Veronika Ströbl, PhD1, Werner Knisel, MD2,3, Ulrike Landgraf, MA2 and Hermann Faller, MD, PhD1
From the 1University of Würzburg, Department of Medical Psychology, Medical Sociology, and Rehabilitation Sciences, Würzburg, 2Rehazentrum Bad Kissingen der Deutschen Rentenversicherung Bund, Klinik Saale, Bad Kissingen, Germany and 3Stadtspital Triemli Zürich, Zürich, Switzerland
OBJECTIVE: Obese patients require sustained lifestyle changes to reduce their health risks. We therefore developed a combined planning and telephone aftercare intervention based on the Health Action Process Approach to enhance physical activity after inpatient rehabilitation for obesity.
DESIGN: Randomized controlled trial.
Patients: A total of 467 obesity rehabilitation patients (55% male; mean age 48 years).
METHODS: Participants were randomized to receive standard obesity rehabilitation or standard obesity rehabilitation plus the new intervention. Participants in the intervention condition planned individual physical activities they intended to perform after discharge and were followed up by 6 phone calls for 6 months. Physical activity and body weight were assessed after 6 and 12 months.
RESULTS: The intervention was well accepted by participants. After 12 months, effects on physical activity, but not body weight, were found. At this point, the duration of physical activity per week was 58 min longer in the intervention group than in the control group. However, body weight was reduced to similar degrees in both groups.
CONCLUSION: The intervention increased physical activity, but did not reduce body weight, compared with standard care. However, even without weight reduction, an increase in physical activity may reduce health risks in obese patients.
Key words: planning intervention; telephone aftercare; obesity; physical activity; body weight.
J Rehabil Med 2012; 00: 00–00
Guarantor’s address: Hermann Faller, Department of Medical Psychology, Medical Sociology, and Rehabilitation Sciences, University of Würzburg, Klinikstr. 3, D 97070 Würzburg, Germany. E-mail: h.faller@uni-wuerzburg.de
Submitted May 14, 2012; accepted September 25, 2012
INTRODUCTION
Health behaviour changes are of utmost importance to reduce health risks in obese patients, such as the risk of developing hypertension, diabetes mellitus, coronary heart disease, and musculoskeletal disorders, among others. Although long-lasting health behaviour changes regarding physical activity and diet are required (1), intervention effects are often short-lived (2). Thus, aftercare plays an important role in maintaining health behaviour changes (3). Physical activity appears to be a specifically promising target for such an intervention, as an increase in physical activity may reduce the health hazards of obesity even in the absence of a reduction in body weight (4). However, changes in exercise are more difficult to sustain than changes in diet (5). Thus, an aftercare intervention for obese patients was developed and evaluated, with the goal of increasing daily physical activity levels after discharge from inpatient medical rehabilitation for obesity. As obesity is highly prevalent in Western societies (6, 7), with more than 50% of the adult population in Germany being overweight or obese (8), demonstrating long-term effects of an aftercare intervention would be highly relevant.
Although many obese individuals build the intention to increase their exercise behaviour, few succeed in actually changing it. To close this intention-behaviour gap, implementation intentions, as described by the Health Action Process Approach model (9), have proved successful (10). Implementation intentions are action plans that describe, in as much detail as possible, when, where, and with whom a person will perform a specific health behaviour. In studies with patients who have cardiological or musculoskeletal disorders, planning interventions have demonstrated positive effects on physical activity behaviour for up to 12 months after medical rehabilitation (11–14).
Telephone aftercare interventions have also proved promising for maintaining weight reduction in obese patients (3). Phone calls allow detection and targeting of problems patients encounter in their daily lives. In previous studies, telephone-based aftercare has shown promising results in patients after discharge from medical rehabilitation. A follow-up intervention through regular phone calls has shown positive effects regarding cardiovascular risk reduction in cardiac rehabilitation patients (15). In a study with obese patients, an aftercare intervention that combined phone calls and home visits proved effective regarding weight loss at the end of the intervention (16). Building on these promising approaches, we developed a new intervention that integrated both planning and aftercare, with the aim of helping patients maintain behaviour changes in their everyday life.
