OBJECTIVE: To identify and compare objective and self-perceived characteristics of patients with chronic obstructive pulmonary disease, who do and do not choose rehabilitation.
SUBJECTS: The study comprised 205 consecutive patients with mild to very severe chronic obstructive pulmonary disease. They chose either inpatient rehabilitation (n = 161) or ordinary outpatient consultations (n = 44).
Measurements: Disease severity was assessed with spirometric tests, health-related quality of life was assessed with the St George’s Respiratory Questionnaire, and mental status was measured using the Hospital Anxiety and Depression Scale. Socio-demographic and social characteristics, and co-morbidity variables were available.
RESULTS: Patients in the rehabilitation group had a lower level of overall health-related quality of life (63.8 vs 47.6, p = 0.000) and a higher prevalence of anxiety (34.6% vs 13.6%, p = 0.007) than the outpatients. The outpatients received more psychological support from spouse/partner than patients in the rehabilitation group (70.5% vs 49.1%, p = 0.012). There were no differences in disease severity and co-morbidity.
CONCLUSION: The decision to choose rehabilitation may be determined by impaired health-related quality of life, psychological distress and lack of psychological support from a significant other. Our findings suggest that patients with chronic obstructive pulmonary disease are conscious of their overall health status and the necessary treatment to maintain or improve it.
Key words: COPD; inpatient rehabilitation; outpatients; self-selection; health-related quality of life; mental status.
J Rehabil Med 2010; 42: 362–367
Correspondence address: Ola Bratås, Faculty of Nursing, Department of Nursing, Sør-Trøndelag University College, Mauritz Hansens gt. 2, NO-7030 Trondheim, Norway. E-mail: ola.bratas@hist.no
Submitted June 29, 2009; accepted November 17, 2009
INTRODUCTION
Chronic obstructive pulmonary disease (COPD) is a leading cause of morbidity and mortality throughout the world. Estimates from the World Health Organization (WHO) show that, in 2001, COPD was the fifth leading cause of death in high-income countries and sixth in nations of low and middle income (1). COPD is expected to rank fifth as cause of death worldwide in 2020 (2).
COPD is characterized by an airflow limitation that is not fully reversible and is associated with an abnormal inflammatory response of the lungs to noxious particles or gases (2). The extent of airflow limitation and emphysema, which is followed by a decline in lung function, varies from person to person. Hence, the severity of COPD is classified into 4 stages (I–IV) by the Global Initiative for Chronic Obstructive Lung Disease (GOLD) Guidelines (2). COPD is also associated with systemic inflammation and skeletal muscle dysfunction that may contribute to limitation of exercise capacity (3).
In addition to breathlessness, patients with COPD may experience symptoms such as pain, fatigue and sleep problems (2, 4). Compared with patients with other chronic diseases, such as epilepsy, angina pectoris, and rheumatoid arthritis, patients with COPD have a worse health-related quality of life (HRQoL) in physical functioning, general health and social functioning (5). It has also been found that patients with COPD experience significantly more psychological distress than the general population (6).
An established and well-documented part of treatment for patients with COPD is the rehabilitation regimen. Pulmonary rehabilitation is administered in inpatient, outpatient or home settings, or a variety of combinations of these. These types of rehabilitation have proven to be effective treatments that enhance physical capacity and HRQoL and reduce psychological distress in patients with COPD (7, 8). Irrespective of administration, a pulmonary rehabilitation programme includes a multidisciplinary assessment that is the basis for development of an integrated treatment plan, patient education, exercise training programme, psychosocial support and follow-up (9). Since patients with COPD constitute 80% of all patients with lung diseases who apply to pulmonary rehabilitation units, one of several strategies in the treatment of COPD is to gear rehabilitation services to COPD patients’ needs (2, 10, 11). Although pulmonary rehabilitation is recommended for all patients with COPD, the GOLD Guidelines emphasize referral to pulmonary rehabilitation at an early stage of the disease to promote earlier use of preventive strategies, e.g. lifestyle adjustment, better psychosocial coping and greater latitude in the exercise prescription (2, 12).
Not all patients with COPD use rehabilitation services. This may be explained by lack of motivation, significant cognitive impairment, inability to attend the programme consistently, unstable medical condition that may pose risk or inadequate financial resources (8). However, little is known about potential clinical, socio-demographical or psychosocial differences between those who use rehabilitation services and those who do not use these services.
