OBJECTIVE: To evaluate the course and identify determinants of community integration for up to 3 years following moderate to severe traumatic brain injury.
DESIGN: Prospective cohort study.
Patients: A total of 119 patients with moderate to severe traumatic brain injury aged 16–67 years.
METHODS: The Community Integration Questionnaire was completed at 3, 6, 12, 18, 24 and 36 months post-injury. Repeated measures analysis of variance was performed to determine changes over time in the Community Integration Questionnaire and its subscales. Bivariate and multivariate regression analyses were used to identify determinants of community integration 36 months post-injury.
RESULTS: Compared with pre-injury, mean home integration, social integration, productivity, and total questionnaire scores decreased 3 months post-injury. Patient scores showed maximal improvement during the first year post-injury. Mean home integration, productivity, and total scores increased to a lesser extent during years 1–3 post-injury. Age, Barthel Index scores, hospital discharge destination, and pre-injury community integration scores were the major determinants of community integration 36 months post-injury (R2 = 60%).
CONCLUSION: After an initial decline, mean community integration scores gradually improve following moderate to severe traumatic brain injury. Understanding the course and determinants of community integration is necessary in order to determine functional prognosis following traumatic brain injury.
Key words: prognosis, craniocerebral trauma, traumatic brain injury, community integration, participation.
J Rehabil Med 2009; 41: 521–527
Correspondence address: Agnes H. P. Willemse-van Son, Erasmus MC, Department of Rehabilitation Medicine, PO Box 2040, NL-3000 CA, Rotterdam, The Netherlands. E-mail: a.vanson-willemse@erasmusmc.nl
Submitted July 9, 2008; accepted March 2, 2009
INTRODUCTION
Outcome following traumatic brain injury (TBI) can vary from complete recovery to death, with many survivors having long-term disabilities (1). Information regarding the course and prognosis following TBI is necessary to determine which patients are at risk for unfavourable outcomes, and to optimize the use of limited healthcare and social resources. For patients with TBI and their families, early prognostic information is important for coping and anticipating long-term consequences. To date, most studies on patients with TBI have focused on short-term outcomes, with a maximum of 6–12 months post-injury. Although a recent review addressed prognostic factors of long-term activity limitations and participation restrictions (2), the clinical and sociodemographic determinants of such restrictions are unknown.
Post-acute rehabilitation programmes for patients with TBI are aimed at optimizing functioning at all levels defined by the World Health Organization (WHO); body functions and structures, activities and participation. Measuring participation is a challenge. It is a multilayered concept encompassing such domains as mobility, domestic life, interpersonal interactions and relationships, as well as community, social and civic life (3). The Community Integration Questionnaire (CIQ) (3) has been designed to assess participation in patients with TBI (4). Earlier studies revealed that several clinical and sociodemographic factors may be related to community integration. Clinical determinants of poor community integration following TBI include a more severe injury, poorer functional performance and disability, extended post-traumatic amnesia (5, 6), prolonged acute hospital stay (5), loss of emotional control (6), poor cognition (5, 7), poor physical condition (5), poor pre-morbid functioning (7), and more severe activity limitation (5, 6). Furthermore, patients injured by a violent mechanism have lower levels of community integration (8), whereas patients injured by motor vehicle accidents have higher levels of community integration (9).
Relevant sociodemographic determinants of community integration are male gender, living with others, emotional distress (4), being a member of a minority race (10–12), lower educational level (8, 11), and unemployment at the time of injury (8, 11). Some studies show that older age is a risk factor for poor community integration (5, 11), whereas one study reported that younger patients were at higher risk for poor community integration (6).
Most studies of community integration following TBI have methodological weaknesses. A majority of studies used a limited follow-up of 1 year (7–11, 13). The 2 studies that used longer follow-up periods had retrospective designs (5, 6). Only one study had a follow-up of 3–4 years and used a prospective design; however, the sample size was small (14). As a consequence, conclusions on determinants of community integration are limited. It is also unclear whether outcome following TBI stabilizes one year post-injury or whether community participation levels change over time. Hammond et al. (15) found that, although the majority of patients remained stable during years 1–5 post-injury, some made dramatic gains, whereas a minority declined. In contrast, a study by Sander et al. (14) showed no changes in mean community integration between the first and third or fourth year. In a second study Sander et al. (16) found no significant changes after discharge from a post-acute rehabilitation programme. However, they stated that CIQ scores can fluctuate over time in individual cases (16). Therefore, the present study was conducted as a prospective cohort study measuring community integration at multiple time points post-injury in comparison with the pre-injury level of community integration. It was aimed: (i) to evaluate the course of participation after moderate to severe TBI until 36 months post-injury; and (ii) to identify determinants of community integration at 36 months post-injury.
