OBJECTIVE: To describe the use of mirror therapy in 2 patients with complex regional pain syndrome type II following traumatic nerve injury.
DESIGN: Two case reports.
SUBJECTS: Two patients with complex regional pain syndrome type II.
METHODS: Two patients received mirror therapy with the painful hand hidden behind the mirror while the non-painful hand was positioned so that, from the perspective of the patient, the reflection of this hand was “superimposed” on the painful hand. Pain was measured with a visual analogue scale.
RESULTS: The first case had developed a severe burning and constant pain in the hand due to a neuroma. In this patient, a strong reduction in pain was found during and immediately after mirror therapy. As a result, the patient was able to perform active exercises that were previously too painful. However, despite the pain relief during and directly after the exercises, the overall level of pain did not decrease. The second patient also had severe burning pain following a glass injury. In this patient, repeated mirror therapy for a 3-month period strongly decreased pain due to causalgia.
CONCLUSION: The presented cases demonstrate that the use of mirror therapy in patients with causalgia related to a neuroma is worthy of further exploration as a potential treatment modality in patients with causalgia.
Key words: pain, treatment, physical therapy, causalgia, complex regional pain syndrome.
J Rehabil Med 2008; 40: 312–314
Correspondence address: R. W. Selles, Department of Rehabilitation, Erasmus MC, Room H016, Dr. Molewaterplein 40 PO Box 2040, 3000 CA Rotterdam, The Netherlands. E-mail: r.selles@erasmusmc.nl
Submitted April 18, 2007; accepted October 29, 2007
Introduction
The use of visual illusions created by a mirror, often referred to as mirror therapy, was first introduced by Ramachandran & Rogers-Ramachandran (1) for the treatment of phantom limb pain. This type of pain can be very severe and is difficult to treat. In some cases, the phantom limb is felt as if it is in an uncontrolled painful cramp. With mirror therapy, by concentrating on the reflection of their normal hand, patients reported that they could control and move the phantom limb, and thus experienced pain relief (2).
Over the last few years, the use of mirror therapy has been reported in a number of studies. Some of these studies have focused on the use of mirror therapy in patients with pain-syndromes, such as phantom limb pain after amputation (3) and brachial plexus avulsion (4) and complex regional pain syndrome (CRPS) type I (5–8). Other studies have focused on the use of mirror therapy for motor training after stroke (9–12). More recently mirror therapy has also been applied during rehabilitation following hand surgery (13).
Causalgia (according to the IASP classified as Complex Regional Pain Syndrome – CRPS type II) may be the result of a neuroma and is generally associated with the scarring and altered sensation of the injured nerve, at the end of which a bulbous swelling may form (14). Because of the severe pain sometimes associated with a neuroma, patients are often significantly disabled. In a review, Vernadakis et al. (14) concluded that, although approximately 150–200 techniques have been proposed for the treatment and prevention, neuroma-related causalgia is still very difficult to treat.
This study describes the use of mirror therapy in 2 patients with causalgia following traumatic nerve injury. To our knowledge, this is the first report on the use of mirror therapy in patients with causalgia in the hand following peripheral nerve injury indicating temporary pain relief during mirror exercises in one subject and a systematic overall decrease in pain in the second subject.
Methods and Results
Two patients with causalgia following a traumatic nerve injury of the upper extremity were included in the study.
During the mirror therapy, a mirror was placed vertically on a table in front of the patient with the painful hand hidden behind the mirror, while the non-painful hand was positioned so that, from the perspective of the patient, the reflection of this hand was “superimposed” on the painful one (Fig. 1). The patient was initially asked to move only the uninjured hand in front of the mirror and to focus on the image reflection for 5–10 min. The patient was asked to imagine that both hands were moving. Then, the patient was asked to perform bilateral hand movements for 5–10 min, during which the patient observed the mirror reflection of the uninjured hand. Also, the therapist touched the uninjured hand while the patient focused on the mirror reflection, visually suggesting that the injured hand was stimulated. After an instructional session, the patient was given a mirror for daily practise in the home situation and was asked to practise 3–5 times each day for approximately 15 min. The patient was asked to perform repeated short 15-min training sessions in order to be able to maintain concentration during the mirror sessions while achieving sufficient practise time (5).
