Ross A. Iles, PhD candidate1, Nicholas F. Taylor, PhD2, Megan Davidson, PhD1 and Paul D. O’Halloran, PhD1
From the Department of Physiotherapy, 1La Trobe University and 2La Trobe University and Eastern Health,
Melbourne, Australia
Ross A. Iles, PhD candidate1, Nicholas F. Taylor, PhD2, Megan Davidson, PhD1 and Paul D. O’Halloran, PhD1
From the Department of Physiotherapy, 1La Trobe University and 2La Trobe University and Eastern Health,
Melbourne, Australia
OBJECTIVE: Low recovery expectations have been identified as a strong and consistent predictor of poor outcome in non-chronic non-specific low back pain (NSLBP). The aim of this study was to explore how people determine their own recovery expectation during an episode of non-chronic NSLBP.
Subjects and methods: In-depth interviews were conducted with a purposive sample of people with non-chronic NSLBP and low recovery expectations. Interviews were audio-recorded and transcribed verbatim. Two researchers independently applied open coding, followed by axial coding to allow themes to emerge from the data using a constant comparison method.
RESULTS: The central theme of the person and 4 subthemes of pain, progress, performance, and treatment emerged from the data. The formation of recovery expectations was dependent on the person’s unique apprasial of their pain, how the condition had progressed, the limitation of their performance of activities, and the impact of different aspects of treatment.
CONCLUSION: Recovery expectation is a person’s appraisal of several factors to determine when they are likely to return to their usual activities during an episode of non-chronic NSLBP. Health professionals should explore the person’s perception of these factors as part of a tailored intervention to prevent non-chronic NSLBP progressing to chronic NSLBP.
Key words: low back pain; recovery expectation; qualitative research; recovery of function.
J Rehabil Med 2012; 00: 00–00
Guarantor/correspondence address: Ross Iles, Department of Physiotherapy, La Trobe University, Melbourne, Bundoora, Victoria 3086, Australia. E-mail: r.iles@latrobe.edu.au
Submitted September 22, 2011; accepted April 18, 2012
INTRODUCTION
Non-specific low back pain (NSLBP) is common, costly and disabling (1, 2). The clinical course for the majority experiencing non-chronic (lasting less than 3 months) NSLBP is characterized by a rapid resolution of pain and disability (1–3). However, for a small proportion NSLBP persists for longer than 3 months and progresses to chronic NSLBP. Chronic NSBLP is characterized by persistent pain and disability and represents a significant challenge in healthcare (2, 4, 5). As a result, the small proportion of people progressing to chronic NSLBP consume the majority of the resources devoted to the management of NSLBP (1–3). Identification of individuals who are at risk of developing chronic NSLBP in the non-chronic phase may allow targeted intervention to prevent the development of ongoing problems, leading to lower financial, personal and societal costs (1, 2).
A number of factors may contribute to the progression of non-chronic to chronic NSLBP, including individual factors, such as age and gender (6), environmental factors, such as workplace issues (7) and psychosocial factors (8), such as attitudes and beliefs. In a recent systematic review of psychosocial predictors of failure to return to work due to non-chronic NSLBP, low recovery expectations were found to be the strongest and most consistent psychosocial predictor of poor outcome (9). However, little is understood about how the construct of low recovery expectation is formed and how it influences outcomes. Two recent qualitative studies examining return to work after occupational NSLBP provide insight into the formation of recovery expectations for return to work (10, 11). However, return to work is just one of a range of important outcomes in NSLBP (12, 13), and the predictive ability of recovery expectations extends beyond the work arena (14). It is therefore important to extend the understanding of recovery expectations to more general activity limitations in order to understand their influence on the progression from non-chronic to chronic NSLBP.
If low recovery expectations are a core predictor of poor outcome in people with non-chronic NSLBP, then understanding the factors that make up a person’s low recovery expectation would be useful to inform clinical management and potentially prevent the development of chronic NSLBP. When an individual reports a low expectation of recovery, it is not known what factors are considered to arrive at that conclusion. Since the goal of early identification of those at risk of developing chronic NSLBP is to target appropriate interventions and prevent the development of chronic disability, further qualitative research is warranted in order to fully understand the impact of recovery expectations on outcomes for people with non-chronic NSLBP.