Hence, the aim of the study was to identify and compare clinical, socio-demographic and social characteristics, self-perceived mental status and quality of life in patients with COPD who were admitted and those who were not admitted to inpatient rehabilitation.The latter group comprises patients referred to ordinary outpatient consultations (outpatients). Knowledge of possible differences between the 2 groups may be useful to further understand incentives for choosing rehabilitation, which in turn could help clinicians at outpatient clinics motivate and encourage their patients with COPD to participate in rehabilitation programmes. In addition, this knowledge may be useful for rehabilitation centres to improve rehabilitation services where necessary.
METHODS
Participants
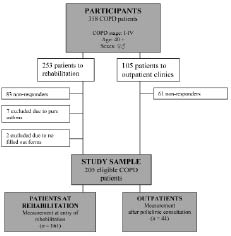
The potential participants in this study comprised 358 male and female patients with COPD who were aged over 40 years with COPD stages I–IV and with no exacerbations. Prior to this study, they had all been encouraged to participate in a rehabilitation programme by their physician. Of their own accord, they selected inpatient rehabilitation (n = 253) or ordinary outpatient consultations (n = 105), as shown in Fig. 1. Participants in the rehabilitation group were recruited from 3 rehabilitation centres in mid and eastern Norway, comprising consecutive cases of COPD patients attending a 4-week inpatient rehabilitation programme during the period March 2007 to December 2007. Participants in the outpatient group were recruited by 3 pneumologists at 2 hospitals and 1 private practice centre in mid-Norway comprising consecutive cases of outpatients with COPD during the period April 2007 to April 2008. In order to reset the effect of former rehabilitation, the outpatient group participants should neither have attended any rehabilitation programme during the last 6 months nor should they have any plans for doing so the following 6 months. As shown in Fig. 1, 144 of the 358 available patients did not respond. Hence, the response-rate was 67% in the rehabilitation group and 42% in the outpatient group. No significant differences were found between responders and non-responders regarding age, gender or disease severity. Since 9 patients in the rehabilitation group were excluded because they had pure asthma and had not completed the forms, the final number of patients in the rehabilitation and outpatient groups was 161 and 44, respectively.
Fig. 1. Study profile with flow of participants, showing available patients, non-responders, excluded patients, and number of eligible patients self-selected to inpatient rehabilitation and outpatient clinics. CODP: chronic obstructive pulmonary disease.
The final study sample comprised 205 eligible patients with COPD. Their mean age was 65.5 years, 53.6% were men, and 85.5% had completed secondary school or less. Approximately one-third of the sample was either diagnosed with moderate, severe or very severe COPD (Table I).
| Table I. Socio-demographic characteristics and chronic obstructive pulmonary disease (COPD) prevalence of the study sample (n = 205) |
| Characteristics | |
| Age, years, mean (SD) | 65.5 (9.3) |
| Males/females, n | 110/95 |
| Education level, n (%) | |
| Primary school | 91 (44.0) |
| Secondary school | 85 (41.5) |
| University/college | 27 (13.2) |
| GOLD COPD stages, n (%) | |
| I (Mild) | 11 (5.4) |
| II (Moderate) | 73 (35.6) |
| III (Severe) | 59 (28.8) |
| IV (Very severe) | 62 (30.2) |
| GOLD: Global Initiative for Chronic Obstructive Lung Diseases; FEV1: forced expiratory volume in 1 s; COPD I: FEV1 ≥ 80%; COPD II: 50% ≤ FEV1 < 80%; COPD III: 30% ≤ FEV1 < 50%; COPD IV: FEV1 < 30%; SD: standard deviation. |
Data collection and procedure
Potential participants in the rehabilitation group were given oral and written information about the study a few days after attending the rehabilitation centre. Parallel data collections were carried out between the 3 rehabilitation centres, which were only interrupted by the summer holiday. The patients who wanted to participate in the study returned the questionnaires and the signed written consent form in a postage-paid envelope to the researcher. The potential participants in the outpatient group were informed orally about the study by the pneumologists during ordinary outpatient consultation. The information they were to give the patients was based on a written and oral presentation from the principal researcher to all 3 pneumologists. The patients who wanted to participate were also given written information about the study when they received the questionnaires. The study was approved by the Regional Committee for Medical Research Ethics, Health Region IV, Norway and the Ombudsman for privacy in research, supervised by the Norwegian Social Science Data Services.
