Charlotte Rose Wicks, BSc (Hons), PG Cert1, Karl Ward, BSc (Hons), PG Cert1, Amanda Stroud, BA (Hons), DClinPsychol, DipClinNeuropsychol1, Alan Tennant, BA (Hons), Ph.D, MD (honaris causa)2 and Helen L. Ford, BSc (Hons), MD1
From the 1Leeds Centre for Neurosciences, Leeds Teaching Hospitals NHS Trust, Leeds, UK and 2Swiss Paraplegic Research, Nottwil, Switzerland
BACKGROUND: People with multiple sclerosis often stop working earlier than expected. Psychological factors may have an impact on job retention. Investigation may inform interventions to help people stay in work.
OBJECTIVE: To investigate the associations between psychological factors and work instability in people with multiple sclerosis.
METHODS: A multi-method, 2-phased study. Focus groups were held to identify key themes. Questionnaire packs using validated scales of the key themes were completed at baseline and at 8-month follow-up.
RESULTS: Four key psychological themes emerged. Out of 208 study subjects 57.2% reported medium/high risk of job loss, with marginal changes at 8 months. Some psychological variables fluctuated significantly, e.g. depression fell from 24.6% to 14.5%. Work instability and anxiety and depression were strongly correlated (χ2 p < 0.001). Those with probable depression at baseline had 7.1 times increased odds of medium/high work instability, and baseline depression levels also predicted later work instability (Hosmer–Lemeshow test 0.899; Nagelkerke R Square 0.579).
CONCLUSION: Psychological factors fluctuated over the 8-month follow-up period. Some psychological variables, including anxiety and depression, were significantly associated with, and predictive of, work instability. Longitudinal analysis should further identify how these psychological attributes impact on work instability and potential job loss in the longer term.
Key words: multiple sclerosis; psychological factors; psychology; anxiety; depressive disorders; employment; work instability.
J Rehabil Med 2016; 00: 00–00
Correspondence address: Charlotte Wicks, Neurology Research Department, D Floor, Martin Wing, Leeds General Infirmary, Leeds LS1 3EX, UK. E-mail: charlotte.wicks@nhs.net
Accepted Jul 7, 2016; Epub ahead of print Sep 26, 2016
INTRODUCTION
Multiple sclerosis (MS) is an auto-immune disease most commonly diagnosed between the ages of 20 and 40 years, thus affecting people in the earlier stages of their working lives. The estimated prevalence rate of MS in Europe is 80 per 100,000 with a mean annual incidence rate of 3.8 per 100,000 and a male:female ratio of 0.6 (1). Whilst there is geographical variance, it is commonly found that rates of MS in the UK are relatively high.
Common symptoms include fatigue, sensory and motor problems, bladder and bowel problems and cognitive impairment. People with MS (PwMS) have an increased risk of losing their jobs, with a high rate of unemployment or early retirement (2, 3). Studies have shown that 50–80% are unemployed within 10 or more years of disease onset (4). Furthermore, quality of life (QoL) is generally reported to be higher in those who are working (5). In addition, understanding ways to promote job retention would not only improve (or retain) QoL, but also help sustain economic self-sufficiency and reduce the need for long-term welfare.
The significance of physical symptoms on employment status in MS has been described in a number of studies (4, 5). Flensner et al. (5) found that fatigue, physical disability, age, sex and level of education predicted work capacity. However, Pompeii et al. (6) found that physical disability cannot be considered a sole indicator of job retention, while other studies have acknowledged the comorbid role of social, cognitive and psychological factors (3, 7). Thus, symptoms such as anxiety and depression (7), pessimism (8) and self-efficacy (9) have also been shown to be associated with an increased risk of unemployment. Ipsen et al. (10) found that patients with increased physical disability have a higher risk of unemployment when combined with factors such as fatigue, depression and anxiety; and Krokavcova et al. (11) reported that MS patients without anxiety were 2.64 times as likely to be employed. However, Johnson et al. (2) did not show any direct associations between psychological symptoms (e.g. anxiety and depression) and employment status in their large sample of employed and unemployed people (n = 1,125). Only 5 variables were significantly associated with employment status (age, sex, duration of disease, severity of disease (Expanded Disability Status Scale score (EDSS) (12)), and difficulties in thinking), with EDSS being the most significant factor, followed by difficulties in thinking (2).
