Gunilla Stenberg, MSc, RPT, Anncristine Fjellman-Wiklund, PhD, RPT and Christina Ahlgren, PhD, RPT
From the Department of Community Medicine and Rehabilitation, Physiotherapy, Umeå University, Umeå, Sweden
Gunilla Stenberg, MSc, RPT, Anncristine Fjellman-Wiklund, PhD, RPT and Christina Ahlgren, PhD, RPT
From the Department of Community Medicine and Rehabilitation, Physiotherapy, Umeå University, Umeå, Sweden
OBJECTIVE: The aim of this study was to explore, from a gender perspective, patients’ expectations prior to seeking healthcare for neck or back pain, and their subsequent experiences of the care and rehabilitation they received.
METHODS: Thematized interviews with 12 patients, 7 women and 5 men, using open-ended questions, were analysed according to grounded theory. Each patient was interviewed before their first appointment with a physiotherapist or general practitioner and 3 months later.
RESULTS: Analysis resulted in 5 categories: “To be taken seriously”, “Getting an explanation”, “To be invited to participate”, “To be assessed and treated individually”, and “To be taken care of in a trustworthy environment”, which were linked by a core category “Getting confirmation”. Two ideal types were identified: the “Confident” type, characterized by self-confidence and pride, and the “Ambiguous” type, characterized by disparagement and shame. The categories were partly perceived in different ways from the two ideal types. The ideal types were not defined by sex; however, more men were found to be of the “Confident” type and more women of the “Ambiguous” type.
CONCLUSION: Gender appears to affect expectations and experiences, in addition to how patients view and express their problems. Healthcare professionals should take this into account in consultations.
Key words: gender; back pain; neck pain; primary healthcare; qualitative research.
J Rehabil Med 2012; 00: 00–00
Guarantor’s address: Gunilla Stenberg, Department of Community Medicine and Rehabilitation, Physiotherapy, Umeå University, SE-90187 Umeå, Sweden. E-mail: gunilla.stenberg@physiother.umu.se
Submitted January 31, 2011; accepted September 22, 2011
Introduction
Differences in healthcare-seeking among women and men with chronic pain are culture-dependent, according to a recent review by Cornally & McCarthy (1). They state that perceptions about how to behave as a man or a woman guide the seeking behaviour (1). Connell (2) define gender as the social and cultural aspects attributed to a person’s sex: how men and women are expected to act according to social norms and ideals. Gender is a constantly ongoing process in which we define ourselves as women and men in social meetings and through gendered practices (2). In accordance with this, stereotypical gender norms, that men are strong and independent and women weaker and need to be taken care of, could influence their seeking behaviour, such that seeking care seems to be more natural for women and that men avoid seeking healthcare even when they ought to. In Sweden, there is a higher proportion of healthcare-seeking among women with neck and shoulder pain than among men (3), and the costs for medical care for chronic low back pain are higher for women than men (4).
Some differences are also found in women’s and men’s experiences of healthcare received. Women with various diagnoses reported more experiences of negative treatment, such as being treated with indifference or disrespect (5). Healthcare professionals did not take time, did not listen, and did not believe or doubted the female patients’ complaints (5). Negative experiences could be due to different expectations of the encounter between women and men. The importance of expectation in healthcare as a predictor of satisfaction is unclear (6). Studies of gender differences in patient expectations are rare. No difference between women and men was found when a random sample of adults on the street was asked hypothetical questions about back pain and their expectations of healthcare (7). In a Dutch study of gender differences in relation to pre-treatment expectations of rehabilitation outcome, men and women responded similarly for 21 out of 25 items asked (8). The differences showed that women more than men expected that rehabilitation would result in fewer problems with housework and that they would more easily be able to accept that they could no longer do things they did earlier. Men, on the other hand, expected that they would enhance their ability to cope with being a spouse and that the cause of their pain would be found (8). In a review the most frequently reported expectations found among patients seeking healthcare for back pain were to be given an explanation for their disorder and a diagnosis (9). However, studies of patients with different symptoms show that many patients do not have their expectations met (10).
The medical history given by the patient is the most important factor for diagnosis (11), and becomes even more important when objective tests are lacking. In such consultations, factors other than the purely medical ones may influence the diagnosis. Different patterns have been found in women’s and men’s communication during consultations; women more often ask for, and hope for, help, while men request medical tests, such as X-rays (12).