We performed a randomized controlled trial with obese rehabilitation patients evaluating a combined planning and telephone aftercare intervention designed to enhance daily physical activity. Participants in the intervention condition were hypothesized to show significantly higher increases in physical activity and decreases in body weight 12 months after rehabilitation (primary outcomes), compared with usual care. Moreover, moderator effects of gender were examined.
METHODS
A prospective, randomized, controlled study was performed, comparing a control condition of standard inpatient medical rehabilitation treatment for obesity (usual care) with an intervention condition consisting of a combined planning and telephone aftercare intervention in addition to standard rehabilitation.
Interventions
All study participants received the standard medical inpatient rehabilitation treatment for morbidly obese patients (usual care), as provided by a rehabilitation clinic of the German Statutory Pension Insurance (Rehazentrum Bad Kissingen der Deutschen Rentenversicherung Bund, Klinik Saale, Bad Kissingen, Germany). This 3-week multimodal, structured, interdisciplinary treatment aims at weight management and is based on nutrition therapy, physical exercise, and psychoeducation (Table I). While the control group received only the standard rehabilitation, the intervention group additionally received a planning intervention provided in a group setting (50 min), followed by an individual counselling session (10 min) 1 week later, before discharge, and 6 phone calls of 5–10 min duration for up to 6 months after discharge. Based on existing intervention programmes (11, 17), manuals were developed for each of the 3 intervention components, covering definition of goals, didactic methods, and media, including a booklet for patients entitled “My Activity Schedule”.
|
Control condition (usual care) |
Intervention condition (planning and aftercare) |
|
|
Standard inpatient rehabilitation for obesity (3 weeks duration) |
Complete medical check-up with assessment of cardiovascular risk factors |
Complete medical check-up with assessment of cardiovascular risk factors |
|
Nutrition therapy (supervised selection of healthy food at daily special buffets; cooking seminars; group counselling about healthy food) |
Nutrition therapy (supervised selection of healthy food at daily special buffets; cooking seminars; group counselling about healthy food) |
|
|
Physical exercise (daily group training courses for obese patients only including swimming; regular use of step counter; individualized gym for improvement of endurance and muscular function) |
Physical exercise (daily group training courses for obese patients only including swimming; regular use of step counter; individualized gym for improvement of endurance and muscular function) |
|
|
Psychoeducation (group seminar about life style change and barriers to reduce body weight; seminar about body perception; group seminar about ability to enjoy) |
Psychoeducation (group seminar about life style change and barriers to reduce body weight; seminar about body perception; group seminar about ability to enjoy) |
|
|
Planning and aftercare intervention |
Not provided |
Group counselling session |
|
Not provided |
Individual counselling session |
|
|
Not provided |
Six telephone aftercare calls |
|
In the group counselling session of 4–10 participants, the transfer of physical activity behaviours into everyday life after discharge from inpatient rehabilitation was addressed. To strengthen their self-management skills, patients were encouraged to reflect on suitable types of physical activity they would like to perform for 45 min each on 5 days a week. Patients were then taught how to plan the implementation of the behaviours selected. Participants also discussed what obstacles they might encounter and how to cope with them. They were shown how to monitor their behaviour and adapt their plans if necessary. The intervention techniques used in the planning intervention were coded according to the classification of Abraham & Michie (18) as follows: provide general information on behaviour-health link, prompt intention formation, prompt barrier identification, prompt specific goal setting, and prompt self-monitoring of behaviour. At the end of the group session, patients were given their booklets and invited to make individual physical activity and coping plans for the time after discharge. Up to 3 activity behaviours could be selected. Patients were offered templates for the individual plans as well as for self-monitoring of behaviours.
After 5–7 days, each patient received an individual counselling session to review the plan they had made. In this session, the time point for the first phone call was also arranged.
The telephone aftercare comprised 6 phone calls within 6 months after discharge from inpatient medical rehabilitation. These calls aimed to enhance compliance with the physical activity plans patients had made and to increase patients’ self-management skills. The phone calls started 2 weeks after discharge and were provided at a decreasing rate to gradually shift responsibility back to the patient. Thus, follow-up calls were scheduled at 2, 5, 9, 13, 18 and 24 weeks after the end of inpatient rehabilitation. The patients’ experiences with the implementation of their exercise plans were discussed. In particular, patients reported on their exercise behaviour, the obstacles they had met, and the coping strategies they had employed. For each activity, the plans were reinforced and, at times, generalized, reduced, or otherwise adapted, as needed. The intervention techniques applied were classified as follows (18): provide general encouragement, prompt review of behavioural goals, provide feedback on performance, use of follow-up prompts, relapse prevention. The phone calls were provided by the sports therapist (UL), who had also led the group and individual counselling sessions at the clinic.
