Helena Gustafsson, MSc1, Peter Nordström, MD, PhD2, Stefan Stråhle, MD3 and Anna Nordström, MD, PhD3
From the 1Department of Surgical and Perioperative Sciences, Sports Medicine, 2Department of Community Medicine and Rehabilitation, Geriatrics and 3Department of Community Medicine and Rehabilitation, Rehabilitation Medicine, Umeå University, Umeå, Sweden
OBJECTIVE: To investigate relationships between individuals’ socioeconomic situations and quality of life in working-aged subjects with Parkinson’s disease.
METHODS: A population-based cohort comprising 1,432 people with Parkinson’s disease and 1,135 matched controls, who responded to a questionnaire. Logistic regression analysis was performed to identify factors associated with life satisfaction and likelihood of employment.
RESULTS: In multivariate analyses, Parkinson’s disease was associated with an increased risk of dissatisfaction with life (odds ratio (OR) = 5.4, 95% confidence interval (95% CI) = 4.2–7.1) and reduced likelihood of employment (OR = 0.30, 95% CI = 0.25–0.37). Employers’ support was associated with greater likelihood of employment (p < 0.001). Twenty-four percent of people with Parkinson’s disease for ≥ 10 years remained employed and 6% worked full-time. People with Parkinson’s disease also more frequently experienced work demands that exceeded their capacity; this factor and unemployment independently correlated with greater risk of dissatisfaction with life (both p < 0.05).
CONCLUSION: People with Parkinson’s disease have an increased risk of dissatisfaction with life. Employment situation is important for general life satisfaction among working-aged individuals. People with Parkinson’s disease appear to find it difficult to meet the challenge of achieving a balanced employment situation.
Key words: Parkinson’s disease; life satisfaction; work.
J Rehabil Med 2014; 46: 00–00
Correspondence address: Anna Nordström, Department of Community Medicine and Rehabilitation, Rehabilitation Medicine, SE-90187 Umeå University, Sweden. E-mail: anna.nordstrom@idrott.umu.se
Accepted Jun 10, 2014; Epub ahead of print Sep 30, 2014
Introduction
Parkinson’s disease (PD) is the second most common neurodegenerative disease, with an estimated prevalence of 0.3% in industrialized countries (1). Although PD occurs most commonly in older age, approximately 30% of patients are diagnosed at an age of < 65 years (2) and a substantial proportion of them are affected in their 30s (3). Several studies have used different methods, most commonly focusing on clinical variables, to investigate the quality of life (QoL) of people with PD. The influences of other factors are less well known, although studies examining demographic variables have found that symptoms and disabilities alone do not explain the degree of impact of PD on QoL (4–6). Attention has been drawn to the importance of social functioning in preserving QoL, and people with young-onset PD have been found to perceive worse QoL than have those with later-onset PD, adjusted for disease severity (7, 8). Challenges associated with being active in the labour market are likely to be important, and most people with PD continue working for only a few years after diagnosis (3, 9–11). Such premature cessation of employment has a distinct economic impact (12). Nevertheless, few studies have explored work-related questions from the patient’s perspective or evaluated possible measures to improve the situation (3, 10, 11, 13). The availability of adjustment in work tasks and supportive attitudes from employers have been reported to be associated with a longer continuation in employment after PD diagnosis (3, 10). The reduction in working hours is hypothesized to be of value in prolonging the duration of employment after disease onset, although no significant association between this adjustment and the time of employment cessation has been proven (11, 13). Furthermore, most studies have examined small numbers of participants, usually recruited through specialist clinics or PD organizations; thus, the representativeness of their findings at the population level is uncertain (3, 10, 11).
The aim of this study was to investigate associations between socioeconomic situation and subjective QoL for people with PD in a large population-based cohort, with particular attention to work-related challenges and possible measures for improvement.
Methods
Study design and participants
The PD cohort for this population-based study was identified through the National Patient Register (NPR), based on subjects’ unique personal identification numbers. This register, administered by the Swedish National Board of Health and Welfare, cover all specialist health care in Sweden. The accuracy of diagnoses in the NPR has been validated previously, most recently against national quality registries for several diseases; positive predictive values of 85–95% have been documented for most diagnoses (International Classification of Diseases (ICD) code, 3-digit level) (14). Individuals eligible for inclusion in this study were in the age range 18–67 years, to match the official retirement age in Sweden.