Both the patient’s expression of expectations and description of symptoms, and the doctor’s interpretation of the same are coloured by gender norms. Malterud (13) states that both patients seeking healthcare and healthcare professionals bring gendered norms and values that affect encounters and medical diagnostics. In gender theory, according to Connell (2), most societies hold the man as the norm, and factors associated with manliness are more highly valued. Doctors respond positively to patients with distinct expectations by granting them what they request (14). Whether this is especially true for male patients was not studied. When interns in a Swedish study were asked to propose treatment for a patient with neck pain, laboratory tests were more often suggested when the patient was presented as a man; when the same patient was presented as a woman, the most frequent suggestions were referral to a physiotherapist or orthopaedic surgeon, and prescription of drugs (15). Non-specific diagnoses are more often assigned to women than to men (12, 15). According to Malterud (13) this could be because medical theory and practice have been constructed by men, using the male viewpoint and language, and that women’s signs of ill health are not fully understood by the medical experts (15).
The aim of this study was to increase our knowledge of the impact of gender in healthcare encounters by exploring patient expectations prior to seeking healthcare for neck or back pain and subsequent experiences of care and rehabilitation received from a gender perspective.
Methods
We chose grounded theory (16) with an emergent design, which is a qualitative method, in order to capture patient perceptions.
Settings
The study was conducted in a primary healthcare setting. In the county of residence of the patients in this study, the County Council guidelines recommend contacting a physiotherapist as the first step for neck or back pain. A physiotherapy appointment in Sweden does not require a referral. When this is not possible, for example when no physiotherapists are available at the healthcare centre, or when the patients are in need of medication or sick leave, the recommendations are that patients make an appointment with a doctor. One of the healthcare centres that participated in this study did not have a physiotherapist, but could recommend physiotherapists at other healthcare centres.
Sample
Thematic interviews were conducted with 12 patients, 7 women and 5 men, aged 20–65 years, when they sought care for neck or back pain. Each patient was interviewed twice: before the first appointment with a new healthcare provider (either a physiotherapist or a general practitioner in 1 of 9 different public healthcare clinics), and 3 months later. The period of 3 months was chosen in order to capture the rehabilitation activities. Patients were informed about the study and asked to participate by a receptionist nurse or physiotherapist at the time the appointment was given. Patients were assured that participation was not necessary to obtain treatment. The patients were chosen purposively, and sequentially, as the data interpretation proceeded. In order to evaluate whether a pattern existed among different groups, the sample was chosen to give maximum variation according to the following criteria: men and women, neck or back disorders, variation in age, marital status, education, and sex of the healthcare professional. Patients should be of working age between 18 and 65 years, and should not have been on sick leave due to neck or back pain in the past year. The patients came from rural and urban regions of Västerbotten County in northern Sweden. Additional background data is provided in Table I. Five of the patients had not previously sought care for neck or back pain in primary healthcare, and the remainder were returning for a new episode of healthcare because of recurrent pain.
| Table I. Background data for the participating patients | ||||||
| Patient number | Duration of current pain | Sex/age, years | Occupation | Married or cohabiting (children at home, n) | Seeking primary healthcare for the first time for neck and back pain | Complaint |
| 1 | 42 months | F/53 | Assistant nurse | Y (0) | N | NP |
| 2 | 6 months | F/53 | Retirement home director | Y (2) | Y | BP |
| 3 | 2 weeks | F/20 | Industrial worker | Y | Y | BP |
| 4 | < 1 week | F/48 | Assistant nurse | Y (2) | N | BP |
| 5 | 1 month | F/29 | Student | Y (1) | Y | BP |
| 6 | 1 month | M/33 | Lorry driver | N | N | BP |
| 7 | 2.5 weeks | M/22 | Youth officer | N | Y | BP |
| 8 | 2 weeks | F/42 | Web designer | Y (2) | Y | NP |
| 9 | 3 months | M/36 | Student | N | N | NP |
| 10 | > 12 months | F/36 | Nurse | Y (2) | N | BP |
| 11 | 1 week | M/65 | Assistant nurse | Y | N | BP |
| 12 | 36 months | M/36 | Industrial worker | Y (3) | N | NP |
| F: female; M: male; Y: yes; N: no.; NP: neck pain; BP: back pain. | ||||||
Data collection
Separate interview guides for the first and follow-up interview were constructed by the research group based on findings from previous research and their own experience. The first interview covered patient experiences of neck or back pain: consequences, support from others, patient understanding of the cause, strategies for managing pain, feelings and expectations about the forthcoming appointment, and earlier healthcare experiences. The second interview examined encounter experiences during the previous 3 months (since the first interview). The questions covered areas such as the extent to which expectations were met, special strategies to obtain preferred examinations or treatments (for example, asking for X-rays), understanding of the cause of the pain, strategies to manage pain, types of treatment, and perception of the general practitioner or physiotherapist. Open-ended questions were asked, and the interview guides were used only to ensure that the information collected covered the research questions. The interviews were carried out in the patient’s home, his or her workplace, one of the healthcare centres, or at the university, in accordance with the patient’s wishes. The first author (GS) performed all of the interviews. Notes were taken during the interview. Each interview lasted between 20 and 90 min. All interviews were audiotaped and transcribed verbatim by the first author, except one that was summarized by hand during the interview due to a technical failure. Two participants, a man and a woman, were not interviewed a second time. One was not interviewed due to the patient’s time constraints and one because of recovery before the physiotherapist appointment.
