Mitsuhiro Ochi, MD1, Satoru Saeki, MD1,2, Taiji Oda, MD1, Yasuyuki Matsushima, MD1 and Kenji Hachisuka, MD1
From the 1Department of Rehabilitation Medicine, School of Medicine, University of Occupational and Environmental Health, and 2Department of Rehabilitation Medicine, Wakamatsu Hospital of the University of Occupational and Environmental Health, Kitakyushu City, Japan
OBJECTIVE: The purpose of this study was to examine the effects of combined therapy using transcranial direct current stimulation (tDCS) with robot-assisted arm training (AT) for impairment of the upper limb in chronic stroke patients, and to clarify whether differences exist in the effect of anodal tDCS on the affected hemisphere (tDCS(a) + AT) and cathodal tDCS on the unaffected hemisphere (tDCS(c) + AT).
METHODS: Subjects in this randomized, double-blinded, crossover study comprised 18 chronic stroke patients with moderate-to-severe arm paresis. Each patient underwent 2 different treatments: tDCS(a) + AT; and tDCS(c) + AT. Each intervention was administered for 5 days, and comprised AT with 1 mA of tDCS during the first 10 min. Outcomes were identified as changes in Fugl-Meyer Assessment (FMUL), modified Ashworth scale (MAS) and Motor Activity Log (MAL) for the upper limb.
RESULTS: Both interventions showed significant improvements in FMUL and MAS, but not in MAL. Distal spasticity was significantly improved with tDCS(c) + AT compared with tDCS(a) + AT for right hemispheric lesions (median –1 vs 0), but not for left hemispheric lesions.
CONCLUSION: Although this study demonstrated that combined therapy could achieve limited effects in the hemiplegic arm of chronic stroke patients, a different effect of polarity of tDCS was seen for patients with right hemispheric lesions.
Key words: stroke; rehabilitation; brain stimulation; robotics; motor recovery.
J Rehabil Med 2013; 45: 137–140
Correspondence address: Satoru Saeki, Department of Rehabilitation Medicine, School of Medicine, University of Occupational and Environmental Health, 1-1 Iseigaoka, Yahatanishi-ku, Kitakyushu City 807-8555, Japan. E-mail: sae@med.uoeh-u.ac.jp
Submitted August 17, 2011; accepted September 5, 2012
INTRODUCTION
Effective rehabilitation therapies are needed for stroke patients showing long-term deficits in upper-arm function. Constraint-induced therapy (1) is a functional task-oriented intervention that has been shown to significantly improve upper limb function in chronic stroke patients, but only for patients with relatively mild hemiparesis of the arm (2). For chronic stroke patients with moderate or severe hemiparesis, robot-assisted arm training (AT) improved the affected arm to some extent (3). Otherwise, brain stimulation techniques, such as transcranial direct current stimulation (tDCS) and repetitive transcranial magnetic stimulation, as an adjunct to other therapies, may magnify therapeutic outcomes. The overarching aim is to increase ipsilesional excitability or decrease contralesional excitability (4). Several basic mechanisms have been proposed for the effects of tDCS (5). Anodal stimulation depolarizes the resting membrane potential of neurones, while cathodal stimulation elicits hyperpolarization. Both will alter spontaneous discharge rates and thus may affect synaptic strength. Potentiation of the effects by combining AT with brain stimulation could be expected to provide more effective therapy for moderate-to-severe hemiparesis of the arm in chronic stroke patients (6).
In a preliminary pilot study of combination therapy, Hesse et al. (7) demonstrated that anodal tDCS to the affected hemisphere with AT for the affected arm improved motor function in stroke patients. Although the combination of AT with tDCS is expected to offer some degree of clinical advantage, differences in the effects of tDCS between the affected and unaffected hemisphere in patients with chronic stroke remain unclear. This crossover, double-blinded study using tDCS with AT for the hemiparetic arm in patients with chronic stroke investigated the effectiveness of combination therapy and whether anodal tDCS to the affected hemisphere with AT or cathodal tDCS to the unaffected hemisphere with AT would lead to better increases in evident motor recovery.