Treatment integrity of the intervention was ascertained by providing manuals for the 3 intervention modules, by training the sports therapist, and by auditing and supervising group session samples in regard to adherence to the manual. For privacy reasons, neither phone calls nor individual sessions were audio recorded.
Measurements
The primary outcomes included changes in physical activity and body weight. Physical activity was measured using the Freiburg Questionnaire for Physical Activity (19). This well-validated, widely-used German self-report questionnaire covers basic activities (e.g. walking, climbing stairs), leisure activities (e.g. cycling, dancing) and sports activities (e.g. jogging, squash). Type of activity, frequency, and duration during defined time frames are assessed, yielding scores for weekly physical activity duration of each of the domains as well as a total score. In addition, each activity is assigned a standardized energy expenditure score (20), allowing for measurements of the total energy expenditure per week.
Body weight was assessed by both self-reports and physician measurements (at 12 months). Both assessments were highly concordant (intraclass correlation coefficient 0.99), with patients reporting slightly lower weight than did physicians (mean difference = –0.61, (standard deviation (SD) 1.88)). For the outcome analysis, the physician measurement of body weight was used whenever possible. Body height was measured by clinic staff during the clinic stay.
Behavioural determinants, as described by the Health Action Process Approach (9), including self-efficacy, action planning and coping planning, were measured using self-report scales (11–13).
Measurements were performed at 4 time-points: beginning of inpatient rehabilitation, end of inpatient rehabilitation, after 6 months and after 12 months. The follow-up assessments were performed through postal correspondence. In the case of non-response, patients were reminded once by phone or post. At the 12-month follow-up, patients were asked to obtain a body weight measurement from their general practitioner. As an incentive, patients received 15 EUR and a pedometer during their stay at the clinic. General practitioners were asked to send patients’ weight protocols back to the research centre in pre-paid, prepared envelopes.
Patient eligibility and recruitment
Patients were eligible if they had obesity (International Classification of Diseases 10 (ICD-10) E66) and had a body mass index (BMI) of between 30 and 44 kg/m2, had started inpatient medical rehabilitation with the goal of reducing their body weight, and were between 18 and 65 years of age. They were excluded if they had type 1 diabetes or a disorder precluding participation in sports therapy. Other co-morbidities were allowed, as they are frequent among obese patients. Patients who had had or were planning to have bariatric surgery were also excluded. Patients who were not able to see, hear, read or understand German or who had severe psychiatric disorders, such as psychotic and substance abuse disorders, were also excluded. Patients were recruited between October 2008 and November 2009. All participants gave written informed consent. The study was approved by the ethics committee of the Faculty of Medicine of the University of Würzburg.
Randomization
Patients were assigned randomly to either the intervention or usual care group. The random sequence was generated at the University of Würzburg by staff not working at the rehabilitation clinic, using a computer program. After having recruited a participant, clinic staff requested the randomization result from the scientific staff by phone (telephone randomization) thus guaranteeing concealment of randomization up to recruitment. Randomization was performed on the basis of the individual patient, stratified by gender. However, during some weeks, randomization had to be performed on a cluster (i.e. group of 10 patients) basis due to the low number of patients admitted to the hospital. This procedure was applied for 90 participants.
Statistical analysis
Primary outcomes were compared between intervention and control groups using analysis of covariance (ANCOVA), adjusting for baseline scores of the outcome variables. ANCOVA with control for baseline scores was used as it is not so susceptible to regression to the mean effects as repeated measures ANOVA. All participants who had provided data were included in the analysis, independent of the number of aftercare phone calls they had received. All outcomes were analysed by intention-to-treat carrying baseline values forward when follow-up values were missing. A two-sided p-value < 0.5 was considered significant. Effect sizes are also reported. In addition, within-group effects, including standardized effect sizes, are reported for both study groups. Moderator analysis was performed by including the moderator variable as an additional factor in the ANCOVA and examining interaction effects. To explore the process translating the intervention effect on physical activity at 12 months (residual adjusted for baseline value), path analysis was used. Model fit was based on a non-significant χ2-test, Comparative Fit Index (CFI) > 0.97, Tucker Lewis Index (TLI) > 0.97, root mean square error of approximation (RMSEA) < 0.05, and standardized root mean square residual (SRMR) < 0.05. Bootstrapping was used to quantify the indirect effect. All statistical analyses were performed using SPSS statistical software version 18 (IBM, Armonk, NY, USA) and MPlus software (Muthén & Muthén, Los Angeles, CA, USA).
