OBJECTIVE: To study factors related to quality of life after a hypoxic period due to cardiac arrest.
DESIGN: Retrospective cohort study.
SUBJECTS: Eighty-eight survivors of out-of-hospital cardiac arrest, admitted to a Dutch academic hospital between 2001 and 2006.
METHODS: Patients received a set of questionnaires at home. The main outcome measures were physical and mental quality of life (Medical Outcomes Study 36-item Short Form Health Survey; SF-36). Potential determinants were cognitive complaints, emotional problems (depression/anxiety), post-traumatic stress, fatigue, daily functioning and participation in society. Multiple linear regression analyses were performed with physical and mental quality of life as dependent variables.
RESULTS: Sixty-three (72%) patients responded. Mean time since cardiac arrest was 36 months (standard deviation (SD) 19) . Backward regression analyses showed that physical quality of life was significantly (p < 0.001, adjusted R2 = 0.531) related to cognitive complaints (β = –0.378), instrumental daily life activities (β = 0.262), post-traumatic stress (β = –0.246) and fatigue (β = –0.226). Mental quality of life was significantly (p < 0.001, adjusted R2 = 0.664) explained by anxiety/depression (β = –0.609), fatigue (β = –0.177) and cognitive complaints (β = –0.175).
CONCLUSION: Quality of life is related to cognitive complaints, fatigue, anxiety/depression, post-traumatic stress and difficulties in daily activities in survivors of out-of-hospital cardiac arrest. Rehabilitation programmes for this group should specifically address these topics.
Key words: heart arrest; quality of life; cognition disorders; hypoxia-ischaemia brain.
J Rehabil Med 2010; 42: 553–558
Correspondence address: Caroline van Heugten, Department of Psychiatry and Neuropsychology, School for Mental Health and Neuroscience, PO Box 616, NL-6200 MD, Maastricht, The Netherlands. E-mail: c.vanheugten@np.unimaas.nl
Submitted September 16, 2009; accepted January 28, 2010
INTRODUCTION
A person’s quality of life (QoL) should be a major outcome measure in studies of survivors of cardiac arrest (1), since reporting survival rates alone does not provide complete information about the success of resuscitation. Several prospective studies have reported that the long-term QoL of cardiac arrest survivors is generally acceptable to good (2–4). However, a substantial group of cardiac arrest survivors experience ongoing problems and a decreased QoL (5). Medical variables cannot reliably predict QoL after cardiac arrest. Although the performance of bystander cardiopulmonary resuscitation (CPR) seems to be associated with a better QoL (4), longer time delays during resuscitation and the type of emergency cardiac care were not related to post-cardiac arrest QoL (6–8). In order to help those survivors with long-term problems, it is important to investigate which factors influence their QoL, as this may identify potential targets for rehabilitation treatment.
Survivors of cardiac arrest are often categorized as “cardiac patients”, although they may also be regarded as “neurological patients” because a cardiac arrest can result in hypoxic brain injury. Indeed, approximately half of cardiac arrest survivors have enduring cognitive impairments, as was shown in a recent systematic review (9). The long-term consequences of hypoxic brain injury secondary to cardiac arrest may therefore be comparable to the long-term consequences of other types of brain damage, such as traumatic brain injury.
Studies on patients with varying other causes of brain injury have revealed that reduced QoL was associated with 3 important variables, namely cognitive impairments, emotional problems and fatigue. Cognitive impairments were related to the QoL of patients after stroke (10). The importance of emotional problems was shown in a study on patients with mild traumatic brain injury in which life satisfaction was related to post-traumatic stress and depression (11). Fatigue was associated with QoL in both stroke patients (12) and traumatic brain-injured patients (13). Similarly, multivariate regression analyses in a cohort of survivors of subarachnoid haemorrhage showed that mood, fatigue, and cognitive complaints were strongly associated with reduced scores on a stroke-specific QoL scale (14).