It is well established that there is a significant level of psychological comorbidity in the MS population, with nearly 1 in 2 PwMS experiencing clinically significant depression in their lifetime, approximately 3 times the prevalence rate in the general population (13). Minden et al. (14) reported elevated lifetime prevalence rates of both anxiety and depression for people with MS relative to the general population (USA) of 36% vs 29% and 54% vs 16%, respectively. There appears to be a consensus that complex patterns of symptoms involving physical, social and psychological factors are all relevant to job retention in MS. For those PwMS who are working, these complex patterns of symptoms present a challenge to maintain their work capacity as the level of “work instability” rises (15). Work instability describes the extent of any mismatch between functional (in)capacity and work demands at a point in time, and its potential impact on job retention/security. It was first identified in the rheumatoid arthritis population and later applied to the MS population by McFadden et al. (16) in their development of an MS-specific scale to screen for risk of sickness absence and job loss. Critical cut-points for the level of risk of job loss was determined though criterion validity, contrasting scale scores with expert judgment (area-under-the-curve analysis).
Despite the importance of maintaining work for PwMS, few studies have included longitudinal data that may reveal more details about the fluctuating condition and its impact on job retention. Thus the current study aims to examine the role of psychological factors associated with maintaining employment in PwMS over time. This analysis looks specifically at the baseline associations, and any fluctuations in those associations in the short-term (i.e. 8 months). This study will continue to measure the impact of psychological factors on work instability for this population of PwMS in paid employment, until a total of 4 time-point data sets have been collected over a 2.5-year period. The basic hypothesis under test is that high levels of negative psychological factors, such as anxiety, depression, pessimism and lack of self-efficacy, will contribute to higher levels of work instability, having adjusted for other factors such as fatigue and mobility limitations.
MATERIAL AND METHODS
Participants were recruited from MS outpatient clinics at Leeds and Bradford hospitals. A 2-phased mixed methodology was employed.
Phase I: Focus group discussions
In 2013, 20 employed people with MS attended 3 focus groups. They were asked to talk about the factors that helped keep them in work. Visual depictions of key ideas taken from the literature (Work, Symptoms, Support, Coping, Performance, Expectations, Sharing, and Future) were used to help start the group discussions, which were recorded and transcribed. Thematic analysis (17) was used to identify key themes from the discussions. Two researchers analysed the data independently and then compared their findings in order to strengthen validity.
Phase II: Self-report questionnaire
The key themes identified from the focus group discussions were used to develop a standardized questionnaire pack made up of relevant measures of psychological variables using validated scales. The scales used address work instability, fatigue, symptoms and impact, anxiety and depression, optimism and pessimism, adjustment to MS, self-efficacy, quality of life and mental well-being, respectively. The final measures used were the Multiple Sclerosis Work Instability Scale (MS-WIS) (16), Neurological Fatigue Index (NFI-MS) (18), the Multiple Sclerosis Impact Scale (MSIS-29) (19), Hospital Anxiety and Depression Scale (HADS) (20), Revised Life Orientation Test (LOT-R) (21), Acceptance of Chronic Health Conditions Scale (ACHC) (22), Unidimensional Self-efficacy Scale for Multiple Sclerosis (USE-MS) (23), Leeds Multiple Sclerosis Quality of Life Scale (Leeds MS-QoL) (24), and the Warwick-Edinburgh Mental Well-being Scale (WEMWBS) (25). Information was also collected on demographic variables including work status, and visual analogue scales for overall health, quality of life, pain and memory and thinking were completed. Participants were asked if they had required assistance to complete the questions.
Inclusion criteria for the prospective study comprised people with a confirmed diagnosis of MS using the McDonald Criteria (26) and who were in paid employment at the time of consent. Written informed consent was obtained prior to study activity and each participant was assigned a study identifier for confidentiality. Participants were encouraged to complete the baseline questionnaire pack during their outpatient clinic visit, on the same day as consent was taken. Those who were unable to complete their questionnaire in clinic, for reasons such as time commitments or fatigue, were given a pre-stamped envelope so that they could complete and return their questionnaire as soon as possible. Month 8 questionnaires were sent out by post with a return envelope provided.