An overview of the inclusion process is presented in Fig. 1. Based on healthcare contacts during 2007–2011, the sampling frame identified 5,763 subjects diagnosed with PD (ICD-10 code G20). The data were checked against the National Registry of the Total Population (RTP), and after exclusion of those who had died, emigrated, or were outside the age limits, 3,064 subjects remained to be considered for inclusion. Of these individuals, 2,002 persons with the most recent healthcare contacts were selected for inclusion. The RTP was used to form the control group by randomly selecting 1 age- and sex-matched control subject for each subject in the case group. Permission for the study was obtained from the research ethics committee of Umeå University.

Data collection and instruments
Data were collected in 2012 using a postal survey sent to all eligible participants. The questionnaire comprised 44 items, several of which had sub-queries. When a question was not relevant to all participants, instructions to go to the next relevant section were provided. The survey was separated into parts regarding the “present” and “past” (before diagnosis for people with PD, 10 years ago for control subjects).
The questionnaire was designed to explore several aspects of respondents’ life situations, including factors descriptive of living conditions, family, vocational situation, leisure, and health, as well as self-assessments of well-being from different points of view. Subjective QoL was investigated using 4 domains (life as a whole, employment situation, financial situation, and leisure) from the Life Satisfaction Questionnaire 11 (LiSat-11) (15), graded from 1 (very dissatisfied) to 6 (very satisfied). Work characteristics were explored using 11 questions from Karasek’s Job Content Questionnaire (16). The prevalence of other diseases was investigated by 1 question including yes/no sub-queries for 11 specific, common health issues and “any other disease” (Table I). Participants who had reduced work time or quit work because of PD were asked to rank their symptoms in relation to interference with work on a scale of 1 to 10, with rankings of 1–3 interpreted as “strongly interfering”, rankings of 4–6 as “moderately interfering”, and rankings of 7–10 as “slightly interfering.” Questions about vocational rehabilitation specified 8 operators (trade union; foreman/boss; company health services; public social insurance; public employment services; primary healthcare; PD treatment responsible doctor; vocational rehabilitation unit) followed by a final question on “other actor”. Each question had 5 response alternatives; 4 levels of support ranging from “I have not received help, despite need” to “I have received very much help”, alternatively “I have not been in need of help from this actor”. In the final analyses, foreman/boss and company health services were pooled into 1 category (employer).The overall response rate was 64.2% (n = 2,567; people with PD, 71.5%; control subjects, 56.6%). Lower response rates were found among subjects in the PD and control groups who were younger, unmarried, and/or immigrants; resided in large cities; and/or had lower education and/or income levels.
|
Table I. Summary of demographics of study participants |
|||||
|
|
PD |
Control |
|||
|
Men |
Women |
Men |
Women |
||
|
Total, n |
917 |
515 |
687 |
448 |
|
|
Age, years, median (quartile range; QR) |
63 (58–65) |
63 (57–65) |
63 (58–66) |
63 (57–65) |
|
|
Years since PD diagnosis, median (QR) |
6.0 (3.25–10) |
7.0 (3–11) |
– |
– |
|
|
Age at diagnosis, years, median (QR) |
55 (49–59) |
54 (49–59) |
– |
– |
|
|
Education level, n (%) |
|||||
|
Primary school |
233 (25.4) |
145 (28.2) |
176 (25.6) |
109 (24.3) |
|
|
Vocational school |
167 (18.2) |
67 (13.0) |
126 (18.3) |
55 (12.3) |
|
|
Secondary school |