METHODS
Procedure
The study consecutively enrolled 119 patients with TBI between January 1999 and April 2004 at 3 Dutch acute care hospitals which were all level-1 trauma centres: Erasmus Medical Centre, Rotterdam (January 1999 to April 2004); Medical Centre Haaglanden, The Hague (January 2003 to February 2004); and University Medical Centre Utrecht, Utrecht (April 2003 to February 2004) (17). All study centres served as treatment centres for acute hospital care for all patients with moderate to severe TBI within their regions. Patients were treated in accordance with the European Brain Injury Consortium guidelines (18). In the Netherlands patients are discharged from the acute care hospitals to their homes (with or without outpatient rehabilitation), inpatient rehabilitation, or a nursing home (19).
Upon admission, patients with acute TBI or family members received verbal and written information about the study and were asked if they were willing to participate. When possible, patients gave informed consent. Otherwise, a family member gave informed consent and patients were asked to give consent at a later time. The medical ethics committee of Erasmus MC approved this study.
Baseline measurements were collected at hospital admission and patients were followed prospectively at 3, 6, 12, 18, 24, and 36 months post-injury. Two study psychologists collected data using structured interviews at the patients’ homes or at the rehabilitation centre or nursing home where the patient resided. If a patient interview was not possible, a family member or professional caregiver was interviewed.
Patients
Inclusion criteria were: (i) admission to a hospital for moderate (Glasgow Coma Scale (GCS) (20) of 9–13) or severe (GCS of 3–8) TBI due to a blunt or penetrating trauma. We classified patients with a GCS of 13 as moderate TBI, according to a study (21) that showed that patients with a GCS of 13 have similar complications, mostly due to intracranial haematomas, as patients with a GCS of 9–12; (ii) aged 16–67 years; and (iii) survival until discharge from the acute care hospital. Exclusion criteria were: (i) insufficient knowledge of the Dutch or English language to participate in the study; or (ii) serious pre-traumatic neurological, oncological, or systemic impairments (e.g. spinal cord injury, psychiatric disorder, cancer) that may interfere with TBI-related disability assessment.
Measures
Community integration. Community integration was assessed using the CIQ, which is designed specifically to assess issues affecting patients with TBI (3, 22). The survey consists of 15 questions about how certain activities are usually performed (alone, with another person, or by someone else), or how frequently activities are performed. Total scores vary from 0 to 29, with higher scores indicating better community integration. The CIQ addresses 3 domains: home integration (range 0–10), social integration (range 0–12), and productivity (0–7). The reliability and validity of the CIQ has been well established (3, 23–27). The CIQ scores obtained from family members and patients were statistically similar (28), there appeared to be no floor or ceiling effects (27). The CIQ was designed to assess community integration in patients living at home; therefore, the CIQ was not assessed at times that patients were admitted to inpatient rehabilitation or a nursing home after discharge from the acute care hospital, but only at time-points when patients lived in their homes. In contrast, data on independent variables were collected at time-points that patients resided in a rehabilitation centre or nursing home.
Independent variables. Potential sociodemographic and clinical determinants were identified by reviewing the published literature. Sociodemographic characteristics assessed included age in years, sex, pre-injury residence (alone vs with others), nationality (Dutch vs other nationality), pre-injury education level (secondary vs post-secondary education), and pre-injury work status (employed vs not employed). Pre-injury community integration levels were assessed retrospectively. Clinical characteristics assessed included lowest GCS score within 24 h of injury, cause of injury (motor vehicle accident vs other cause), length of stay in hospital (in days), hospital discharge destination (home vs a inpatient rehabilitation or a nursing home), and computed tomography (CT) results (normal vs abnormal). Presence or absence of hypoxia (PaO2 ≤ 8; SaO2 ≤ 90%), hypotension (systolic blood pressure ≤ 90 mmHg), and hypothermia (≤ 35°C) at admission was noted; a clinical diagnosis was also considered sufficient evidence of these conditions.