The first author previously worked as a physiotherapist in primary healthcare, and she therefore tried to put aside her prior knowledge and try to be as open-minded as possible during the interviews. This intention was supported by the interview guide and the fact that patients did not know the profession of the interviewer. Since two interviews were conducted with each patient, questions that emerged during analysis of the first interview could be asked in the second. A summary was made at the end of each interview, and this gave patients the opportunity to correct misunderstandings.
Data analysis
The analysis was carried out in 3 steps: coding and categorizing of the interviews, construction of ideal types, and comparison of the ideal type experiences after 3 months, including a model describing the ideal type’s experience of healthcare and rehabilitation. The analysis was carried out in accordance with the grounded theory method of constant comparison (16). A preliminary analysis of the interview and the memo-taking was made after each interview. For initial open coding we used a software package (OpenCode 3.4© 2007, UMDAC and Division of Epidemiology and Public Health Sciences, Department of Public Health and Clinical Medicine at Umeå University, Sweden). The open codes were merged into categories to find emerging themes and a core category. Axial coding was performed to find relations between the categories. If new questions were suggested by the analysis, they were asked in the next interview. No substantial new information could be added to the categories after 12 interviews and we considered theoretical saturation (16) reached.
To further explain and clarify, the material was described from two dimensions found in the emerged categories; these were labelled “ideal types”. An ideal type is a theoretical construct presenting the essential features, and is not meant to represent “real” people; rather it is a way to make phenomena understandable (17).
In the present study, the ideal types represent dimensions of having back or neck pain; the patients could not be included in only one ideal type, but were found to move between ideal types between the first and second interview. In the third step, a model was developed that described the ideal type experience of healthcare and rehabilitation.
To assure credibility in the analysis, open coding was performed independently by the 3 authors and then discussed in order to establish codes as a negotiated outcome. The authors took precautions to ground our interpretations in the data by making constant comparisons throughout the analysis, going back to the interviews, looking for negative examples, and challenging our interpretations. Further crystallization was used through the process of the analyses (18). Crystallization is a qualitative technique in which a phenomenon is studied from different angles. The results of this study were presented to 3 different research groups; one with gender competence, one with methodology competence, and one with physiotherapy competence. Thus, different perspectives were raised and discussed in order to provide a deeper and more complex understanding of the topic.
This study was approved by the ethics committee of the Medical Faculty of Umeå University (Dnr 07-149M).
Results
Desire for confirmation permeated the entire interview material and “Getting confirmation” emerged as the core category. The categories are all elements of the core category. The analysis resulted in 5 categories, representing factors important for both expectations and experiences. The categories were: “To be taken seriously”, “Getting an explanation”, “To be invited to participate”, “To be assessed and treated individually”, and “To be taken care of in a trustworthy environment” (Table II).