There are few studies that have investigated possible cognitive or psychosocial factors affecting QoL after cardiac arrest. One study showed that memory complaints were related to QoL in a study on survivors of out-of-hospital cardiac arrest (15). Another study identified that post-traumatic stress was common after cardiac arrest and was negatively related to QoL (16). In addition, anxiety and depression were also reported frequently after cardiac arrest and affected perceived health improvement and social functioning (8). However, the amount of information on factors affecting QoL after cardiac arrest is limited and an integrative multivariate model is currently lacking.
The aim of this study was therefore to investigate potential determinants of QoL after a hypoxic period due to cardiac arrest. It was hypothesized that QoL would be affected by the same factors that influence QoL of other brain-injured patients, namely cognitive complaints, emotional problems and fatigue.
METHODS
Survivors of out-of-hospital cardiac arrest who had been admitted to the Department of Cardiology of Maastricht University Medical Centre (MUMC+), the Netherlands, between January 2001 and December 2006 were invited to participate in this retrospective cohort study. MUMC+ is an academic hospital in the southern part of the Netherlands and is the primary referral centre for a radius of 25 km, with a catchment area of approximately 200,000 inhabitants, which is served by a single ambulance service. The incidence of cardiac arrest in this area is 9.2 per 10.000 for people between 20 and 75 years old (17). Survival rates until discharge are, in general, low (18), being 7.4% in this specific region (19).
For inclusion in this study, participants had to be survivors aged 18 years or older, still alive at the time of the study, and with sufficient knowledge of the Dutch language to complete the questionnaires.
Patient data for potential participants for this study were retrieved from 2 hospital databases containing all out-of-hospital cardiac arrests in Maastricht and the surrounding area (17, 20). Furthermore, the admission registers from 2001 to 2006 of the Coronary Care Unit were hand-searched for admissions stating “cardiac arrest” or “resuscitation”. After retrieving potential participants, data were checked for accuracy of the diagnosis and for survival until discharge. Next, the general practitioners of all potential participants were contacted to confirm whether the subjects were currently still alive. People thought to be alive received information about the study by post, together with the informed consent form and the set of questionnaires. The study protocol was approved by the medical ethics committee of MUMC+.
Other results about the respondents and their caregivers concerning their long-term functioning have been published elsewhere (5).
Assessment instruments
Socio-demographic and medical variables. The following socio-demographic variables were extracted from the notes: age, gender, marital status, living situation, educational and work situation. The medical variables extracted were: age at time of cardiac arrest, time since cardiac arrest, location of cardiac arrest, presence of witnesses, performance of bystander cardiopulmonary resuscitation, initial cardiac rhythm, number of defibrillations, interval from collapse to return of spontaneous circulation, (sub)acute interventions, left ventricular ejection fraction and cardiovascular history.
Quality of life. The Medical Outcomes Study 36-item Short Form Health Survey (SF-36), a 36-item generic QoL measure distinguishing 2 domains, namely physical health and mental health. The scores on the 2 domains range from 0 to 100. Higher scores represent a better experienced QoL. Norm values for the Dutch population are a mean (standard deviation (SD)) of 76.3 (SD 26) for the physical component and 78.0 (SD 23) for mental component (21).
Participation in society. The Community Integration Questionnaire (CIQ), a 15-item questionnaire that assesses the level of social participation in society in 3 domains: Home Integration, Social Integration and Productive Activity (22).
Basic activities of daily living. The Barthel Index (BI), a widely used instrument that measures basic (personal) activities of daily living (ADL). The instrument consists of 10 items and measures to what extent a person can perform basic ADL activities independently. High scores indicate a high level of independence (23).
Instrumental activities of daily living. The Frenchay Activities Index (FAI), an accepted measure for instrumental (extended) activities of daily living, that reports on the performance of 15 daily life activities (24).
