Andrea Santamato, MD1, Maurizio Ranieri, MD, PhD2, Francesco Panza, MD, PhD3, Vincenza Frisardi, MD3, Maria Francesca Micello, MD1, Serena Filoni, MD4 and Pietro Fiore, MD1
From the 1Department of Physical Medicine and Rehabilitation, University of Foggia, 2Department of Neurological and Psychiatric Sciences, University of Bari, 3Geriatric Unit & Gerontology-Geriatrics Research Laboratory, Department of Medical Sciences, IRCCS Casa Sollievo della Sofferenza, San Giovanni Rotondo and 4Fondazione Padre Pio Rehabilitation Center San Giovanni Rotondo, Foggia, Italy
OBJECTIVE: Some patients receiving botulinum toxin type A therapy develop immunological resistance due to the production of neutralizing antibodies against the neurotoxin, thus partially or completely reducing the therapeutic effect.
CASE REPORT: We report here neurophysiological and clinical findings for a 58-year-old man treated with botulinum toxin type A for spasticity after ischaemic stroke, who became a secondary non-responder patient. Subsequent treatment with a different preparation of botulinum toxin type A had a great therapeutic effect on his spasticity. The muscles injected and the dosages were the same for each treatment, but evaluation with the Modified Ashworth Scale after treatment with the second preparation showed a reduction of approximately 2 points compared with the first examination. The clinical results were also supported by extensor digitorum brevis testing of the right muscle, which showed a reduction in compound muscle action potential, whereas it was unchanged in the non-injected muscle. No side-effects were reported, and after 1 year of treatment with this formulation clinical benefits were still evident.
CONCLUSION: The neurophysiological and clinical results obtained in this patient suggest that switching therapy from a complexing protein-containing product to a product potentially free of complexing proteins, which has low immunogenicity, may be a viable therapeutic option in secondary non-responder patients.
Key words: botulinum toxin type A; antibodies; EDB test; compound muscle action potential.
J Rehabil Med 2012; 00: 00–00
Correspondence address: Andrea Santamato, Department of Physical Medicine and Rehabilitation, University of Foggia, “OORR”, Viale Pinto, IT-71100 Foggia, Italy. E-mail: a.santamato@unifg.it
Submitted December 7, 2011; accepted April 2, 2012
INTRODUCTION
Botulinum toxin type A (BTX-A) represents the gold standard therapy for focal spasticity and related disorders. Its main advantages are low prevalence of complications, reversibility and efficacy in reducing spastic hypertonia (1). Although treatment with BTX-A is effective and safe, it needs to be repeated periodically, and some patients develop secondary immune resistance or do not obtain effective control of symptoms. Good treatment practice includes several points to avoid the development of antibodies against the neurotoxin component of the BTX-A drug, called neutralizing antibodies (BTX-A-ab). The risk of the development of BTX-A-ab is increased with short intervals between injections, high doses of injected BTX-A, and the immunological properties of the Botulinum toxin preparation used (2, 3). In addition, it has been suggested that the reagibility of the individual patient’s immune system (i.e. the ability of an antigen to stimulate an immune response) influences the formation of BTX-A-ab (2). Neutralizing antibodies directed against the core neurotoxin can interfere with pharmacological activity, potentially leading to loss of clinical efficacy, and thus partially or completely reducing its therapeutic effect.
In clinical practice, the choice of dose and frequency of injections are designed to minimize antibody formation. Data are missing on the BTX-A-ab prevalence in adult patients undergoing long-term treatment for spasticity. Yablon et al. (4) evaluated 3 post-stroke spasticity studies, which were restricted to less than 1 year of treatment, and which included BTX-A-ab detection in 191 out of a total of 235 patients by the mouse protection assay. Turkel et al. (5) described 1 of the 317 subjects with post-stroke spasticity who became BTX-A-ab positive after BTX-A treatment. This subject responded clinically to the first 4 treatments, but became a non-responder at treatment 5. Dressler et al. (6) noted that treating with BTX-B patients with BTX-A-ab, they developed after second and third injections also BTX-B-ab. A new type of BTX-A, Xeomin® (Merz Pharmaceuticals GmbH, Frankfurt, Germany), contains only the pure neurotoxin (150 kDa) through a manufacturing process that separates it from complexing proteins, such as haemagglutinins (HA) and other proteins in the neurotoxin complex produced by fermentation of Clostridium botulinum (7). A previous study hypothesized that complexing proteins are responsible for most of the immunogenic response, facilitating the development of neutralizing antibodies against the active neurotoxin, leading to partial or complete clinical unresponsiveness (treatment failure) to BTX-A (8).