Classification of severity and stages of COPD
Lung function, expressed by post-bronchodilator forced expiratory volume in 1 s (FEV1), was assessed by spirometric tests carried out by trained personnel. Classification of severity and COPD stages were carried out according to GOLD Guidelines (2).
Assessment of anxiety and depression
The Hospital Anxiety and Depression Scale (HADS) was used to assess the presence of anxiety and depressive symptoms. The HADS was constructed by Zigmond & Snaith in 1983 (13) as a quick way to separately measure depression and generalized anxiety in patients in non-psychiatric hospital clinics. The questionnaire was designed to be used in both inpatient and outpatient settings, and is easily self-administrated in approximately 5–10 min (14). Anxiety (HADS-A) and depression (HADS-D) are assessed as separate components, each with 7 items, rated on a 4-point scale: 0 (not present) to 3 (significant symptoms). This 4-point score has a range of 0–21 for anxiety and 0–21 for depression (14). Higher scores indicate more severe symptomatology. Various cut-offs have been used, although Zigmond & Snaith (13) recommend a cut-off score of ≥ 8 for both scales to include all possible case. Various studies have shown that HADS has a high degree of validity and reliability (15), which is also true for the Norwegian version (16).
Assessment of health-related quality of life
The St George’s Respiratory Questionnaire (SGRQ) is a disease-specific instrument designed for measuring HRQoL in patients with chronic lung disease by assessing symptoms, physical functioning and psychosocial impacts of COPD (17, 18). The SGRQ is widely used and has been translated into at least 70 languages, including Norwegian (19). The questionnaire is divided into 3 sections: a symptom score concerned with the frequency and severity of respiratory symptoms, an activity score concerned with activities that are limited by breathlessness, and an impact score with a range of aspects on social functioning and psychosocial disturbances resulting from airway disease (18, 20). The score ranges from 0 to 100 for each domain, with higher values reflecting decreasing HRQoL. The scores for the 3 components can also be added together to give a composite total score. Different studies have shown high degree of validity and reliability for the original version and the Norwegian version (20, 21).
Socio-demography, social characteristics and co-morbidity
Variables on socio-demographic and social characteristics and co-morbidity were accessible. Co-morbidity was measured as organ-specific diseases in the past 12 months, with “yes/no” response categorized in no co-morbidity, 1–4 and 5–8 additional diseases. Social characteristics were measured as psychological support from spouse/partner, children or siblings and frequency of social participation with an organization or a club and were categorized as “never”, “a few times a year” and “once a month or more”.
Statistical analyses
Analyses were carried out using SPSS version 16.0 for Windows. Baseline characteristics data with normal distribution are presented as means with standard deviation (SD) and those not normally distributed as medians. For comparison between responders and non-responders, a 2-sided t-test for independent samples and a Pearson χ2 test was used. A comparison between the rehabilitation group and the outpatient group was undertaken by the use of a 2-sided t-test for independent samples, a non-parametric Mann-Whitney U test and a Pearson χ2 test. Spearman bivariate correlation was used to investigate associations between variables. A p-value < 0.05 was considered statistically significant.
Scoring procedure, calculation methods, item weights and handling missed items were treated according to recommendations by the authors of the HADS (13) and the SGRQ (18, 22). The SGRQ scoring manual programme adjusted for up to 24% of missing items in the questionnaire (≤ 11 items), with a maximum number of missing items of 1, 4 and 6 for the components symptoms, activity and impact, respectively. Missing items beyond that were treated as missing and not included in the different SGRQ sub-scores. In this study, 189 of 205 responders (92.2%) had a complete SGRQ.