Cognitive complaints. The Cognitive Failures Questionnaire (CFQ), a 25-item questionnaire on self-reported cognitive failures. A higher score represents the experience of more cognitive complaints (25).
Emotional problems. The Hospital Anxiety and Depression Scale (HADS), a 14-item questionnaire, designed to detect the presence of mild degrees of mood disorders in non-psychiatric hospital outpatients (26). The HADS consists of 2 sub-scales: depression and anxiety. Higher scores represent more emotional problems.
Post-traumatic stress. The Impact of Event Scale (IES), which measures psychological reactions that take place after a traumatic event. The IES consists of 15 items and explores the level of post-traumatic stress by asking for intrusive and avoidance symptoms (27, 28).
Fatigue. The Fatigue Severity Scale (FSS), a 9-item questionnaire that measures the impact of fatigue symptoms in daily activities, with a higher score indicating a more negative impact (29).
Statistical analysis
Descriptive statistics were used to present the demographic, medical and resuscitation characteristics of the study population. To investigate possible differences between the responders and the non-responders, the t-test and χ2 test were used for age and gender, respectively.
Assessment instruments in which more than 15% of the items were missing, were not used in our analyses. When there were less than 15% missing items, the missing data were imputed by dividing the sum of the scale by the number of items answered and then multiplied by the total number of items of that measurement instrument.
Because of the non-parametric distribution of most of the variables, Spearman’s rank correlations coefficients (2-tailed) were calculated to investigate relationships between the physical and mental QoL and the potential determinants. A p-value < 0.01 was considered statistically significant.
The influence of the potential determinants on QoL was determined with multiple linear regression analyses (backward method) for the physical and mental domains separately. The independent variables that were introduced were the variables with a significant correlation with QoL. A limit value for elimination in the regression analyses was set at p < 0.10. For the regression models a p-value of < 0.05 was considered statistically significant. The regression models were checked for independence of errors and absence of co-linearity and outliers.
Statistical analyses were performed using the software package SPSS version 15.0 and 16.0 (SPSS Inc., Chicago, IL, USA).
RESULTS
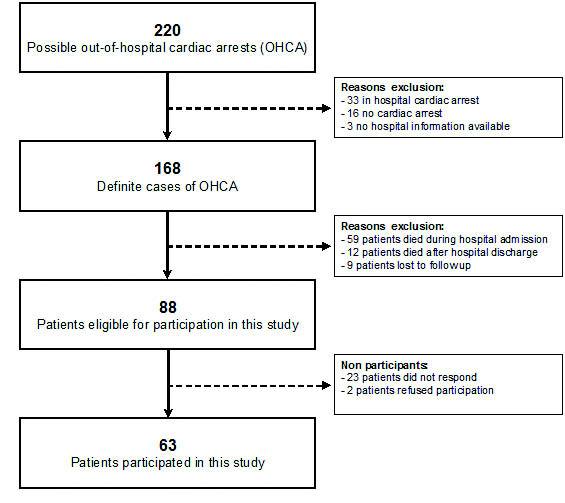
From the databases searched, 220 persons with a possible out-of-hospital cardiac arrest were identified. After excluding those who did not fulfil the inclusion criteria, or who had died, or who were lost to follow-up, 88 persons remained who were eligible for this study. This group received the set of questionnaires at home. Sixty-three persons responded by returning the questionnaires: a response rate of 72% (Fig. 1 for flow chart of patient inclusion).
Fig. 1. Patient inclusion flowchart.
There were no significant differences in gender (t = –0.62, p = 0.54) or age (χ2 = 0.04, p = 0.84) between the responders and the non-responders.
