OBJECTIVE: To demonstrate the muscle strength characteristics of shoulder internal and external rotators and the effects of isokinetic exercise on muscle activity in patients with adhesive capsulitis.
DESIGN: Cohort study with control subjects.
PARTICIPANTS: Eight patients with adhesive capsulitis and 8 controls.
METHODS: Maximal isometric and isokinetic strength tests of shoulder internal and external rotators in the scapular plane were carried out. Muscle activities of the rotators were recorded in resting and during maximal isometrics. Muscle strength variables (peak torque, total work and power) and myoelectric variables (resting root-mean-square amplitude pre- and post-tests and the external-internal rotator co-activity in resting and during isometric contractions) were recorded. A mixed repeated-measure analysis of variance test was used to examine the within-group and between-group differences.
RESULTS: For affected shoulders, smaller isometric average torque of internal rotators and high-speed peak torque, total work and power of external rotator were observed. The external/internal rotator ratio of peak torque in high-speed testing also exhibited significant decrease. The myoelectric variables showed no significant changes.
CONCLUSION: High-speed external rotator strength and isometric internal rotator strength of the affected shoulders were decreased significantly. Isokinetic exercise may not increase the resting muscle activities and co-activity. These results provide a reference in planning muscle strengthening programmes and goals for these patients.
Key words: shoulder, rotator cuff, exercise, muscle strength, electromyography.
J Rehabil Med 2009; 41: 563–568
Correspondence address: Hsiu-Chen Lin, Department of Physical Therapy, China Medical University, No.91 Hsueh-Shih Road, Taichung TW-40402, Taiwan, ROC. E-mail: hclin@mail.cmu.edu.tw
Submitted June 30, 2008; accepted March 3, 2009
INTRODUCTION
Adhesive capsulitis, also known as frozen shoulder, is one of the most frequent pathologies in the middle-aged population. The aetiology of frozen shoulder is unclear, possibly involving a non-specific chronic inflammatory reaction of subsynovial tissue and resulting in capsular and synovial thickening, but the problem affects the function of the glenohumeral joint (1–3). The onset of frozen shoulder is usually gradual and idiopathic, but it may also be acute and associated with a history of minor injury to the shoulder joint (1, 4, 5). Time course of the frozen shoulder is divided into 3 stages: the painful stage, the stiffening stage, and the thawing stage (3). In the painful stage, gradual onset of shoulder pain lasts from weeks to months. Pain, which can be severe, may cause pronounced sleep disturbance (1, 2, 6). The stiffening stage is characterized by progressive loss of active and passive ranges of motion (ROM) that may last up to one year (5). Most patients lose ROM in glenohumeral external rotation, abduction, and internal rotation during this stage, considered as the “capsular pattern” (6, 7). The final, thawing phase constitutes a period of gradual motion improvement. Once in this stage, patients may require up to 9 months to regain functional motion.
In clinics, physicians usually apply acupuncture, arthroscopic release or manipulation under anaesthesia to relieve the pain or loosen the joint (8–11). Physical therapists augment their motor function using joint mobilization techniques, stretching and muscle strengthening exercises (12, 13). Most of these treatments emphasize loosening the joint in order to restore movement (13). The muscle strengthening exercise is usually integrated in the treatment programme to maintain the regained ROM, prevent disuse atrophy and restore muscle function (8, 12–15). Recommendations for frozen shoulder rehabilitation also included the restoration of a good articular surface kinematics and correction of the muscle and movement imbalances as treatment goals (12, 13). As the most mobile joint of the body, articular surface movements of the shoulder rely on the co-ordinated control of the surrounding muscles. Any impaired muscular performance may influence shoulder movements and then contribute to joint dysfunction. Therefore, the frequently observed pain-induced muscle spasm and muscle weakness around the affected shoulder may also cause pain and restricted movements in individuals with adhesive capsulitis (8). Isometric and isokinetic muscle strengths of shoulder rotators have been reported to be influenced by other shoulder conditions (16–19). However, to the authors’ best knowledge, the alterations of muscular performance in patients with adhesive capsulitis have not been reported.