Therefore, the aim of this study was to gain a deeper understanding of low recovery expectations to better inform the clinical management of people with non-chronic NSLBP.
METHODS
This study forms the second phase of a mixed methods sequential explanatory research design (15). In this design quantitative data is first collected, analysed and utilized to identify characteristics to guide purposeful sampling for the second qualitative phase (15–17).
The first phase of this research consisted of two quantitative systematic reviews regarding prognosis in non-chronic NSLBP (9, 14). The first review identified that low recovery expectations are a robust predictor of failure to return to work (9). The second review identified that recovery expectations are also predictive of non-work outcomes and provide the strongest prediction when expectations are measured within 3 weeks of NSLBP onset using a specific and time-based measure (14). Therefore, this second phase aims to build on the results of these two quantitative reviews using qualitative methods to explore the construct of low recovery expectations.
Participants
A purposive sampling strategy (15, 16) was used to select participants with non-chronic (less than 3 months’ duration) NSLBP and low recovery expectations. People presenting to the emergency department of a metropolitan hospital for treatment of an episode of NSLBP were screened for eligibility by the attending physiotherapist. Exclusion criteria were pain due to a specific cause (such as tumour, fracture or recent pregnancy), suspected neural compromise and a history of back surgery.
To be eligible, participants were to be aged between 18 and 65 years, had an onset of NSLBP within the past 8 weeks and had low recovery expectations, defined as a response of 7 or less to the question, “How certain are you that you will return to ALL of your usual activities 1 month from today?” on a scale from 0 (not certain at all) to 10 (completely certain). Previous studies have found that recovery expectations are positively skewed (14) and pilot testing of the recovery expectation question prior to commencement of the study found that a score of 7 or less on the 10-point scale represented the lowest third of responses.
In-depth interviews
Interviews were conducted by the first author and lasted approximately 30 min. The interview was based around the participant’s response to the question “How certain are you that you will return to ALL of your usual activities 1 month from today on a scale from 0 (not certain at all) to 10 (completely certain)?” The interview revolved around 4 topics: asking the person to describe their back problem; asking the person to consider different aspects they considered when determining their recovery expectation score; asking the person what would change their recovery expectation; and asking the person to identify any barriers to their return to usual activities. A list of questions covering these areas was devised; however, participants were encouraged to discuss any issues they felt were important around their back problem and their expectation of recovery. In line with recommendations data were analysed inductively (16), with analysis occurring as data were being collected and when new themes emerged from an interview, these themes were also explored in subsequent interviews via additions to the question list. Recruitment continued until saturation was reached and no new themes emerged from the interviews (16).
Interviews were audio-recorded and transcribed verbatim. Transcripts were compared with the audio-recording of interviews by the lead author before being posted to participants to ensure the transcript was an accurate reflection of the conversation and to allow the participant to make any additions or corrections. No participants made corrections or additions and upon return of the file to the researcher, all identifying information was removed from the transcript.
Ethics approval for the study was granted by the university and health service ethics committees and all participants provided written informed consent.
Analysis
Interview transcripts were coded by two researchers independently. One researcher coded transcripts manually, while the other used the QSR NVivo 8 computer program (QSR International) to assist with organizing and coding the data. Codes were derived from the transcripts to illustrate the phenomenon as described by the participants,
allowing themes regarding the formation of recovery expectation to emerge from the data. This was done first using open coding techniques, followed by axial coding to group and collapse codes into common themes where possible (16–18). Constant comparison was used to ensure earlier interviews were examined for codes and themes emerging from later interviews (17). After the initial coding the researchers compared codes and discussed any differences in coding labels to reach consensus.
Several strategies were employed to ensure the credibility or trustworthiness of the analysis (16–18). The sampling method used identified participants with low recovery expectations to provide relevant examples of the phenomenon of interest. To identify the range of elements contributing to low recovery expectations in people attending an emergency department for treatment of non-chronic NSLBP, recruitment continued until no new themes emerged from interviews. Recorded interviews, verbatim transcripts and participant checking of transcripts ensured that the content that was analysed was a true reflection of the interviews. Codes and themes were allowed to emerge from the data rather than trying to fit the data to any pre-existing framework. Two researchers independently coded the transcripts and later compared and discussed codes in an attempt to reduce the influence of one individual’s interpretations of the phenomenon. An iterative approach was taken to the analysis to ensure all interviews were analysed for the same codes and themes. Finally, direct quotes were used to provide examples of the themes emerging from the data.
