome data. Together with the small number of studies found for each comparison, small sample sizes (median 56) and short follow-up periods (median 11 weeks), these aspects may have contributed to an overestimation of treatment effects.
Implications for further research
A major concern for further studies is that defined interventions based on a structured decision-making process should be applied to clearly-defined clinical patterns. To do so, a valid and practical classification system for shoulder disorders is needed. The use of similar shoulder-specific outcome measures for pain, activity and participation restrictions is recommended to facilitate future pooling of data. To enable the reader to judge the clinical value of statistically significant study results and to allow a transfer of study results into daily practice, sufficient statistical data for within- and between-group results, and a detailed description of treatment modalities tested should be provided. There is an urgent need for more high-quality randomized controlled trials in this field.
REFERENCES