RESULTS
Participant flow and baseline characteristics
Fig. 1 shows the participant flow throughout the study. Of 958 patients screened, 544 were eligible and 467 participated (non-consent rate 13%). At the 12-month follow-up, 341 participants (73%) had provided data (intervention group n = 177, 78%; control group n = 164, 69%). Of these, objective weight measurements were available for 79%.
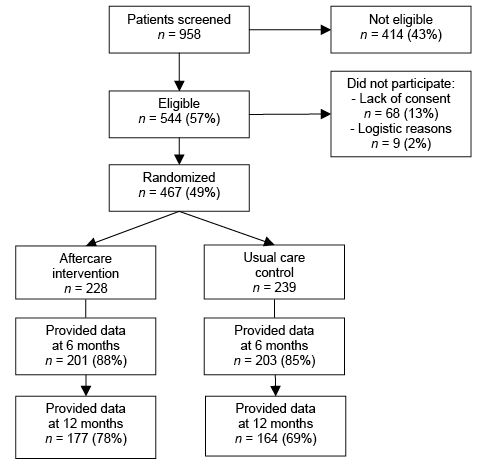
Fig. 1. Participant flow.
The patients’ mean age was 48 years (SD 9.8, range 18–64 years) and 55% were male. The proportion of low, medium and high social-economic status was 2%, 60%, and 36%, respectively. The mean BMI was 36 kg/m2 (SD 3.5). The proportion of obesity grades I, II and III was 38%, 45%, and 16%, respectively. The mean number of co-morbid disorders was 3 (SD 1.3, range 0–7). The most frequent co-morbidities were hypertension (74%), type 2 diabetes (64%), musculoskeletal disorders (50%), and hyperlipidaemia (48%). As Table II shows, the intervention and control groups were well balanced regarding baseline characteristics, with the exception of physical activity, which was higher in the control group than in the intervention group. Therefore, baseline physical activity was controlled for during the analysis of this outcome. Patients who had refused to participate did not differ from participants regarding age, gender, marital status, education or physical activity. However, they tended to have a lower BMI (data not shown). Patients who had not provided data at the 12-months time-point were younger and had a higher baseline BMI, but did not differ from responders regarding baseline physical activity (data not shown). However, at the 12-month time-point, intervention group participants were less frequent among drop-outs than among respondents (41% vs 52%, p = 0.037).
|
Table II. Baseline characteristics of the sample |
||
|
Intervention group (n = 228) |
Control group (n = 239) |
|
|
Age, years, mean (SD) |
48.54 (9.77) |
48.03 (9.77) |
|
Gender, male, n (%) |
124 (54) |
134 (56) |
|
Marital status, n (%) |
||
|
Never married |
49 (22) |
53 (22) |
|
Married |
142 (62) |
152 (64) |
|
Divorced |
30 (13) |
29 (12) |
|
Widowed |
7 (3) |
5 (2) |
|
Education, n (%) |
||
|
Less than junior (< 10 years; basic secondary school) |
54 (24) |
63 (26) |
|
Junior (10 years; middle-level secondary school) |
88 (38) |
89 (37) |
|
Senior (high-school graduate) |
81 (35) |
80 (34) |
|
Other |
5 (2) |
7 (3) |
|
Working status, n (%) |
||
|
Full-time |
165 (72) |
182 (77) |
|
Part-time |
28 (12) |
30 (13) |
|
Unemployed |
20 (9) |
19 (810) |
|
Other |
15 (7) |
6 (3) |
|
Physical activity, duration, h/week, mean (SD) |
5.56 (4.86) |
6.51 (5.12) |
|
Physical activity, energy expenditure, kcal/week, mean (SD) |
2,398.41 (2,160.99) |
2,829.60 (2,315.46) |
|
BMI, kg/m2, mean (SD) |
36.41 (3.56) |
36.26 (3.44) |
|
BMI: body mass index; SD: standard deviation. |
||
Treatment effects
Both intervention and control groups showed increased physical activity from baseline to both the 6- (Table III) and 12-month follow-up time-points (Table IV), but the increase tended to be larger in the intervention group. At 6 months, significant, small effects on duration of physical activity (p = 0.014) and energy expenditure (p = 0.009) were evident (Table III). After adjustment for baseline imbalance, estimated mean physical activity per week in the intervention group was 74 min longer than in the control group.