210 (22.9) |
121 (23.5) |
151 (22.0) |
107 (23.9) |
|
|
University |
293 (32.0) |
175 (34.0) |
228 (33.2) |
174 (38.8) |
|
|
Missing |
14 (1.5) |
7 (1.4) |
6 (0.9) |
3 (0.7) |
|
|
Occupation, n (%) |
|
|
|||
|
Work, full-time |
183 (20.0) |
54 (10.5) |
347 (50.5) |
175 (39.1) |
|
|
Work, part-time |
195 (21.3) |
110 (21.4) |
103 (15.0) |
94 (21.0) |
|
|
Disability pension, full-time |
415 (45.3) |
240 (46.6) |
171 (24.9) |
102 (22.8) |
|
|
Disability pension, part-time |
83 (9.4) |
57 (11.1) |
22 (3.2) |
16 (3.6) |
|
|
Unemployed |
49 (5.3) |
20 (3.9) |
35 (5.1) |
17 (3.8) |
|
|
Relationship status, n (%) |
|
|
|||
|
Married/cohabiting |
718 (78.3) |
378 (73.4) |
539 (78.5) |
327 (73.0) |
|
|
Single |
111 (12.1) |
60 (11.7) |
90 (13.1) |
52 (11.6) |
|
|
Divorced |
62 (6.8) |
30 (5.8) |
37 (5.4) |
35 (7.8) |
|
|
Widowed |
12 (1.3) |
32 (6.2) |
10 (1.5) |
21 (4.7) |
|
|
Missing |
14 (1.5) |
15 (2.9) |
11 (1.6) |
13 (2.9) |
|
|
Children, yes, n (%) |
635 (69.2) |
378 (73.4) |
536 (78.0) |
375 (83.7) |
|
|
Income, Euro, thousands, mean (SD) |
36.6 (21.4) |
27.5 (16.7) |
41.7 (32.9) |
31.1 (14.2) |
|
|
Other diseases, n (%) |
|
|
|
|
|
|
Angina pectoris |
88 (9.6) |
26 (5.0) |
79 (11.5) |
21 (4.7) |
|
|
Back pain |
294 (32.1) |
190 (36.9) |
173 (25.2) |
116 (25.9) |
|
|
Psychiatric disease |
35 (3.8) |
20 (3.9) |
8 (1.2) |
9 (2.0) |
|
|
Diabetes |
63 (6.9) |
20 (3.9) |
67 (9.8) |
24 (5.4) |
|
|
Allergy |
109 (11.9) |
81 (15.7) |
99 (14.4) |
86 (19.2) |
|
|
Skin disease |
79 (8.6) |
29 (5.6) |
48 (7.0) |
30 (6.7) |
|
|
Hypertension |
177 (19.3) |
93 (18.1) |
212 (30.9) |
106 (23.7) |
|
|
Ulcers/gastritis |
44 (4.8) |
46 (8.9) |
33 (4.8) |
43 (9.6) |
|
|
Cancer |
27 (2.9) |
16 (3.1) |
22 (3.2) |
14 (3.1) |
|
|
Pulmonary disease |
11 (1.2) |
8 (1.6) |
11 (1.6) |
15 (3.3) |
|
|
Bowel disease |
19 (2.1) |
27 (5.2) |
13 (1.9) |
15 (3.3) |
|
|
Other |
156 (17.0) |
108 (21.0) |
53 (7.7) |
39 (8.7) |
|
The following additional data were collected from the RTP and the National Registry of Income and Taxation: sex, age, marital status, country of birth, citizenship, municipality, and income.
Statistical analysis
SPSS® software (version 21 for Windows; IBM) was used for statistical analyses. Descriptive statistics for categorical data are presented as absolute numbers and percentages. Differences between groups (PD and control) were investigated with the χ2 test, t-test, or Mann-Whitney U-Test (for data that was not normative). A p-value < 0.05 was considered significant. Statistics for occupation type are based on cross-sectional data reported in the survey. Disease duration data are based on the year of PD diagnosis (drawn from the survey), excluding the presence of symptoms before diagnosis. Binary logistic regression analysis was used to investigate independent factors associated with 2 outcomes: satisfaction with life and the opportunity to work. The outcome variables were dichotomized as follows: dissatisfaction with life was defined as a score ≤ 3 (defining any level of dissatisfaction) in the global domain of the 6-graded LiSat-11 scale (15) and work was defined as any extent of work (vs no work). Analyses including general factors were performed for the whole cohort and for each group (PD and control) separately. Additional analyses including disease-specific factors were performed for the PD group. Odds ratios (ORs) and 95% confidence intervals (95% CI) were calculated for each independent factor.
Results
Demographic data
The study population comprised 1,432 people with PD (median age 63 years; quartile range 58–65 years) and 1,135 control subjects (median age 63 years; quartile range 58–66 years) (p = 1.00). For subjects with PD, the median time since diagnosis was 6 (quartile range 3–10) years. Twelve participants with PD were ≤ 40 years of age and 95 were ≤ 50 years of age.