RESULTS
Thirteen people were interviewed between July 2009 and March 2011 (Table I). Participants ranged in age from 22 to 64 years, with a mean age of 51 years. Both sexes were represented and most participants worked full-time. Nine people reported previous episodes of back pain. The majority of the interviews were conducted within 2 weeks of the onset of the problem, with 2 interviews conducted 6 weeks after onset. Eleven participants reported an improved recovery expectation at the interview compared with the screening, with participant 6 (P6) the only participant reporting a lower recovery expectation at the time of interview.
| Table I. Summary of participants | |||||||
| Participant number | Gender | Days between onset and interview | First episode of back pain? | Previous number | Work status | Recovery expectation at screening | Recovery expectation at interview |
| P1 | M | 42 | No | Unknown | Not working | 4 | 4 |
| P2 | M | 5 | No | 1 | Full-time | 3 | 5 |
| P3 | F | 14 | Yes | 0 | Full-time | 4 | 6 |
| P4 | F | 9 | No | 2 | Full-time | 7 | 8 |
| P5 | F | 7 | No | 4 | Full-time | 4 | 6 |
| P6 | M | 14 | No | 2 | Full-time | 5 | 4 |
| P7 | M | 6 | Yes | 0 | Full-time | 5 | 9 |
| P8 | M | 42 | No | 3 | Full-time | 7 | 9 |
| P9 | F | 8 | Yes | 0 | Full-time | 4 | 5 |
| P10 | M | 11 | Yes | 0 | Full-time | 2 | 3 |
| P11 | F | 11 | No | 5 | Part-time | 7 | 10 |
| P12 | F | 4 | No | 2 | Casual full-time | 0 | 5 |
| P13 | M | 4 | No | 4 | Full-time | 7 | 8 |
| Summary | 7 M 6 F | Median 9 | 4 Yes 9 No | Median 2.5a | 1 not working 1 part-time 1 casual full-time 10 full-time | Median 4 | Median 6 |
| aMedian for those with previous episodes (P2, 4, 5, 6, 8, 11, 12 and 13, excluding unknown number of episodes for P1). | |||||||
Codes emerging from the data were collapsed into 1 central theme and 4 key subthemes (Table II). The overarching theme was that of the person, reflecting the individual’s appraisal of multiple factors dependent on elements such as past experience, beliefs and attitudes. Subthemes of pain, progression, performance and treatment were also identified. When forming their expectation of recovery individuals considered their pain levels, how the condition had progressed, how pain impacted their current and predicted performance of their usual activities, and the impact of treatment and treating professionals to date (Table II). Each of these subthemes were dependent on the person’s apprasial of each aspect when determining their expectation of recovery (Fig. 1).
| Table II. Coding information for recovery expectation | |
| Categories of coded statements | |
| Central theme | |
| Person | Belief Attitude Past experience |
| Subthemes | |
| Pain | Pain descriptors Barrier to activity |
| Progression | Improvement Getting worse |
| Performance Subtheme: Usual activities of Subtheme: Work | Basic tasks Bending Walking Lifting Sitting Driving Housework Gardening Recreational Specific work tasks Work environment Modification of task |
| Treatment | Diagnosis Imaging Influence of practitioner |
Fig. 1. The theme of the person is central to the construction of recovery expectations and influences the interconnected subthemes of pain, progress, performance and treatment.
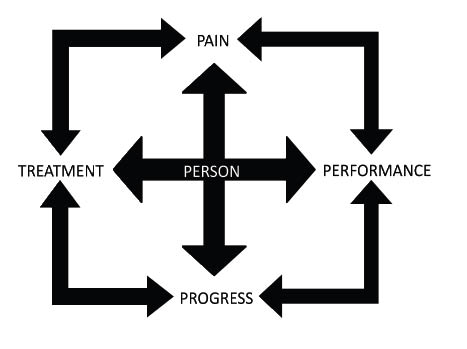
Central theme: Person
The impact of a person’s lived experience, not only of NSLBP but of life in general, was a very important part of determining expectations of recovery. While each participant considered common aspects when determining their recovery expectation, the contribution of each aspect was determined by the person’s own appraisal of what they considered to be the key characteristics of their NSLBP experience. This appraisal was a reflection of past experience, attitudes and beliefs that were unique to each individual. For example, a range of attitudes toward pain were described, ranging from passive attitudes to recovery to very active approaches to exercise and rehabilitation.