|
Table III. Within- and between-groups effects on physical activity and weight at 6 months (intervention n = 228, control n = 239) |
||||||
|
Baseline Mean (SD) |
6 months Mean (SD) |
Within-group change SES (95% CI) |
Between-group effects ANCOVA |
|||
|
p |
η2 |
|||||
|
Physical activity, duration, h/week |
0.014 |
0.014 |
||||
|
Intervention |
5.56 (4.86) |
9.24 (6.10) |
0.78 (0.59–0.98) |
|
|
|
|
Control |
6.51 (5.12) |
8.50 (5.17) |
0.40 (0.22–0.58) |
|
|
|
|
Physical activity, energy expenditure, kcal/week |
0.009 |
0.009 |
||||
|
Intervention |
2,398.41 (2,160.99) |
3,654.01 (2,517.56) |
0.53 (0.34–0.72) |
|
|
|
|
Control |
2,829.60 (2,315.46) |
3,451.27 (2,115.37) |
0.28 (0.10–0.46) |
|||
|
Weight, self-report, kg |
0.52 |
0.001 |
||||
|
Intervention |
109.8 (15.6) |
102.3 (15.9) |
0.47 (0.28–0.65) |
|||
|
Control |
109.7 (16.1) |
102.7 (16.0) |
0.43 (0.26–0.62) |
|||
|
BMI, self-report, kg/m2 |
0.66 |
0.001 |
||||
|
Intervention |
36.41 (3.56) |
33.93 (3.81) |
1.00 (0.80–1.19) |
|||
|
Control |
36.26 (3.44) |
33.94 (3.85) |
1.00 (0.81–1.19) |
|||
|
Bold figures indicate: (i) regarding within-group effects: SES of the control group is outside the 95% CI of SES of the intervention group; or (ii) regarding between-group effects: significant between-group effect (ANCOVA: p < 0.05). ANCOVA: analysis of covariance; BMI: body mass index; CI: confidence interval; SES: standardized effect size (positive SES represents improvement); SD: standard deviation; η2: effect size, (small = 0.0099, medium = 0.0588, large = 0.137). |
||||||
At 12-months, the differences between the intervention and the control group in duration of physical activity (p = 0.0118) and energy expenditure (p = 0.008) were maintained (Table IV). The estimated difference in duration amounted to 58 min per week, after adjustment for baseline imbalance.
Although both groups reduced their body weight from baseline to the 12-month time point, no between-group difference was evident (Table IV). Thus, our expectation regarding weight loss could not be confirmed.
Pre-planned subgroup analyses for those participants who had reported at baseline that they did not perform any sports activities as a subtype of physical activities (n = 318) showed significant between-group differences at 12 months in both duration (p = 0.024, η2 = 0.016) and energy expenditure (p = 0.023, η2 = 0.016) of physical activities and in particular of sports activities favouring the intervention group (duration: p = 0.055, d = 0.21; energy expenditure: p = 0.026, d = 0.25).
Moderator analyses
We explored whether the intervention effects differed between females and males. The interaction effect of treatment by gender showed trends for both the duration of physical activity (p = 0.08, η2 = 0.008) and the energy expenditure (p = 0.10, η2 = 0.007) at the 6-month time-point. Post-hoc simple effects analysis revealed that significant, small effects on both outcomes in favour of the intervention group were observed only in men (duration: p = 0.008, η2 = 0.018; energy expenditure p = 0.028, η2 = 0.012), but not in women. However, at 12 months, no interaction effect of gender was observed. For the BMI, no interaction effects of gender were observed at 6 and 12 months.