The number of employed subjects was lower among people with PD than among controls (37.8% (n = 542) vs 63.3% (n = 719) p < 0.001), while part-time work was more common among people with PD (21.3% (n = 305) vs 17.4% (n = 197) p < 0.05). More people with PD than control subjects received disability pensions (55.5% (n = 795) vs 27.4% (n = 311), p < 0.001), and the mean income was lower among people with PD (Table I). The percentages of subjects with PD in full- and part-time employment were 28.6% and 24.3%, respectively, within 5 years of diagnosis (n = 420); 15.2% and 23.5%, respectively, 5–9 years after diagnosis (n = 455); and 6.1% and 18.2%, respectively, ≥ 10 years after diagnosis (n = 362).
Life satisfaction and employment situation
Scores in all 4 LiSat-11 domains were significantly lower among people with PD than among control subjects (p < 0.001). (Fig. 2). For “life as a whole” 37.6% (n = 538) of people with PD and 8.5% (n = 97) of control subjects expressed dissatisfaction (score ≤ 3); for “working situation” 38.2% (n = 547) of people with PD and 14.7% (n = 167) of control subjects reported dissatisfaction (both p < 0.001).
Further analysis revealed that more people with PD than control subjects experienced work demands that exceeded their capacity (36.2% (n = 196) vs 13.2% (n = 95); p < 0.001), with no significant difference between people employed full- and part-time within groups. Among those in part-time employment, more control subjects than people with PD perceived the capacity to work more (38.6% (n = 76) vs 9.8% (n = 30); p < 0.001).
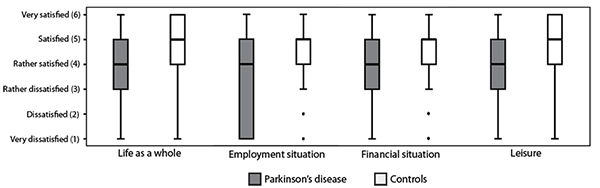
Fig. 2. Life satisfaction scores by group (p < 0.001 for all).
Impact of working situation on satisfaction with life as a whole
Logistic regression was used to investigate independent associations between the outcome of dissatisfaction with life as a whole and exposure to several demographic, social and health-related factors (Table II). In the model including the whole cohort, PD was found to be the strongest risk factor for dissatisfaction with life as a whole (OR = 5.4, 95% CI = 4.2–7.1). Significant work-related risk factors were unemployment (OR = 3.4, 95% CI = 2.5–4.6) and the perception that work demands exceeded one’s capacity (OR = 2.7, 95% CI = 1.8–2.9), both compared with an employment situation equal to one’s capacity. In a model including only the PD group, an additional significant association with longer disease duration was found (OR = 1.04/year, 95% CI = 1.02–1.07).
|
Table II. Models evaluating risk of dissatisfaction with life as a whole |
||||||
|
|
Whole cohort OR (95% CI) |
p |
Control subjects OR (95% CI) |
p |
People with PD OR (95% CI) |
p |
|
Age (OR per year) |
0.99 (0.97–1.01) |
0.17 |
0.96 (0.90–1.01) |
0.08 |
0.99 (0.96–1.01) |
0.22 |
|
Gender |
|
|
|
|
|
|
|
Women |
1.00 |
|
1.00 |
|
1.00 |
|
|
Men |
1.49 (1.18–1.88) |
0.001 |
2.72 (1.57–4.69) |
< 0.001 |
1.17 (0.89–1.55) |
0.27 |
|
Family |
|
|
|
|
|
|
|
Married |
1.00 |
|
1.00 |
|
1.00 |
|
|
Single |
1.91 (1.39–2.64) |
< 0.001 |
1.98 (1.05–3.75) |
0.04 |
1.73 (1.13–2.66) |
0.01 |
|