To explore muscle function associated with shoulder movements, muscle strength test and electromyographic examination may be used. An isokinetic machine is proved to be reliable and is frequently used in clinics to investigate muscle strength (20). The movement restriction occurs primarily in shoulder external and internal rotation in patients with adhesive capsulitis. Therefore, the priority for muscle strength test would be shoulder rotators. To further understand the balance of agonist and antagonist muscle strength, normative values of agonist/antagonist shoulder strength ratios have been reported (21), but no literature has documented this information in patients with adhesive capsulitis. For these patients, muscle spasm is frequently observed and defined as involuntary hyperactivity of a muscle, and thus may result in increased co-contraction of the agonist and antagonist. Through electromyographic examination, muscle spasm may be evaluated by detecting the level of myoelectric activities in resting status and also the muscle co-activity, which is defined as the level of simultaneous activation in the agonist and antagonist. Muscle co-activity played an important role in stabilizing the controlled joint and guiding the articular surface movements; however, it may also reduce movement accuracy in individuals with muscular incoordination (22). To better understand the alterations in muscular performance in patients with adhesive capsulitis, this study aimed to demonstrate the muscle strength characteristics of the shoulder external rotators (ER) and internal rotators (IR), and to investigate the effects of isokinetic testing on the muscle activities of shoulder rotators.
METHODS
Participants
Eight participants with adhesive capsulitis were enrolled from the Department of Physical Medicine and Rehabilitation, China Medical University Hospital, as the adhesive capsulitis (AC) group. The patients were diagnosed in the stiffening stage of frozen shoulder by a physiatrist and this was confirmed with arthrography, which ruled out those with rotator cuff tear, calcific deposits and cardiac disease-related shoulder pain. The restricted movement occurred in all directions for one shoulder, but with more than 50° of total ROM in external and internal rotation, allowing them to perform isokinetic strength tests. They had had pain in one shoulder for at least one month (range 1–6 months) and had not had night pain in the week prior to the test. The gender- and age-matched control group consisted of 8 participants with no history of upper extremity injury. Informed consent was obtained from each participant before the tests. The participants' demographics are shown in Table I.
| Table I. Participant demographics (mean (standard deviation)) |
| | Control group | Adhesive capsulitis group | |
| Gender, men/women, n | 3/5 | 3/5 | |
| Weight, kg | 67.6 (10.5) | 61.8 (8.9) | |
| Age, years | 47.2 (6.3) | 49.2 (9.5) | |
| | | Affected side | Non-affected side |
| Range of motion, degrees* | | | |
| External rotation [range] | 89.4 (15.3) [5–105] | 59.4 (20.4) [35–90] | 77.5 (14.6) [50–95] |
| Internal rotation [range] | 66.3 (15.9) [45–90] | 29.4 (17.0) [5–60] | 63.1 (16.9) [40–90] |
| *Measured with participant supine and shoulder abduction 90°. |
Instrumentation and experimental protocol
The isokinetic dynamometer (KinCom 500H, Chattanooga, USA) and the surface electromyography (EMG) system (MA-300, Motion Lab, USA) were used to measure muscle strength and myoelectric data. These data were collected simultaneously through an analogue-to-digital card (DaqCard-700, National Instruments, USA) and recorded into a laptop computer. Before the electromyographic measurement, the skin was cleaned with alcohol to reduce skin impedance. The pre-amplified surface electrodes (MA-411, Motion Lab, USA) were placed onto the following muscles around both shoulders: supraspinatus (supraspinous fossa, just above middle of scapular spine); infraspinatus (infraspinous fossa, 2 finger-breadths below the midline of the scapular spine) and teres major (scapular lateral border, 3 finger-breadths above the inferior angle) (23). The raw surface EMG (sEMG) data were visually checked for electrocardiac or other significant artefacts and the electrodes were rearranged if contaminated.