We report here a case of a 58-year-old man treated with botulinum toxin type A for spasticity after ischaemic stroke, who became a secondary non-responder patient. Subsequent treatment with a different preparation of botulinum toxin type A had a good therapeutic effect on his spasticity.
CASE REPORT
A 58-year-old man with spasticity after ischaemic stroke was found at first examination to have flexed elbow and fingers with spasticity graded 3 on the Modified Ashworth Scale (MAS) (9), and, for the lower limb, MAS 3 at the ankle. The total dosage of BTX-A injected under ultrasound guidance ranged from 550 to 700 MU, diluted in 2 ml 0.9% saline, according to the European Consensus Conference for high dosages (1). Of these dosages, a total of 70–80 MU BTX-A was injected into the pectoralis major, 100–150 MU into the biceps brachialis, 50–75 MU into the pronator teres, 80–120 MU into the flexor digitorum superficialis, 75–100 MU into the flexor digitorum profundus, 75–100 MU into the flexor carpi ulnaris, and 20–40 MU into the thumb flexor. A maximum dosage of 200 MU was injected into the ankle plantiflexors. Each treatment was associated with electrical stimulation (30 min of rectangular current pulses, at 4 Hz, 2 ms, with the intensity adjusted to elicit visible muscle contraction) and stretching of the injected muscles. The patient reported a significant reduction in spasticity for only one year of therapy. During successive treatments every 3 months the patient did not report any effect with the same dosage of BTX-A. An ultrasound examination of the spastic injected muscles excluded fibrosis, and a radiographic examination excluded the presence of muscle-tendon degeneration.
A suspicion of secondary resistance to BTX-A was raised. Therefore, an extensor digitorum brevis (EDB) test for antibody detection was performed (10). EDB compound muscle action potential (CMAP) amplitude of both sides was recorded by transcutaneous supramaximal electrical nerve stimulation of the peroneal nerve, before and after 70 MU BTX-A injection into the EDB muscle. CMAP amplitudes before injection were 12.1 mV and 11.4 mV for the left and right EDB muscle, respectively (normal value > 3 mV) (11). Four weeks after BTX-A injection into the right EDB, the decrease in CMAP amplitude was absent (10.2 mV). No significant change in CMAP amplitude was found after BTX-A injection and the patient is considered a secondary non-responder. The patient was therefore treated with oral muscle relaxant (baclofen (Lioresal, Novartis, Pharmaceuticals, Bethesda, USA) lioresal at a dosage of 100 mg/day), to obtain the same effect as BTX-A injection, but the presence of side-effects, such as continuous cephalalgia and sleepiness, was considered significant enough to suspend the administration.
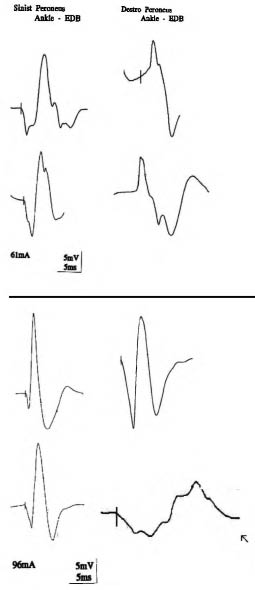
Several months later the patient was treated with BTX-A Xeomin®, which is free of complexing proteins such as haemagglutinins and other proteins, and has low immunogenicity supposing the presence of BTX-A-ab as hypothesized after the EDB test. The muscles injected and the dosages were the same as used previously, and evaluation showed a reduction of approximately 2 points on the MAS compared with the first examination. The clinical results were also supported by the EDB test into the right muscle, which showed a reduction in CMAP (13.6 mV before and 2.9 mV 4 weeks after BTX-A injection), whereas it was unchanged in the non-injected muscle (27.9 mV before and 26.4 mV) (Fig. 1). No side-effects were reported after injection, and after one year of treatment with this formulation, with injections every 3 months, good clinical benefits continued.