The group of responders consisted of 54 men (86%) and 9 women. Their mean age was 60.0 (SD 12.7) years. The mean time since cardiac arrest was 36.0 (SD 18.8) months. The demographic characteristics of the patients are presented in Table I. For the marital status, living situation and work situation both the results at the time of cardiac arrest and their current situation are shown. Table II shows information on the cardiac arrest, resuscitation, medical interventions and patient history.
| Table I. Demographic characteristics of the participants (n = 63) |
| | At time of cardiac arrest | Current situation |
| Age, years Mean (SD) Range | 57.3 (12.5) 18–81 | 60.2 (12.7) 20–85 |
| Gender, n % Male Female | | 54 (86) 9 (14) |
| Marital status, n % Married/living with partner Unmarried/divorced/widowed Unknown | 47 (75) 15 (24) 1 (2) | 46 (73) 15 (24) 2 (3) |
| Living situation, n % Home (independent) Home (with help from others) Sheltered housing Nursing home | 54 (86) 8 (13) 1 (2) – | 53 (84) 8 (13) 1 (2) 1 (2) |
| Education, n % Primary school Secondary school High school University Other/unknown | | 7 (11) 12 (19) 30 (48) 6 (10) 8 (13) |
| Working situation, n % Full-time/self-owned company Part-time Permanently unfit to work Volunteer work No job Retired Housewife | 30 (48) 5 (8) 5 (8) – – 17 (27) 6 (10) | 17 (27) 10 (16) 6 (10) 1 (2) 1 (2) 22 (35) 6 (10) |
| SD: standard deviation | | |
| Table II. Medical data of the participants |
| | n | |
| Age at time of cardiac arrest, mean (SD) | 63 | 57.3 (12.5) |
| Time since cardiac arrest (months), mean (SD) | 63 | 60.0 (18.8) |
| Location of cardiac arrest, n (%) Street/public area Home In the ambulance Other | 63 | 30 (48) 20 (32) 4 (6) 9 (14) |
| Witnessed cardiac arrest, n (%) | 63 | 56 (89) |
| Bystander CPR, n (%) Yes, by lay person Yes, by trained person No | 63 | 26 (41) 23 (37) 14 (22) |
| Initial cardiac rhythm, n (%) Ventricular Fibrillation Ventricular tachycardia/Ventricular Fibrillation Other rhythm | 62 | 55 (89) 6 (10) 1 (2) |
| Number of defibrillations, median (range) | 63 | 2 (0–12) |
| Interval collapse – ROSC (min), median (range) | 47 | 10 (2–35) |
| (Sub)acute interventions, n (%) none/only catheterization Catheterization with PCI Coronary artery bypass graft Implantable cardioverter defibrillator Therapeutic hypothermia | 63 | 24 (38) 28 (44) 13 (21) 25 (46) 17 (27) |
| LVEF < 1 week after cardiac arrest, mean (SD) | 58 | 47.5 (12.7) |
| Cardiovascular history, n (%) Myocardial infarction Cardiac arrest Cardiac interventions (PCI, CABG) Claudicatio intermittens Cerebrovascular accident Diabetes mellitus | 63 | 19 (30) 2 (3) 8 (13) 4 (6) 2 (3) 3 (5) |
| CPR: cardiopulmonary resuscitation; LVEF: left ventricular ejection fraction; ROSC: return of spontaneous circulation; PCI: percutaneous coronary intervention; SD: standard deviation. |
Table III shows the scores on all the questionnaires. All outcome measures were not normally distributed, except the FSS and CIQ. When more than 15% of the items were missing, this person was not taken into account in the analyses; this was the case for 2 patients on the SF-36 per subdomain, CIQ, FAI, CFQ and FSS. In case of less than 15% missing values, data were imputed; this varied from one patient (1.6%) on the HADS to 8 patients (12.7%) on the CFQ. For 6 patients this was only one item, for one patient 2 items and for one patient 3 items on the CFQ.