RESULTS
A total of 161 patients chose inpatient rehabilitation and 44 chose outpatient clinics. Men and women were nearly equally represented in the rehabilitation group (49% men vs 51% women), while the majority of patients in the outpatient group were men (70.5% men vs 29.5% women). This observed gender difference between the total groups was significant (p = 0.012). More patients in the outpatient group were married/had a partner (81.8%) compared with the rehabilitation group (63.4%) (p = 0.021), while more patients in the rehabilitation group were divorced/separated (21.7%) than in the outpatient group (6.8%) (p = 0.024). The outpatients received more psychological support from spouse/partner than patients in the rehabilitation group (70.5% vs 49.1%, p = 0.012). A majority of the rehabilitation patients (58.9%) had previously participated in another rehabilitation programme, while more than 6 months previous to the study 22.7% of the outpatients had done so (p = 0.000). The outpatients more often participated in an organization or a club once a month or more than did the patients in the rehabilitation group (47.7% vs 32.3%), but this result failed to reach statistical significance. The difference in mean age between the groups (65.0 in the rehabilitation group and 67.2 in the outpatient group) was not statistically significant, neither the observed differences in education on primary school (46.5% vs.38.6%), secondary school (40.3% vs 47.7%) and university/college (13.2% vs 13.6%) (Table II).
| Table II. Socio-demographic and social characteristics in patients with chronic obstructive pulmonary disease self-selected to inpatient rehabilitation and outpatient clinics |
| | Rehabilitation patients n = 161 | Outpatients n = 44 | p-value |
| Age, years, mean (SD) | 65.0 (9.1) | 67.2 (10.2) | 0.166 |
| Males/females, n | 79/82 | 31/13 | 0.012 , χ2 = 6.4 |
| Marital status, % |
| Always been single | 3.7 | 4.5 | 0.804 |
| Married/live-in | 63.4 | 81.8 | 0.021 |
| Divorced/separated | 21.7 | 6.8 | 0.024 |
| Widow/widower | 11.2 | 6.8 | 0.399 |
| Education, % |
| Primary school | 46.5 | 38.6 | 0.352 |
| Secondary school | 40.3 | 47.7 | 0.375 |
| University/college | 13.2 | 3.6 | 0.941 |
| Psychological support, % |
| From spouse/live-in | 49.1 | 70.5 | 0.012 |
| From children | 25.5 | 11.4 | 0.047 |
| From siblings | 6.2 | 6.8 | 0.884 |
| Participation in an organization or a club, % |
| Never or few times a year | 67.7 | 52.3 | 0.059 |
| Once a month or more | 32.3 | 47.7 | 0.059 |
| Former participation in rehabilitation, % |
| Yes | 58.9 | 22.7 | 0.000, χ2 = 8.0 |
| No | 41.1 | 77.3 | |
There was no significant differences between the groups in mean COPD stages, but more patients in the rehabilitation group were diagnosed with very severe COPD (34.2% vs 15.9%, p = 0.020), whereas more outpatients were diagnosed with severe COPD (40.9% vs 25.5%, p = 0.045). The prevalence of co-morbidity was equally distributed in the groups (Table III).
| Table III. Mean and prevalence of chronic obstructive pulmonary disease (COPD) stages, and co-morbidity in patients self-selected to inpatient rehabilitation and outpatient clinics |
| | Rehabilitation patients n = 161 | Outpatients n = 44 | p-value |
| Mean COPD stages I–IV (SD) | 2.88 (0.96) | 2.70 (0.77) | 0.276* |
| Prevalence of GOLD COPD stages, % |
| I (Mild) | 6.2 | 2.3 | 0.305# |
| II (Moderate) | 34.2 | 40.9 | 0.409 |
| III (Severe) | 25.5 | 40.9 | 0.045 |
| IV (Very severe) | 34.2 | 15.9 | 0.020 |
| Prevalence in co-morbidity, % |
| No additional diseases | 7.5 | 13.6 | 0.200# |
| 1–4 additional diseases | 77.6 | 77.3 | 0.959 |
| 5–8 additional diseases | 14.9 | 9.1 | 0.321 |
| GOLD and COPD stages, see Table I. *2-sided t-test for independent samples; #Mann-Whitney U test. |
Since the prevalence of severe and very severe COPD differed between the groups and might be associated with HRQoL, we checked the association through correlation analyses between the SGRQ subscales and COPD stages (FEV1). The correlations in the rehabilitation group ranged from 21.4% (p = 0.008) to 24.7% (p = 0.002) and in the outpatient group it ranged from 30.6% (p = 0.046) to 34.1% (p = 0.025), indicating a significant week association between disease severity and HRQoL in both groups.