Divorced |
1.98 (1–33–2.95) |
0.001 |
0.84 (0.33–2.13) |
0.71 |
1.81 (1.09–3.04) |
0.02 |
|
Widowed |
1.88 (1.06–3.32) |
0.03 |
3.39 (1.03–11.2) |
0.04 |
1.94 (0.97–3.89) |
0.06 |
|
No children |
1.00 |
|
1.00 |
|
1.00 |
|
|
Have children |
0.89 (0.70–1.14) |
0.37 |
1.10 (0.59–2.02) |
0.77 |
0.83 (0.59–1.17) |
0.30 |
|
Education level |
|
|
|
|
|
|
|
Primary school |
1.00 |
|
1.00 |
|
1.00 |
|
|
Vocational school |
0.87 (0.63–1.20) |
0.40 |
0.42 (0.19–0.90) |
0.03 |
1.07 (0.72–1.60) |
0.73 |
|
Secondary school |
0.97 (0.71–1.31) |
0.82 |
0.72 (0.37–1.41) |
0.34 |
1.09 (0.74–1.59) |
0.67 |
|
University |
0.84 (0.63–1.12) |
0.23 |
0.72 (0.39–1.35) |
0.31 |
0.79 (0.55–1.13) |
0.20 |
|
Working situation |
|
|
|
|
|
|
|
Employed, work equal to one’s capacity |
1.00 |
1.00 |
|
1.00 |
|
|
|
Employed, work beyond one’s capacity |
2.70 (1.84–3.95) |
< 0.001 |
2.27 (0.86–5.96) |
0.10 |
2.80 (1.78–4.41) |
< 0.001 |
|
Employed, capacity to work more |
0.84 (0.38–1.87) |
0.67 |
1.13 (0.35–3.63) |
0.84 |
0.67 (0.22–2.17) |
0.53 |
|
Unemployed |
3.36 (2.48–4.56) |
< 0.001 |
3.63 (1.83–7.22) |
< 0.001 |
2.77 (1.90–4.05) |
< 0.001 |
|
Income (OR per SD increase) |
0.79 (0.70–0.89) |
< 0.001 |
0.57 (0.44–0.74) |
< 0.001 |
0.90 (0.77–1.04) |
0.15 |
|
Parkinson’s disease |
5.44 (4.19–7.07) |
< 0.001 |
|
|
|
|
|
Years with PD (OR per year) |
– |
|
– |
|
1.04 (1.02–1.07) |
0.001 |
|
Comorbidities |
|
|
|
|
|
|
|
Angina pectoris |
1.54 (1.07–2.21) |
0.02 |
1.70 (0.83–3.49) |
0.15 |
1.70 (1.07–2.71) |
0.03 |
|
Back pain |
1.25 (1.00–1.56) |
0.05 |
2.20 (1.34–3.63) |
0.002 |
1.14 (0.87–1.49) |
0.36 |
|
Psychiatric disease |
1.80 (1.03–3.15) |
0.04 |
7.27 (2.18–24.3) |
0.001 |
1.68 (0.83–3.39) |
0.15 |
|
Diabetes |
1.33 (0.88–2.00) |
0.18 |
1.51 (0.73–3.14) |
0.27 |
1.35 (0.79–2.32) |
0.27 |
|
Allergy |
1.01 (0.74–1.37) |
0.96 |
0.61 (0.30–1.27) |
0.19 |
1.10 (0.75–1.59) |
0.63 |
|
Skin disease |
1.24 (0.84–1.83) |
0.29 |
0.74 (0.28–1.97) |
0.54 |
1.26 (0.78–2.03) |
0.35 |
|
Hypertension |
1.07 (0.83–1.39) |
0.61 |
1.01 (0.59–1.72) |
0.97 |
1.11 (0.80–2.03) |
0.35 |
|
Ulcers/gastritis |
2.02 (1.34–3.04) |
0.001 |
1.82 (0.80–4.15) |
0.15 |
2.23 (1.32–3.77) |
0.003 |
|
Cancer |
2.01 (0.97–4.14) |
0.06 |
1.45 (3.44–6.11) |
0.61 |
3.08 (1.10–8.62) |
0.03 |
|
Pulmonary disease |
0.74 (0.26–2.11) |
0.57 |
1.07 (0.22–5.20) |
0.94 |
1.43 (0.24–8.54) |
0.69 |
|
Bowel disease |
1.32 (0.75–2.35) |
0.33 |
2.26 (0.71–7.23) |
0.17 |
1.03 (0.52–2.03) |
0.94 |
|
Other |
1.41 (1.07–1.85) |
0.01 |
2.22 (1.13–4.34) |
0.02 |
1.29 (0.93–1.78) |
0.12 |
|
PD: Parkinson’s disease; OR: odds ratio; CI: confidence interval; SD: standard deviation. |
||||||
Challenges and help with employment situation for people with Parkinson’s disease
Overall, 59.1% (n = 846) of people with PD reported that they had reduced work time or quit work because of the disease; in this group, the most common symptoms reported to strongly interfere with work were “stiffness and/or slowness of movement” (44.5%, n = 377), “stress intolerance” (35.6%, n = 301), “sleep disturbance/ fatigue” (23.8%, n = 201) and “tremor” (22.7%, n = 192).