| Table III. Quality of life, participation, basic and instrumental activities of daily living, cognitive complaints, emotional problems, post-traumatic stress and fatigue of the participants |
| Domain Measurement instrument | n | Cut-off | Mean (SD) | Median (range) |
| Quality of life SF-36 physical SF-36 mental | 58 55 | – – | 71.8 (19.6) 73.0 (20.5) | 77.4 (28–100) 79.5 (26–100) |
| Participation in society Community Integration Questionnaire | 61 | – | 14.7 (5.5) | 15.0 (4–26) |
| Basic activities of daily living Barthel Index | 63 | < 15 | 19.4 (2.1) | 20.0 (7–20) |
| Instrumental activities of daily living Frenchay Activities Index | 61 | – | 25.7 (8.7) | 27.0 (6–41) |
| Cognitive complaints Cognitive Failures Questionnaire | 61 | > 43 | 29.8 (18.4) | 30.0 (0–73) |
| Emotional problems Hospital Anxiety and Depression Scale, total – subscale anxiety – subscale depression | 63 63 63 | > 10 > 8 > 8 | 8.5 (6.4) 4.4 (3.4) 4.2 (3.6) | 7.0 (0–25) 4.0 (0–14) 3.0 (0–12) |
| Post-traumatic stress Impact of Event Scale | 63 | > 25 | 13.0 (13.7) | 8 (0–53) |
| Fatigue Fatigue Severity Scale | 61 | > 3 | 4.3 (1.6) | 4.3 (1–7) |
| SD: standard deviation. |
The mean/median score (range) on the SF-36 in our population was 71.8/77.4 (28–100) on the SF-36 physical domain and 73.0/79.5 (26–100) on the SF-36 mental domain. The scores in our sample are somewhat lower than in the Dutch norm population (21).
Table IV shows the Spearman’s rank correlations between the 2 SF-36 domains and the other variables. No significant correlations were found between the SF-36 domains and the CIQ and the BI.
| Table IV. Spearman’s correlations between quality of life and the potential determinants |
| | SF-36 Physical | SF-36 Mental |
| CIQ | 0.29 | 0.26 |
| BI | 0.22 | 0.10 |
| FAI | 0.44† | 0.41* |
| FSS | –0.61† | –0.57† |
| CFQ | –0.55† | –0.40* |
| HADS | –0.48† | –0.73† |
| IES | –0.37* | –0.43† |
| *p ≤ 0.01; †p ≤ 0.001. CIQ: Community Integration Questionnaire; BI: Barthel Index; FAI: Frenchay Activities Index; FSS: Fatigue Severity Scale; CFQ: Cognitive Failures Questionnaire; HADS: Hospital Anxiety and Depression Scale; IES: Impact of Event Scale; SF-36: Short Form 36. |
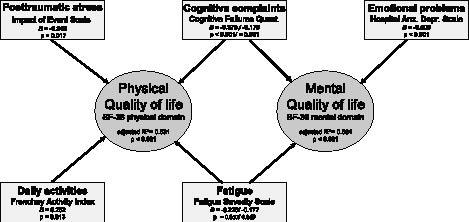
Fig. 2 presents the results of the backward regression analyses. The variables with significant correlations in Table IV were introduced as independent variables.
Fig. 2. Regression analyses: determinants of physical and mental quality of life.
For the SF-36 physical domain the model could significantly explain 53% of the variance (p < 0.001, adjusted R2 = 0.531). Four variables contributed to the model: in order of impact, the CFQ (β = –0.378, p = 0.001), FAI (β = 0.262, p = 0.013), IES (β = –0.246, p = 0.017) and the FSS (β = –0.226, p = 0.057). The final model for the SF-36 mental domain accounted for 66% of the variance (p < 0.001, adjusted R2 = 0.664). In this model, mental QoL was related to the HADS (β = – 0.609, p < 0.001), the FSS (β = –0.177, p = 0.069) and the CFQ (β = –0.175, p = 0.081).