METHODS
Study design
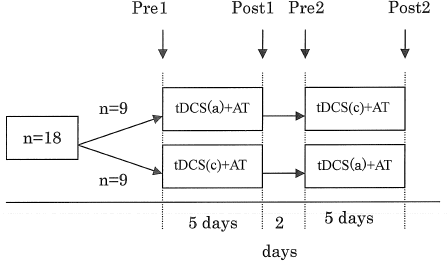
This study used a randomized, double-blinded, crossover design. All subjects received two interventions, comprising either anodal tDCS to the affected hemisphere with AT (tDCS(a)+AT) or cathodal tDCS to the unaffected hemisphere with AT (tDCS(c)+AT) for 5 days in a cross-over manner (Fig. 1). The end of one intervention was separated from the start of the next intervention by two days, to minimize any carry-over effect.
Fig. 1. Experimental design. Transcranial direct current stimulation (tDCS) (a) + arm training (AT): anodal tDCS on the affected hemisphere with Arm Trainer (AT) training; tDCS (c) + AT; cathodal tDCS on the unaffected hemisphere with AT training.
Subjects
Subjects comprised 18 patients (14 men, 4 women) ≥ 18 years old with long-term, moderate-to-severe motor impairment of an upper limb (Fugl-Meyer Assessment for the upper limb (FMUL) score < 44) from a first stroke that had occurred ≥ 6 months before the study. Exclusion criteria were: previous stroke, preceding epilepsy, severe cognitive impairments, serious cardiac or orthopaedic problems, or metallic implants within the brain. Mean age was 61.1 years, and the mean time between stroke and this intervention was 4.4 years (Table I). Stroke subtype was haemorrhagic in 11 cases and ischaemic in 7 cases. Written informed consent was obtained from all subjects before inclusion in the study, and the study protocols were approved by the university ethics committee.
|
Table I. Baseline characteristics of subjects (n = 18) |
|
|
n |
|
|
Age, years, mean [median] (SD) |
61.1 [58.5] (10.0) |
|
Sex, n (%) |
|
|
Male |
14 (78) |
|
Female |
4 (22) |
|
Stroke subtype, n (%) |
|
|
Haemorrhagic |
11 (61) |
|
Ischaemic |
7 (39) |
|
Affected side, n (%) |
|
|
Left |
12 (67) |
|
Right |
6 (33) |
|
Time since stroke, years, mean [median] (SD) |
4.4 [4] (3.4) |
|
FMUL, mean [median] (SD) |
|
|
Total score |
22.6 [18] (15.9) |
|
Hand score |
3.8 [1] (4.4) |
|
MAS, mean [median] (SD) |
|
|
Elbow |
2.6 [2.5] (1.2) |
|
Wrist |
3.2 [3] (1.0) |
|
Finger |
3.1 [3] (1.2) |
|
MAL, mean [median] (SD) |
1.5 [0] (2.7) |
|
FMUL: Fugl-Meyer Assessment of the upper limb; MAS: modified Ashworth scale; MAL: amount of use in the Motor Activity Log; SD: standard deviation. |
|
Study interventions
AT was performed using the Bi-Manu-Track robotic arm trainer (Reha-Stim, Berlin), which enables the mirror-like practice of two movement cycles: forearm pro-supination, and wrist flexion-extension (8, 9). The patient sat at a height-adjustable table with elbows bent at 90º and forearms in the mid-position in an arm trough. Each hand grasped a handle, with a strap holding the paretic hand in place. Two computer-controlled modes were selected: (i) passive-passive (PP), with both arms moved by the machine; and (ii) active-passive (AP), with the non-affected arm driving the affected side. Within one session, subjects practiced 500 forearm cycles (PP = 100, AP = 400), and 500 wrist cycles (PP = 100, AP = 400), for a total of 1000 cycles (or 2000 repetitions).
Direct current was transferred by a saline-soaked pair of surface sponge electrodes (35 cm2) and delivered by a specially designed battery-driven, constant current stimulator (DC Stimulator Plus; neuroConn, Ilmenau, Germany). To stimulate the primary cortex (M1), one electrode was placed over C3/C4 (International 10/20 Electroencephalogram System), approximately corresponding to the location of the motor cortex. The other electrode was placed over the contralateral supraorbital area. For anodal stimulation, the anode electrode was placed over M1 of the affected hemisphere and the cathode electrode over the contralateral supraorbital areas, whereas the cathode was placed over M1 of the unaffected hemisphere and the anode over the contralateral supraorbital area for cathodal stimulation. To hide the position of the electrodes for both subjects and therapists, we set the electrodes from behind the subject and bandaged the whole head of the subject without the therapist being present, before the commencement of the intervention. For active stimulation, patients received 1 mA of tDCS for the first 10 min during AT training.