Statistical methods and sample size
For the longitudinal study as a whole, the statistical approach is to analyse trajectories using latent growth curve models (LGCM) within a Structural Equation Modelling (SEM) framework, where the various ordinal questionnaire data will have been transformed via Rasch analysis (27). For SEM a recommendation has been made for a minimum of 200 cases (28). Specifically, for the LGCM, this sample size will give 85% power to reject a null hypothesis of zero slope variance and zero latent covariance (df2) with 4 time-points over the duration of the study (Longitudinal Study designer). This sample size is also consistent with a high degree of precision for the Rasch analysis, where such a sample will be able to calibrate items to within 0.3 logit difficulty with 95% confidence (29).
In the current paper, which addresses only 2 time-points, emphasis is placed upon descriptive statistics and associations, together with an exploration of the changes in proportion of both physical and psychological variables, and baseline predictors for 8-month work instability using logistic regression. With the exception of the HADS Anxiety and Depression scales, which have clinical cut points, and the MS-WIS, which has physical therapy and ergonomic derived cut-points, all other questionnaires are divided into tertiles of their operational range, representing low-medium-high levels of the construct under consideration.
Ethical approval for this study was given by the Yorkshire and Humber Research Ethics Committee.
RESULTS
Phase I: Focus groups
Twenty employed people with MS participated in 3 focus groups in May 2013.
Participants were asked to talk about how and why they were in employment and what helped them stay in work. The key themes identified from these discussions were disclosure, self-management, work environment and illness-related. Some quotes are presented in Fig. 1 that demonstrate these themes.
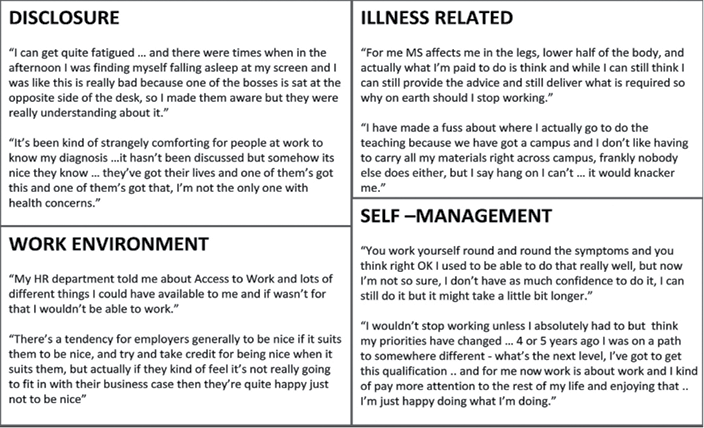

Fig. 1. Main themes emerging from the focus groups. MS: multiple sclerosis.
Phase II: Baseline characteristics and outcomes
A total of 221 employed people with MS from Leeds and Bradford were initially recruited to Phase II of the study. Five subjects left work before completing their baseline questionnaires with 208/216 (96.3%) completing and returning the baseline questionnaire (Table I).
|
Table I. Demographic group characteristics |
||
|
|
Questionnaire Cohort (baseline) n (%) |
Questionnaire Cohort (month 8) n (%) |
|
Questionnaires sent |
216 |
207a |
|
Questionnaires returned (total) |
208 (96.3) |
195 (94.2) |
|
Opted withdrawal |
2 |
3 |
|
Not returned (reason unknown)b |
6 |
9 |
|
Age, years, mean (SD) |
40.6 (9.2) |
– |
|
Female |
155 (74.5) |
144 (73.8) |
|
Male |
53 25.5) |
51 (26.2) |
|
EDSS at baseline |
n/a n/a |
|
|
0–3.0 |
136 (65.4) |
|
|
3.0–6.0 |
38 (18.3) |
|
|
> 6.0 |
34 (16.3) |
|
|
Disease progression |
||
|
RRMS |
183 (88.0) |