“Yeah, it’s a bit like I’m in limbo. Yeah, I just, you know I can’t move forwards, I can’t do anything except manage pain and kick back. Um, and that’s no fun.” (P11)
“It’s to how, to how people mentally and physically work at it isn’t it? You know, I mean I could say I’ve got a sore back, sit on my arse on go off on sick leave for 3 months couldn’t I? You won’t get better, you’re not going to get better are you?” (P10)
The importance of past experience with injury or illness also emerged as an important determinant of recovery expectation. In the case of participants who had experienced episodes of NSLBP before, this experience was used as a comparison to the current episode and incorporated into the expectation of recovery. Otherwise other injuries or illnesses were used as a comparison, and when the current experience was beyond any of their past experiences, lowered recovery expectations reflected that uncertainty.
“So the first time I did it and the time just recently have been the worst, in between it’s, it’s been pretty bad but not like the first and last time. Yeah, just much, much more pain.” (P5)
Past experience also extended to treatment-related factors and had an impact on beliefs and attitudes towards recovery. Past experiences were combined with the experience of the current episode as part of the individual’s appraisal of the treatment they were being provided.
“So I’m, even though with my past experience I’ve been bitten, I’m trying my hardest to put my trust in the professionals so to speak.” (P3)
So, while each participant considered common subthemes of pain, progression, performance and treatment when determining their expectation of recovery, how each person processed these factors was highly individual and reflecting the lived experience of each person.
Subtheme: Pain
The experience of pain was an important consideration for participants and was a major barrier to return to usual activities.
“Just the pain. Just all, well that’s all there is, there’s just the pain like if all the pain was in one spot it’d be fine because the pain is going from my lower back all the way down my thigh all the way down my calf and then into the numbness it feels like I’m basically disabled like I couldn’t really do anything.” (P6)
As a result, a decrease in pain was strongly linked to an increase in expectation of recovery. Participants used pain levels, with or without analgesia use, to judge whether their condition was improving as part of determining their recovery expectation.
“Well I suppose I’m just thinking if I go off these tablets and I’m in, I don’t go back to that original pain, I think, well yeah, something has recovered in these couple of days.” (P12)
Subtheme: Progression
When determining their expectation of recovery participants compared their current pain with their initial pain to determine how much their condition had progressed. This rate of improvement was projected into the future to determine when they might return to all usual activities.
“When they asked me that question in hospital I was feeling atrocious, I could hardly move, so I said zero. How I’m feeling now is I can actually get up and walk.” (P13)
“Yeah, 2 months I reckon, 2 months because it’s been 10, 15 days and I get, I can see the progress.” (P3)
Seeing steady improvement was strongly linked to increasing expectation of recovery. The importance of this progression was most clearly illustrated by the one participant whose expectation of recovery decreased between screening and interview.
“Cause it’s just, it’s a pain that it feels like it’s, it’s staying there. It’s just it’s been like this for 2 weeks and ever since I’ve been to the hospital, nothing has got better really.” (P6)
This participant did not experience any improvement in their condition, and indeed reported the condition had worsened and this had a clear impact on his expectation of recovery.
Performance
Participants not only judged the progression of the condition by the level of pain, but also by the extent to which pain interrupted their performance of a range of activities. These activities were coded into two distinct categories; first, the usual activities of daily living and, secondly, work. All participants mentioned specific activities they were having difficulty with as a result of their condition. The most commonly mentioned activities included bending, sitting, walking, housework and gardening.
“I’m anticipating walking, getting out into the natural environment, getting out into my garden, bending down mucking around with the cat.” (P12)
The intrusion of back pain into the performance of basic activities and the impact on daily life was clearly a consideration when determining expectation of recovery.
“…to be able to drive my car to my girlfriend’s, to be able to go out for dinner or to be able to do things, I need to be able to sit in my car.” (P6)
When considering return to usual activities, all working participants spoke about specific tasks transferred into the work environment. The characteristics of the work environment were specific to each individual, as was the potential for modifications that could be made to reduce the physical demands of the job.