Post-acute functional measures included the Barthel Index (BI) (29) and the Functional Independence Measure plus Functional Assessment Measure (FIM+FAM) (30) measured at time of discharge from the acute care hospital. The BI, which has good reliability and validity (31), consists of 10 items on activities of daily living (e.g. bowel and bladder status, grooming, dressing, and bathing) each with 2 or 4 response categories (0–3 points). Total scores range from 0 (severely restricted) to 20 (no restrictions). The FIM+FAM, which has good reliability and validity (32–35), consists of 30 items that are evaluated on a 7-point scale (completely independent to totally dependent). The FIM+FAM evaluates motor and cognitive functioning with respect to self-care, sphincter control, transfers, locomotion, communication, psychosocial adjustment, and cognitive functioning. The FIM+FAM motor scale ranges from 16 (totally dependent) to 112 (totally independent) and the FIM+FAM cognitive scale ranges from 14 (totally dependent) to 98 (totally independent).
Statistical analysis
Descriptive analyses were performed using the Statistical Package for the Social Sciences (SPSS), version 12.0.1. Baseline characteristics for patients followed-up and not followed-up at 36 months post-injury were compared using the Mann-Whitney U test for continuous variables and χ2 test for categorical variables.
To determine whether the course changed over time for home integration, social integration, productivity, and total CIQ, a repeated measures analysis of variance (ANOVA) was performed using the PROC MIXED procedure in SAS 8.2. The advantage of this procedure is that it does not require complete follow-up data. Likelihood methods allow for missing data with this procedure. For all patients, time was included as a categorical variable in the model to test changes over time.
To identify possible predictors of total CIQ score at 36 months, we first tested all independent variables for bivariate relationships using SPSS 16.0.1. Bivariate relationships between community integration and independent variables were tested with Spearman’s correlations for continuous variables and with t-tests for dichotomous variables. Because of the small sample size and relatively large number of independent variables, we selected variables only with p < 0.10 for the multivariate analysis. p < 0.05 (2-sided) was chosen as the level of significance for the multivariate analysis.
RESULTS
Population
Table I presents baseline characteristics, post-acute functional level, and pre-injury CIQ for the study participants (n = 119). The mean age was 34 years; the male to female ratio was 3:1; most patients were of Dutch nationality; most patients lived with a partner or parent; mean GCS score was 7.1; and 94% had an abnormal computed tomography (CT) scan. The BI score at discharge from hospital was 15. The mean FIM+FAM motor score at discharge from hospital was 87 and the mean FIM+FAM cognitive score at discharge from hospital was 76. The mean pre-injury CIQ score was 19.3.
| Table I. Characteristics of patients with moderate to severe traumatic brain injury (n = 119) |
| Patient characteristics | |
| Age, years, mean (SD) | 34 (13.2) |
| Gender, men/women, n | 86/33 |
| Dutch nationality, n (%) | 111 (93) |
| Lived alone pre-injury, n (%)* | 17 (14) |
| Low pre-injury education level (secondary education), n (%)* | 58 (50) |
| Employed pre-injury, n (%)* | 93 (80) |
| Pre-injury home integration, mean (SD)* | 4.9 (3.3) |
| Pre-injury social integration, mean (SD)* | 8.9 (2.1) |
| Pre-injury productivity, mean (SD)* | 5.7 (1.3) |
| Pre-injury total CIQ, mean (SD)* | 19.3 (4.3) |
| Motor vehicle accident cause of injury, n (%)* | 85 (73) |
| Lowest GCS score in the first 24 h, mean (SD) | 7.1 (3.0) |
| Length of hospital stay, days, median (range) | 32 (4–173) |
| Hospital discharge destination to inpatient rehabilitation or a nursing home, n (%) | 62 (52) |