| Table II. Categories, subcategories and examples of open codes for the core category: Getting confirmation | ||
| Categories | Subcategories | Open codes |
| Being taken seriously | Trusts in own ability | Takes things into one’s own hands |
| Be taken seriously | Not be put on a waiting list | |
| Feels brushed aside | ||
| Wants doctor’s understanding | ||
| Worries about being regarded as a “complaining old woman” | Afraid of not being believed | |
| Feels judged in advance | ||
| Wants to convince | Tries to convince others about seriousness | |
| Ready to work for own health | ||
| Getting an explanation | Getting an explanation | Seeks an expert |
| Needs a diagnosis in order to take steps | ||
| Confused by contradictory messages | ||
| Own theories | Looks for connections | |
| Blames work | Blames work | |
| Thinks about the cause | Doubts the cause | |
| Is clear about the cause | ||
| Being invited to participate | Participation | Participation in diagnosis and treatment |
| Expects passive help | Wants treatment | |
| Wants to be helped to help oneself | Wishes to be helped to help oneself | |
| Wants to take own responsibility | ||
| Wants instructions for exercise routine | ||
| Being assessed and treated as an individual | Treated as an individual | Important to get undivided attention |
| Being taken care of in a trustworthy environment | Wants to be taken care of | Continuity is important |
| Wants follow-up | ||
| Totality | Multidisciplinary staff | |
| Assurance | Received reassuring answer | |
| Was not told what would happen next | ||
Expectations were related to upcoming appointments with a general practitioner (2 patients) and a physiotherapist (10 patients). However, when the patients talked about their experiences of healthcare and rehabilitation, they also included experiences from other healthcare visits.
Ideal types: the “Confident” and the “Ambiguous”
In the second step of the analysis, two ideal types, the “Confident” and the “Ambiguous”, were identified from the material (Table III). The ideal types are first described in general and then all categories are described as seen by the ideal types. The ideal types described both similar and typical specific expectations and experiences
The “Confident” ideal type regarded pain as a confirmation of being strong or hard-working. The pain was associated with physically demanding work, often at traditionally male workplaces. They did not doubt that they were entitled to be helped, and took help from healthcare for granted. The “Ambiguous” ideal type expressed complex feelings about pain. They sought help for problems they had experienced for a long time but could no longer control. In the interview, they tried to convince the interviewer that their condition was serious. At the same time, they belittled themselves, felt ashamed and expressed the attitude that others might have had a greater need of healthcare; they did not want to be a burden. They doubted the value of their pain in the eyes of others.
“You get used to being in pain. How much pain am I actually in? How painful is it? How would someone else have reacted? How much is this pain worth?” Woman, 36 years old.
The “Ambiguous” type felt forced into an identity that they wanted to distance themselves from. They felt that the identity was degrading and associated with inactivity, laziness and weakness. This led them to emphasize strongly that their pain was “genuine” in contrast to elderly people or other back pain sufferers who might be feigners.
Willingness to discuss the pain varied. The “Confident” type did not conceal their neck or back problem from others; rather, they simply told people about it but did not complain. The “Ambiguous” type, however, were reluctant to tell others about their pain for fear of being viewed as whiners. They did not want others to feel sorry for them. The ideal types were not totally defined by sex; however, the “Confident” type included more men, whereas more women were the “Ambiguous” type.
To be taken seriously. The “Confident” type trusted their own abilities to get what they wanted from healthcare. As a man explained when answering a question about whether he was afraid of not being taken seriously:
“Oh no, not me. I’m not afraid of it either [with emphasis]. My God, I can speak for myself, you know. You only have to kick up a fuss in that case.” Man, 65 years old.
The “Ambiguous” type were afraid of not being taken seriously when seeking healthcare. This made them hesitant to seek help and some of them had been waiting for months, hoping for things to get better on their own. They feared being regarded as a “complaining old woman”.
On the question of whether things would have been different when seeking healthcare if she had been a man instead, a woman said:
“Yes maybe. I can tell you when I think of going to the doctor, for example, I hesitate because I don’t want to be one of those whining old women, even if I am quite young. But many women of my age have problems.” Woman, 36 years old.
Because of the fear of not being taken seriously, the “Ambiguous” type were eager to convince others of the seriousness of their condition and their willingness to contribute to their treatment.
Patients expressed both good and bad experiences of the healthcare that followed their first interview. The good experiences related to confirmation of their condition. The bad experiences often involved feelings of being rejected. “Being taken seriously” was expressed with strong emotion when patients talked about their experiences. The “Ambiguous” type, in particular, appreciated that they had been taken seriously. They were surprised when their condition or request was not disputed, and stressed that being taken seriously was one of the most important factors when visiting healthcare. Conversely, they felt ashamed when their disorders were questioned.
“When I go to the health centre, it always feels like they’re a little stressed and that you are a bit of a nuisance when you’re there. You feel that you shouldn’t really be coming there at that time, because they think that’s a time for urgent cases and they wonder why you’re there if your problem is not urgent…She asked me, ‘Why have you come at this time?’, and then I said that I phoned my doctor and she booked the time [laugh]. It felt as if she said, ‘You come here and take up my time. This wasn’t so terribly important.’” Woman, 29 years old.