Before the strength tests, the participant was first placed seated, with the trunk well stabilized with his or her shoulder in the scapular plane (at 90° of abduction and 30° of horizontal adduction), elbow at 90° of flexion and forearm in the neutral position (24). After a 5-min warm-up, a 5-sec EMG data of the tested muscles in resting status was collected before the muscle strength tests. Another resting EMG would be recorded after the muscle strength tests. During the isometric strength tests, participants were asked to perform maximal contractions, each for 5 sec at 2 tested angles (0° (neutral position) and –15° (lengthening position for the tested muscle), while the myoelectric activities of shoulder rotators were recorded simultaneously. Afterwards, the isokinetic tests including 5 maximal concentric then eccentric contractions at high-speed (180°/sec) and low-speed (60°/sec) of shoulder internal and external rotation in the scapular plane. The movement range was set in the pain-free 50° of shoulder rotation around neutral. The non-affected shoulder was tested first to allow familiarity of testing procedures. The order of which shoulder was tested for the control participants was randomly assigned. During testing, no participants complained of pain or discomfort. Isometric testing variables (average torque) and the maximum isokinetic testing variables out of 5 contraction trials (peak torque, total work, and power) were obtained for each strength test. The ratios of peak torques of ER and IR (ER/IR ratio) for high-speed, low-speed isokinetic testing and isometric testing were then calculated.
Data reduction
All strength variables were normalized by the individual’s body weight. The sEMG data were processed using a self-written programme in MATLAB (Mathworks, Massachusetts, USA). The raw sEMG data were full-wave rectified and Butterworth band-stop filtered at 60 Hz to reduce the effects from AC power line. To investigate the exercise effect on muscle spasm, the resting root-mean-square (rRMS) of the filtered sEMG before and after the maximal isometric and isokinetic contractions was calculated. In addition, muscle co-activity of ER and IR was calculated using the activation level of each muscle, obtained from the filtered sEMG normalized by the maximum of voluntary isometric contractions, and defined as: where EMGS represents the smaller activation, while EMGL represented the larger activation of the 2 (25, 26). The activation ratio of agonist and antagonist was then multiplied by the sum of the activity found in these 2 muscles. This weighted product may provide an insight regarding the co-activation of paired muscles. High co-activation values represented a high level of simultaneous activation of both muscles, whereas low co-activation values represent either low-level of simultaneous activation of both muscles or high-level activation of one muscle against low-level activation of the paired muscle. Low co-activation values indicated more selective activation of muscles, whereas high co-activation values indicated more generalized muscle activation (25, 26). In this study, co-activation was calculated for the pair of supraspinatus-teres major, and infraspinatus-teres major in order to represent muscle spasm in resting and during isometric contractions. Myoelectric variables (rRMS and muscle co-activity) were obtained using the customized MATLAB programme (Mathworks).
Statistical analysis
A mixed repeated-measure analysis of variance (RM-ANOVA) test with one between-subject factor (between AC and control groups) and one within-subjects factor (between the affected and non-affected shoulder of the AC group and the right and left side of control group) were used to analyse the main effects and the interactions for each of the strength and myoelectric variables. The statistical significance was set at 0.05. We found significant interaction between these 2 factors, so the comparisons using paired t-tests of separate groups were performed first, and then the comparisons of the control group with the non-affected or affected shoulder of the AC group using an independent t-test. All statistical comparisons were performed using SPSS statistical software (SPSS Inc., Chicago, IL, USA).