| Abnormal CT pattern, n (%) | 97 (94) |
| Hypoxia present, n (%) * | 32 (32) |
| Hypotension present, n (%) * | 12 (12) |
| Hypothermia present, n (%) * | 16 (21) |
| FIM+FAM motor, mean (SD)* | 87 (25.0) |
| FIM+FAM cognitive, mean (SD)* | 76 (20.3) |
| Barthel Index, mean (SD)* | 15 (6.3) |
| *Data missing for: living status (n = 1), education level (n = 4), pre-injury work status (n = 3), pre-injury home integration (n = 27), pre-injury social integration (n = 28), pre-injury productivity (n = 27), pre-injury total CIQ (n = 28), cause of injury (n = 2), CT pattern (n = 16), presence of hypoxia (n = 20), presence of hypotension (n = 21), presence of hypothermia (n = 44), FIM+FAM motor (n = 21), FIM+FAM cognitive (n = 23), Barthel Index (n = 25). SD: standard deviation; CT: computed tomography; CIQ: Community Integration Questionnaire; GCS: Glasgow Coma Scale; FIM+FAM: Functional Independence Measure plus Functional Assessment Measure. |
CIQ measurements were available for 91 patients pre-injury, 52 patients at 3 months, 65 patients at 6 months, 82 patients at 12 months, 85 patients at 18 months, 84 patients at 24 months, and 94 patients at 36 months. At the 36-month follow-up, 25 measurements were unavailable because 3 patients had died, 16 were lost to follow-up, 4 were residing in a nursing home, and 2 were not assessed due to logistical problems. Patients who completed 36-monhts follow-up had a higher education level (p = 0.020), were more likely to be employed prior to injury (p = 0.017), and were more likely to have an episode of hypoxia (p = 0.017), than the patients who did not complete the final follow-up (n = 25). There were no other significant differences between patients followed-up and not followed up at 36 months post-injury.
Community integration
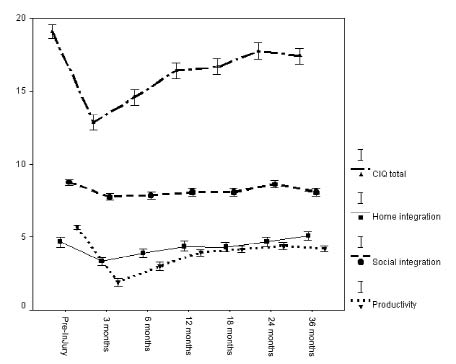
Fig. 1 shows the course of home integration, social integration, productivity, and total CIQ from pre-injury to 36 months post-injury. Time was significantly associated with home integration (p < 0.001), social integration (p < 0.001), productivity (p < 0.001), and total CIQ (p < 0.001).
Fig. 1. The course of the total Community Integration Questionnaire (CIQ), home integration, social integration, and productivity scores from pre-injury to 36 months post-injury. Data presented are estimated means (± standard error of the mean (SEM)) as calculated with repeated measurements analysis of variance.
Regarding home integration, 558 out of a potential 833 scores (119 patients × 7 time-points) were available for ANOVA. Compared with pre-injury, the mean home integration score decreased at 3 months post-injury (decrease 1.30 points, standard error (SE) = 0.33, p < 0.001). At 6 months post-injury, home integration scores improved, but the mean level remained below the mean pre-injury level (p = 0.019). At 12 months, mean home integration scores attained pre-injury levels; a modest increase beyond pre-injury levels occurred during the subsequent 24 months (p = 0.014).
For social integration, 555 scores were available for ANOVA. Compared with pre-injury, the mean social integration score decreased 3 months post-injury (decrease 1.00 points, SE = 0.23, p < 0.001). The mean social integration score stabilized at the 3-month level, experienced a small increase at 24 months post-injury, but remained low compared with pre-injury levels at the 36-month follow-up (difference 0.69 points, SE = 0.21, p = 0.002).
For productivity, 558 scores were available for ANOVA. Compared with pre-injury, the mean productivity score decreased 3 months post-injury (decrease 3.69 points, SE = 0.28, p < 0.001). Subsequently, the mean productivity level increased at 6 and 12 months post-injury, stabilized, then showed a small increase at 24 months post-injury. At 36 months post-injury, the mean productivity level remained significantly low compared with the mean pre-injury level (difference 1.45 points, SE = 0.20, p < 0.001).