Fig. 1. The mirror therapy used in the 2 subjects. The subject was positioned in such a way that the reflection of the non-involved hand was “superimposed” on the painful hand.
Pain was measured before the start and repeatedly after the start of the intervention by asking the patient to complete a visual analogue scale (VAS), which was scored between 1 and 100.
Case 1: Instantaneous and short-term pain reduction in a patient with causalgia due to a neuroma
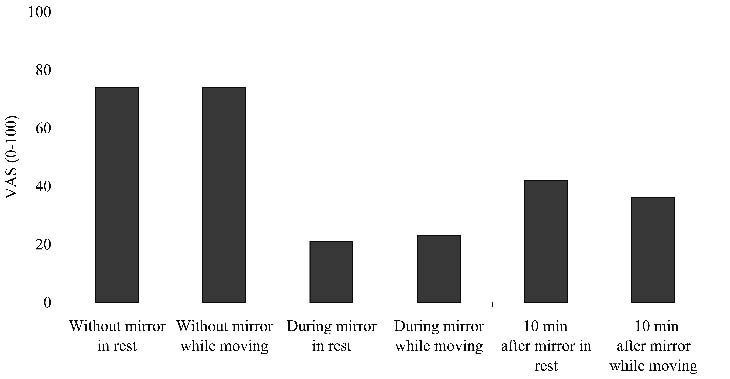
A 36-year-old woman presented 6 months after sustaining a glass injury of the right hand at wrist level, cutting the ulnar and median nerve as well as the flexor tendons of the third, fourth and fifth fingers. On the day of the injury, the nerves were microsurgically anastomosed with a 10/0 suture and the flexor tendons were repaired with a modified Kessler 5/0. Immobilization in a Kleinert splint was prescribed for 4 weeks and passive and active exercises were started gradually under the supervision of a hand therapist. In addition to the motor and sensory deficits caused by the ulnar and median nerve lesions, the patient developed a severe burning and constant pain in the palm of the hand, radiating to the fingers. About 10 months after injury, physical examination revealed a painful palpable tumour at the ulnar side of the wrist. Echosonography confirmed the presence of a neuroma of the ulnar nerve with a diameter of 3 cm. The patient was scheduled for surgical treatment and in the mean time she was treated once a week by a hand therapist to reduce pain and to maintain mobility of the joints and hand function. The causalgia was severe (80 on the VAS scale) and resistant to physical therapy and medication (gabapentin). The patient reported that she was unable to use her hand in daily activities and did not tolerate her hand being touched by the therapist. When using the mirror, the patient instantaneously reported a very strong pain reduction (Fig. 2). As a result, the patient was able to perform active exercises that were previously too painful. Ten minutes after ending the mirror session, the patients still reported pain reduction.
Fig. 2. Visual analogue scales (VAS) of the pain reported by case 1 during the first session. During the following 2 weeks, similar scores were obtained.
The mirror practices were performed for 3 weeks. Repeated use of the VAS revealed that the instantaneous and short-term pain reduction (approximately 30–45 min) was consistent during the 3-week period. However, the pain levels after the mirror therapy sessions returned to the initial (high) level.
Due to pregnancy, the neuroma surgery was postponed. Two years after the mirror training, the surgery had not been performed. Although the patient still regularly experiences pain, she is able to work again part-time. In retrospect, the patient reported that the mirror practices have specifically helped her to practise without much pain and to regain active movement of the involved hand, which helps her in activities of daily life. The patient no longer used medication for the pain.
Case 2: Long-term pain relief in a patient with severe pain after neuroma
The second patient was a 33-year-old woman who had sustained a glass injury at work, causing a complete lesion to the common digital nerves of the 3rd and 4th finger of her right hand close to the distal palmar crease. The injury was microsurgically repaired within 24 hours of the injury. In the first months after the injury, she developed signs of a neuroma, which was surgically treated about one year later. About 3 years post-injury the patient still experienced severe burning pain. She would not tolerate the hand being touched due to the pain. An intensive period of rehabilitation treatment was prescribed, including physical and occupational therapy. The treatment included desensitization therapy, which had no effect. According to the patient, the pain was constantly present and very severe.