171 (87.7) |
|
SPMS |
15 (7.2) |
17 (8.7) |
|
PPMS |
6 (2.9) |
5 (2.6) |
|
Other |
4 (1.9) |
2 (1) |
|
Duration |
||
|
> 10 years |
56 (26.9) |
– |
|
< 10 years |
152 (73.1) |
– |
|
Marital status |
||
|
Married |
148 (71.2) |
103 (52.8) |
|
Single |
39 (18.8) |
32 (16.4) |
|
Higher educationc |
129 (62.0) |
119 (61.0) |
|
MS Worsened |
90 (43.3) |
76 (39.0) |
|
Confirmed relapse |
59 (28.4) |
34 (17.4) |
|
Disclosed MS |
193 (92.8) |
177 (90.8) |
|
Employed (Total) |
208 (97.7) |
185 (94.9) |
|
Full time |
132 (63.5) |
113 (57.9) |
|
Part time |
76 (36.5) |
62 (31.8) |
|
Left employment |
n/a – |
10 (5.1) |
|
Sick leave |
||
|
≤ 7 days |
153 (73.6) |
137 (70.3) |
|
8 > 30 days |
32 (15.3) |
26 (13.3) |
|
≥ 30 days |
23 (11.1) |
12 (6.2) |
|
aOne patient formally decided to withdraw after completing their baseline questionnaire and prior to Month 8 time-point. bNon-returns at baseline were excluded from continuing in the study. cHigher education is defined as achieving diploma, degree level certificate or above. SD: standard deviation; EDSS: Expanded Disability Status Scale; RRMS: Relapsing Remitting Multiple Sclerosis (MS); SPMS: Secondary Progressive MS; PPMS: Primary Progressive MS. |
||
Work and sick leave
All 5 subjects who left work before completing their baseline questionnaire had RRMS. For the remaining 208 in work, employment type did not vary by disease course (χ2 1.17; p = 0.335). The median (IQR) time off sick over the previous 6 months was 0.5 days (0–9.75) with a range of 0–182 days, signifying that a few subjects with high sick leave days were skewing the mean number of days off sick. A small number (6.7%) had not disclosed their MS to their employer, and this group averaged 4.6 days sick leave.
Multiple sclerosis work instability scale
Over half (57.2%) of working subjects were at medium or high risk of job loss, as determined by the MS Work Instability Scale (MS-WIS), and a strong association was observed between the type of MS and the risk of job loss (χ2 16.6 (df 2); p < 0.001). Almost half (47.6%) of those with progressive MS were at high risk of job loss, compared with 17.1% of those with the RR type.
Multiple sclerosis impact of physical and psychological symptoms
This at-work cohort reported low to moderate impact from their physical symptoms (Table II). Likewise the score on the psychological component of the MSIS-29 indicated a moderate to low impact. Just 15% of subjects were found in the upper third score range of either of these domains. There was a strong association between the risk of job loss and both the physical and psychological components of the MSIS-29 (e.g. physical= χ2 106.5 (df 4); p < 0.001) (e.g. Physical; Fig. 2).
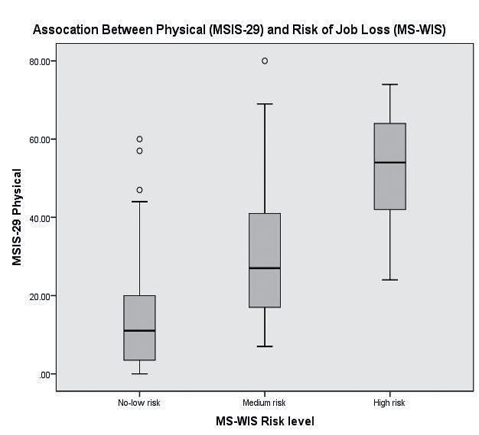
Fig. 2. Box-and-whisker plot for associations between physical impact of multiple sclerosis (MS) (MSIS-29) and risk of job loss (Multiple Sclerosis Work Instability Scale (MS-WIS)) in the baseline cohort.