For total CIQ, 553 scores were available for ANOVA. Compared with the mean pre-injury level, the mean community integration score decreased 3 months post-injury (decrease 6.20 points, SE = 0.50, p < 0.001). Subsequently, the mean community integration scores significantly increased at 6 and 12 months, then stabilized. Increased mean levels of community integration were noted at 24 months and remained stable at 36 months.
Determinants of community integration
Table II presents bivariate relationships between independent variables and 36-month post-injury CIQ scores. The following patients had lower community integration scores 36 months post-injury: males, older patients, those living with others pre-injury, those with longer hospital stays, those with abnormal CT scans, those with lower BI scores (more dependence), those with lower FIM+FAM motor scores (more dependence), those with lower FIM+FAM cognitive scores (more dependence), those with low pre-injury CIQ scores, and those who were discharged to inpatient rehabilitation or a nursing home. As expected, the BI correlate strongly with the FIM+FAM motor scores (Spearman’s rho = 0.89, p < 0.001), and therefore could not be entered simultaneously into the multivariate analysis. We chose the BI score for the multivariate model because the questionnaire requires less time to administer, and therefore would be more valuable in clinical practice.
| Table II. Bivariate linear regression analyses for the Community Integration Questionnaire (CIQ) total scores at 36 months post-injury (n = 94) |
| Predictive variable | Bivariate analysis |
| Mean (SEM) | p-value |
| Sociodemographic characteristics |
| Age, years* | –0.32 | < 0.002 |
| Sex | | |
| Male | 16.97 (0.68) | 0.012 |
| Female | 19.50 (0.71) | |
| Nationality | | |
| Dutch | 17.82 (0.54) | 0.580 |
| Other | 16.50 (3.05) | |
| Pre-injury living status | | |
| Alone | 21.00 (1.06) | 0.018 |
| With parent or partner | 17.27 (0.57) | |
| Pre-injury education level | | |
| Secondary | 16.96 (0.78) | 0.167 |
| Post-secondary | 18.45 (0.73) | |
| Pre-injury work status | | |
| Employed | 17.84 (0.61) | 0.596 |
| Unemployed | 17.04 (0.93) | |
| Pre-injury CIQ scores†* | 0.54 | < 0.001 |
| Clinical characteristics |
| Cause of injury | | |
| Motor vehicle accident | 17.65 (0.61) | 0.945 |
| Other | 17.74 (1.09) | |
| Lowest GCS score in the first 24 h* | 0.054 | 0.605 |
| Length of hospital stay, days* | –0.19 | 0.062 |
| Hospital discharge destination | | |
| Home | 19.16 (0.61) | 0.009 |
| Inpatient rehabilitation or nursing home | 16.45 (0.82) | |
| Computed tomography | | |
| Abnormal | 17.50 (0.55) | 0.007 |
| Normal | 23.55 (1.56) | |
| Hypoxia | | |
| Present | 18.69 (1.04) | 0.311 |
| Absent | 17.51 (0.65) | |
| Hypotension | | |
| Present | 17.77 (1.78) | 0.923 |
| Absent | 17.94 (0.60) | |
| Hypothermia | | |
| Present | 17.04 (1.66) | 0.651 |
| Absent | 17.77 (0.704) | |
| Post-acute functioning |
| FIM+FAM motor at discharge from hospital†* | 0.37 | 0.001 |
| FIM+FAM cognitive at discharge from hospital†* | 0.32 | 0.005 |
| Barthel Index at discharge from hospital†* | 0.39 | 0.001 |
| *Results for continuous data calculated by Spearman’s correlation. †CIQ pre-injury (n = 83); FIM+FAM motor (n = 78); FIM+FAM cognitive (n = 76); Barthel Index (n = 74). SEM: standard error of mean; GCS: Glasgow Coma Scale; FIM+FAM: Functional Independence Measure plus Functional Assessment Measure. |
Table III shows the multivariate results for community integration at 36 months post-injury. Age, BI score, hospital discharge destination, and pre-injury CIQ score were the major determinants of community integration and explained 60% of the variance (F(4,63) = 23.30, p< 0.001). The addition of age, BI score, and hospital discharge destination to the model explained more variance than the pre-injury CIQ score alone (which explained 31% of the variance). Older age, a lower BI score (more dependence), discharge from hospital to inpatient rehabilitation or a nursing home, and lower pre-injury CIQ score predicted lower levels of community integration. Adding other independent variables to this model did not reveal other significant determinants. When the FIM+FAM motor score was entered into the model in place of the BI, a model with similar predictive value was found (F(4,65) = 22.8, p < 0.001, R2 = 59%): age, hospital discharge destination, pre-injury CIQ score and FIM+FAM motor score determined community integration.