RESULTS
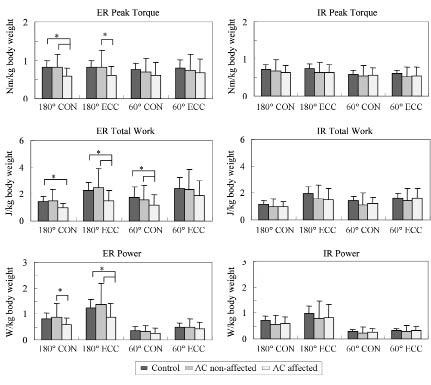
The ROM of the non-affected shoulder in the AC group showed no statistical difference compared with the control group. However, the restricted ROM of the affected shoulder and decreased functional level of daily activities in the AC group were observed (Table I). In isokinetic testing, we found no significant difference in strength variables between the right and left sides in the control group. The mean values of these variables of both sides in the control group were therefore used for between-group comparisons. For the AC group, there was no significant difference in the IR isokinetic varibales, either in between-side or in between-group comparisons. In contrast to shoulder IR, significant differences and interaction were found in the peak torque, total work, and power of shoulder ER in high-speed concentric and eccentric testing, also in the ER total work in low-speed concentric testing. For between-side comparison in the AC group, the ER of the affected shoulder showed significant decreases in peak torque, total work and power in high-speed testing (p < 0.05). Similar results were found in the between-group comparison of the affected shoulder with the control group. In low-speed testing, ER total work of the affected shoulder was also significantly smaller compared with both the non-affected shoulder and the control group (Fig. 1).
Fig. 1. Comparison of the isokinetic muscle characteristics in adhesive capsulitis (AC) and control groups. *Indicates statistical significance of p < 0.05. CON: concentric contraction; ECC: eccentric contraction; 180°: isokinetic speed at 180°/sec; 60°: isokinetic speed at 60°/sec; ER: external rotators; IR: internal rotators.
In isometric testing, IR average torque of the affected shoulder in the AC group was significantly smaller compared with the control group in both neutral and lengthening positions, while ER strength showed trends of decrease (p = 0.055 for 0° position and p = 0.058 for –15° position) (Table II). The ER/IR ratios were not different in between-group and between-side comparisons, except that significantly smaller values were observed in the affected side of the AC group in the high-speed testing compared with those of the control group (Table III). In sEMG measurements, the muscle co-activities of the ER-IR pairs in isometric muscle contractions or in resting condition showed no significant difference before and after the muscle strength tests, or in between-side and between-group comparisons (Fig. 2). Similar findings were also found in the comparison of rRMS (Table IV). Significant differences were found only in the infraspinatus and teres major of the left shoulder in the control group, with smaller RMS values after the strength tests compared with before.
| Table II. Isometric average torque (mean (standard deviation)) in the adhesive capsulitis and control groups |
| | Control group (Nm/kg bw) | Non-affected side (Nm/kg bw) | Affected side (Nm/kg bw) |
| Internal rotators |
| 0° | 1.67 (0.39) | 1.19 (0.92) | 0.94 (0.35)* |
| –15° | 1.71 (0.52) | 1.11 (0.59) | 0.85 (0.34)* |
| External rotators |
| 0° | 1.74 (0.59) | 1.19 (0.62) | 1.07 (0.70) |
| –15° | 1.7 (0.47) | 1.18 (0.68) | 1.08 (0.69) |
| *Indicates significant difference (p < 0.05) between affected side and control. Testing position at 0°: in neutral position of external and internal rotation; testing position at –15°: in slight lengthening position of the tested muscle. bw: Body weight. |
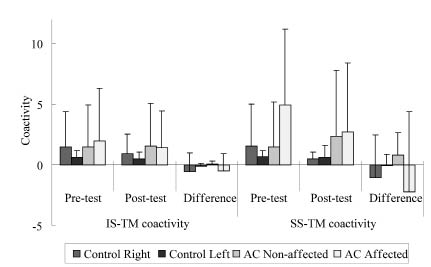
Fig. 2. Mean muscle co-activity in resting status before and after the muscle strength tests (pre- and post-test), and the changes between 2 measurements (difference). IS: infraspinatus; TM: teres major; SS: supraspinatus; AC: adhesive capsulitis.