|
Table II. Baseline and month 8 scale outcome |
||
|
Scale |
Baseline cohort |
Month 8 cohort |
|
Numeric Rating Scale, median (IQR) Health QoL Pain |
4 (2.5–5) 3 (2–5.25) 2 (0.5–5.0) |
3.5(2.0–5.3) 2.6 (1.2–4.6) 2.2 (2.2–4.5) |
|
Impact (MSIS-29), median (IQR) Physical Impact Psychological Impact |
23.5 (11–42) 12 (6–20) |
26.0 (10–40) 11 (5–19) |
|
Fatigue Index (NFI-MS), median (IQR) |
||
|
Physical subscale Cognitive subscale Summary subscale |
15 (12–19) 6 (5–8) 19 (14–23) |
16 (11–20) 7 (4–9) 20 (15–24) |
|
Work Instability (MS-WIS), % High risk Medium risk Low risk |
20.2 37.0 42.8 |
21.5 38.7 39.8 |
|
Anxiety and Depression (HADS), % At least Possible Anxiety (8+) Probable Anxiety (11+) At least Possible Depression (8+) Probable Depression (11+) |
42.5 22.1 25.3 6.1 |
34.2 22.5 13.6 7.0 |
|
Life Orientation (LOT-R), % Pessimistic (lower third) Neutral (middle third) Optimistic (upper third) |
20.2 51.0 28.8 |
28.0 44.1 28.0 |
|
Self-efficacy (USE-MS), % Low level (lower third) Medium level (middle third) High level (upper third) |
7.5 58.2 34.3 |
7.0 73.87 18.63 |
|
Quality of life (Leeds MS QoL), median (IQR) |
(7–14) |
10 (7–14) |
|
IQR: interquartile range; QoL: quality of life; MSIS-29: Multiple Sclerosis Impact Scale; NFI-MS: Neurological Fatigue Index; MS-WIS: Multiple Sclerosis Work Instability Scale; HADS: Hospital Anxiety and Depression Scale; LOT-R: Revised Life Orientation Test; USE-MS: Self-efficacy Scale for Multiple Sclerosis. |
||
Hospital Anxiety and Depression Scale
There was also a strong association between levels of anxiety and depression, and levels of work instability (χ2, p < 0.001) (Fig. 3). Of those at high risk of job loss, 54.8% had probable anxiety, compared with 6.7% of those at low risk. Similarly, 21.4% of those at high risk had probable depression, compared with 2.2% of those at low risk.
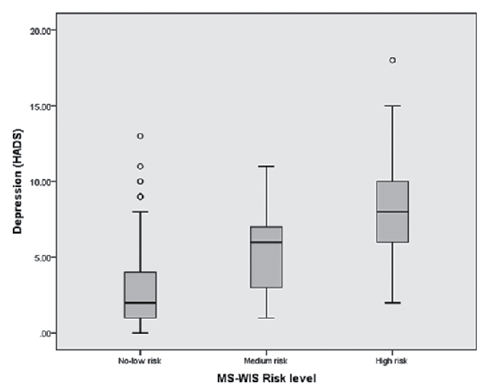
Fig. 3. Box-and-whisker plot for associations between depression (Hospital Anxiety and Depression Scale (HADS)) and risk of job loss (Multiple Sclerosis Work Instability Scale (MS-WIS)) in the baseline cohort.
Pessimism and optimism
Of the study subjects, 28.8%, 51.0% and 21.2%, respectively, displayed optimistic, neutral and pessimistic perspectives at baseline. A strong association was also found between orientation and anxiety and depression (χ2 29.7 (df 4); p ≤ 0.001). Thus, just 5.0% of those with an optimistic orientation were classified with probable anxiety, compared with 42.9% of those with a pessimistic orientation. Likewise, none of those who were optimistic were classified as probable depression, compared with 21.4% of those who were pessimistic. Similarly, just 6.7% of those who were optimistic were at high risk of job loss, compared with 35.7% of those with a pessimistic orientation (χ2 22.5 (df 4); p < 0.001).
Self-efficacy
For those with low self-efficacy the majority (87.5%) showed medium-high risk of job loss on the MS-WIS, as did 71.3% of those with medium self-efficacy, but only 25.7% of those with high self-efficacy showed such levels of risk (χ2 71.4 (df 4); p ≤ 0.001).
Multiple sclerosis quality of life
The majority of participants (83.7%) reported moderate to good quality of life (QoL). QoL was associated with most other variables, including anxiety and depression, self-efficacy and optimism-pessimism. For example, only 5.2% of those with a good QoL (lower third score range) were pessimistic in perspective, whereas only 5.9% of those with poor QoL (upper third of score range) were optimistic in their perspective (χ2 38.6 (df 4); p < 0.001). Of those reporting a good QoL, none were at high risk of job loss compared with 64.8% of those reporting a poor QoL (χ2 84.0 (df 4; p < 0.001).