| Table III. Multivariate model for predicting community integration at 36 months post-injury. Results are presented as regression coefficients (β) with 95% confidence intervals (CI) and p-values |
| Predictive variable | β | 95% CI (β) | p-value |
| Intercept | 8.39 | 1.63 (15.15) | |
| Age, years | –0.12 | –0.19 (–0.05) | 0.001 |
| Barthel Index | 0.25 | 0.08 (0.43) | 0.006 |
| Hospital discharge destination (to inpatient rehabilitation or a nursing home) | –2.10 | –4.05 (–0.15) | 0.036 |
| Pre-injury CIQ score | 0.54 | 0.34 (0.74) | < 0.001 |
| CIQ: Community Integration Questionnaire. |
DISCUSSION
In this prospective study we evaluated the course of community integration from pre-injury to 36 months post-injury for patients with moderate to severe TBI. Furthermore, we identified determinants of community integration at 36 months post-injury. All CIQ subscales initially declined following injury, but slowly increased over time. Maximal improvement occurred during the first year following injury and several domains showed small improvements between years 1 and 3 post-injury. However, most domains did not reach pre-injury levels. Some increases were transient and non-sustained at 36 months.
Because there are no standardized normal values for CIQ, some researchers (36, 37) have used a non-disabled sample as a referent to interpret findings in patients with TBI (22, 23, 38). Others have used retrospectively collected pre-injury CIQ scores (12). Pre-injury CIQ scores and non-disabled CIQ scores range from 17.4 to 20.5, whereas post-injury TBI patient CIQ scores range from 13.0 to 17.7 (3, 12, 22, 37). Our findings for pre-injury and post-injury CIQ scores were consistent with these previously reported ranges. Our finding that participation modestly increased one year following TBI contrasts with a longitudinal study by Sander et al. (14), which showed no changes in community integration between the first and third or fourth year (14). Differences in study populations and power may explain this difference.
Pre-injury community integration, age, hospital discharge destination, and the post-acute BI score were the major determinants of community integration at 36 months post-injury in this study. Our finding that older persons had lower community integration levels than younger persons is consistent with other studies (5, 10, 11, 13). This may be partly explained by the observation that most persons reduce their activity patterns as they age. Another possibility is that older patients have a poorer recovery compared with younger patients, which leads to participation restrictions. The hospital discharge destination was a determinant in this study. The discharge destination can reflect poorer functioning, which was also related to community integration in other studies (5, 6). The post-acute BI score was a significant predictor of community integration in this study. Previous research indicates that post-acute functional factors predict several aspects of community integration at one year post-injury (14, 39) but not at 2 or 3–4 years post-injury (14). Post-acute measures of levels of functioning have also predicted long-term disability and productivity level (2).
In contrast to several other researchers (7, 8, 11, 13), we found no prognostic value for pre-injury work status. However, 80% of our study participants were employed prior to injury; this percentage is much higher compared with other studies. It is possible that the effect of pre-injury employment could not be detected due to small sample variability.
Pre-injury education level and nationality were not predictive in this study, although they were found to be predictors in other studies (8, 10–12). No prognostic value was found for the GCS score in this study of patients with moderate to severe TBI. However, the GCS has predicted community integration in a study including also patients with mild TBI (7). An abnormal CT scan showed a bivariate relationship with community integration, whereas cause of injury, presence of hypoxia, presence of hypotension and presence of hypothermia did not.
Multivariate analysis did not show that any of these clinical characteristics were significant determinants of community integration. According to the International Classification of Functioning, Disability and Health (ICF) (40) published by the World Health Organization, activities and participation restrictions are determined by many factors. These include disease factors such as injury severity, as well as personal factors and environmental factors, which are especially useful in predicting long-term outcome. Although most clinical characteristics were predictive for short-term outcome (i.e. up to 6 months post-injury), they may be less important than personal or environmental factors (e.g. coping style, social environment, and depression) in predicting long-term outcome. Others have concluded that injury severity may be a less important predictor than pre-morbid status and 6-month post-injury cognitive status (14, 39).