Outcome measures
Trained evaluators who were unaware of study group assignments assessed patients after randomization. The outcome was a change in FMUL, modified Ashworth scale (MAS) and Motor Activity Log (MAL) during the intervention, compared with the baseline value before the intervention.
The FMUL measures motor and sensory impairment in the upper limbs (10). The scale ranges from 0 to 66, with higher scores indicating better functioning. MAS measures spasticity (muscle tone) on a scale of 0–5, with higher scores indicating more severe spasticity (11). The MAL is a structured interview that elicits information about 14 activities of daily living, rating quality (Quality of Movement (QOM) scale) and frequency (Amount of Use (AOU) scale) in use by the hemiplegic arm to accomplish each ADL. Both scales are anchored at 6 points, and total score for the scale is derived as the mean of the item scores. Either the QOM or AOU scale alone can also be applied. As subjects in this study showed moderate-to-severe impairment, QOM was not considered applicable and only AOU was determined (12).
These evaluations were made at baseline (Pre1, Pre2) and immediately after each session of intervention (Post1, Post2) by an occupational therapist who was blinded to intervention allocation.
Statistical analyses
Outcomes for analysis were changes in FMUL, MAS and MAL. Analyses were carried out using JMP version 8.0 statistical software (SAS Institute, Cary, NC, USA). To compare the outcome measures that were ordinal data from Pre with those from Post, Wilcoxon signed-rank tests were used for each session. Considering that each patient underwent two different stimulation conditions (tDCS(a) and tDCS(c)) and had different orders of stimulation (1st and 2nd sessions), Wilcoxon signed-rank test was used to test whether the stimulation condition and the order, respectively, had a significant effect of on the primary outcome. Values of p < 0.05 were considered significant.
RESULTS
Table I summarizes the demographics and characteristics of the subjects. All patients were right-handed and had experienced stroke ≥ 6 months before the study. In all cases, tDCS+AT was well tolerated and no adverse effects related to application of tDCS + AT were observed.
To test whether tDCS + AT training was associated with a significant motor improvement, we performed a Wilcoxon signed-rank test of outcomes (i.e. improvement from baseline for FMUL, MAS and MAL) for each stimulation condition (Table II). These analyses showed small but significant improvement effects on FMUL and MAS (elbow, wrist and finger) with both stimulations, but no improvement in MAL.
Finally, we tested whether stimulation condition (tDCS(a) and tDCS(c)) was associated with motor performance, considering the order of stimulation (1st and 2nd). Comparing motor improvements between 1st and 2nd sessions, there were no statistical difference. This analysis showed no effect of stimulation order on the outcomes. As for stimulation condition, only tDCS(c) + AT was associated with a significant improvement in MAS for the finger (Table II). According to further subgroup analysis, in patients with an affected right hemisphere, mean improvement in finger MAS was significantly larger with tDCS(c) of the unaffected left hemisphere than with tDCS(a) of the affected right hemisphere (median –1 vs 0; Wilcoxon signed-rank test, p = 0.03). In patients with an affected left hemisphere, improvements were similar for tDCS(c) of the unaffected right hemisphere and tDCS(a) of the affected left hemisphere. The effects of tDCS thus differed according to laterality of the affected hemisphere.