Short-term variation in physical and psychological characteristics
Of the study subjects, 94.2% (195/207) completed the month 8 follow-up (with 1 patient formally withdrawing prior to the month 8 dispatch). Although numbers of non-responders were small (13, including 3 subjects who formally decided not to continue), there was no significant difference between responders and non-responders by age (t = 1.794; p = 0.074); gender (χ2 0.9; p = 0.525) type of MS (progressive vs relapsing) (χ2 0.09; p = 1.0), or their level (low, medium, high risk) of Work Instability at baseline (χ2 0.532 (df 2); p = 0.766).
At 8 months, disease type was stable, but a small number (3%) had transitioned from relapsing to secondary progressive. There was a significant fall in those reporting a confirmed relapse during the previous 6 months, from 32.4% at baseline to 20.6% at 8 months (χ2 5.3; p = 0.021).
Of those who remained in the study, 1-in-7 at baseline had reported a high physical and psychological impact of the condition (MSIS-29 upper third score range) at baseline, and this remained unchanged. There was no change in reported levels of fatigue (NFI-MS; Wilcoxon signed-rank test, p = 0.282), or of pain (NRS; Wilcoxon signed-rank test, p = 0.320). However, while 42.5% displayed possible or probable anxiety (HADS-A) at baseline, this fell to 34.2% at 8 months, with a greater fall in depression from 25.3% to 13.6% (HADS-D), the latter being significant (Wilcoxon signed-rank test Z –2.42, p = 0.016).
The percentage reporting moderate or high levels of self-efficacy (93%) remained stable, but this masked internal movements in either direction. For example, of those reporting high levels of self-efficacy at baseline (USE-MS upper third score range) only 69.1% retained this level at 8 months.
Similar variation was observed in the optimistic-pessimistic characterisation (LOT-R). Over a third (33.6%) moved their orientation, although it was rare for someone to move from a pessimistic to optimistic position, or vice versa (2.5%). While there was no significant change in the level of well-being (SWEMWBS) (Wilcoxon signed-rank test, p = 0.506), there was some movement across the low-moderate-high levels, although no one traversed from low to high or vice versa.
Of those in work at both baseline and at 8 months, 72.6% had not changed their level of work instability, 16.7% had shifted to a higher level of risk, and 10.8% to a lower level of risk. While the time to follow-up for the first wave was only 8 months, an exploratory stepwise conditional logistic regression sought to examine potential baseline predictors for subsequent risk of job loss. With a Nagelkerke R Square of 0.579; a Hosmer & Lemeshow χ2 of 0.889, and correctly predicting 83.9% of risk levels (no risk; some risk), baseline risk was strongly predictive of 8 month risk (odds ratio (OR) 22.0: 95% confidence interval (CI) 9.5–50.9); a relapsing remitting MS disease course reduced risk (OR 0.183; CI 0.040–0.84); while possible depression at baseline increased the risk (OR 7.10; CI 1.72–29.41) (Table III). At this early follow-up stage, other baseline factors did not show results of significance.
|
Table III. Logistic regression analysis: how baseline variables relate to the odds of high/medium work instability at month 8 |
|||
|
Odds ratio |
95% CI |
p-value |
|
|
Relapsing remitting MS |
0.183 |
0.040–0.841 |
0.029 |
|
Depression |
0.010 |
||
|
Possible |
7.101 |
1.715–29.406 |
0.007 |
|
Probable |
7.202 |
0.614–84.412 |
0.116 |
|
Baseline WIS |
22.006 |
9.510–50.918 |
0.000 |
|
95% CI: 95% confidence interval; MS: multiple sclerosis; WIS: Work Instability Scale. |
|||
DISCUSSION
Focus groups with PwMS indicated a number of psychological-related themes relevant to job retention. A postal questionnaire was constructed with standardized instruments, mostly validated for MS, but with some generic scales, which was designed to capture these themes within the wider bio-psychosocial model. The initial results of this longitudinal study show that while physical factors remain relatively stable in the short term among this working population of PwMS, psychological variables are much more changeable. The study provides significant evidence that these psychological variables are related to levels of work instability, and further follow-up data should determine the direction of this relationship.
Although over half of all participants were at medium to high risk of job loss, most also reported low to moderate impact from their symptoms and moderate to good quality of life. However, there was a strong association between anxiety and depression and levels of work instability, and low self-efficacy was also correlated with medium to high risk of job loss. This indicates that further study of the psychological determinants of job instability is indeed warranted.