Getting an explanation. The patients hoped to meet an expert on back and neck pain and to get a clear explanation for their pain, even though they had their own theories about its cause. The “Confident” type were clear about the cause of their pain, placing the blame on hard work. The “Ambiguous” type were more hesitant and partly blamed themselves when they talked about the cause of their pain. They felt vindicated if they received a diagnosis, a good explanation and a prognosis. Referral to X-ray or orthopaedics was not crucial for a feeling of confirmation. However, those who did not receive an explanation or prognosis were very disappointed. Simply explaining it as back pain was not sufficient; patients wished to be given a more precise explanation. The “Ambiguous” type said that during the consultation they thought of asking the general practitioner for an X-ray referral or other investigations to clarify the cause, but had refrained from doing so. They could not explain why they had refrained.
The message from the healthcare professional could sometimes be confusing or contradictory; for example, if the patients followed their advice and restrictions, but improvements did not occur, and the general practitioner or physiotherapist persisted with the assessment and continued to give the same advice.
“But then it feels a little frustrating as it [pain] doesn’t get better. Seeing that I do all those exercises and they say that’s what helps. Even when they’ve twisted me this way and that and massaged, it hasn’t really felt any better. This is frustrating because he says that it is good, and then I don’t really understand why it doesn’t feel better.” Woman, 29 years old.
To be invited to participate. The patients expressed a willingness to participate in their treatment. They expected advice, guidance and training programmes. The “Confident” type expected more passive treatment than the “Ambiguous” type. The “Ambiguous” type, who thought that they had contributed to the pain because they had not been training enough, were eager to state their willingness to do a lot on their own.
Participation was an emphasized experience. The patients felt that they had been invited to participate in the assessment and treatment options if their own theories about the condition were listened to and confirmed. When their own thoughts about the causes of the pain were ignored or rejected, or when they were not invited to take part in the treatment, they were frustrated even if they had become pain-free.
A comment about not being put on an exercise programme: “No [with emphasis]. I think that was a real pity. I would like to have had that, for sure, so that you can work on it yourself. Certainly it’s good and a luxury to be treated just like that, of course. But it wasn’t really geared up for me, I suppose, in that I didn’t really know what I had cured or what he’d helped me with.” Man, 22 years old.
To be assessed and treated individually. Those who did not have any previous experience of healthcare did not express expectations about individuality during the first interview. Those with previous experience, especially the “Ambiguous” type, wanted to be seen as individuals. They feared being regarded as one of many with back problems in a large segment of the population.
A feeling of being individually assessed and treated was important when talking about the experience. The patients did not want a standard training programme. They wanted the confirmation of being treated as a unique individual rather than a patient on a conveyor belt.
“It feels like I am unique for her. I think she starts out from the basis that every patient is unique, that there isn’t an ‘off-the-shelf’ solution in my case.” Woman, 42 years old.
To be taken care of in a trustworthy environment. Patients wanted to “To be taken care of in a trustworthy environment”. A feeling of being in safe hands was important. This included not being frightened or offended. Having follow-up consultation was also important, as well as the continuity of care. When talking about their experiences, being viewed as a whole person rather than simply as a body part was central. The “Ambiguous” type, who felt they were not getting confirmation of their illness, wished for a more multi-disciplinary management.
To be confirmed or not. The core category that emerged was “Getting confirmation”. In the follow-up interview, patients expressed that confirmation was obtained if they were taken seriously, had pain confirmed by an explanation, were invited to participate, were treated individually, and were taken care of in a trustworthy environment. In the third step of the analysis, a comparison of experiences after 3 months was carried out for the two ideal types, and was described in a model (Fig. 1). The analysis showed that “Confident” and “Ambiguous” types reacted differently and in accord with whether they did or did not receive confirmation of their illness. During the process, the patients moved between the two types, as illustrated in Fig. 1. If the “Confident” type received confirmation of their illness (A in Fig. 1), they felt trust in the healthcare received even if they had not fully recovered. They were satisfied, and experienced a reorientation that the pain could now be controlled. If the “Ambiguous” type received confirmation of their illness (B in Fig. 1), there was a movement from “ambiguity” towards “confidence”, and they also felt satisfied and reoriented.