“It’s been sort of in the back of my mind thinking about work and when I go back how and I going to deal with it, what, what are the things or the modifications or the tools that I can um, do, or do I ask to work from another work centre temporarily, or to make it a little bit easier on myself, so I that I can make that full easy recovery, yeah.” (P12)
When a participant perceived support for modifying their work tasks and the workplace, recovery expectations were positively influenced. The expectation of being able to work was also significantly impacted by the nature of the tasks performed at work. One participant described a physically demanding job that had no potential for lighter or alternate duties, and this decreased their expectation of being able to return to work in the near future.
Treatment
Treatment-related factors had a clear impact on recovery expectations. Information provided by the doctor or the physiotherapist could increase or decrease expectations depending on how the individual perceived the information that was provided. An example of this was the participant who considered the motivations of the health professional who was providing the information.
“Well on this particular occasion what that girl [physiotherapist] said in the hospital, had a massive impact on me because I was pretty scared… But it’s just what she said and that, that probably had more impact because it was unsolicited comment, than if I’d asked her ‘well what’s going to happen?’” (P7)
The importance of diagnosis clearly emerged from the data, with several participants stating that being given a clear diagnosis would impact their expectations. Having a clear explanation for their symptoms and knowing what was wrong would increase recovery expectations.
“If the physio had said, oh right, you’ve had, you’ve got such, I know you can’t do it, you… the pain is coming from here, it’s probably such and such, we’ll do a CT, we’ll do an MRI, we’ll find out exactly where it is and we’ll give you the appropriate exercises or not appropriate exercises” (P12)
The role of imaging in providing a diagnosis emerged from several participants, with one participant particularly focused on the results of a magnetic resonance imaging (MRI) scan. For this participant their recovery expectation was almost completely dependent on the results of the investigation.
“I’m not sure how they can start rehabilitating me when they don’t have the MRI, you know what I mean? Because then once they know what it is, then they can fix it. But with, a CT scan won’t show up enough to know what, how [to] fix it.” (P10)
DISCUSSION
For people in this study, expectation of recovery appeared to be a construct centred on the person’s appraisal of 4 subthemes of pain, progression, performance and treatment (Fig. 1). The importance of the lived experience of the individual was represented in the variation in the experience and meaning of pain across participants. The International Association for the Study of Pain (IASP) definition of pain refers to the individual nature of pain when defining it as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage.” (19; p. 209). The interpretation of pain will be different for each person depending on their past experience, attitudes and beliefs around, not only NSLBP, but all aspects of their experience of injury or ill health. This individual nature of recovery expectations may help to explain why other psychosocial factors, such as job satisfaction, depression, anxiety and stress, have not been found to predict work outcome (9). The impact of each of these factors alone may be too specific to each individual to emerge as important in predictive models. However, the suggested cognitive appraisal of the identified subthemes in the development of recovery expectation may be consistent enough to identify people at risk of poor outcome.
Of the 4 identified subthemes, the perception of progression appeared to have the greatest influence in determining recovery expectation. Previous research has suggested that the meaning of recovery is highly individualized and specific to a person’s context (20), and this was demonstrated in the current study by the differences between individuals when determining the progress of their back problem. If the person perceived improvement in their condition, it was likely to enable a prediction of whether and when return to usual activities would occur. Without improvement in the condition, expectation of recovery was likely to be low since there was no perceived recovery to date. Pain and the activities that each person could perform were used as indicators of how the back problem had improved, and aspects of treatment such as input from a health professional and being given an explanation for the symptoms served to inform the person of what level of progress could be expected at a given stage. These factors appear to be appraised by the person and compared with their own meaning of recovery to determine the expected likelihood of being able to return to all of their usual activities.
Other studies have identified the importance of a change in the condition in predicting those who progress to chronic NSLBP. Lack of change in pain intensity and disability status in the first 3 months has been strongly related to development of chronic NSLBP (20, 21). The longitudinal qualitative study of people with chronic NSLBP by Snelgrove et al. (21) described the challenge of managing what was perceived as an unchanging pain experience despite fluctuations in symptoms. The current study suggests that several factors are involved in the person’s perception of improvement, and that it is important in the early stages of low back pain that the person perceives some level of improvement in order to have a positive expectation of recovery.