Fig. 1. In both parts of the figure, each upper row represents compound muscle action potential (CMAP) before botulinum toxin type A (BTX). A injection into the right extensor digitorum brevis (EDB) muscle, while the lower row represents CMAP after the treatment. The upper half of the figure shows no reduction in CMAP amplitude after BTX-A injection. The lower half of the figure shows a decrease in CMAP amplitude (arrow) after changing BTX-A product, corresponding to good clinical benefits. Normal CMAP amplitude value for EDB muscle > 3 mV (11).
DISCUSSION
Failure of BTX-A treatment in patients with focal spasticity is generally associated with several factors. In fact, there are many possible reasons for loss of response to botulinum neurotoxins, BTX-A-ab being only one of these reasons. Other possible factors include errors related to drug preparation or administration (e.g. storage, reconstitution), improper selection of muscles (e.g. injecting muscles with fixed contractures or not injecting all the relevant muscles), inadequate doses per injection site or area, change in underlying disease presentation, or expectation effects (2). It is therefore good practice to administer doses that are sufficient to provide meaningful duration of clinical effect. The risk of antibodies is increased with short inter-injection intervals and high doses injected, and injection series with intervals of less than 3 weeks (“booster’’ injections) should also be avoided (2). The immunological quality of the BTX-A drugs used has also been recognized as a risk factor (3). Antibody-induced failure of therapy usually develops within the first 2–3 years of BTX-A treatment (6).
In the present report, the patient reported evidence of reduction in spasticity after changing BTX-A formulation. In fact, after one year of therapy with products containing complexing proteins eliciting the production of neutralizing antibodies, the MAS score was not reduced. This failure can be explained by the production of antibodies against BTX-A, as confirmed by EDB test. The EDB test represents an easy screening method to detect patients in whom secondary non-responding is probably caused by antibody formation. It is sufficiently specific and no contradictions were found between the “gold standard test” (mouse bioassay) and the clinical EDB test (10). The patient was therefore treated with BTX-A Xeomin®, which is potentially free of complexing proteins with low immunogenicity. The MAS score and EDB test revealed a positive pharmacological effect.
The dose was chosen after considering previous studies, which described a dose ratio of 1:1 for BTX-A Xeomin® to another conventional BTX-A complex product (Botox® Allergan, Irvine, UAS) (12). Preliminary experiments with Xeomin® also suggest that the absence of complexing proteins is associated with reduced immunogenicity. In a preclinical animal study with cynomolgus monkeys, repeated injections with 4.8, or 16 U/kg BTX-A Xeomin® or control were not associated with the development of neutralizing antibodies in each group, despite clear evidence of biological activity of the neurotoxin, particularly in the highest-dose group (13). Hence, the presence of complexing proteins in commercially available BTX-A preparations may facilitate an immunogenic reaction, and the development of neutralizing antibodies against the active neurotoxin may lead to partial or complete clinical unresponsiveness to BTX-A (i.e. treatment failure) (8). In the present report, the BTX-A used had the same efficacy and safety profile as complexing protein-containing products used in the treatment of spasticity in a secondary non-responder patient. However, because secondary non-responders without evidence of serum antibodies have been found (2), given the efficacy and safety in the management of spasticity also (14), we proposed switching therapy in this patient, who became a non-responder or poor-responder for antibody resistance, from a complexing protein-containing product to a product potentially free of complexing proteins, which has low immunogenicity. We report here the neurophysiological and clinical results obtained using a BTX-A product free of complexing proteins. In terms of clinical efficacy, both BTX-A Botox® and BTX-A Xeomin® result in a similar reduction in CMAP values 3 months after injection (a 40% reduction in CMAP compared with baseline) (12). Therefore, during our 1-year follow-up period, the patient was injected 4 times. On the other hand, possible differences in terms of immunogenicity between these two preparations should be tested in longer-term clinical trials. However, we cannot be certain that the therapeutic result was obtained exclusively by changing the BTX-A product, since, in their previous studies, Sankhla et al. showed spontaneous disappearance of BTX-A-ab after cessation of application (15). Moreover, this report also indicates that, for secondary non-responder patients, it is possible to change not only the serotype, but also the BTX-A product when the development of antibodies is suspected.
The authors declare no conflicts of interest.
REFERENCES