The “Ambiguous” patients who did not receive confirmation of their illness were dissatisfied and unhappy (C in Fig. 1). They doubted the assessment and felt helplessness. They felt more ashamed, lost their orientation and felt forlorn. If the “Confident” patients did not receive confirmation of their illness, their reactions (D in Fig. 1) were either anger, frustration and feelings of shame and abandonment, or they remained proud and blamed the professional’s ignorance. Because of these attitudes, they did not lose orientation and continued to seek confirmation until they got it.
Disconfirmation was experienced more negatively by women than by men, irrespective of ideal type. If disconfirmed, women usually ended up in field C in Fig. 1.
DISCUSSION
The results of this study show that patient expectation was to have their disorder confirmed by the physiotherapist or general practitioner. This remained the most important factor 3 months later when they described their experiences of care. Essential for their experiences of confirmation were: “To be taken seriously”, “Getting an explanation”, “To be invited to participate”, “To be assessed and treated individually”, and “To be taken care of in a trustworthy environment”.
Being the “Confident” ideal type made it easier to experience confirmation while; being “Ambiguous” made it difficult to do so. The ideal types were not defined by sex, but more men expressed features characteristic of the “Confident” type and more women expressed features characteristic of the “Ambiguous” type.
The core category in this study was “Getting confirmation”. According to Gustafsson & Pörn (19), confirmation in healthcare is a process that yields evidence; external evidence in the form of a relationship or an interaction between the patient and healthcare professionals, and internal evidence in the form of self-assessment. Confirming interactions are present when a patient receives external evidence that either strengthens their positive self-assessment or weakens their negative self-assessment (19). When applying Gustavsson’s & Pörn’s theory in our study, each of the categories can be seen as examples of external evidence. The “Confident” type had a positive self-assessment and the “Ambiguous” type had a negative self-assessment according to the features of the ideal types. Patients felt confirmed when the external evidence strengthened their positive self-assessment, as for the “Confident” type, as shown by A (Fig. 1), or when external evidence weakened their negative self-assessment, as for the “Ambiguous” type, as shown by B (Fig. 1). Confirmation led to the patient being able to move on. The “Ambiguous” type, as shown by C (Fig. 1), were strengthened in their negative self-assessment and this led to disconfirmation and an inability to act.
The “Confident” ideal type in field D (Fig. 1) handled loss of external evidence in different ways: men regarded it as shortcomings in the healthcare providers and searched for new healthcare contacts. Women lost their positive self-assessment and were ashamed. External evidence appeared to be more important for women than for men. The negative self-assessment among the “Ambiguous” could be due to the stereotype of women as complainers seeking healthcare with unnecessary disorders. The stereotype is historically derived; the male body was viewed as the norm and associated with strength and rationality, and the female body was viewed as a deviation from the norm and associated with weakness and emotionality (20). Ideas about differences between the female and male body and how to handle pain still derive from gender: boys, more often than girls, are told not to cry; as adults, stoicism is expected from men and when women express pain it does not need to be taken seriously (21). The “Confident” type found it easier to apply the male stereotype, about back and neck pain because it legitimized the pain including for women. It was more difficult for the “Ambiguous” type to apply the female stereotype for back pain, which includes an image of a weak woman who complains without genuine cause and does not legitimize the pain. In this study, the “Ambiguous” type also included male patients. Resistance of female pain patients to being connected with a negative image was examined previously in an interview study of female chronic pain patients (22). Other manifestations in our study were that the “Ambiguous” type tried to convince the healthcare professionals of the seriousness of their condition and expressed apprehension about not be treated as an individual, but as representative of a group. Since women might be perceived as more emotional and complaining, there is a risk that women’s pain is underestimated (23). The stereotype of women as complainers could have led to more women being found among the “Ambiguous” type, but the patients’ thoughts about how they would be perceived by others as back pain patients (without being women) also led to feelings of shame and ambiguity. In previous studies, patients with chronic back pain described feeling discredited among family, friends, co-workers, and in healthcare and society (24). However, in this study this was also found among some of the patients with acute back pain.
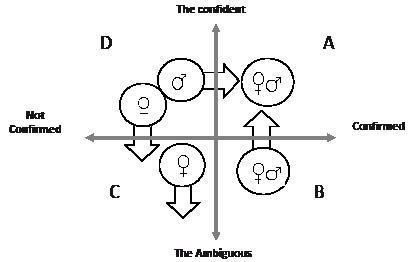
Fig. 1. Model of the interplay between ideal type, experience of confirmation and gender during the treatment period. “Confirmed” in this figure means: “To be taken seriously”, “Getting an explanation”, “To be invited to participate”, “To be assessed and treated individually”, and “To be taken care of in a trustworthy environment”. ♀: female; ♂: male.