The themes and subthemes identified in the current study of expectation of recovery for usual activities are similar to those found in qualitative studies of expectation to return to work (10, 11). Self-efficacy was identified as a major component of forming expectation to return to work by Shaw & Huang (10). Self-efficacy, the confidence in being able to successfully complete a specific task, is developed over the lifespan and is influenced by a wide range of factors unique to an individual’s life experience (22). The current study identified the importance of a person’s life experience in the appraisal of their ability to perform a range of activities; however, that appraisal was also applied to pain and the progression of the condition when determining expectations for return to usual activities. The model of recovery expectation for usual activity described in the current study also shares common elements with the models of expectation developed by Olson et al. (23) and Janzen et al. (24), particularly the suggestion that expectations are socially and culturally dependent and are highly individual.
The present study was able to add to previous literature, which has focused on work-related recovery expectations by providing information about the patient’s perception of recovery expectation in returning to usual activities. Furthermore, the emergence of themes that are person-focused (such as the experience of pain and its progression) mean that the findings of the research may have clinical applicability. Data from the current study adds to the literature by suggesting possible points of clinical intervention for improving activity in both leisure and work settings. The data suggest that interventions that enable the person to explore the meaning and experience of pain and how the condition is progressing should be explored in the non-chronic phase of NSLBP. Interventions could focus on any differences in the activities the person is currently able to perform and the activities that they are required to perform as part of their usual activities. Attention should also be paid to factors around treatment and diagnosis, with the aim to address unhelpful beliefs and attitudes. One such approach is health coaching using cognitive behavioural and motivational interviewing techniques. This approach has been found to be effective in increasing physical activity levels (25) and changing health behaviours in chronic health conditions, such as coronary heart disease (26), asthma (27) and diabetes (28). A recent trial of coaching added to usual physiotherapy care found that coaching improved recovery expectations as well as measures of activity limitation due to non-chronic NSLBP (29). Addressing a person’s low recovery expectations early in the course of NSLBP may reduce the likelihood of the progression to chronic NSLBP.
The current study highlights opportunities for health professionals to have a positive effect on recovery expectation. For the individuals in this study the treating practitioner could influence expectations in both positive and negative directions. Implementation of guidelines for the treatment of NSLBP that emphasize the role of advice regarding activity and discourage unnecessary use of imaging modalities such as X-rays and computed tomography (CT) scans (30) would be expected to have a positive influence on recovery expectations. However, people with NSLBP often expect diagnostic tests in order to arrive at a clear diagnosis for the pain that informs their recovery expectation (31). A further problem for the practitioner is the prevalence of a pessimistic view of NSLBP (32). Given our results that suggest expectations are a complex and unique appraisal of pain, progression, performance and treatment, each interaction with a health professional should be seen as an opportunity to impact a person’s expectation of recovery (33, 34).
Strengths and weaknesses
The strength of the current study is the emergence of potential suggestions of how to intervene in order to promote a more positive outcome for people with low recovery expectations and non-chronic NSLBP. A health practitioner, upon identification of low recovery expectations, is likely to be able to positively impact recovery expectation through consideration and exploration of the themes identified in this analysis.
This study examined a small sample of people with non-chronic NSLBP and low recovery expectations from a single metropolitan location. As a result, the findings may be difficult to apply outside of this location. The screening for potential participants, gathering of data and the analysis performed in this study was conducted by physiotherapists and researchers with physiotherapy training. Therefore, the findings of this study are likely to contain a bias towards a physiotherapy perspective of non-chronic NSLBP. The sampling strategy employed identified only participants with low recovery expectations. Further research in this area could explore whether differences exist between people with high, medium and low recovery expectations to gain a stronger understanding of this construct.
In conclusion, recovery expectation is a person’s complex appraisal of their pain, progression, performance and treatment to determine when they are likely to return to their usual activities during an episode of non-chronic NSLBP. When a person is identified as having low recovery expectations in the non-chronic phase of NSLBP, health professionals should explore the person’s perception of these factors as part of a tailored intervention aimed to prevent the progression from non-chronic to chronic NSLBP.
REFERENCES