Mediator analyses
We tested whether the intervention effect on physical activity at 12 months was mediated by behavioural determinants. We selected as mediators those behavioural determinants that showed significant treatment effects at the intermediate time-points. Path analysis revealed that the intervention impacted on action planning at the end of rehabilitation, which translated into task self-efficacy at 6 months, which in turn translated into physical activity at 12 months (Fig. 2). This model fit the data well (χ2 = 1.12, p = 0.57; CFI = 1.00; TLI = 1.04; RMSEA = 0.000; SRMR = 0.014). Serial multiple mediator analysis with bootstrapping proved significance of the indirect effect (indirect effect: 0.013; 95% CI: 0.026–0.005). However, the intervention impacted physical activity at 12 months, also via a direct path, suggesting partial mediation. Gender did not moderate these links.
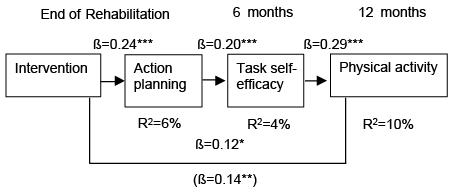
Fig. 2. *p < 0.05, ***p < 0.001. Path analysis of intervention effect on physical activity. β: beta weight; R2: explained variance. Beta weight of univariate path from intervention to physical activity at 12 months is shown in parentheses.
Feasibility and acceptance
The intervention was delivered as described in the protocol. Virtually all patients took part in the group and individual sessions, and 57% received 6, 28% 5, and 9% 4 telephone calls. The mean number of calls was 5.3 (SD 1.1). Only rarely were scheduled calls omitted, mainly for patient-related reasons, such as shift work or vacation. The mean duration of the individual phone calls was 8.2 min (SD 3.0). The mean cumulated duration of all phone calls was 44.0 min/patient (SD 19.9). Most phone calls were made in the late afternoon or early evening.
Group and individual counselling sessions, as well as follow-up phone calls, were well accepted by the patients. The counselling sessions were evaluated as very good to good (mean = 1.69, (SD 0.69); on a scale ranging from 1 = very good to 6 = not satisfactory). Similarly, the various components of the session were evaluated as very good to good on additional 10 items (data not shown). At 6 and 12 months, patients evaluated the total aftercare programme as very good to good (6 months: mean = 1.64 (SD 0.80); 12 months: mean = 1.70, SD 0.80; 6-point scale, as described above). The 6-month duration of the aftercare programme was judged to be exactly appropriate by 53% and too short by 44% of the participants, respectively. Eighty percent of participants rated the frequency of the phone calls as exactly right, while 16% would have preferred to receive more frequent calls.
DISCUSSION
In this prospective, randomized, controlled study, the effects of a combined planning and telephone aftercare intervention on physical activity could be demonstrated both at the 6-month and 12-month follow-up assessments. At 12 months, intervention patients reported a 58 min longer duration of physical activity per week, compared with control patients. It is noteworthy that the control condition also aimed at lifestyle changes including planning for exercise after discharge.
Although the differences observed may appear to be small, they are in the range of effects described in previous systematic reviews (21–24). It is noteworthy, however, that the present intervention achieved an effect that was maintained for 12 months, i.e. 6 months after the intervention terminated, in contrast to other studies evaluating telephone-based interventions for patients with type 2 diabetes or hypertension (25, 26), but consistent with a study evaluating a pedometer-based telephone intervention, including behavioural strategies, among cardiac patients (27). The current finding of effects even in the subgroup of sedentary patients who did not perform any sports is consistent with previous studies (14, 26, 28).
The results of path analysis were consistent with partial mediation of treatment effects on physical activity at 12 months via action planning at the end of rehabilitation and task self-efficacy at 6 months. This model fits the data well. It is in line with our theoretical background, the Health Action Process Approach (9).
Contrary to our expectations, no incremental effects of the intervention on body weight were observed. A reduction in body weight was evident in both groups. Thus, standard rehabilitation targeting both diet and exercise appeared to be effective on its own, with the aftercare programme having no additional impact on body weight. However, body weight has not been the immediate target, but rather a distal goal of the intervention, whereas physical activity was addressed immediately. Indeed, intervention group patients had only received a short group session and an even shorter individual counselling session, and the total time expended on the aftercare calls was also rather limited. However, longer and more intensive interventions tend to provide stronger effects (5, 29–31).