| Table IV. Root-mean-square of resting muscle activation (mean (standard deviation)) before and after the muscle strength tests (pre- and post-test) |
| Muscles | Pre-test (mV) | Post-test (mV) | p-value |
| Control group | | | |
| Supraspinatus | | | |
| Left | 0.030 (0.029) | 0.030 (0.029) | 0.914 |
| Right | 0.096 (0.197) | 0.025 (0.030) | 0.272 |
| Infraspinatus | | | |
| Left | 0.025 (0.015) | 0.020 (0.013) | 0.030* |
| Right | 0.098 (0.193) | 0.021 (0.014) | 0.278 |
| Teres major | | | |
| Left | 0.029 (0.024) | 0.019 (0.015) | 0.040* |
| Right | 0.096 (0.192) | 0.022 (0.016) | 0.296 |
| Adhesive capsulitis group | | | |
| Supraspinatus | | | |
| Non-affected side | 0.049 (0.051) | 0.053 (0.052) | 0.695 |
| Affected side | 0.068 (0.072) | 0.070 (0.055) | 0.929 |
| Infraspinatus | | | |
| Non-affected side | 0.071 (0.153) | 0.070 (0.156) | 0.864 |
| Affected side | 0.082 (0.158) | 0.073 (0.159) | 0.208 |
| Teres major | | | |
| Non-affected side | 0.068 (0.144) | 0.068 (0.147) | 0.877 |
| Affected side | 0.069 (0.151) | 0.064 (0.150) | 0.143 |
| *Indicates significant difference (p < 0.05) between post-test and pre-test. |
DISCUSSION
This study aimed to investigate the characteristics of muscular performance of the shoulder rotators in patients with adhesive capsulitis. Muscle strength and muscle activities tests of the non-affected side of the AC group showed no significant difference compared with the control group. These results suggest that the non-affected side in these patients was not significantly affected with respect to muscle strength or muscular activation during resting or maximal contractions. Only approximately 15% of patients might develop bilateral disease (27). For the patients with unilateral shoulder involvement, however, the muscular performance in the non-affected shoulder may be considered a good reference of treatment goals during rehabilitation.
We found that the IR muscle strength of the affected shoulder in the AC group was altered only in the isometric testing (Table II). On the other hand, the ER muscle strength performances of the affected shoulder were significantly worse, especially in high-speed tests (Fig. 1). The muscle strength, and both fast twitch (FT) and slow twitch (ST) muscle fibre areas, decreased significantly after 5–6 weeks of immobilization (28). Generally, both types of fibres were affected approximately equally (28, 29); however, considerable and unpredictable variations with predominant influence on FT or ST fibres may affect muscle performance in different movement speeds. The decreased abilities to generate peak torque, total work and power could be a result of the limited range of shoulder motion, but could also be the reason to cause the restrained movement. Our study design could not determine the cause-effect relationship between the muscle strength and limited ROM in the patients with adhesive capsulitis. However, these deficits could hinder recovery significantly, since external rotation was usually the most limited movement for these patients. Therefore, the treatments should not focus only on resolving ROM limitation or pain, but also on the muscle strengthening programme. Based on our results, the rehabilitation programme for these patients should focus more on high-speed strength training for ER and isometric strength training for IR.
In the low-speed isokinetic strength test, ER total work in the affected shoulder, but not the peak torque or power, was significantly smaller compared with either the non-affected shoulder or the control group. These results suggest that these patients could produce maximal muscle strength in lower speed movements, but had decreased ability to retain that force output. To sustain the force output required muscular endurance, which can be measured by total work of the contraction. Therefore, a muscle endurance training programme of the shoulder external rotation in low-speed tasks should be recommended for these patients. Though it was not statistically significant, the average values of the ER strength variables for the affected side were smaller than those for the non-affected side. This was probably due to the small sample size, which was limited by the failure of our testing machine. In the retrospective power analysis, it showed that only with a subject number greater than 25 could statistical significance be reached.