In this study, patients who did not get confirmation lost orientation and felt forlorn. They did not have a plan for further action. According to Gustafsson & Pörn (19), confirmation increases confidence in individuals’ ability for self-determination and is a component of human motivation. However, healthcare professionals should be especially observant when patients display features described under the “Ambiguous” ideal type, to enable patients to adjust their efforts to obtain a confirming interaction (Table III).
| Table III. Categories and open codes in the construction of the ideal types | ||
| Ideal types | Categories | Open codes |
| “Ambiguous” | Belittles oneself | Does not want to be a nuisance |
| Speaks ironically about the problem | ||
| Proud of not taking advantage of the health system | ||
| I am not that kind of person | Self-image that does not fit having back problems | |
| Feelings of shame | Feels guilty about incapacity | |
| Bad conscience due to not doing any exercise | ||
| Does not talk about the problem | Worries about being viewed as a “complaining old woman” | |
| “Confident” | Talks about the problem | Just talks about the problem |
| Blames work | Blames work | |
| Pride | Strong man | |
| Getting help is girlish | ||
| Back pain is the price of endurance and strength | ||
A surprising result of this study was that the patients placed so little emphasis on recovery. Another study also noted that patients, when talking about their experiences, did not complain about not being cured, but rather that they were not taken seriously (25). In this study, patients also emphasized the importance of “Being taken seriously”. The “Confident” and the “Ambiguous” type had different strategies to achieve this and they were closely linked to their perception of self-value. The “Confident” type took the help of healthcare for granted and trusted in their ability to get the care they required. The “Ambiguous” type, on the other hand, were eager to convince the healthcare professionals about the seriousness of their condition. The recent Swedish national debate about sick leave and its increasing societal costs could be the reason for this. One could speculate that patients with a strong self-identity were less affected by the debate, while the “Ambiguous” type thought it was about them and prepared themselves with arguments, such as the seriousness of their pain. This has been shown previously among patients with chronic pain (26).
The “Ambiguous” type expressed feelings of shame prior to seeking healthcare. However, if they felt confirmed in the encounter they started to move toward the “Confident” end of the spectrum. When the “Ambiguous” type were not confirmed, feelings of shame increased. Feelings of shame could have a detrimental influence on rehabilitation. Shame-inducing encounters have been found to delay return to work (27). As the “Ambiguous” type included more women shame could be one reason why women are more on sick leave than men. Gustafson et al. (28) found that shame changes to self-respect when women with fibromyalgia and widespread pain are believed and receive a diagnosis.
The expressed will to participate in the treatment by both the “Confident” and the “Ambiguous” types was encouraging. They wanted training programmes and advice about self-care. Over the last decade, there has been a discussion about the need for the management of neck and back pain based on evidence of effectiveness (29). The focus has shifted from passive treatments, such as rest and sick leave, to a focus on physical activity and avoidance of sickness absence (30). Our findings are supported in a review that found patients with long experience of back and neck pain desired greater participation in their treatment (9). May showed that satisfaction among patients with back pain was connected to provision of information, empathy and promotion of self-care (31).When the ideal types in this study talked about expectations and experiences in different ways they based this on gender and concepts about neck or back pain; for example, when the “Ambiguous” type were reluctant to tell others about their pain for fear of being viewed as complainers. As gender is created in relations, healthcare professionals’ ideas about gender also influences the encounter (13). This interaction was not studied here, but another study showed that women and men with the same symptoms presented themselves in different ways (32). They were also treated in different ways by their doctor (32). It is important to be aware of ideas of gender, but at the same time, one must be careful not to apply one template to all men and a different template to all women (33). We hope that the results of the present study will encourage rehabilitation professionals not to abandon “Ambiguous” patients, but rather to listen to their expectations and utilize their motivation to participate in treatment. This would not only counteract feelings of shame and of being rejected among the patients, but would also lead to more efficient rehabilitation, as motivated patients can be rehabilitated more cost-effectively than less motivated patients (34).