Pre-injury community integration level, age, hospital discharge destination, and the post-acute BI can assist clinicians in identifying which patients are at risk for lower community integration and which might benefit from additional care or long-term facility placement. This information would also assist clinicians in providing more detailed information regarding functional prognosis. In our study sample, patients with low pre-injury community integration, older age, discharged from hospital to inpatient rehabilitation or a nursing home, or a lower BI were at risk for more long-term community integration problems, than patients without these characteristics.
This study has some limitations. Although the CIQ is considered sensitive for measuring differences between diagnoses (23), it is not yet evident whether the CIQ is sensitive to changes over time (41). Furthermore, standardized normal values for the CIQ do not exist. Previous studies assessing the CIQ cross-sectionally presented challenges in determining whether statistically significant changes were clinically relevant. Although drawing conclusions is difficult, the decline in community integration at 3 months post-injury was relatively large. Comparisons of mean pre-injury scores with mean scores at 3 months post-injury, showed a decrease of 6.20 points for the total CIQ (1.30 points for home integration, 1.00 points for social integration, and 3.69 points for productivity). Especially for productivity and total CIQ scores these changes seem clinically relevant. Future research on the psychometric properties for sensitivity to change and the development of normative values will provide more information about the interpretation of such results. Furthermore, the CIQ was designed to measure the level of participation in the community. Therefore, patients living in a nursing home at 36 months post-injury were not assessed for community integration and results can only be generalized to patients living at home.
Additionally, there were differences in baseline characteristics between patients followed-up and not followed-up. Loss to follow-up is a common problem in both prospective cohort studies and TBI studies and can lead to selection bias. Socioeconomically disadvantaged patients are more likely to be lost to follow-up, whereas more severely injured patients have less loss to follow-up (41). We found a similar pattern, in that patients who were not followed-up had lower education levels, were less likely to be employed pre-injury, and were less likely to experience hypoxia. The loss to follow-up might have resulted in selection bias, and therefore generalizations should be made cautiously.
Finally, our sample size was relatively small; therefore, some determinants may have been undetectable. However, we believe the sample was representative for a normal population of patients with moderate and severe TBI, as it was procedure that all patients with moderate and severe TBI were referred to the 3 hospitals from which we included patients.
In conclusion, patients with TBI experienced significant declines in community integration following TBI, but slowly improved for most domains over time. Although maximal improvement occurred during the first year post-injury, improvements for most domains also occurred beyond one year. Lower pre-injury community integration, older age, a hospital discharge destination to inpatient rehabilitation or a nursing home, or lower BI scores were associated with lower community integration, than patients without these characteristics. Eventually, these determinants may be useful tools to determine which patients are at risk for lower community integration and would benefit from additional care or long-term facility placement. Norm values on participation specified for age categories and the relation of community integration on quality of life and use of healthcare resources in patients with TBI are important topics for future research.
ACKNOWLEDGEMENTS
This study was performed as part of the “Long-term prognosis of functional outcome in neurological disorders”, the Department of Rehabilitation Medicine, VU Medical Centre, Amsterdam, and supported by the Netherlands Organisation for Health Research and Development (project: 1435.0020).
This manuscript was written on behalf of the FuPro-II study group: G. J. Lankhorst, J. Dekker, A. J. Dallmeijer, M. J. IJzerman, H. Beckerman, V. de Groot: VU University Medical Centre Amsterdam (project coordination); E. Lindeman, G. Kwakkel, I. G. L. van de Port: University Medical Centre Utrecht/Rehabilitation Centre De Hoogstraat, Utrecht; H. J. Stam, A. H. P. Willemse-van Son: Erasmus Medical Centre, Rotterdam; G. M. Ribbers: Rehabilitation Centre Rijndam, Rotterdam; G. A. M. van den Bos: Department of Social Medicine, Academic Medical Centre, University of Amsterdam, Amsterdam.
REFERENCES