|
Table II. Results for assessment in anodal and cathodal transcranial direct current stimulation (tDCS) with Arm Trainer (AT) training (n = 18) |
||||
|
tDCS(a)+AT |
tDCS(c)+AT |
|||
|
Pre Mean [median] (SD) |
Post Mean [median] (SD) |
Pre Mean [median] (SD) |
Post Mean [median] (SD) |
|
|
FMUL |
||||
|
Total |
23.2 [19] (16.6) |
24.6 [23] (17.0)a |
23.6 [18] (16.7) |
24.6 [21.5] (17.4)a |
|
Hand |
3.3 [1] (4.3) |
3.8 [1.5] (4.9) |
3.7 [1.5] (4.9) |
3.8 [1.5] (4.9) |
|
MAS |
||||
|
Elbow |
2.4 [2.5] (1.1) |
2.1 [2] (1.1)a |
2.5 [2.5] (1.2) |
2.0 [2] (1.1)a |
|
Wrist |
3.0 [3] (1.1) |
2.4 [2.5] (1.3)a |
2.9 [3] (1.1) |
2.4 [2.5] (1.3)a |
|
Finger |
2.8 [3] (1.3) |
2.3 [3] (1.4)a |
2.9 [3] (1.2) |
2.1 [2] (1.4)ab |
|
MAL |
1.6 [0] (2.7) |
1.7 [0] (2.8) |
1.6 [0] (2.8) |
1.7 [0] (3.2) |
|
ap < 0.05 by Wilcoxon signed-rank test, pre vs post. bp < 0.05 by Wilcoxon signed-rank test for improvement between pre and post, tDCS(a)+AT vs tDCS(c)+AT. FMUL: Fugl-Meyer Assessment of the upper limb; MAS: modified Ashworth scale; MAL: amount of use in the Motor Activity Log; SD: standard deviation. |
||||

DISCUSSION
We showed that both tDCS(a)+AT and tDCS(c)+AT could achieve a limited but a similar magnitude of motor improvement in the FMUL and MAS for the affected arm in chronic stroke patients. This finding strengthens not only the results of the preliminary pilot study by Hesse et al. (7), which found that anodal tDCS to the affected hemisphere with AT for the affected arm in subacute stroke patients improved motor function, but also supports the use of cathodal stimulation to the unaffected hemisphere as having similar effects to anodal stimulation of the affected hemisphere in chronic stroke patients (13). The finding that cathodal stimulation of the contralateral hemisphere could yield motor improvements similar to anodal stimulation of the affected hemisphere in combined therapy is important. Although significant motor improvement in FMUL and MAS was seen with the combined intervention, upper-limb function in daily activities as evaluated by MAL was unchanged. As our subjects showed severe impairment of the upper limbs, the magnitude of change in Fugl-Meyer score might have been small to allow functional activity. We agree with Kwakkel et al. (3), who showed a significant improvement in upper limb motor function using upper arm robotics after stroke, even though no significant improvement was found in ADL function. However, the important finding is that, even in chronic stroke patients with severe upper limb dysfunction, this combined therapy showed effects on motor function. We thought that these effects were due to both the intensive bilateral, repetitive practice of AT and the activation of motor neurones by tDCS.
Comparing anodal and cathodal stimulations in combined therapy, distal spasticity was significantly improved with cathodal stimulation compared with anodal stimulation in patients with an affected right hemisphere. Conversely, no significant differences in motor improvement or spasticity were observed between stimulation of the affected or unaffected hemisphere in patients with an affected left hemisphere. AT reportedly improves spasticity for distal rather than proximal upper limb after stroke (7–9). The use of cathodal stimulation of the unaffected hemisphere was based on the hypothesis that this stimulation would suppress activity locally and release the damaged hemisphere from possible excessive transcallosal inhibition, potentially allowing some functional improvement. Our findings were similar to those reported by Fregni et al. (14) that mean improvement of motor performance with cathodal tDCS of the unaffected hemisphere was higher when the left hemisphere was inhibited in chronic stroke patients. Transcallosal inhibition by the unaffected hemisphere could differ according to whether the right or left hemisphere is affected.
Some limitations need to be considered when interpreting the results of this study. First, compared with patients in previous studies, our subjects showed more severe impairment for a longer period of time after stroke, and the duration of intervention was shorter. These factors may have contributed to our findings that tDCS + AT provided a smaller benefit with respect to motor function, such as FMUL scores. A second limitation was the heterogeneity of subjects, given the inclusion of both haemorrhagic and ischaemic strokes. However, the influence on outcome measures was considered minimal in this study, since improvements in outcome measures were not associated with stroke subtype. Thirdly, inclusion of a sham stimulation group as controls might have facilitated interpretation of the results. Despite these limitations, the nature of the study as a randomized, controlled trial strengthens the significance of the results, although the crossover design reduced the quality score.
In conclusion, this study demonstrated the limited effects of therapy combining tDCS and AT in achieving significant improvement in the hemiplegic arm of chronic stroke patients. However, a difference was seen with the polarity of tDCS, with inhibition of the unaffected left hemisphere (i.e. unaffected dominant hemisphere) by cathodal tDCS improving distal spasticity more than anodal tDCS of the affected hemisphere in patients with a right hemispheric lesion. Future studies are warranted to identify the effects of differences in tDCS polarity in combination therapy using a larger population.
ACKNOWLEDGEMENTS
The authors would like to thank Noriaki Kato, MD, Akiko Hachisuka, MD, Kosei Yoshikawa, MD, Hideaki Itoh, MD and Yoko Nakayama for their assistance. This study was partially supported by a Grant-in-Aid for Scientific Research (C) (21500504).
REFERENCES