Only 12.8% (n = 183) of people with PD reported that their employment situation had not changed. Support related to the employment situation had been provided in most cases by doctors responsible for PD treatment; 60.7% (n = 869) of people with PD had received help from doctors and 5.1% (n = 73) reported a lack of help from this source. Employers had provided help to 33.7% (n = 483) of people with PD, and 14.4% (n = 206) reported that they had not received the help needed from employers. Help from a vocational rehabilitation unit was received by 30.8% (n = 441) of people with PD, and requested but not received by 14.7% (n = 210) of this group.
Factors affecting the opportunity to work
Logistic regression analyses adjusted for confounders were performed to identify independent factors related to the opportunity to work (Table III). In the model including the whole cohort, having PD was associated with a significantly reduced chance to work (OR = 0.30, 95% CI = 0.25–0.37). Among people with PD, additional significant factors were disease duration (OR = 0.90/year, 95% CI = 0.87–0.92) and receipt of vocational rehabilitation support from the employer (some help: OR = 3.0, 95% CI = 1.9–4.7; much help: OR = 3.2, 95% CI = 1.9–5.3), compared with not receiving the help needed.
|
Table III. Models evaluating likelihood of employment |
||||||
|
|
Whole cohort OR (95% CI) |
p |
Control subjects OR (95% CI) |
p |
People with PD OR (95% CI) |
p |
|
Age (OR per year) |
0.86 (0.84–0.87) |
< 0.001 |
0.77 (0.73–0.81) |
< 0.001 |
0.89 (0.87–0.92) |
< 0.001 |
|
Gender |
|
|
|
|
|
|
|
Women |
1.00 |
|
1.00 |
|
1.00 |
|
|
Men |
1.60 (1.32–1.95) |
< 0.001 |
1.57 (1.15–2.14) |
0.004 |
1.58 (1.19–2.11) |
0.002 |
|
Family |
|
|
|
|
|
|
|
Married |
1.00 |
|
1.00 |
|
1.00 |
|
|
Single |
0.92 (0.68–1.24) |
0.57 |
0.88 (0.55–1.41) |
0.59 |
1.23 (0.77–1.98) |
0.39 |
|
Divorced |
0.81 (0.56–1.17) |
0.25 |
0.78 (0.42–1.43) |
0.42 |
1.15 (0.66–1.98) |
0.62 |
|
Widowed |
0.60 (0.34–1.07) |
0.08 |
0.66 (0.29–1.49) |
0.32 |
0.57 (0.24–1.37) |
0.21 |
|
No children |
1.00 |
|
1.00 |
|
1.00 |
|
|
Have children |
1.61 (1.27–2.04) |
< 0.001 |
1.51 (1.00–2.27) |
0.04 |
1.92 (1.30–2.84) |
0.001 |
|
Education level |
|
|
|
|
|
|
|
Primary school |
1.00 |
|
1.00 |
|
1.00 |
|
|
Vocational school |
1.20 (0.91–1.59) |
0.21 |
1.24 (0.80–1.93) |
0.33 |
1.12 (0.72–1.74) |
0.61 |
|
Secondary school |
1.44 (1.10–1.89) |
0.009 |
1.10 (0.71–1.69) |
0.68 |
1.59 (1.06–2.39) |
0.03 |
|
University |
1.80 (1.42–2.30) |
< 0.001 |
1.77 (1.22–2.57) |
0.003 |
1.92 (1.33–2.77) |
< 0.001 |
|
Parkinson’s disease |
0.30 (0.25–0.37) |
< 0.001 |
– |
|
– |
|
|
Years with PD (OR per year) |
– |
|
– |
|
0.89 (0.87–0.92) |
< 0.001 |
|
Comorbidities |
|
|
|
|
|
|
|
Angina pectoris |
0.58 (0.41–0.81) |
0.002 |
0.57 (0.34–0.93) |
0.02 |
0.49 (0.28–0.85) |
0.01 |
|
Back pain |
0.70 (0.57–0.86) |
0.001 |
0.53 (0.37–0.73) |
< 0.001 |
0.82 (0.62–1.10) |
0.19 |
|
Psychiatric disease |
0.22 (0.11–0.44) |
< 0.001 |
0.03 (0.01–0.18) |
< 0.001 |
0.34 (0.14–0.81) |
0.02 |
|