Significantly smaller values of the ER/IR ratio were found in the affected sides of the AC group than those of the control group in high-speed testing (Table III). The explanation may be the decreased ER peak torques in the affected side of the AC group (Fig. 1). The values of ER/IR ratio of the control group in this study were greater than 1 (Table III), which meant the peak torques of ER were greater than those of IR. Hugh et al. (21) reported an average isometric ER/IR ratio of 0.74–0.78 for the corresponding age groups in the healthy population. This discrepancy could be due to different testing positions and tested angles (30, 31). The testing position for the present study was in the scapular plane, whereas it was in the frontal plane for the previous studies (21, 30). These results indicated that the scapular plane may be a position that favours the shoulder ER to generate relatively larger muscle force. In the previous study, the tested angle was 30º of shoulder external rotation, but neutral and –15° (lengthening) positions were adopted in the present study. Considering the length-tension property of muscle contraction, ER was shortened further and the less force output could be generated in the more external rotated position (31, 32). Together, our findings suggested that, to selectively strengthen shoulder ER, training around shoulder neutral rotation in the scapular plane should be adopted for these patients.
| Table III. External rotators/internal rotators strength ratio (mean (standard deviation)) in the adhesive capsulitis and control groups |
| | Control group | Non-affected side | Affected side |
| Speed 180°/sec | | | |
| Eccentric contraction | 1.51 (0.61) | 1.25 (0.27) | 0.94 (0.20)* |
| Concentric contraction | 1.69 (0.63) | 1.33 (0.31) | 0.99 (0.21)* |
| Speed 60°/sec | | | |
| Eccentric contraction | 1.27 (0.63) | 1.20 (0.35) | 1.06 (0.26) |
| Concentric contraction | 1.22 (0.61) | 1.44 (0.53) | 1.19 (0.21) |
| Speed 0°/sec | | | |
| Isometric contraction at 0° | 1.45 (0.57) | 1.42 (1.31) | 1.21 (0.68) |
| Isometric contraction at –15° | 1.29 (0.59) | 1.14 (0.56) | 1.41 (0.82) |
| *Indicates significant difference (p < 0.05) between affected side and control. Isometric at 0°: tested in neutral position; isometric at –15°: tested in slight lengthening position. |
Muscle spasm and capsular contracture are 2 potential pathologies of limited shoulder ROM in patients with adhesive capsulitis. The rRMS values, indicating the level of muscle spasm in the resting status, showed no significant changes in the AC group and slight decreases in the control group after the muscle strength tests (Table IV). This suggested that shoulder rotators were able to return to the relax status even after the maximal contractions. No significant differences were found in ER-IR co-activity between the strength tests or between sides and groups. However, tendencies of decreased co-activities of muscle ER-IR co-activity after maximal contractions and larger value in the affected shoulder in resting status can be observed (Fig. 2). A higher level of co-activity implied a more tightened joint, and may be one of the factors that compromised the shoulder rotators performance in these patients. The similar rRMS and co-activity values before and after the strength tests suggested that these exercises may not cause discomfort or increased muscle spasm. Thus, shoulder muscle strengthening exercises for these patients is encouraged. Further studies may focus on the optimal dosage of isokinetic exercises for patients with adhesive capsulitis.
In conclusion, the impairments in muscle performance could be quantified by isokinetic testing. The results of this study showed similar muscular performances in the non-affected shoulders of the patients with adhesive capsulitis and in the shoulders of control participants. In the affected shoulders, the external rotation muscle strength in the high-speed isokinetic testing and the internal rotation isometric strength were decreased significantly. These findings suggested the needs of incorporating muscle strengthening programme, especially the rotators, into the management of these patients; however, the efficacy of a proper isokinetic training programme would need further investigation. Isokinetic testing would not increase the resting muscle activities and co-activity, suggesting that this type of muscle contraction or exercise may not increase muscle spasm and could be a good training option for clinical patients with AC.
ACKNOWLEDGEMENTS
The authors would like to thank Professor Chen-An Tsai for his statistical consultation. This study was sponsored by National Science Council of Taiwan (NSC93-2815-C-039-007-B) and China Medical University (CMU93-ST-07).
REFERENCES