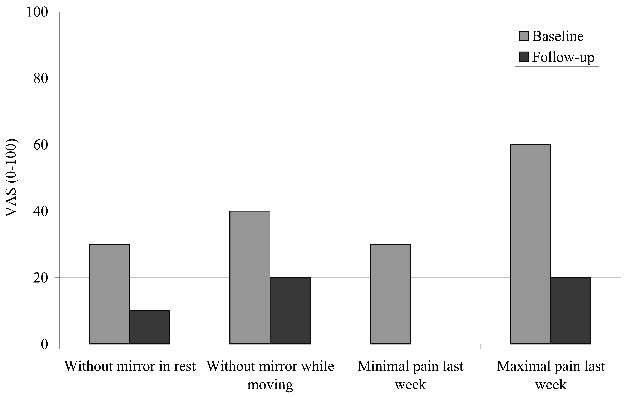
After 2 months of physical and occupational therapy, during which little effect on the pain was obtained, we started mirror therapy using the same protocol as described for case 1. During this period, the patient was not using any pain medication. Five months of mirror therapy exercises had a dramatic positive effect on the pain in the hand (Fig. 3). The hand was still painful, but the subject reported that the exercises did not cause any pain while using the mirror. Over the 5-month period, the pain in-between mirror sessions decreased consistently; a finding that the patient contributed entirely to the mirror practices. The patient reported that she started using the hand more often again in daily life situations. After 5 months, she was discharged from further treatment, although she still continued mirror exercises at home for 15–30 min each day.
Fig. 3. Visual analogue scales (VAS) of the pain reported by case 2. The first two VAS scores correspond to the pain reported by the patient at the time of measurement without the mirror present. Follow-up was 5 months after start of the mirror exercises.
Discussion
The present study reports on the use of mirror therapy in 2 patients with causalgia of the hand associated with a neuroma after peripheral nerve injury. In case 1, a strong reduction in pain was found during mirror therapy and immediately after mirror therapy. In case 2, it was found that repeated mirror therapy decreased pain due to causalgia that had been present for several years without a substantial positive effect of surgical and rehabilitation interventions.
The underlying mechanisms of pain reduction during mirror therapy are not clear. In the literature, several hypotheses have been described. For example, it has been suggested that the experienced pain may be the result of a mismatch between motor intention and proprioceptive or visual feedback. Ramachandran and co-authors (2, 15) initially suggested that the phantom pain could be the result of a disruption of the normal interaction between motor intention and appropriate sensory feedback. Using the mirror, a visual illusion can be created of a normal and pain-free movement of the limb. This idea may be in line with the hypothesis of a cortical origin of pain as described by Harris (16). Harris suggested that in those conditions where there is no convincing demonstrable or local nociceptive aetiology (e.g. CRPS type I, repetitive strain injury, phantom limb pain and focal hand dystonia), pain could be the result of a mismatch between motor intention, proprioceptive and visual feedback, in the same way that nausea can be the result of the mismatch between vestibular and visual information (5, 6, 16). A mechanism of action of mirror therapy could therefore be that a visual illusion is created that solves the mismatched between motor intention, proprioceptive and visual feedback. Another related idea is based on studies showing that altered or absent sensory feedback results in cortical reorganization of body representations in the primary somatosensory and motor cortex (S1 and M1) and that the amount of reorganization is correlated with the severity of the experienced pain (17, 18). This cortical reorganization in pathological conditions may be influenced by providing alternative sensory input using a visual illusion, thereby reducing pain (4, 13).
While in phantom pain and CRPS type I a clear peripheral aetiology for pain is lacking, suggesting that the mirror therapy influences a central nervous system component of pain (centralization), in patients with causalgia, a local origin for the pain is generally assumed. From the present study, it cannot be concluded which mechanisms caused the pain reduction in the 2 patients. While mechanisms such as distraction of attention can have a major impact on pain perception, we think that it is unlikely to have an effect of the magnitude found in case 1. Similarly, such mechanisms may not be able to explain the long-term pain relief found in case 2. Future studies with a larger population may indicate in which patients with causalgia after a peripheral nerve injury mirror therapy can be successful.