Of the study subjects, 22.1% were rated at baseline as having probable anxiety on the HADS, with 6.1% rated as probable depression. These figures reflect the previously reported patterns in this population of anxiety being more prevalent than depression (e.g. 30). Both anxiety and depression are associated with work instability in this study, although at this stage it is not possible to determine direction of causality, or indeed whether or not such associations are bi-directional over time. However, both are amenable to change via psychological interventions, such as CBT.
The key issue here is that the fluctuation in these psychological characteristics is suggestive of state variables, which can be subject to change following intervention, rather than trait variables, which can be highly resistant to change. The fact that psychological variables show strong associations with the physical health and daily functioning of PwMS suggests psychological interventions could be effective in helping PwMS improve how they cope with their MS in the context of their work. Ipsen et al. (10) demonstrated interventions such as health-promotion programmes can play a role in reducing symptoms, such as pain, depression, anxiety, and sleep problems in a Non-MS Population. Understanding further the relationship these symptoms have with work instability could potentially lead to psychological interventions, which improve the likelihood of job retention in patients with MS.
The optimism/pessimism results are interesting as there was some movement between these categories over the first 8 months; 33.6% reported a change in their orientation. Optimism/pessimism has been shown to be a mediator in the relationship between improved depression and benefit-finding in psychotherapy for depression (31), with benefit finding being considered a successful marker of adaptation to chronic conditions. In addition, motivational interviewing (MI) is cited as a possible work-place intervention in the latest NICE Guideline Scope on Workplace Health (32). By eliciting perceived importance of a change in behaviour as well as confidence in achieving the change, MI can help increase the success rate for people receiving employment support (33). Confidence is a key ingredient of optimism, and therefore understanding how optimism is linked with job maintenance could inform MI programmes for people with MS.
We found that over 90% of participants had disclosed their MS to their employer. This topic had been discussed in depth in the focus groups, but it appears that working with an undisclosed condition was not a prominent feature of this research sample.
The data from the 8-month comparison shows the importance of the longitudinal design. While disease level was generally stable and there were no significant changes in pain and fatigue, psychological variables had varied and 17% of the sample had moved to a higher level of job instability, while some had reduced their level of instability. Given these risk levels are based upon cut-points, it is possible that the data represent small movements across such cut-points, and longer term trends may be more informative. Nevertheless, initial indications from the logistic regression suggest that screening for depression and work instability may be an important element in routine clinical monitoring in order to identify those at increasing risk of job loss, offering potential avenues for intervention from psychological and work-related services.
Further investigation of the relative contributions of these different factors to work instability will be carried out at further time-points. Longitudinal studies of this kind should also be able to identify intra-and inter-individual changes in such attributes, and seek to identify where such changes impact on the ability to maintain meaningful employment, or are a consequence of increasing work instability. At the present time, no causality of direction is inferred by the associations, but as additional time-points are accrued, evidence should build to support causality hypotheses.
Weaknesses
A potential weakness of the study is the lack of a validated measure of cognitive functioning. Ideally a brief neuropsychological screen would have been carried out on all participants (e.g. Brief International Cognitive Assessment for Multiple Sclerosis (BICAMS) (34)), but this was not possible (even using just the Symbol Digit Modalities Test) given the time and resources available. Instead, a simple visual analogue scale (VAS) covering the following aspects of cognition was used: I have problems making decisions and working things out; I can’t say what’s on the tip of my tongue; I can’t seem to concentrate; I forget where I have put things; and My thinking seems slowed down. The relationship between cognitive function (as reported on the VAS) and other outcome variables will be reported later.
In addition, due to the importance of having a brief questionnaire pack that would be completed by as many participants as possible over all time-points, mood was assessed by the HADS rather than by diagnostic measures of psychiatric status; as such this study reports anxiety/depression symptom severity and not anxiety/depression disorders. This scale has been previously validated for use in the MS population (35).
Strengths
The data collection tool was built upon the lived experience of PwMS, and what was deemed important to them in the context of their work. The scales used to ascertain the various domains, with the exception of the cognition items, have all being validated for use with MS. As data accrue over time, the opportunity will arise to strengthen the predictive power for work instability, and highlight the possible pathways for intervention.
REFERENCES