Moderator analysis revealed an interaction effect of gender at 6 months, but not 12 months: male participants benefited more from the intervention than did females (32). Women may have employed higher planning competencies at the start than did men, such that a planning intervention may have had no additional benefit for them. Moreover, women may perceive physical activities as more challenging than men, thus preventing them from exercising, as their role responsibilities are less consistent with sports activities (33). In our study, the intervention was performed by a female therapist. Effects of the gender match between therapist and participant may also be considered.
As a combined intervention was examined, the component that was most important for increasing physical activity cannot be clearly determined. Interventions that included cognitive or behavioural strategies, such as planning or self-monitoring, have proved particularly effective (21, 24, 34). For maintaining behaviour change, follow-up prompts appear to be important components (5). Moreover, the continuity of therapeutic contact seems to have been particularly favourable (30). Thus, all of these components may play an important role in producing sustained effects. However, future research may wish to disentangle the active factors by using dismantling designs.
Among the strengths of the study is the large, naturalistic sample of obese patients treated in a German inpatient rehabilitation clinic. The participation rate was high, with only 13% of those approached not consenting to partake. Further strengths include the randomized design, the 1-year follow-up, and the analysis by intention-to-teat. Moreover, objective measurements of body weight were obtained for most patients.
Several limitations must also be considered. Objective weight measurements were not obtainable for all patients. However, self-reported and measured weights were highly concordant. Although weight tends to be underreported (35), high agreement between self-reported and measured weight has also been found in other studies (36). While objective measurements of body weight were included, no objective measurements regarding the other primary outcome, physical activity, were made. Thus, self-reports may have been influenced by the tendency of social desirability. However, self-reports of physical activity have been shown to be reliable and valid when tested against maximum oxygen uptake or treadmill performance (37–39). With a participation rate of 73% at the 12-month assessment point, selection bias cannot be excluded, as patients who dropped out had a higher BMI and were younger than those who continued to participate, and because the proportion of drop-outs was different between intervention and control groups. Even though this may pose a risk of bias and limit generalization of our results, factors associated with drop-out are consistent with previous research in this field (40). Moreover, the intention-to-treat analysis used may produce rather conservative estimates of the intervention effects. Another limitation is that patients in the control condition did not receive an active aftercare intervention. Thus, the mere effects of time and attendance provided for intervention patients cannot be precluded. In particular, when asked about what aspects of the intervention they judged to be most important, many patients mentioned unspecific features of personal contact and support. However, examining the new intervention against a no-intervention control condition seemed warrantable. In the next step of research, the intervention may be tested against an unspecific attention-placebo condition providing rapport without targeting the presumed active ingredients of the intervention, i.e. behavioural determinants, such as planning and monitoring of behaviour. Despite the use of randomization for allocating participants to either the intervention or control condition, baseline imbalance was observed regarding physical activity, one of the primary outcomes. Although this difference was produced by chance, it needed to be adjusted for by ANCOVA, as recommended (41). This imbalance may have also impacted other variables, such as body weight changes, in favour of the control condition. Moreover, contamination cannot be ruled out in a parallel groups trial. Participants of the control condition may also have received information from the planning intervention or may have endorsed compensatory strategies to overcome the supposed disadvantage of being allocated to the control condition, which may have diluted treatment effects. However, despite these limitations, a randomized design seems to be preferable over a quasi-experimental design that meets more severe limitations.
In conclusion, the combined planning and telephone aftercare intervention providing 6 phone calls to obese patients may be effective in increasing energy expenditure by physical activity of participants at the 12-month follow-up. The intervention proved feasible and was well accepted by patients. The benefit of this intervention must be contrasted with the time and effort spent. Time expenditure was rather limited, but some phone calls needed to be provided in the evening hours, thus demanding that the therapist worked flexible hours. However, this aftercare programme may be considered to be worth the costs for improving health in this large but under-treated population.
ACKNOWLEDGEMENTS
This work was funded by the German Federal Ministry of Education and Research (grant number FKZ 01GX0722). We thank Dr Karin Meng for performing the bootstrap analysis.
REFERENCES