In conclusion, the cases described here demonstrate that the use of mirror therapy in patients with causalgia related to a neuroma is worthy of further exploration. Larger studies are warranted to investigate whether permanent pain relief in case 2 can also be found in other patients with similar disorders. The optimal intensity, frequency and duration of mirror therapy sessions should also be determined. Although the instantaneous pain relief in case 1 may not have resulted in a long-term decrease in pain, the patient still experienced a very strong (temporary) pain relief that could be used therapeutically to perform exercises that would otherwise not be tolerated. The short-term periods of pain relief could be used to maintain strength and joint mobility during the weeks prior to surgical treatment of the neuroma.
References
1. Ramachandran VS, Rogers-Ramachandran D. Synaesthesia in phantom limbs induced with mirrors. Proc R Soc Lond B Biol Sci 1996; 263: 377–386.
2. Ramachandran VS, Hirstein W. The perception of phantom limbs. The D. O. Hebb lecture. Brain 1998; 121: 1603–1630.
3. Brodie EE, Whyte A, Waller B. Increased motor control of a phantom leg in humans results from the visual feedback of a virtual leg. Neurosci Lett 2003; 341: 167–169.
4. Giraux P, Sirigu A. Illusory movements of the paralyzed limb restore motor cortex activity. Neuroimage 2003; 20 Suppl 1: S107–S111.
5. McCabe CS, Haigh RC, Ring EF, Halligan PW, Wall PD, Blake DR. A controlled pilot study of the utility of mirror visual feedback in the treatment of complex regional pain syndrome (type 1). Rheumatology (Oxford) 2003; 42: 97–101.
6. Moseley GL. Graded motor imagery is effective for long-standing complex regional pain syndrome: a randomised controlled trial. Pain 2004; 108: 192–198.
7. Vladimir Tichelaar YI, Geertzen JH, Keizer D, Paul van Wilgen C. Mirror box therapy added to cognitive behavioural therapy in three chronic complex regional pain syndrome type I patients: a pilot study. Int J Rehabil Res Internationale Zeitschrift fur Rehabilitationsforschung 2007; 30: 181–188.
8. Moseley GL. Graded motor imagery for pathologic pain: a randomized controlled trial. Neurology 2006; 67: 2129–2134.
9. Altschuler EL, Wisdom SB, Stone L, Foster C, Galasko D, Llewellyn DM, et al. Rehabilitation of hemiparesis after stroke with a mirror. Lancet 1999; 353: 2035–2036.
10. Sathian K, Greenspan AI, Wolf SL. Doing it with mirrors: a case study of a novel approach to neurorehabilitation. Neurorehabil Neural Repair 2000; 14: 73–76.
11. Stevens JA, Stoykov ME. Using motor imagery in the rehabilitation of hemiparesis. Arch Phys Med Rehabil 2003; 84: 1090–1092.
12. Stevens JA, Stoykov ME. Simulation of bilateral movement training through mirror reflection: a case report demonstrating an occupational therapy technique for hemiparesis. Top Stroke Rehabil 2004; 11: 59–66.
13. Rosen B, Lundborg G. Training with a mirror in rehabilitation of the hand. Scand J Plast Reconstr Surg Hand Surg 2005; 39: 104–108.
14. Vernadakis AJ, Koch H, Mackinnon SE. Management of neuromas. Clin Plast Surg 2003; 30: 247–268, vii.
15. Ramachandran VS, Altschuler EL, Hillyer S. Mirror agnosia. Proc R Soc Lond B Biol Sci 1997; 264: 645–647.
16. Harris AJ. Cortical origin of pathological pain. Lancet 1999; 354: 1464–1466.
17. Maihofner C, Handwerker HO, Neundorfer B, Birklein F. Patterns of cortical reorganization in complex regional pain syndrome. Neurology 2003; 61: 1707–1715.
18. Maihofner C, Handwerker HO, Neundorfer B, Birklein F. Cortical reorganization during recovery from complex regional pain syndrome. Neurology 2004; 63: 693–701.