Patients in the rehabilitation group scored significantly higher on median SGRQ activity score, impact score and total score (73.3 vs 55, p = 0.000; 50.4 vs 34, p = 0.000; 64 vs 48, p = 0.000, respectively), while there was no difference on SGRQ symptom score. The median anxiety and depression scores on HADS were higher in the rehabilitation group than in the outpatient group, with a score of 6 vs 3.5 on anxiety (p = 0.006) and 5 vs 4 on depression (p = 0.031), respectively. Finally, the prevalence of possible HADS anxiety cases was higher in the rehabilitation group (34.6% vs 13.6%, p = 0.007), while no difference was found in possible HADS depression cases between the groups (Table IV).
| Table IV. Median scores of the SGRQ and the HADS, and prevalence of anxiety and depression in patients with chronic obstructive pulmonary disease self-selected to inpatient rehabilitation and outpatient clinics |
| | Rehabilitation patients | Outpatients | p-value |
| Total | Median | IQR | Total | Median | IQR |
| SGRQ scores |
| Symptoms | 160 | 67.5 | (51.0–84.1) | 44 | 60.2 | (44.4–77.0) | 0.122 |
| Activity | 150 | 73.3 | (59.8–86.7) | 42 | 55.0 | (41.4–67.4) | 0.000 |
| Impacts | 151 | 50.4 | (34.8–60.6) | 43 | 34.0 | (22.0–46.9) | 0.000 |
| Total score | 148 | 63.8 | (47.9–72.4) | 43 | 47.6 | (31.9–61.8) | 0.000 |
| HADS scores | | | | | | | |
| Anxiety | 159 | 6.0 | (3.0–9.0) | 44 | 3.5 | (1.0–7.0) | 0.006 |
| Depression | | 5.0 | (2.0–8.0) | | 4.0 | (2.0–6.75) | 0.031 |
| Prevalence of anxiety and depression, % |
| HADS anxiety | 159 | | | 44 | | | |
| Normal cases | 65.4 | | | 86.4 | | | 0.007 |
| Possible cases | 34.6 | | | 13.6 | | | |
| HADS depression | 159 | | | 44 | | | |
| Normal cases | 69.1 | | | 84.0 | | | 0.051 |
| Possible cases | 30.8 | | | 16.0 | | | |
| SGRQ: St George’s Respiratory Questionnaire; HADS: Hospital Anxiety and Depression Scale; normal cases = HADS cut-off < 8; possible cases = HADS cut-off ≥ 8; IQR: interquartile range. |
DISCUSSION
In the study sample, 59% had a FEV1 < 50% of the predicted value, and thus have severe or very severe airway obstruction. This is not in accordance with the COPD population in Norway, as approximately 10% are expected to have severe or very severe COPD (23). On the other hand, the level of disease severity in the present study reflects patients with COPD at rehabilitation centres and in outpatient clinics, i.e. they are mainly treating a selected group of patients with severe or very severe COPD. The mean age of the responders (65.5 years) is in accordance with the COPD population, as the largest prevalence of COPD in Norway is among people aged between 60 and 74 years (23). The gender distribution in the study sample, 110 males vs 95 females, may reflect that the prevalence of the disease is now almost equal in men and women in developed countries, probably reflecting the changing patterns of tobacco smoking (2). Regarding education, 85.5% of the responders had a primary and secondary school education, while 13.2% had a university or college education, which is in accordance with the education level for people aged between 60 and 66 years in the general population in Norway (24). Hence, except for disease severity, the external validity of the data in the study sample can be regarded as satisfactory.
Marital status may influence the self-selection of patients with COPD to inpatient rehabilitation or outpatient clinics, as more outpatients are married or have partners who live with them than do patients in the rehabilitation group. Thus, fewer patients in the rehabilitation group receive psychological support from a spouse or partner compared with those in the outpatient group. The essential care, support and encouragement that a life partner gives may be crucial to a patient with COPD; it can also lead to improved compliance with therapies and better disease self-management for the patient (25). Hence, our finding suggests that lack of psychological support from a significant other may play a role in the patient believing that inpatient rehabilitation is in his or her best interest.
More patients in the rehabilitation group have very severe COPD compared with the outpatients. Very severe COPD may imply serious breathlessness with extensive limitations both in physical and social activities. Thus, our finding suggests that the most sick and disabled patients may have a particular need for inpatient rehabilitation, as is also reported in the literature (26). On the other hand, our results show that disease may not be the only deciding factor in self-selection to inpatient rehabilitation or outpatient clinics, because no differences were found in mean COPD stage or in the prevalence of co-morbidity between the groups. Hence, the incentive behind choosing rehabilitation may be influenced by other factors beyond disease severity and co-morbidity, e.g. psychological distress, impaired quality of life and lack of psychosocial support. These factors are considered important to incorporate in a pulmonary rehabilitation programme (9, 11).