Diabetes |
0.69 (0.48–0.99) |
0.04 |
0.76 (0.45–1.27) |
0.29 |
0.59 (0.32–1.08) |
0.08 |
|
Allergy |
1.01 (0.77–1.32) |
0.95 |
1.10 (0.72–1.69) |
0.65 |
0.88 (0.59–1.32) |
0.55 |
|
Skin disease |
0.82 (0.57–1.19) |
0.30 |
1.46 (0.79–2.72) |
0.23 |
0.60 (0.34–1.04) |
0.07 |
|
Hypertension |
1.10 (0.87–1.36) |
0.45 |
0.76 (0.55–1.04) |
0.09 |
1.41 (1.00–1.99) |
0.05 |
|
Ulcers/gastritis |
1.12 (0.77–1.64) |
0.55 |
1.33 (0.73–2.44) |
0.36 |
0.92 (0.52–1.63) |
0.77 |
|
Cancer |
0.77 (0.39–1.53) |
0.45 |
0.61 (0.23–1.61) |
0.32 |
0.53 (0.16–1.83) |
0.32 |
|
Pulmonary disease |
0.42 (0.15–1.15) |
0.10 |
0.61 (0.19–1.94) |
0.41 |
0.18 (0.02–1.99) |
0.16 |
|
Bowel disease |
0.68 (0.38–1.22) |
0.20 |
0.86 (0.32–2.30) |
0.77 |
0.68 (0.30–1.55) |
0.36 |
|
Other disease |
0.68 (0.52–0.89) |
0.004 |
0.53 (0.32–0.90) |
0.02 |
0.72 (0.50–1.03) |
0.07 |
|
Support from employer |
|
|
|
|
|
|
|
Not received help needed |
– |
|
– |
|
1.00 |
|
|
Received some help |
– |
|
– |
|
2.99 (1.89–4.74) |
< 0.001 |
|
Received much help |
– |
|
– |
|
3.19 (1.92–5.29) |
< 0.001 |
|
No need for help |
– |
|
– |
|
1.48 (0.98–2.23) |
0.06 |
|
PD: Parkinson’s disease; OR: odds ratio; CI: confidence interval. |
||||||
Discussion
Subjective QoL, explored in terms of life satisfaction (15), was poorer among people with PD than among control subjects in all areas investigated, and the risk of dissatisfaction with life as a whole was higher for individuals in unfavourable working situations (work demands exceeding capacity or unemployment). The socioeconomic consequences of PD identified in our analyses included lower employment rate and lower income compared with matched control subjects. As income level was not independently related to life satisfaction in the PD group, the importance of employment for QoL appears to extend beyond the financial consequences of reduced work capacity. Among people with PD, the chance to work was greater for those who had received help from their employers.
These findings are not surprising, as several previous studies have described similar consequences of PD, including early retirement, loss of income, and impact on social functioning, in working-aged individuals (3, 10–13, 17). However, few studies have investigated subjects’ perspectives of the socioeconomic consequences of this disease. To our knowledge, this study is the first population-based research to include a group of matched control subjects, enabling direct comparison between groups of demographic data related to subjective well-being and individuals’ experiences of their life situations.
The challenge of achieving a balanced working situation was obviously more difficult for people with PD, many of whom reported that work demands exceeded their capacity, than for control subjects. To our knowledge, no similar data are available for direct comparison with our findings. Several studies have discussed challenges at work for patients with PD (3, 10, 11), but associations with subjective QoL in a wider context have not been thoroughly examined.