The importance found in our study of obtaining an explanation and a diagnosis is consistent with the results found in other studies (9, 10, 31, 35). The biomedical model, which views that the diagnosis is a confirmation of real pain experienced by the patient, is still the dominant perspective in medicine. A diagnosis gives the patient access to treatment and financial support (9). However, most back and neck patients do not receive a clear diagnosis and cannot be confirmed as either sick or healthy (36). A shift in the perspective from a biomedical to a more biopsychosocial perspective began in the 1980s (37). The biopsychosocial perspective constitutes the basis for the International Classification of Functioning, Disability and Health (ICF) developed by the World Health Organization (WHO) (38). This is a classification dealing with domains that affect health (e.g. body structure and function, activity, participation, environment and personal factors) and is commonly used in rehabilitation. All of our study patients placed the focus of their pain on body structure and function. However, the “Confident” type also emphasized environmental factors and the “Ambiguous” type emphasized personal factors as affecting health. Both patients and primary care healthcare professionals could benefit from wider use of the ICF model. It would be advantageous to shift the focus away from body structure and function to include other components that have an impact on their condition. This would be even more important when a diagnosis based on clinical and laboratory tests and X-rays is difficult. According to Salomon, placing the cause of pain outside the patient can legitimize the symptoms and strengthen the patient’s handling of social and emotional problems that contribute to the symptoms (35). This is in line with how the “Confident” type handled their pain in our study when the blame was placed on their work.
Methodological discussion
A limitation of this study is that two of the patients had appointments with general practitioners and the rest with physiotherapists. This occurred because one healthcare centre had no physiotherapist on duty and one patient was in need of sick leave. It can be presumed that patient expectations differ depending on who an appointment is with, since physiotherapists and doctors typically use different treatment methods. For example, patients with an appointment with a general practitioner expect a diagnosis and prescription of pain-relieving drugs. Patients with physiotherapy appointments expect manual treatments and training programmes. However, in the analysis no difference in patient expectations was found by healthcare provider profession. Neither could any concordant differences be found with regard to patient experiences of the care based on the care provider’s profession or sex. This was due to the design of the study, in which the patients included experiences from other healthcare visits when talking about experiences of care. Earlier studies show that female doctors spend more time in consultation and give more information compared with their male colleagues (39). Female and male physiotherapists use partially different methods when treating patients with neck or back pain (40).
Four patients in our study were working in healthcare. This could have had an impact on the results, but in the analysis these patients were represented both in the “Ambiguous” type and in the “Confident” type, as confirmed and not confirmed, and consequently did not have affect the results.
All 3 authors are physiotherapists and women. This could certainly have had an impact on the interviews and analysis. However, findings in qualitative studies should not be seen as generalizable truths, but as the researchers’ description and interpretation of the data. Being a physiotherapist could be an advantage in the analysis, as it provides an inside perspective of the patient-physiotherapy interaction. At the same time, it could be a disadvantage if personal experiences are allowed to dominate the analysis. For that reason, as described in the analysis, we put emphasis on constant comparison and crystallization.
As gender is created in social relations, the fact that the interviewer (GS) was a woman could have affected how the patients presented their pain and expectations. This may have made it easier for women to experience a mutual understanding in sharing their experiences and for men to strengthen their maleness. A male interviewer might have obtained slightly different answers. However, we think the main results would not change, as men and women were found in both ideal types. A danger when studying gender in small samples is that the results can be used to strengthen stereotyped concepts about how women and men behave. Further studies are needed to understand the large variation in gendered practice and, in more depth, how gender impacts patient expectations and experiences in healthcare and rehabilitation.
It is also important to investigate further how the interaction between healthcare personnel and patients is affected by gender.
Contextualization is an important feature in qualitative studies. In our study, all of the patients were native Swedes with full access to the social security system. Therefore, differences in ethnicity or access to sickness compensation should not have influenced the results. The same study conducted in another society with a different social security or medical system and other norms about gender and neck or back pain may have yielded different results.
The results of this study were not affected by age or education. The sample was chosen for maximum variation, and this made the material less sensitive to those parameters. Earlier studies have shown that ethnicity, social class (21), age, and education (5) may have an impact on satisfaction with healthcare.
In conclusion, the results of this study show that “Getting confirmation” is the most important factor in discussing expectations and experiences. Patients who blame and depreciate themselves need to be recognized and given support by healthcare and rehabilitation personnel in order to increase their function and satisfaction with care. Gender has an impact on the expectations and experiences of neck or back pain patients when they seek healthcare, and this requires further study.
Acknowledgements
The authors would like to thank the participants in the study. The study was supported by grants from Västerbotten County Council, Sweden (ALF), and the National Graduate School of Gender studies, Umeå University, Sweden.
References