The differences between the groups in SGRQ activity, impacts and total score indicate an impaired HRQoL among patients in the rehabilitation group compared with the outpatients. An impaired HRQoL in patients with COPD may be associated with disease severity (27), as in the rehabilitation group with a higher prevalence of very severe COPD compared with the outpatient group. However, our analyses show only a weak correlation between disease severity and the SGRQ subscales, which corresponds to other studies that found a relatively weak association between HRQoL and disease severity (FEV1) in patients with COPD (28, 29). Other factors, such as dyspnoea-related limitations, depression and exercise tolerance, have shown to be more strongly related to HRQoL, measured by the SGRQ, than disease severity (30). Irrespective of that, the patient’s perception of a low HRQoL may make him or her feel that a rehabilitation programme is necessary.
The differences between the groups on HADS anxiety and depression scores and in the prevalence of possible HADS anxiety cases indicate a higher level of psychological distress in the rehabilitation group than in the outpatient group. Possible HADS anxiety cases were recorded in 34.6% of the patients in the rehabilitation group, which is in line with Troosters et al. (31), who found that 20–40% of patients with COPD referred to rehabilitation were anxious.
Psychological characteristics interact with physical symptoms and play an important role in how people with COPD experience and manage their disease, often more than their physical problems, which can be objectively measured (32). Hence, our results suggest that it is the patients with high levels of anxiety and depression who may be interested in a rehabilitation programme.
Our findings show that the outpatients had better psychological health, HRQoL and social conditions than the patients with COPD who had been admitted to rehabilitation. As these differences could be related to previous participation in rehabilitation, it is noteworthy that a total of 77.3% of the outpatients reported no previous participation, compared with 41.1% of the patients admitted to rehabilitation. Hence, it may be considered an unnecessary medicalization from a clinician’s position to try to motivate this group of patients for rehabilitation. However, the nature of the disease is progressive, which makes pulmonary rehabilitation suitable and perhaps necessary for all patients with COPD in order to prevent further deterioration of the disease.
This study has some limitations. There are significant differences in gender between the groups that are caused by the small number of women in the outpatient group. Since female patients with COPD tend to report a lower HRQoL and a higher level of anxiety and depression than males (33, 34), we checked whether this gender bias may have contributed to the differences between the groups. In the study sample, females scored significantly higher on anxiety than males, while no differences were obtained regarding depression and the SGRQ scores (data not shown). Hence, the difference in the prevalence of anxiety between the groups may be caused by gender bias. Furthermore, one must keep in mind that this is a relatively small study with a sample size of 44 responders in the outpatient group. A larger sample would have been more representative of the COPD population, and thus have more generalizability. Furthermore, the selection of patients in the present study is not random with, subsequently, a non-probability study sample. A response-rate of 42% in the outpatient group is not optimal; however, no differences were found between responders and non-responders in terms of disease severity, age and gender. Finally, it is questionable whether 6 months is an adequate time limit in order to discount the effects of former rehabilitation in the outpatient group. Since the effects of rehabilitation usually last longer, a comparison of HRQoL, anxiety and depression between former participants in rehabilitation (22.7%) and remaining patients in the outpatient group was performed. Contrary to what was expected, the former participants scored significantly higher on all the SGRQ subscales, while no differences were seen on anxiety and depression (data not shown). Hence, no effects of former rehabilitation seem to be present among these particular patients in the outpatient group.
In conclusion, choosing rehabilitation may be determined by impaired HRQoL, psychological distress, being divorced or separated and lack of psychological support from a significant other, rather than disease severity alone. Patients with COPD who choose not to participate in a rehabilitation programme have better psychological health, HRQoL and social conditions compared with those who are admitted to rehabilitation. Thus, our findings suggest that patients with COPD are conscious about their overall health status and needs for treatment to maintain or improve it. Our findings also underpin the need for an overall inpatient rehabilitation model in which the physical as well as the psychosocial needs of the patient with COPD are met.
Conflict of interest: The authors declare no conflict of interest.
REFERENCES