In our cohort, people with PD had 70% less likelihood of being in employment than did control subjects, after adjustment for other covariates. As in other studies, our descriptive data indicated that employment rates were low among people with PD within a few years of diagnosis (10–13). Retrospective studies with special attention to this concern have been conducted in Finland (10), the UK (13) and Ireland (11), where employment rates have been <15% at 10 years after PD diagnosis. Data for the first years following diagnosis have varied more, ranging from 15% at 3 years post-diagnosis in the Finnish cohort (10) to 40% at 5 years post-diagnosis in the Irish cohort (11). We found comparatively high employment rates, with 24% of people with PD working at ≥10 years after diagnosis. Differences in social security systems probably have important effects on these rates. In Sweden, support for disabled people in the labour market is part of general policy, “focused on the relation between the person and the environment, rather than personal characteristics.” (18). Work time reduction is commonly regarded as an adjustment with the hypothetical potential to prolong the duration of employment after PD onset (10, 11, 13), but no attempt to identify convincing effects has, to our knowledge, been successful. Schrag & Banks (13) interpreted that abrupt cessation of employment was more common than a reduction in working hours among patients with PD, as the frequency of part-time work among these subjects did not differ from registry-based data from age-matched subjects in the general population. In contrast, we found a higher frequency of part-time work among people with PD than among control subjects. In addition, a substantial number of healthy control subjects worked part-time by choice, whereas very few people with PD who were in part-time employment perceived the capacity to work more. These findings indicate that using purely quantitative data has probably resulted in an underestimation of the difference between groups, and this should be kept in mind when evaluating employment rates without examining subjective variables.
The remarkably large group of individuals still working a decade after onset of PD, among whom the vast majority worked part-time, may indicate that reduction in working hours has been successful in prolonging the opportunity for these individuals to work.
Support received from employer appeared to be of particular importance for the opportunity to stay in work. Previous studies have reported similar findings (3, 10). Our data revealed no clear association between the receipt of help from a vocational rehabilitation unit and the likelihood of employment, but these analyses relied on cross-sectional data, and the lack of significant findings should be interpreted with caution. This form of help may have been provided late in many cases. Only a minority of people with PD in our cohort reported that their employment situation had not been affected. In addition to the cardinal motor symptoms of PD, stress intolerance and fatigue appeared to commonly and strongly interfere with work capacity, which is a finding similar to those of previous studies (10, 11).
The main strengths of the present study are the large PD cohort and the comparison of subjective variables with a control group drawn from the same population. The accuracy of diagnoses listed in Swedish registries can be expected to be high (14), but our goal of recruiting a large, population-based study group prevented clinical evaluations of disease severity. We also lacked access to medical records. Thus, a main limitation of our study is the lack of details for objective variables. We are also aware that the representativeness of the group is not certain, as the response rate introduces a risk of bias. The choice to rely heavily on participant-reported data could be considered another study limitation. However, we expect that most participants were able to provide accurate answers to survey questions regarding the present time. A few survey questions asked participants to provide retrospective information, such as the year of diagnosis, but we expect that the importance of such information to respondents rendered major recall bias unlikely. The complete design of the present survey has not been validated, but life satisfaction was assessed by questions from the LiSat-11 scale; a recognized instrument (15). Furthermore, inaccurate answers in the control group or PD group would probably bias the differences between the groups towards zero. The gender differences found in this study were not specific to people with PD, and could thus be interpreted as a reflection of societal perspectives, rather than disease-specific consequences.
In conclusion, in working-aged individuals in Sweden, PD was associated with an increased risk of dissatisfaction with life. The social factors found to be of significant importance in our cohort were relationship status and working situation, and the importance of work appeared to extend beyond purely financial concerns. An employment situation balanced with one’s capacity appeared to be more difficult to achieve for people with PD; many of these individuals faced early cessation of employment, and a large number of those who remained active in the labour market perceived that work demands exceeded their capacity. However, for individuals affected early in life and worried about their future employment opportunities, it is an encouraging finding that almost 25% of people who had lived with PD for a decade or more remained active in the labour market. Also, the strong correlation between employers’ support and a higher likelihood of employment indicates that a helpful approach to modifiable, non-medical factors may considerably improve the opportunities to remain active in the labour market.
Acknowledgement
This present study was founded by Västerbotten County Council.
References