DISCUSSION
This retrospective cohort study has shown that QoL can be at risk after out-of-hospital cardiac arrest. The QoL scores were slightly below that of the general Dutch population (21). This is in line with previous studies on QoL after cardiac arrest (6, 30). Mental QoL could be affected more than physical QoL, probably because significant motor impairments after cardiac arrest are rare. In addition, both cognitive and emotional functioning contribute to mental QoL. Both are known to be at risk after hypoxic brain injury (5, 31, 32).
The correlation matrix showed that QoL significantly correlated with instrumental daily activities, severity of fatigue, amount of cognitive complaints, level of mood disturbance (anxiety/depression) and degree of post-traumatic stress. In contrast, QoL was not related to participation in society and basic (personal) ADL functioning. That social participation was not related to QoL is surprising. However, this might be explained by the fact that the majority of the participants were no longer working and were over 60 years old, implying that their participation may already have been limited prior to the cardiac arrest. Basic ADL activities were hardly impaired and showed a clear ceiling effect, which probably explains the lack of any detectable influence.
The regression analyses revealed that physical QoL was significantly related to cognitive complaints, performance of instrumental daily activities, post-traumatic stress and fatigue. Mental QoL was primarily affected by anxiety/depression and, to a lesser extent, to fatigue and cognitive complaints. Both models could explain a substantial amount of the variance, 53% and 66%, respectively. Instrumental daily activities contributed only to physical QoL, probably because a minimal level of physical fitness is necessary to perform these daily activities. Post-traumatic stress also contributed to physical QoL only. In contrast, in a group of subarachnoid haemorrhage patients, comparable in the sense that they also have brain injury without clear physical impairments, post-traumatic stress disorders strongly predicted both mental and physical QoL after 13 months (33). Anxiety and depressive symptoms were strongly related to mental QoL alone, as would be expected since both are measures of mood disturbance. Cognitive complaints and fatigue were related to both physical and mental health. Fatigue is clearly a concept with both a mental and a physical aspect. That cognitive problems also affect physical health is an interesting finding, and possibly arises because cognitive impairments, for example in memory and planning, reduce the performance of complex physical activities.
There are some limitations to this study. First, the design was retrospective, which may have led to a selection bias and makes it difficult to draw causal relationships between QoL and the potential determinants. Secondly, not all potential participants actually participated. Although the response was relatively high, this may have led to selection bias. It is possible that some people were in such a poor condition that completing the questionnaires was not possible for them. On the other hand, it might also be that those without any complaints did not want to participate as they felt that there was “nothing wrong”, or due to the fact that they were too busy with their daily life. Looking at the incidence rates in the region and the number of patients retrieved from the hospital files, the sample can however be regarded as highly representative. Thirdly, time since cardiac arrest varied between 1 and 6 years and therefore participants may have been in different phases of recovery. Fourthly, we used self-report. The self-reporting of cognitive complaints has to be interpreted with caution, especially in cases of severe hypoxic brain injury. However, self-report of mood and activities are probably valid. To overcome the weaknesses mentioned above, a larger, prospective study would be necessary, in which cognitive impairments should be objectified with neuropsychological tests. Such a study is currently being conducted (34).
In conclusion, this study has shown that QoL after cardiac arrest seems to be affected by multiple factors including cognitive complaints, fatigue, emotional problems, post-traumatic stress and difficulties in daily activities. A similar pattern has been shown in patients after stroke (10, 12, 14) and traumatic brain injury (11, 13). This confirms our hypothesis that a survivor of a cardiac arrest should not only be regarded as a “cardiac patient”, but also as a “brain-injured patient”. Furthermore, our finding that QoL is related to a diversity of factors, suggests that multidisciplinary rehabilitation programmes focussing on these factors, should be developed and evaluated.
AcknowledgEments
We are grateful to B. Eikemans, J. de Munter, M. de Munter and J. Partouns for their help in identifying potential participants and collecting medical data. S. Bekkers and A. Gorgels are thanked for facilitating this study.
The study is funded by the Netherlands Organization for Health Research and Development (ZON/MW) and Fonds Nuts/Ohra.
REFERENCES